Scores




Atrial fibrillation is one of the leading causes of stroke, usually recognized by the palpitations in the chest area, with sensations of irregular heartbeat, and followed by shortness of breath. These symptoms, often paired with weakness, fatigue, lightheadedness or dizziness, should be a warning signal to patients that they might have the condition that doubles the risk of heart-related deaths and is associated with a 5-fold increased risk for stroke if left untreated.
But, there lies the problem. The atrial fibrillation stays untreated because the patients often don't have any symptoms, and usually find out about their condition on regular checkups. Even after they find about it, some patient still don't consider it a serious condition, and refuse to be put on blood thinner medications, which might have dangerous consequences.
Another problem when dealing with atrial fibrillation and stroke risk is the treatment with oral anticoagulants, i.e. decision when to start it and what drug to use, which is completely intuitive for most healthcare providers. Also, it's not easy for patients too, to learn that they not only have a high stroke risk, but also that they'd be put on a medicine that could make them bleed from their gut or into their head.
Therefore, knowing the stroke and bleeding risk, as well as the effects of particular oral anticoagulants is crucial before starting the therapy.
This is why healthcare providers should resort to calculators helping them with specific numbers on stroke or bleeding risk, as well as other support tools that could help them to evaluate the effects of OAC treatment. Some of these calculators and decision support tools are readily available as mobile apps.
We already reviewed MAQI2 Anticoagulation Toolkit app that helps healthcare providers answer difficult questions and make decisions regarding anticoagulation therapy.
Another similar app we review today is AnticoagEvaluator app, created by the American College of Cardiology (ACC) with the goal to help clinicians dealing with these complex questions and decisions by providing specific numbers on stroke and bleeding risk, as well as benefits and risks of therapy with oral anticoagulants.
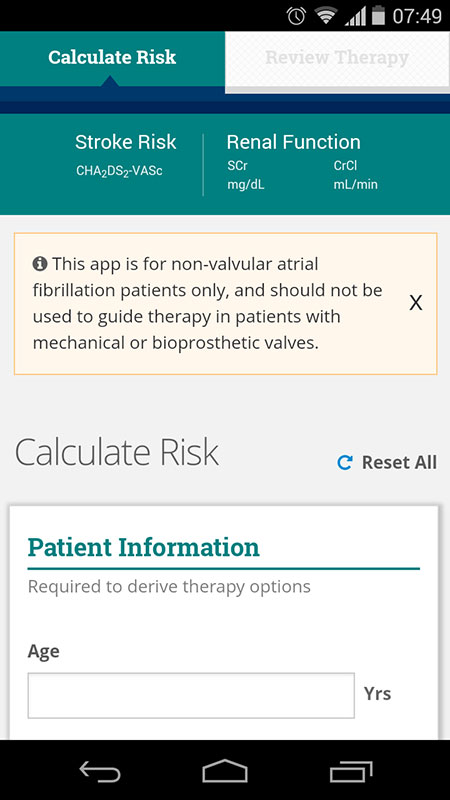
Upon starting the app, you'll notice it has simple and straightforward design, very much similar to the interface of another app by College of Cardiology, called Statin Intolerance app that we reviewed couple of months ago.
