Scores




Stroke is the fifth leading cause of death in the United States, killing more than 130,000 Americans each year, which is 1 of every 20 deaths. According to CDC data[1], every year, about 795,000 people in the United States have a stroke. About 610,000 of these are first or new strokes, while 185,000 are recurrent strokes. A leading risk factor for stroke is atrial fibrillation, a type of irregular heartbeat (arrhythmia), which affects an estimated 2.2 million people in the U.S.
Normal heart contracts and relaxes to a regular beat. But, in atrial fibrillation, the upper chambers of the heart (the atria) beat irregularly (quiver) instead of beating effectively to move blood into the ventricles. This can cause blood to collect in the heart and potentially form a clot, which can break off and travel to a person’s brain, causing a stroke. It's estimated that about 15–20 percent of stroke sufferers also have atrial fibrillation.
Most common symptoms of atrial fibrillation are palpitations in the chest area, with sensations of a racing, uncomfortable, irregular heartbeat or a flip-flopping in your chest, usually followed by shortness of breath. Some patients may experience weakness, fatigue, lightheadedness or dizziness.
However, atrial fibrillation is often asymptomatic, so most people actually don't know that they have it. They usually find out about their condition on regular checkups, but they still don't consider it a serious condition, although untreated atrial fibrillation doubles the risk of heart-related deaths and is associated with a 5-fold increased risk for stroke. This risk of developing clots that may cause stroke is a reason why patients with atrial fibrillation are put on blood thinners, such as warfarin.
Recently, there was a case of 67-year-old female with a medical history of mild hypertension and Type II diabetes. She was diagnosed with atrial fibrillation while undergoing a routine checkup. The patient was asymptomatic and was unaware she has Afib. She was taking Aspirin preventively tho, but the new diagnose required new medications. Warfarin is the first choice, but would target-specific oral anticoagulant (TSOAC) be better for her, especially knowing how complex monitoring and dosage adjustments for Warfarin are, as well as drug interactions and potential side effects such as gastrointestinal bleeding or hemorrhagic stroke? If you decide to keep up with Warfarin, how would you adjust it?
These are types of questions you'll have to answer often, each time you admit patients with diagnoses requiring an anticoagulant therapy.
Fortunately, the University of Michigan developed a handy app called MAQI2 Anticoagulation Toolkit, which purpose is to help you answer those questions and simplify the decision-making process.
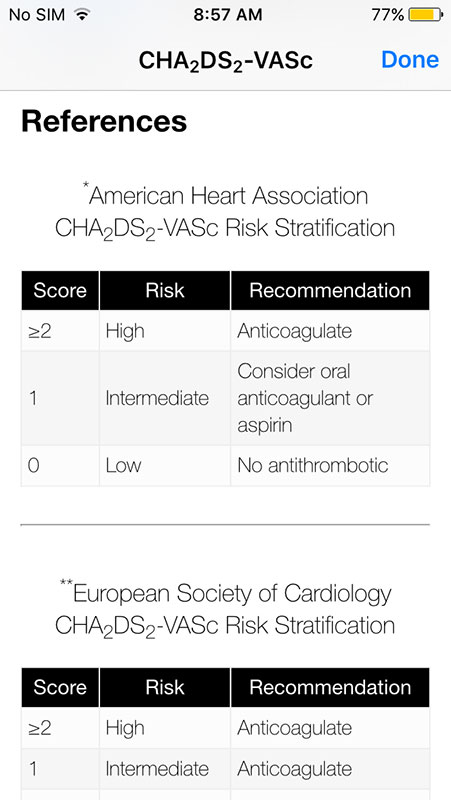
The app is based on Anticoagulation Toolkit PDF, which is available as a resource within the app. Several published guidelines, such as American Heart Association (AHA)/ACC, the European Society of Cardiology, the CHEST guidelines, including a number of clinical trials, also helped shaping the content of this app.
The design of Anticoagulation Toolkit app is simple and straightforward. There are basically few interactive screens that users may switch between by tapping on tabs.
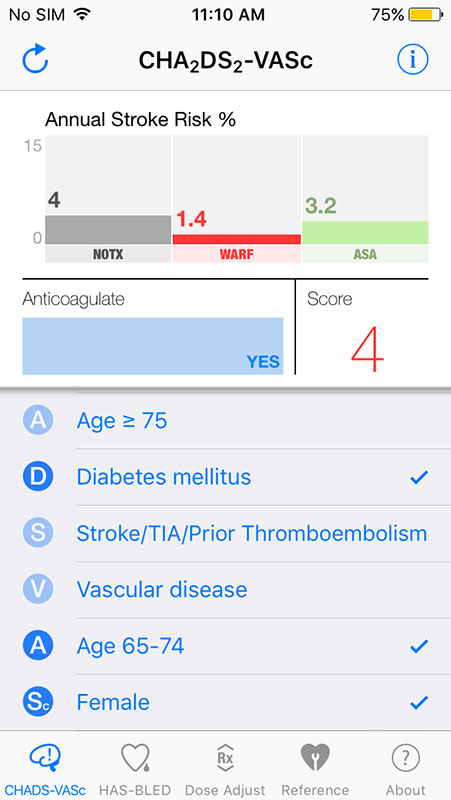
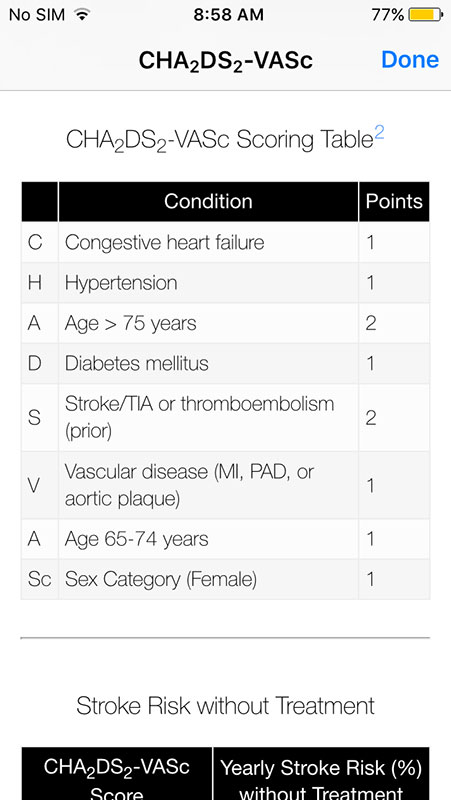
First tab CHA2DS2-VASc provides stroke risk scores, and it is an expansion of the original CHADS2 score, including 3 additional stroke risk factors: age 65-74, female sex, and history of vascular disease. These additional risk factors are believed to more accurately determine stroke risk and the need for anticoagulation in patients with CHADS2 scores of 0 or 1. The CHA2DS2-VASc score is recommended over CHADS2 in the 2014 AHA/ACC/HRS Atrial Fibrillation Guidelines.
