Scores




Sepsis is a serious systemic condition caused by certain infections, such as infections of the lungs (e.g., pneumonia), urinary tract (e.g., kidney), skin, and gut, as well as by certain germs, such as Staphylococcus aureus (staph), Escherichia coli (E. coli), and some types of Streptococcus (strep) that all can cause sepsis more than other bacteria.
While anyone can develop sepsis from an infection, it usually occurs in people aged 65+ years or children younger than 1 year, as well as in people with weakened immune systems, or who have chronic medical conditions, such as diabetes.
According to CDC, more than 90% of adults and 70% of children who developed sepsis had a particular health condition that may have put them at risk. Sepsis is also a serious problem in hospitals worldwide, although it usually begins outside of the hospital for nearly 80% of patients.
Sepsis remains the ninth leading cause of disease-related death and the primary cause of infection-related death in the ICU. It results in 1.3 million hospitalizations per year and over 250,000 deaths in the US, which is more than breast cancer, prostate cancer, and AIDS combined.
Sepsis can quickly lead to circulatory shock, organ failure and death mainly due to late recognition and treatment. Sepsis doesn't present with a single sign or symptom, and that's why it's hard to detect and treat. It is rather a combination of symptoms, that may include fever, sore throat, vomiting, diarrhea, shivering, pain or discomfort, shortness of breath, high heart rate, clammy or sweaty skin, and confusion or disorientation.
The key to surviving sepsis is a prompt recognition and treatment with IV antibiotics IV fluids within 1 hour of diagnosis, and other medication that stabilize a blood pressure within 3 and 6 hours depending on symptom severity. Delays that may easily occur in busy hospital environments can lead to avoidable complications and deaths.
This is why it is important that healthcare providers, especially those working in ICU have guidelines that could help them act rapidly once they identified sepsis in patients.
With this purpose, Escavo made the Sepsis Clinical Guide app that we reviewed on SteadyHealth, which is a comprehensive reference on sepsis diagnosis and management for mobile devices.
Since the key to surviving sepsis is rapid recognition and treatment, Escavo recently introduced another sepsis app called Sepsis Timer, which is a simple clinical decision support tool with a timed checklist designed to help busy clinicians perform key steps to treat sepsis within prescribed time intervals.
The treatment steps and timelines described and used in Sepsis Timer app are based on Surviving Sepsis Campaign (SSC) guidelines that got the recommendations from the Institute of Healthcare Improvement (IHI) and the US Centers for Medicare and Medicaid Services (CMS).
The app basically put these sepsis guidelines into a checklist type format with the goal to ensure the patient with sepsis receives treatments implemented within 3- and 6-hour period.
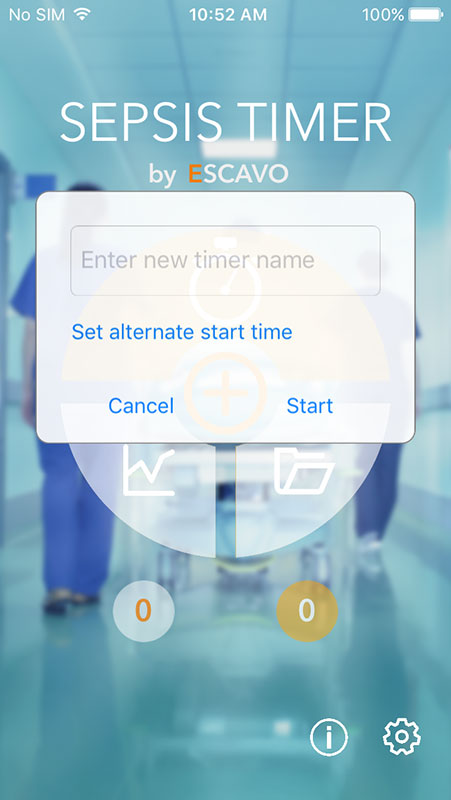
Sepsis Timer app has a simple and elegant interface that features a timer on the main page which allow users to start a new sepsis timer, view the list of active timers, view stats of completed timers, and view list of completed and archived timers.
Before starting using their first time, users will be asked to review the Information section which provides a user manual for using the app, helps users understand sepsis basics, and gives more info about the developers.