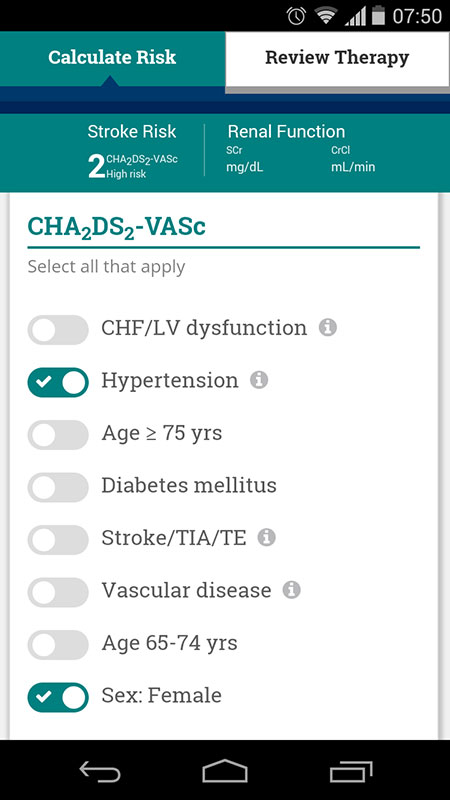
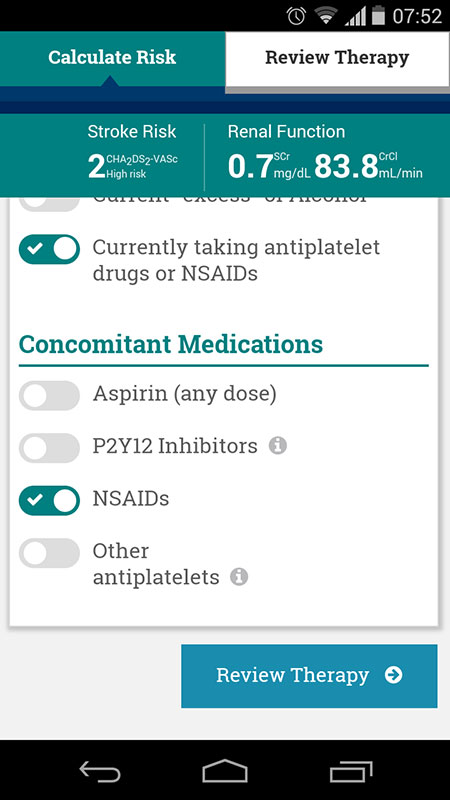
The AnticoagEvaluator app opens to the main screen, which is basically a calculator, allowing user to first enter patient's information, such as age and sex, and then can calculate the CHA2DS2-VASC and HAS-BLED scores, as well as Creatinine Clearance. Users can also add the information about the concomitant medications, i.e. if the patient is using Aspirin, NSAIDs, P2Y12 inhibitors or other antiplatelet drugs.
These calculators are separated in sections, and the users are supposed to enter data in each (if applicable) before proceeding to review the therapy.
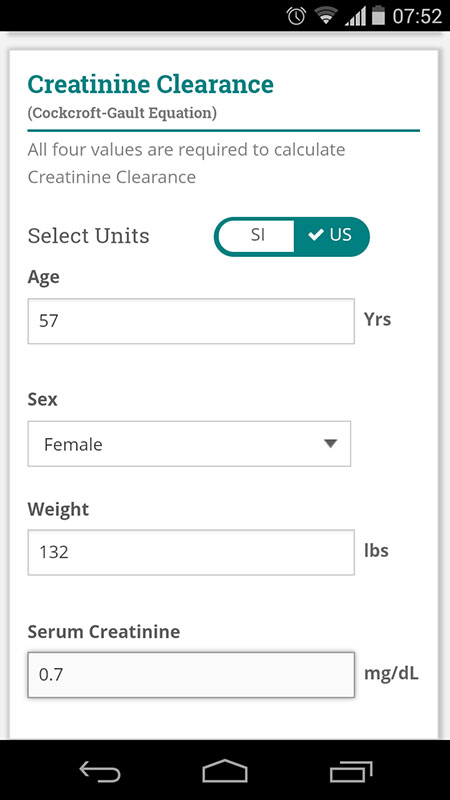
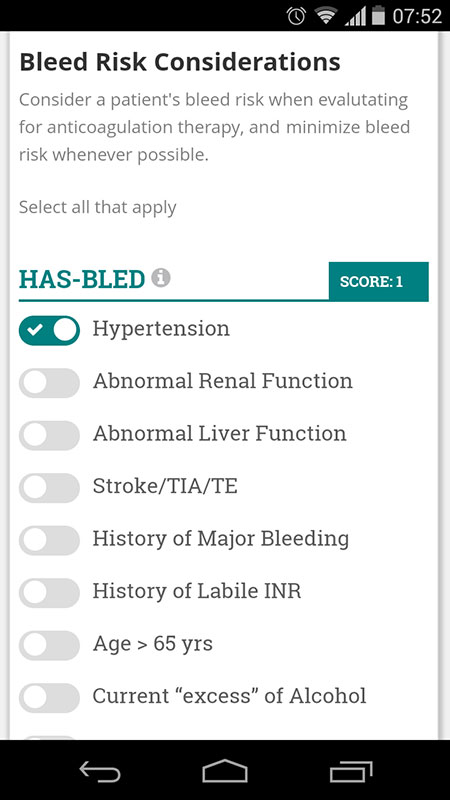
For this review, I've entered the data for 57-year old female patient with mild hypertension, who was also using Naproxene as a relief for her gout.
