Scores




The life expectancy from the age of retirement continues to increase, for both men and women, but not all these additional years are spent in good health.
Frailty, a common clinical syndrome which is characterized by age-associated physiological decline and heightened vulnerability to adverse health outcomes, or as The American Geriatrics Society defines it, "a state of increased vulnerability to stressors due to age-related declines in physiologic reserve across neuromuscular, metabolic, and immune systems," remains a significant problem for older adults.
This means that frail older adults are less able to adapt to stressors such as acute illness or trauma than younger or non-frail older adults.
Frailty has been characterized by several indicators/symptoms, including low energy, slowed walking speed, low physical activity, low grip strength, and/or unintentional weight loss.
The increased vulnerability in frail individuals contributes to increased risk for multiple adverse health outcomes, including procedural complications (i.e. after surgeries), falling, institutionalization, disability, and death.
Identification of elderly patients who are frail or at risk of becoming frail is one of the major challenges in clinical practice nowadays, especially geriatric medicine devoted to bringing quality care to the ever-growing elderly population.
General practitioners play a key role in the assessment of frailty. Due to an often busy practice, they need to be supported by screening tools, which should be both user-friendly and time-efficient.
The problem here is that no single definition or assessment test for frailty has been agreed upon, but they are rather provided in numerous clinical tools.
Deciding which tool is the most useful could be challenging for providers, especially when assessing the frailty in elderly patients scheduled for various surgical procedures.
Among seven different frailty tools, the Essential Frailty Toolset (EFT) was found to be the most efficient in predicting of one-year mortality and disability in patients undergoing aortic valve replacement.
The EFT helps providers unravel the association between frailty and mortality during and after surgical procedures.
The advantages of this toolset include the ease of use with only four components, and increasing medical scientific literature supporting its validity.
Frailty Tool app we review today is based on the evidence-based Essential Frailty Toolset (EFT) and designed for providers to easily evaluate frailty and 1-year mortality risk for elderly patients.
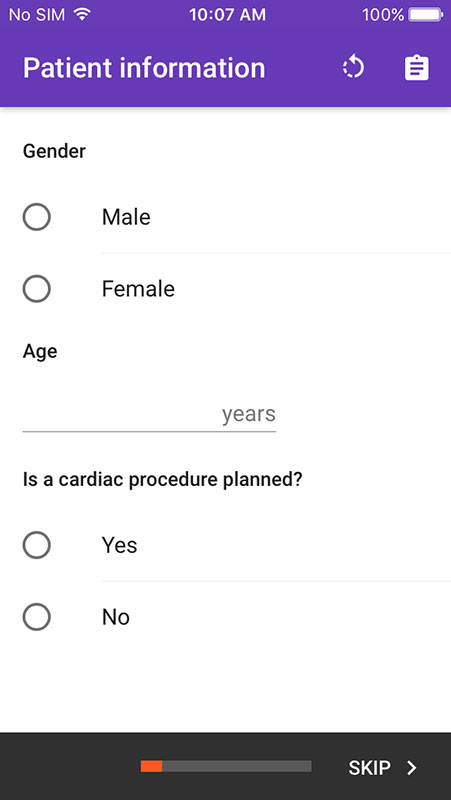
The app is straightforward and easy to use. Upon opening, it would ask providers to enter basic information about their patient, including their age and gender, as well as if a cardiac procedure is planned, and if so, which one, i.e. TAVR, SAVR, mitral surgery, isolated or non-isolated CABG, or other.