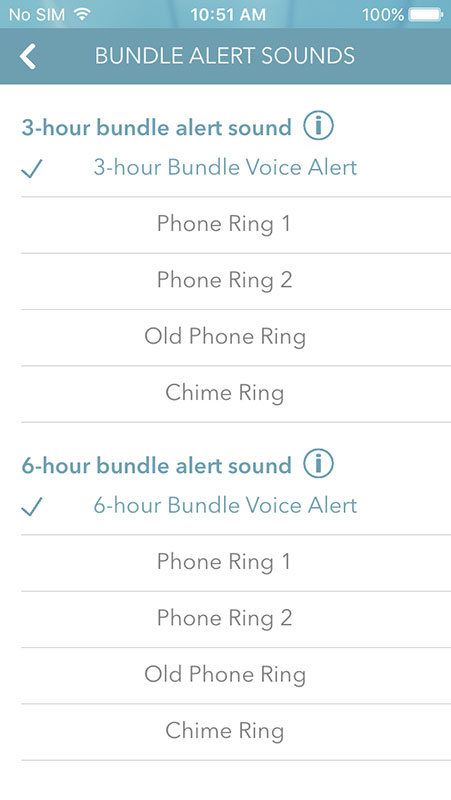
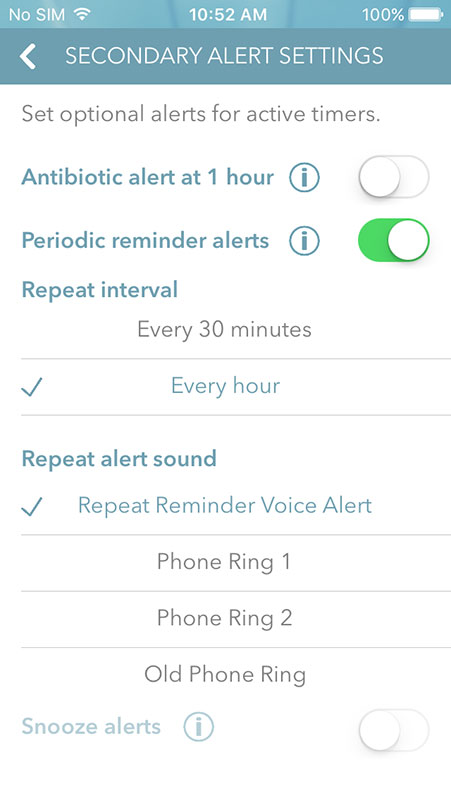
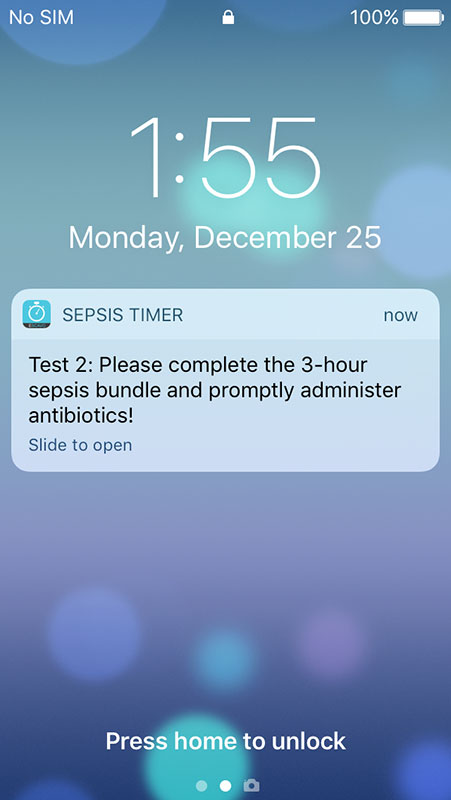
Also, the app would suggest you open settings so you can set timer alerts and reminders, along with the sounds, as well as to set stats view.
To start using the timer, simply tap on the plus symbol and add timer name and set alternate start time (if you don't want to use the current time).
