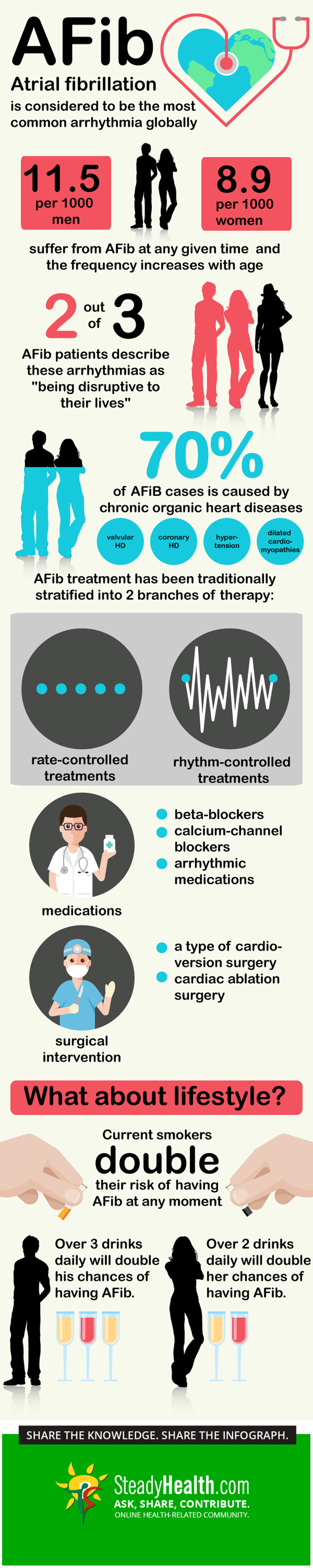
Atrial fibrillation (AFib) is considered to be the most common arrhythmias globally. It is believed that AFib can occur as frequently as in about 8.9 per 1000 women and 11.5 per 1000 men at any given time in a population and the frequency of this disease increases with age [1]. In 70 percent of cases, AFib is caused by chronic organic heart diseases such as valvular heart disease, coronary heart disease, hypertension and dilated cardiomyopathies [2].
The sensitive cardiac muscles gradually change their structure after dealing with chronic pathologies and this can drastically affect the electric flow through the heart and change the way your heart beats [3]. In 2 out of every 3 AFib patients, these arrhythmias are described as "being disruptive to their lives" [4]. The standard of care for this condition has been traditionally stratified into 2 branches of therapy:
- rate-controlled treatments and
- rhythm-controlled treatments [5].
Rate-Controlled Philosophy
The first method of therapy we will consider is rate-controlled management for atrial fibrillation. The aim of heart rate control is to minimize excessive heart rates and to prevent the symptoms and malaise associated with the cardiac changes linked with AFib [6]. This can be achieved through one of two ways:
- medications and
- surgical intervention.
The medications used in this case are termed negative chronotrophic drugs — medications that alter the flow of potassium and sodium through the heart [7]. This effect can reduce the flow of electricity through the atrioventicular node (AV) — the main natural pacemaker that keeps the heart beating constantly and consistently [8].
If medications do not meet the therapeutic control of AFib, surgical intervention will be required.
Cardiac catheter ablation surgery is quickly becoming the gold-standard for long-term control of AFib. A cardiac surgeon uses specialized electrodes to determine where is an excessive discharge in cardiac muscle and then will burn the muscle to reduce the interference in the heart rate [11].
Cardiac ablations will improve the conduction through the heart but generally require multiple surgeries to have a sustained impact. A recent study found that in 188 patients that required cardiac ablation surgery, 139 of them still had arrhythmias after the first procedure and 90 after the second procedure. In total, 91 percent of these recurrences occurred within two years after the surgery. In this same study, only 7 patients experienced any kind of severe complications after the operation with no deaths and 82 percent of patients stated that their symptoms had improved significantly [12].
The ideal patients for rate-controlled strategies are generally suffering from persistent AFib and are less than 65 years old. These patients will be less symptomatic and may only have underlying hypertension with no evidence of heart failure [13].
Rhythm-Controlled Philosophy
Another dogma for the controlling of AFib is the rhythm-controlled philosophy. This theory is used for a different group of patients and is beneficial for patients suffering from paroxysmal AFib or new onset AFib after the age of 65. These patients typically also have underlying heart failure and are more symptomatic [13].
Patients presenting with AFib will generally be started on a combination of medications that alter the electrical flow throughout the heart. These medications will often be a combination of beta-blockers, calcium channel blockers, and amiodarone. The medications most effective in this category of management are termed anti-arrhythmic medications and members of Class I and Class III are generally those used when a patient presents with AFib [14].
Although these medications are effective initially in managing a patient's AFib, the unfortunate truth is these medications are often a bridge to some type of cardioversion surgery because of the vast profile of side effects that are linked to these medications. Drugs such as amiodarone are used from the beginning of therapy but can result in serious side effects such as thyroid toxicity, skin discoloration photosensitivity, and numerous gastrointestinal complications that often force patients to seek alternative therapy [15].
As mentioned above, cardioversion is the next step in management that many of these patients will need to endure due to the advanced nature of their symptoms. This surgery involves the placement of electrodes in the heart and then a secondary device will keep the energy level in check to prevent further episodes of AFib. In a recent study used to determine the effectiveness of cardioversion, 244 participants were enrolled and it was found that almost 90 percent had a return to a normal cardiac sinus rhythm. Furthermore, 34 percent required no additional intervention almost 3 years after the surgery. [16]
Lifestyle Modifications
If you have a smoking or drinking problem and had ever visited a medical office, there is a good chance that you have been educated about the dangerous and negative impacts cigarettes and alcohol have on your health. Sure they are dangerous to your lungs and liver but did you also know that they could be two key factors in you developing AFib later on in life?
One study found that there is a dose-dependent link between alcohol consumption and the likelihood of developing AFib.
This effect can be much worse because as you age, your body is not able to process the alcohol as effectively and even half this consumption of alcohol over the age of 60 could lead to negative consequences for your heart. [17]
Another study specific to cigarette smoking and AFib found that no matter of what quantity of cigarettes you smoked during your life, smokers had a higher risk of developing AFib compared to non-smokers. Current smokers double their risk of having AFib at any moment while those who quit smoking still have about a 1.5 times more chance of developing the condition compared to non-smokers. [18]
Still looking for more info about atrial fibrillation treatment? The editor suggests:
- 3 Exercise Safety Tips When You Have Atrial Fibrillation
- Atrial Fibrillation Treatment: The Differences In Approach Between Cardiologist And Cardiac Surgeon
- 3 Diet Tips For Atrial Fibrillation Prevention
- Alcohol And Atrial Fibrillation: Will Drinking Worsen Your Cardiac Disease
- Natural And Alternative Treatment For Atrial Fibrillation
- Better Diagnosis: The Key For Atrial Fibrillation Treatment Success
- Irregular Heartbeat And Heart Palpitations: Difference Between Atrial Fibrillation And Arrhythmia
- Infographic bby SteadyHealth.com


Your thoughts on this