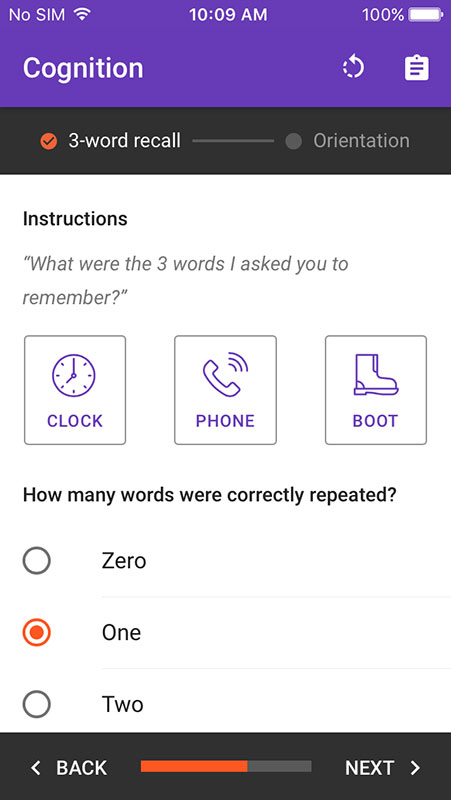
The app would then take a provider through a simple step-by-step guide intended to help administer the Essential Frailty Toolset (EFT). The first step is asking your patient to repeat and remember three words displayed on your phone that you should say to them loud and clear.
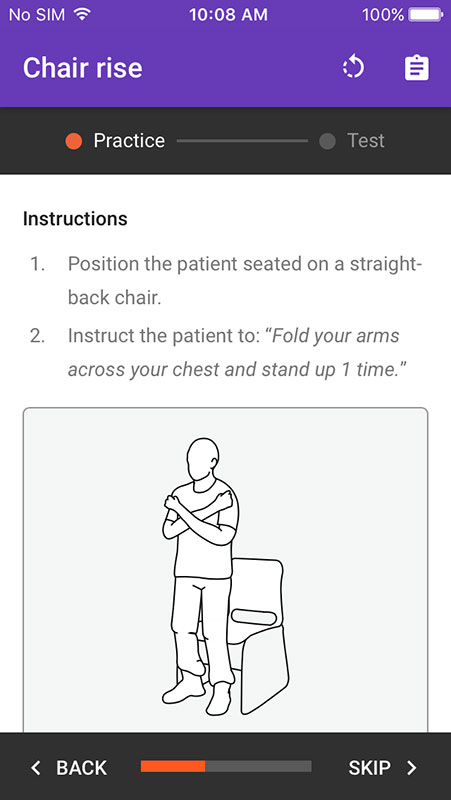
After the patient successfully repeated all three words or three unsuccessful attempts, you can move onto the next step, which is a one chair rise with arms folded across the chest.
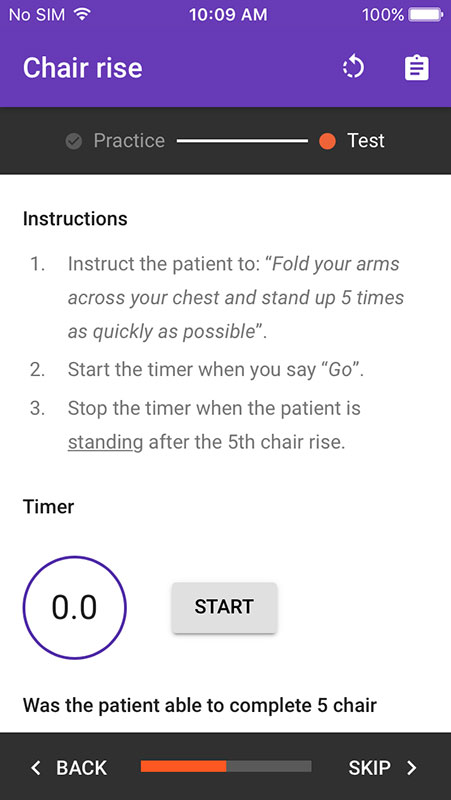
Next step is asking your patient to repeat chair rise five times. There's also a timer that measures the time needed for completing this step.
After this step, you need to test patient's cognition by asking them to repeat three words you asked them to remember and mark the number of words correctly repeated. You'd then test their orientation by asking your patient what day of the week and month is it, and to say if they know their current location, i.e. hospital and floor.