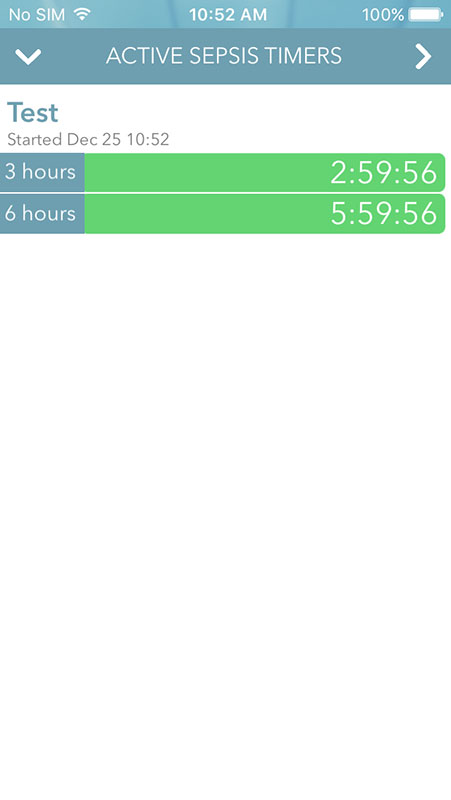
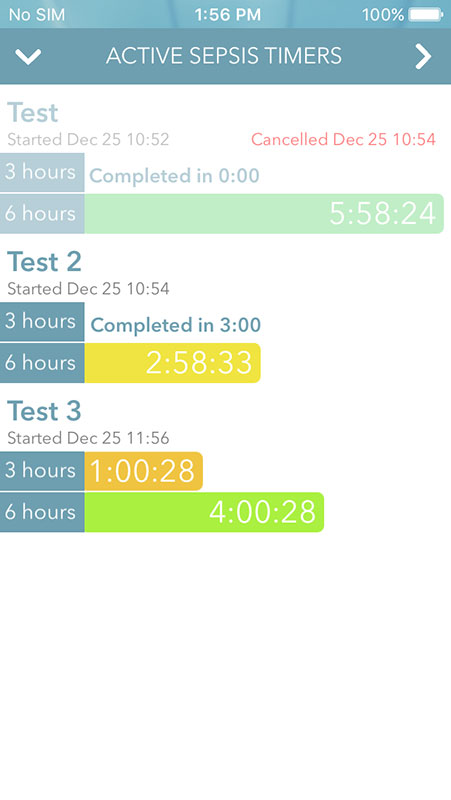
You'd be taken to the Active Sepsis Timers page that can also be accessed by tapping on the stopwatch icon on the timer. You'd see all the timers you've started, with remaining times for 3- and 6-hour cut-offs. Tap on these to open sepsis bundles for both timeframes.
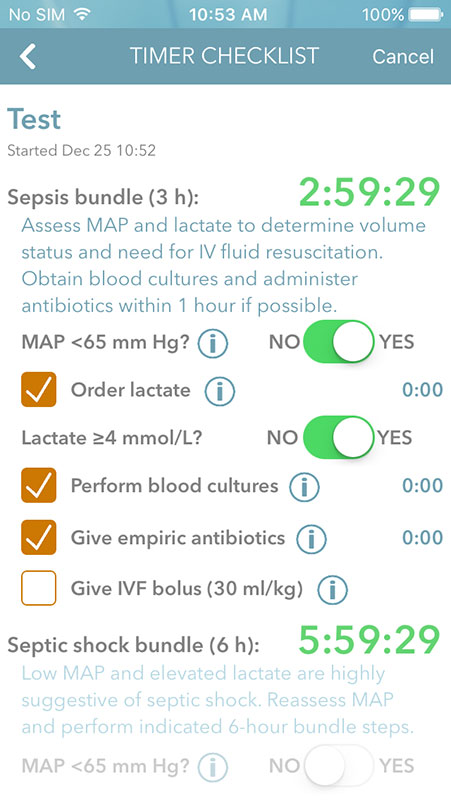
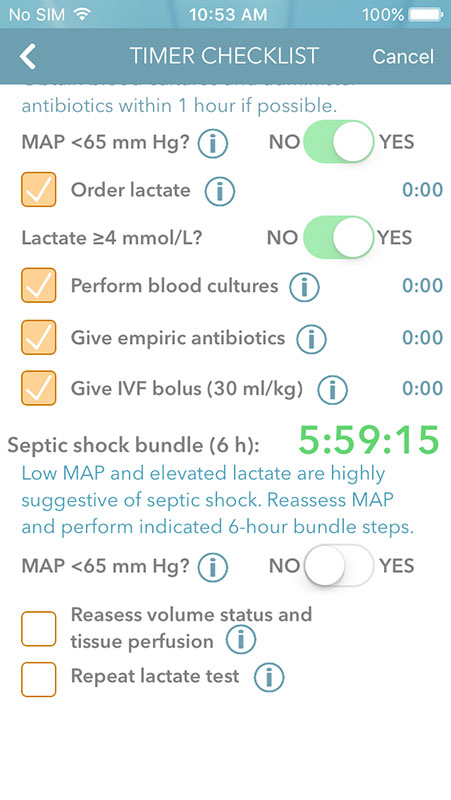
Sepsis treatment bundles are presented as a checklist based algorithm that allows clinicians to order lactate based on MAP assessment, perform blood cultures, give empiric antibiotics within 1 hour, and perform 60-hour bundle steps, including reassessing MAP and volume status, and repeating lactate test if necessary.
This ensures that patients receive the proper care at the right time, which is crucial for successful sepsis treatment.
