Scores




Chronic obstructive pulmonary disease (COPD) is a common condition among primary care patients, characterized by progressive airflow limitation that is usually associated with an enhanced chronic inflammatory response in the airways and the lung.
COPD is a preventable and treatable disease, usually associated with smoking, yet it is still often diagnosed late and may be undertreated or even untreated when it's recognized, which is the possible reason why COPD has risen to become the third leading cause of death in the United States.
To make a formal diagnosis of COPD, providers must perform spirometry, which is often not easily accessible to primary care clinicians and patients and remains underused as a diagnostic and follow-up assessment. Also, diagnosis and management of COPD was not a significant part of medical training for many clinicians.
Many national and international organizations create and disseminate guidelines and care recommendations to supplement limited training and provide updated information on diagnosis and management of COPD.
However, these recommendations and guidelines are often not in a format that is suitable for point-of-care use. For example, the current 2017 Global Initiative for Chronic Obstructive Lung Disease (GOLD) recommendations provide an important evidence and guidelines for COPD management, but with 132 pages are quite lengthy and inconvenient to use at point-of-care.
This is one of the reasons why COPD Foundation made the brief, point-of-care COPD Foundation Pocket Consultant Guide (PCG) back in 2007 with major updates in 2012 and 2016.
The PCG guide is basically a tri-fold card to be used in the office, emergency department or hospital. COPD foundation also made this guide available online and as a mobile app that we review today.
COPD Foundation Pocket Consultant Guide mobile app is even more convenient than its paper card version, knowing that many clinicians use their mobile phones and apps in their daily practice.
The app was designed to be a practical tool to assist practicing clinicians in managing the diagnosis and treatment of individuals with COPD at the point of care.
The PCG is designed to help clinicians identify patients for whom spirometry should be performed, and determine how patients should be classified based on spirometry, including the type of additional assessments and diagnostic evaluations.
The app includes the two most recommended questionnaires for the assessment of COPD patients, COPD Assessment Test (CAT) and the mMRC Breathlessness scale, a form that includes spirometry and COPD exacerbations.
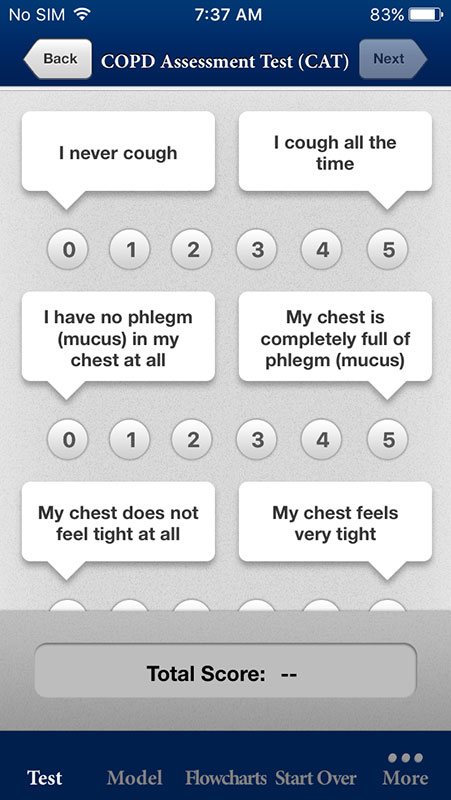
CAT assessment tool will take users through the set of questions trying to determine the possibility and severity of COPD. The users respond by assigning a number from a 0-5 scale to the question.
For example, the first question asks about a cough with possible answers 'I never cough' that corresponds 0 on the scale, and 'I cough all the time' that corresponds 5.
In the same fashion, users need to provide other answers about phlegm in chest, chest tightness, energy levels, and so on, which all add points to the total score.
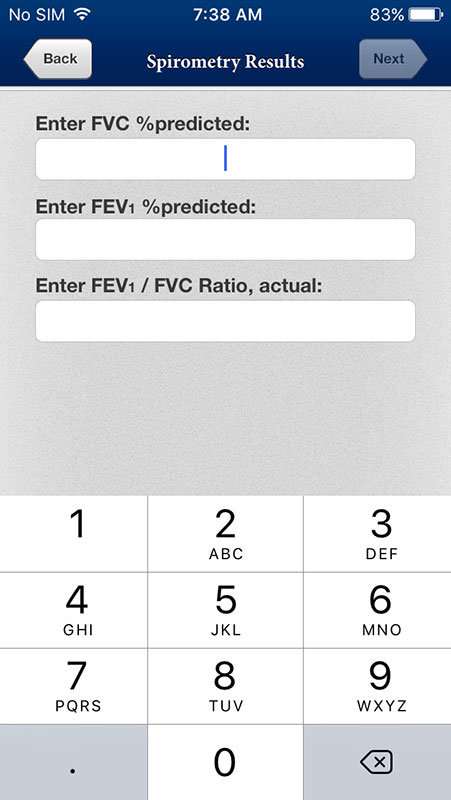
In the next step, clinicians are asked to provide patient's percentage of forced vital capacity (FVC), a percentage of forced expiratory volume in 1 second (FEV1), and FEV/FVC ratio for further assessment.