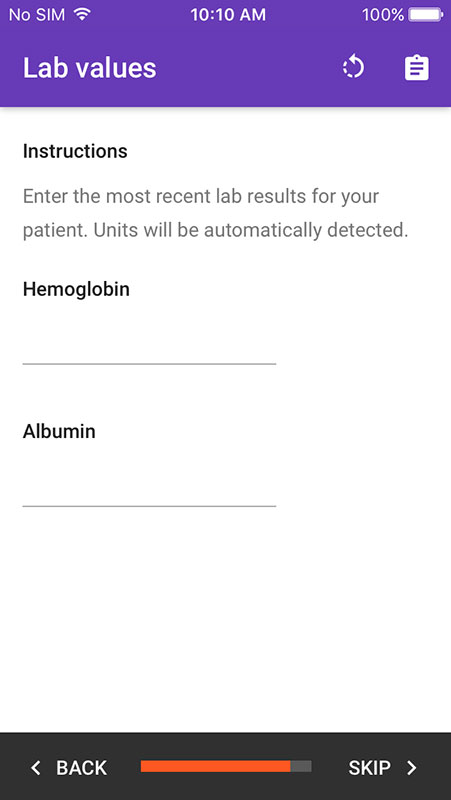
Finally, the providers need to enter the most recent lab values for their patient, i.e. hemoglobin and albumin.
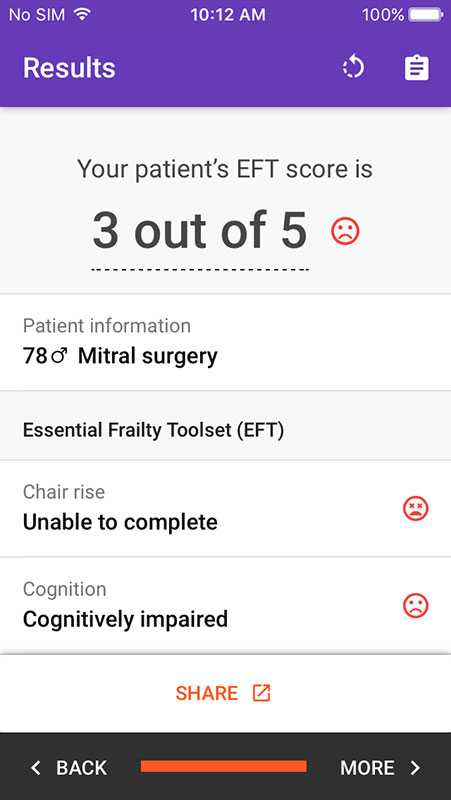
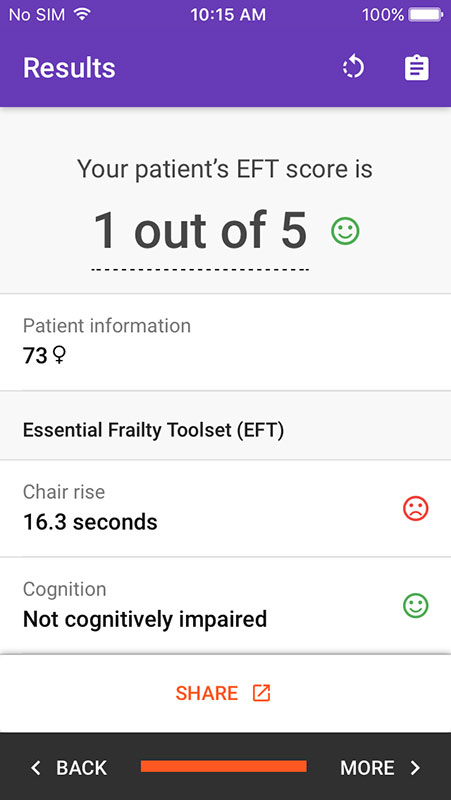
Based on the data provided, the built-in calculator will automatically compute EFT Score and 1-year mortality risk for your patient.