Based on our case, i.e. 67-year old patient female patient, with hypertension and type 2 diabetes, we got a score of 4, which indicates a high risk of stroke with recommended anticoagulant therapy.
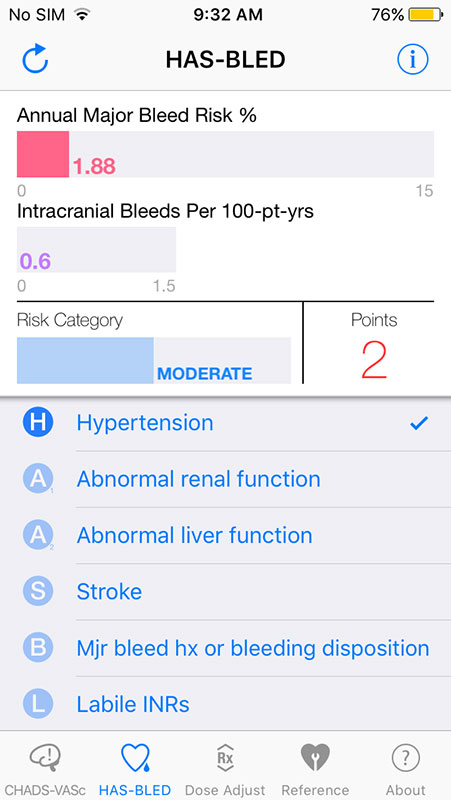
Next HAS-BLED tab estimates the risk of major bleeding for patients on warfarin for atrial fibrillation. Our patient was in moderate risk category with 1.88% annual major bleed risk.
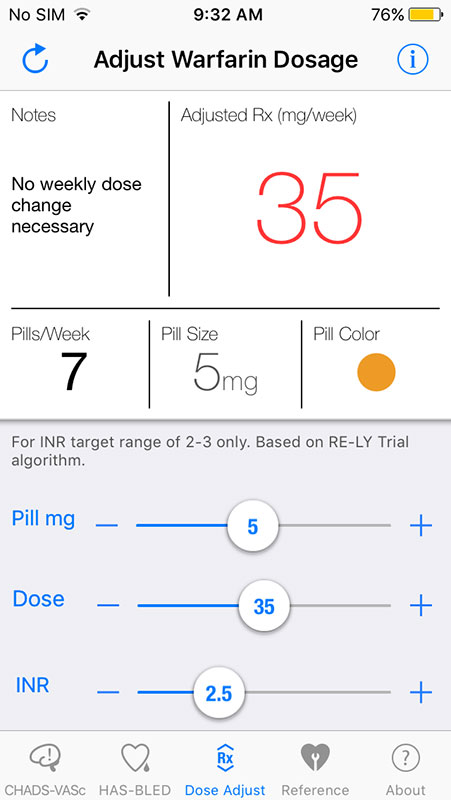
Dose Adjust tab gives info about Warfarin dosage based on results we got so far. Here, you'll also get recommendation if weekly dose changes are necessary. We got a recommendation not to change the dose for our patient, i.e. to keep it on 5mg per day.
Reference tab opens Anticoagulation Toolkit PDF file, which provides more useful information, especially about various risk models, FDA approved anticoagulants and their comparison, choice of anticoagulant based on patient's characteristics, identifying patients appropriate for TSOAC therapy, etc.
It would be much better if this info is provided in a more interactive way, like the rest of this app. Instead, PDF is just a file to read, which can be inconvenient on smaller screens.
Nevertheless, Anticoagulation Toolkit app is an excellent, easy-to-use and well-referenced tool, which provides the most current evidence-based calculators and dosing information on anticoagulants.
Benefit: All health professionals working in Internal Medicine, Emergency Medicine, Cardiology, Family Medicine, or any other providers who prescribe or manage patients on anticoagulants, as well as students and residents, may benefit from this app.
Verdict:
For- Easy-to-use and intuitive interface
- Evidence-based calculators and most current treatment suggestions
- Excellent reference info
- Finally available for Android
- Not much info about the TSOAC in the app
- Anticoagulation Toolkit should be provided in mobile-friendlier format



































Your thoughts on this
Loading...