Finally, clinicians will be asked about a number of exacerbations the patient had in the last 12 months, with three options to choose: 0, 1, and 2 or more.
On the following page, the results would be displayed showing the patient's spirometry guide and providing a guidance for categorizing spirometry results.
These results fall into 3 major groups, including normal, spirometry grade 0 (SG0); obstructive lung disease, spirometry grades 1-4 (SG1-4); and reduced lung function without obstruction, spirometry grade undefined (SG-U).
This page also highlights the other roles of spirometry, including identifying those with lower FEV1 (below 60%) who may benefit from evaluation of hypoxemia at rest or with exercise and for those with FEV1<45% predicted in whom you should consider computed tomography (CT) evaluation for emphysema.
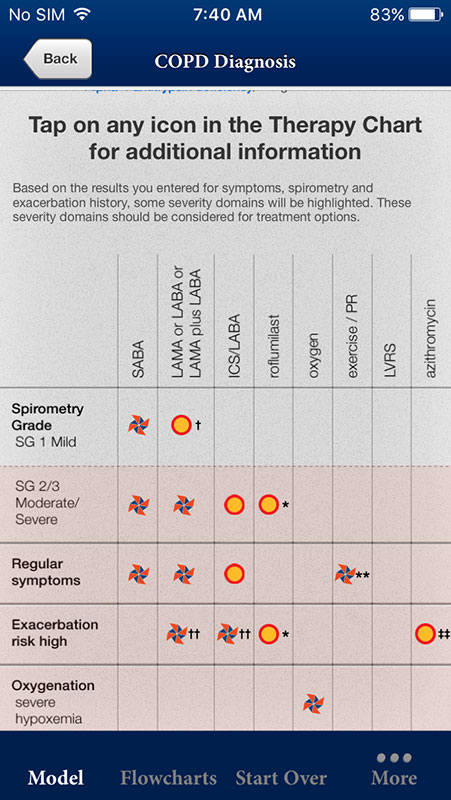
There are also treatment options listed in a chart, with icons that users can tap on to view additional information about each option, i.e. first line and second line of therapy.
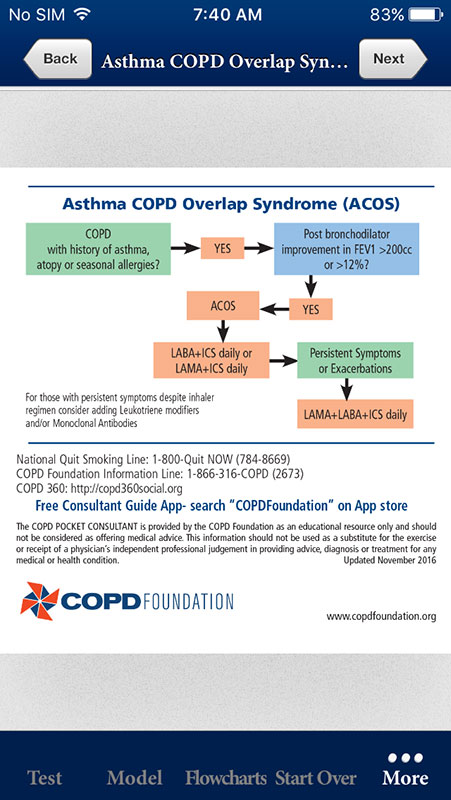
Flowcharts tab features the algorithm for COPD management with very clear and precise instructions, as well as Asthma COPD Overlap Syndrome (ACOS) algorithm. Both algorithms use color codes and are easy to follow and understand.
Similar to CAT, mMRC Breathlessness scale asks clinicians to answer how breathless are their patients by choosing one of the grades from 0 to 4.
This part may be confusing at the first use because you don't see grades to choose from, only the blue area that actually slides up and down, allowing you to choose your answer. Similarly to CAT assessment, users are then asked about post spirometry use results (FVC and FEV percentage), as well as about exacerbations, before being taken to the page with spirometry grade results and recommendations.