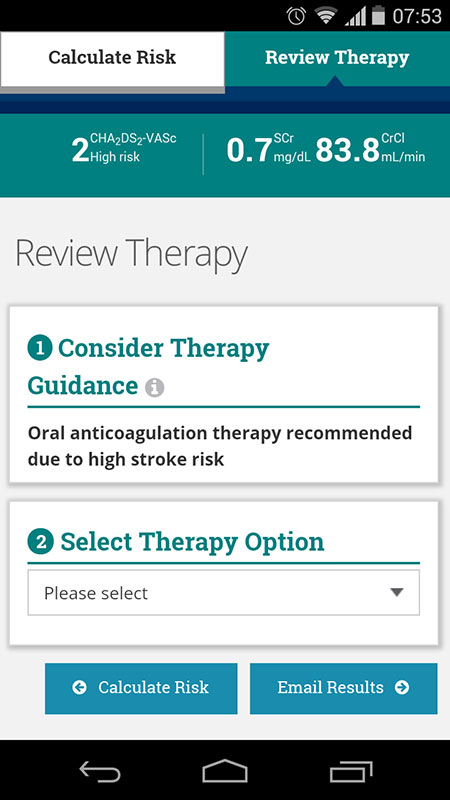
After entering all the information, the app automatically calculated the stroke risk, which was high in this case, along with the renal function, suggesting me to start oral anticoagulation therapy on the Review Therapy screen.
On the same screen, you can now select therapy option with couple of antithrombotic medications, from antiplatelets (Aspirin, Clopidrogel) to anticoagulants, such as Warfarin. You can also choose no therapy option to evaluate the baseline annual stroke risk levels.
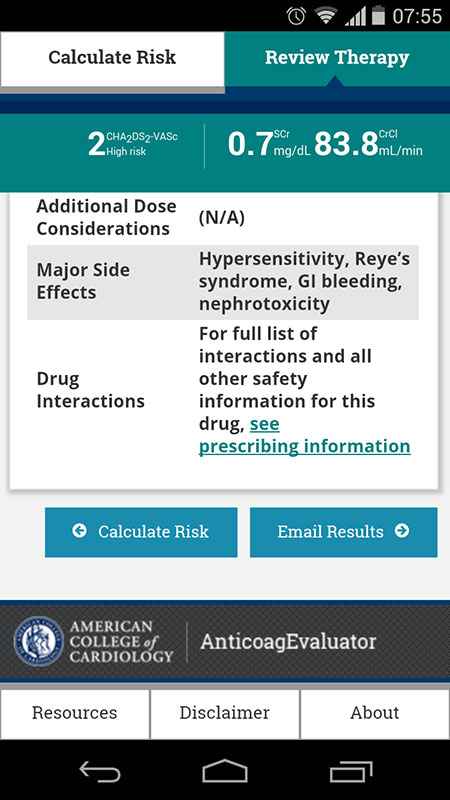
Choosing any of the medications from the list will provide you with further info on standard daily dose based on clinical trials, as well as information on stroke risk/benefit, bleeding risk, and safety information, which includes additional dose considerations, major side effects and interactions with other drugs.
If I put my patient on Aspirin, I would inform her that the risk of stroke can be reduced by approximately 22% with the risk of major bleeding of 1.1%. Warfarin would reduce the stroke risk by additional 44%, but the risk of major bleeding would be increased to 3.8%.
I can tell this to my patient during her visit, or I could share these results with her by sending an email (the app supports this option).
All dosing information and calculations in AnticoagEvaluator app are based on SPARC Tool developed by Peter Loewen, Pharm D, and also supported by authority recommendations and guidelines available in the Resources section of this app, which also links to other anticoagulation resources and other ACC's mobile tools.
I can only conclude that the AnticoagEvaluator app is great tool meant to support clinical decision on the best antithrombotic therapy options, allowing healthcare providers to discuss these options with their patients and explain them the benefits and risks of such therapy.
Benefit: Healthcare providers who want to inform their patients on the best antithrombotic therapy options, including risks and benefits of such therapy.
Verdict:
For- Straightforward and easy-to-use interface
- Calculator with lots of recommendations
- Made by authority source with lot of references
- Ability to email the results
- I couldn't find anything particularly bad about this app




































Your thoughts on this
Loading...