Table of Contents
This year just in the United States about 500,000 people will be diagnosed with atrial fibrillation, also known as A-fib. In atrial fibrillation, "bad connections" at the pulmonary veins, which bring oxygenated blood back from the lungs, cause "short circuits" in the conduction of the electrical impulses from the sinoatrial node that time the beating of the heart.
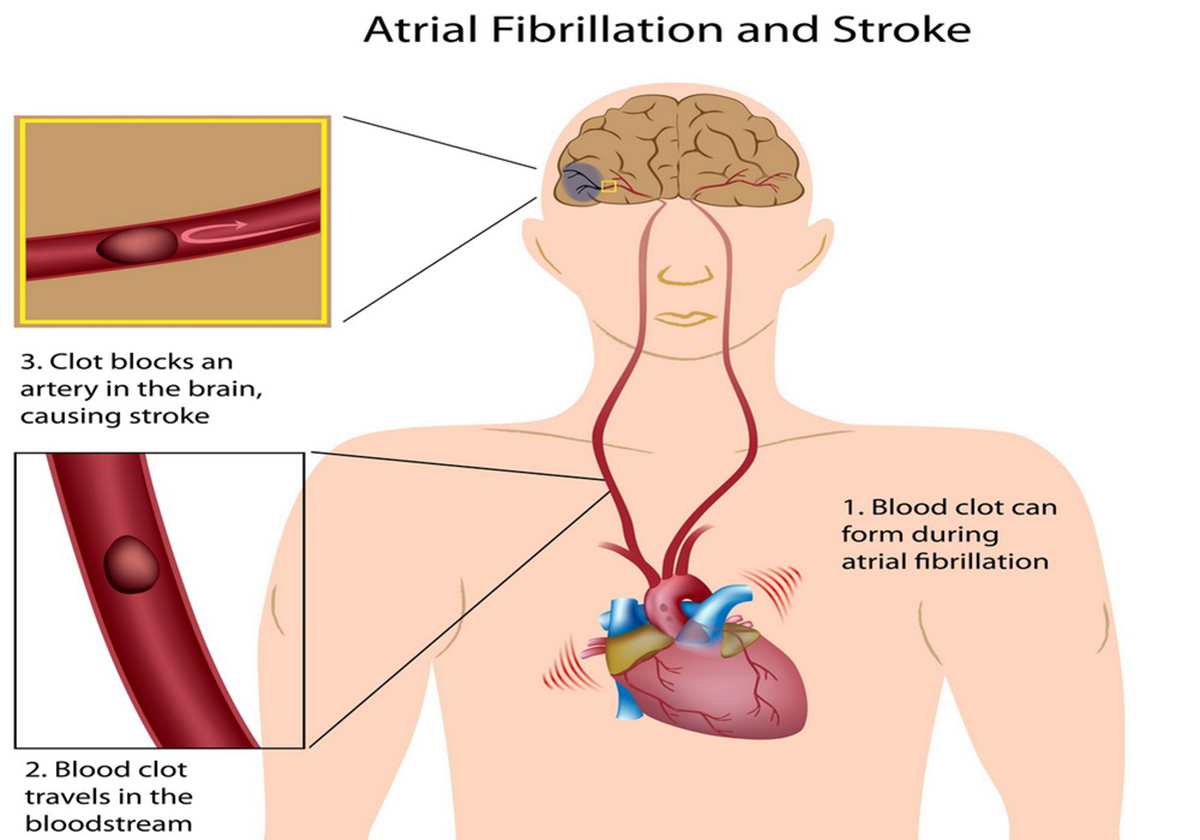
Instead of a steady impulse traveling across the atria to make them beat in rhythm, a series of disorganized impulses takes over. One "spark" in either or both of the upper chambers of the heart can cause more, so that the rhythm of the atria becomes more and more disorganized. The left atrium loses its ability to pump blood efficiently into the left ventricle for distribution to the rest of the body, and clots form. These clots may escape and eventually cause stroke.
A-fib may be paroxysmal, occurring for just a few minutes or a few hours until the atria restore their normal rhythms, or it may be permanent, occurring all the time. Often atrial fibrillation causes no symptoms at all, but in about 10% of cases, there may be:
- General weakness, dizziness, or fatigue.
- Fainting, or feeling as if one is about to faint.
- Palpitations, a sense of fluttering in the chest.
- A "blue at the gills" appearance, cyanosis (bluish skin due to lack of oxygen) in the neck and face.
- Enlarged eyes, bulging neck veins, or sudden accumulation of "water weight" in the mid-section.
- Swollen feet and ankles.
Usually, the pulse is rapid, in the 110-140 beats per minute range. The lower the blood pressure, the greater the clinical significance placed on rapid pulse.
Sometimes atrial fibrillation is so severe it is necessary to shock the heart back into normal rhythm. The procedure is not "horrific" but neither is it painless.
In milder cases, doctors put A-fib patients on various blood thinners to prevent the coagulation of the blood that leads to the clots that block arteries and cause stroke. Using blood thinners, however, is generally problematic.
Coumadin (warfarin), for example, has to be taken in a precise dosage. Too much causes bleeding even without cuts or scrapes. There's a real risk of hemorrhagic stroke, when a blood vessel "leaks" rather than clots, with an overdose of this medication.
Too little Coumadin doesn't stop clotting. And it's necessary to be careful with diet when taking Coumadin. This medication works by interfering with the ability of the blood to use vitamin K in making clotting factors. Leafy greens contain vitamin K, and eating a healthy salad can make this medication less effective.
See Also: Ten Essential Facts About Stroke
The newer medications dabigatran (Pradaxa), rivaroxaban (Xarelto), apixaban (Eliquis), and edoxaban (Lixiana) don't require dietary restrictions and are less likely to "work too well" and cause hemorrhagic strokes. But they are expensive, and as one user puts it, the bleeding from a paper cut can look like a crime scene.
Walking can become painful. Participation in sports or working around the house is out of the question, because of the bleeding risk. Easy bleeding and bruising becomes very upsetting to family members, especially grandchildren. But a new technology offer a different approach.
- Catching Clots: Saving the Lives of A-Fib Patients, Ivanhoe News Service. http://search.ivanhoe.com/channels/p_channelstory.cfm?storyid=32806&channelid=CHAN-100010. Accessed 8 February 2014.
- Photo by shutterstock.com
- Photo courtesy of adamci by FreeImages : www.freeimages.com/photo/71005


Your thoughts on this