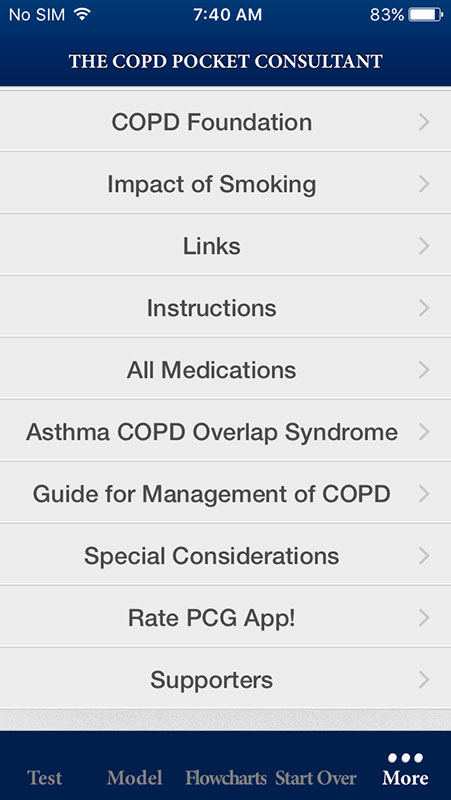
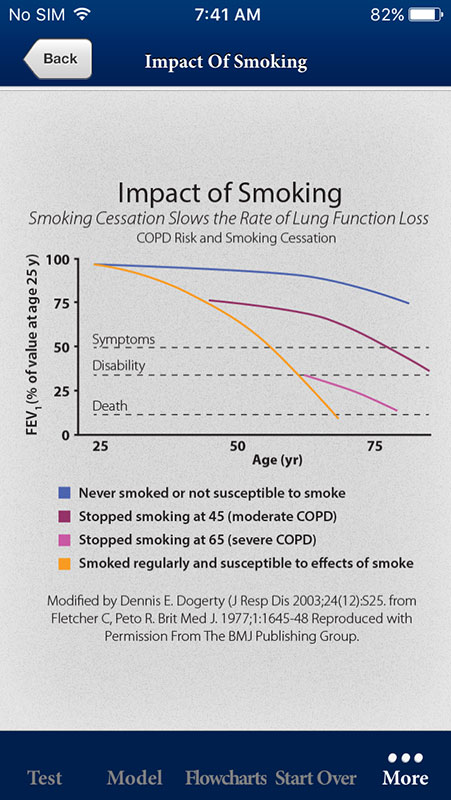
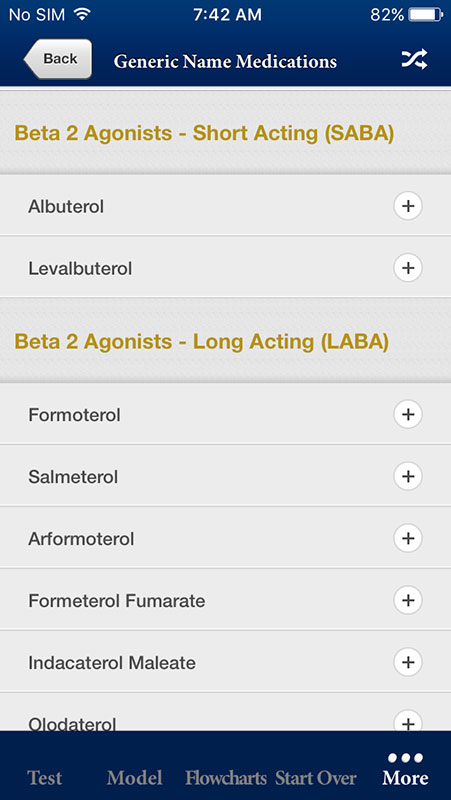
COPD Foundation Pocket Consultant Guide app also contains other useful information, such as a list of generic medications used to treat COPD and other respiratory conditions, Impact of Smoking graph showing the COPD risk and smoking cessation, links, etc.
The app is available for free, currently only on iOS, while the version for Android users is promised to be released later this year.
Overall, COPD Foundation Pocket Consultant Guide app is an essential resource for diagnosis and management of COPD at the point of care.
There is a slight bias concern because CAT assessment is literally owned by Big Pharma (GlaxoSmithKline) and it is only available via this app. Still, this doesn't diminish its value, mostly because it is freely available to practicing physicians and other clinicians who treat COPD patients.
Benefit: All clinicians can use this app as a COPD assessment and management resource
Verdict:
For- Provides recommendations for diagnosis and treatment of COPD in an easy-to-follow format
- Results are provided in a format that can be used at the point of care
- Spirometry results and treatment options are briefly, but well explained
- The assessment tools are owned by Big Pharma







































Your thoughts on this
Loading...