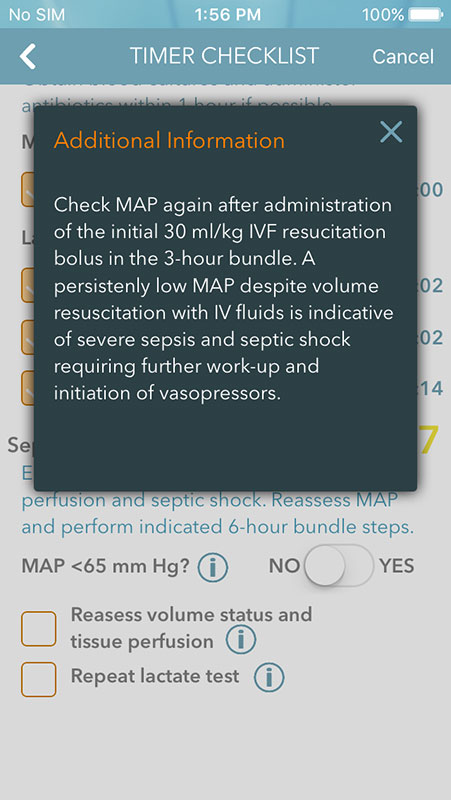
Each of the steps in the Timer Checklist has 'i' button which provides additional information about the particular step, i.e. blood cultures should be performed before antibiotics, cultures should be drawn from two sites, antibiotic regimen should cover Gram-negative and Gram-positive bacteria and comprise of double or triple antibiotic therapy, and so on.
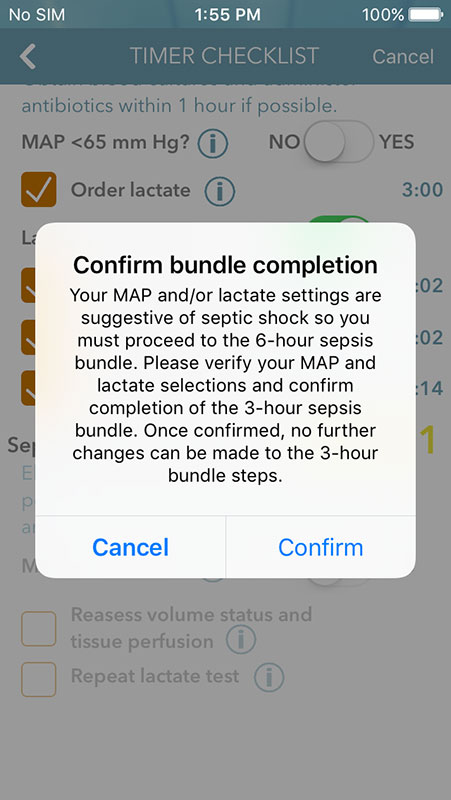
After completing and checking all steps, the app would prompt you to confirm bundle completion., which would mark the bundle as completed on the Active Sepsis Timers page.
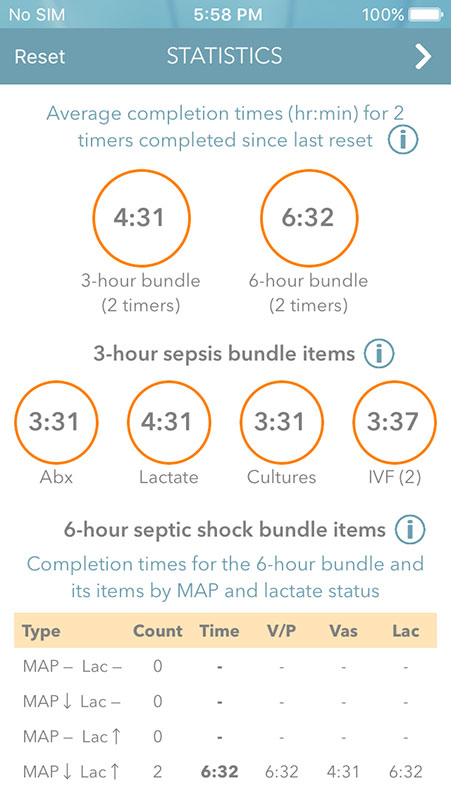
You can proceed to the Statistics page that would show average response times for completed timers, i.e. treatment steps and bundles over time. This is a great tool for tracking your response times.
Stats page also features Info buttons that would provide users with more information about the stats, bundles and completion times.
Sepsis Timer provides a lot of useful information, however, it would be good if it also links to the Sepsis Clinical Guide app that provides more evidence-based information.
Also, unlike Sepsis Clinical Guide app, Sepsis Timer app is not available for Android at this time.
Overall, Sepsis Timer is easy to use app that utilizes timers and reminder alerts which are evidence-based and well-referenced to ensure that clinicians provide their patients who have sepsis with the proper care at the right time.
Benefit: Clinicians across any specialty who care for patients with sepsis
Verdict:
For- Easy to use checklist interface implementing 3- and 6-hour bundles based on recent sepsis guidelines
- Users can set reminders
- Additional information sections throughout the app explaining each critical step
- It would be good if the app links to the Sepsis Clinical Guide app
- Not available for Android


































Your thoughts on this
Loading...