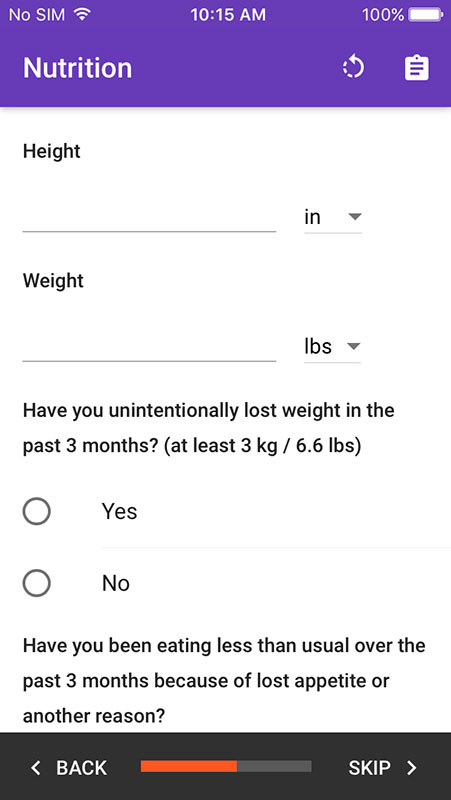
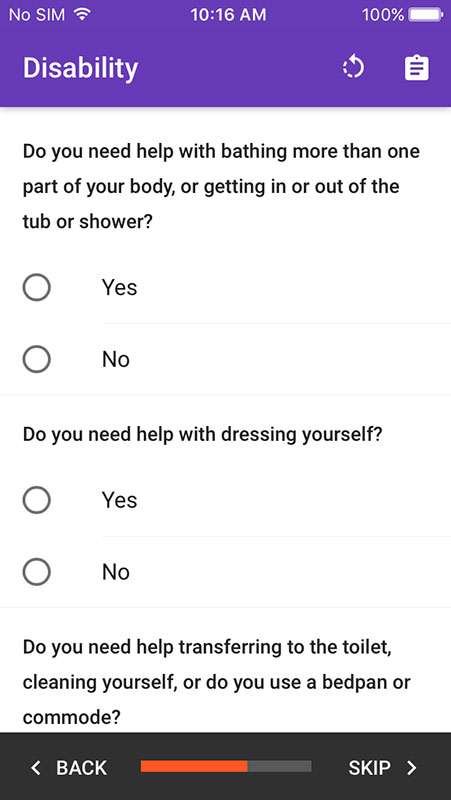
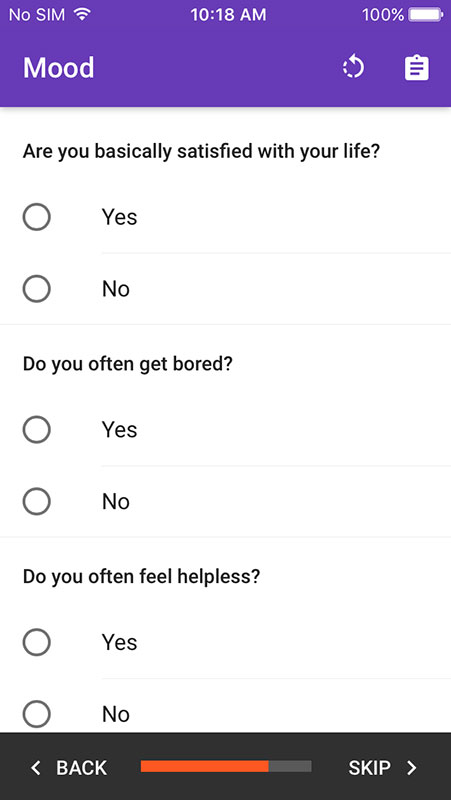
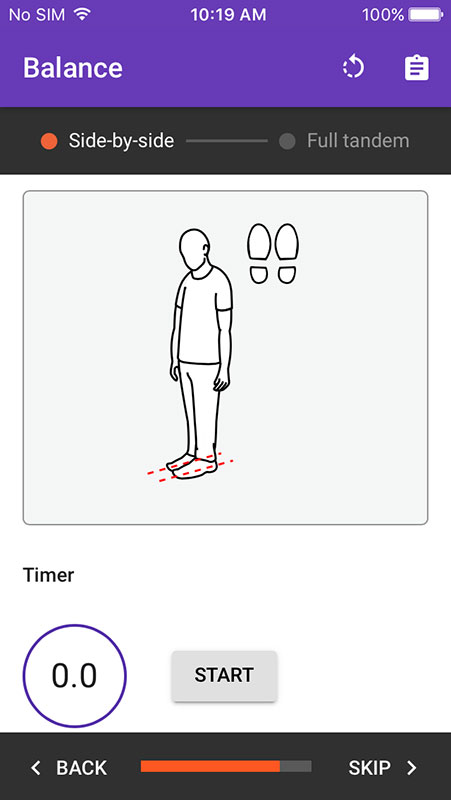
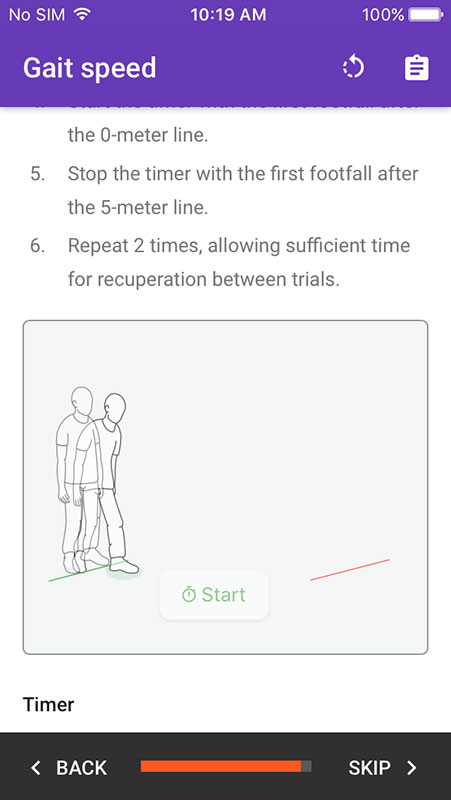
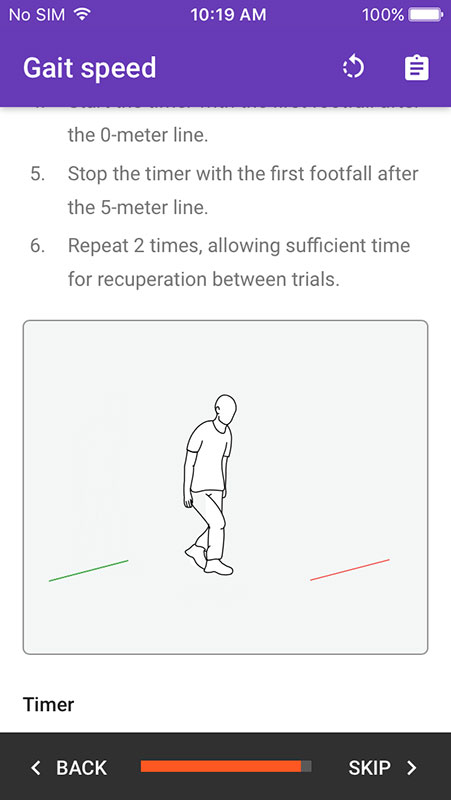
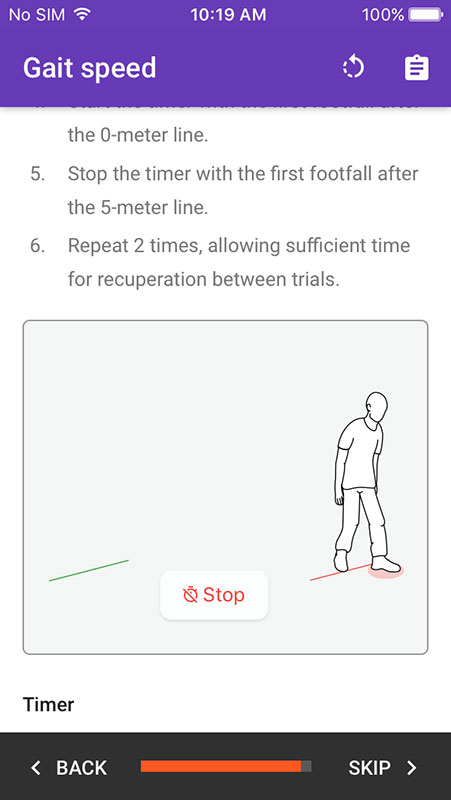
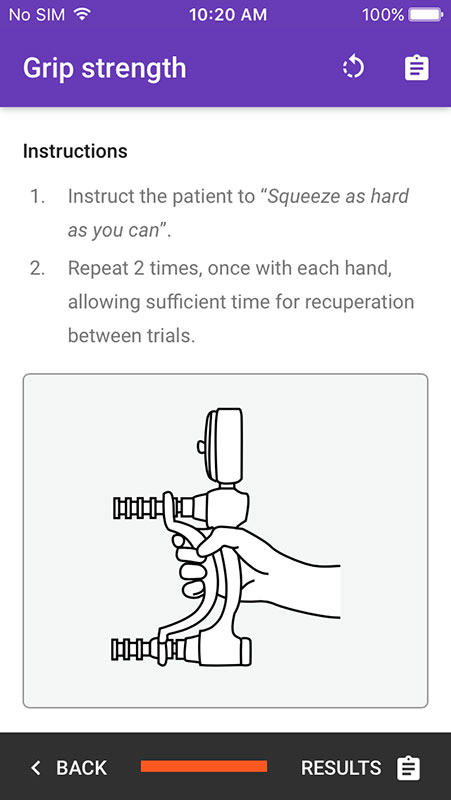
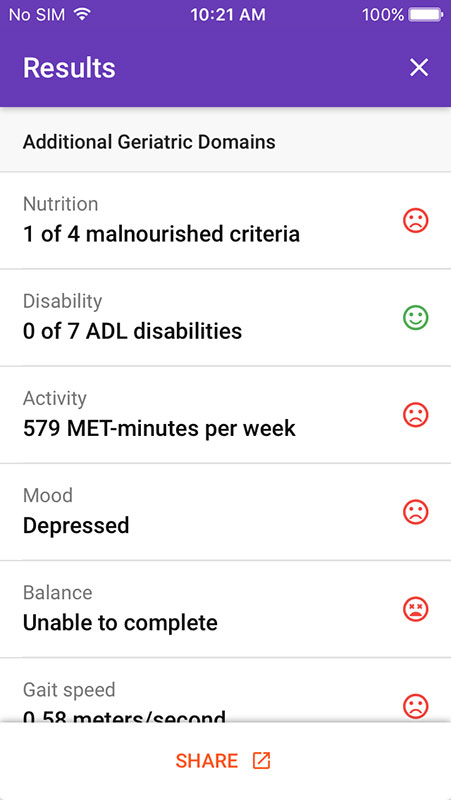
Providers can continue with the expanded toolset which includes additional indicators for nutrition (height, weight, weight loss, etc.), disability, activity, mood, balance, gait speed, and grip strength. It would add results to the previous score, alongside the recommendations for treatment.
The main advantage of Frailty Tool app is the fact that it calculates the scores based on valid and evidence-based Essential Frailty Toolset (EFT), as well as expanded EFT.
However, the app lacks any additional information about the supporting literature, the Essential Frailty Toolset (EFT), or how to use the score, so providers unfamiliar with the scale may have trouble understanding it.
The app is available in English and French languages, and that's another great thing about it.
Overall, Frailty Tool app is a useful evidence-based guide and a calculator that enables healthcare providers and surgeons to calculate the 1-year mortality risk from common cardiovascular procedures due to a underlying frailty in geriatric patients.
Providers can use the app with patients and their families at the point of care to discuss the best options for their patients, i.e. surgical vs. non-surgical.
Benefit: Healthcare providers who care for geriatric patients, providers performing pre-op evaluations, as well as surgeons would benefit from this app.
Verdict:
For- Simple guide to EFT with easy-to-use calculator that predicts 1-year mortality
- Guide is supported by timer and instructional illustrations
- Expanded toolset includes additional indicators
- Available in English and French
- The app lacks any information about the supporting literature, the Essential Frailty Toolset, or how to use the score






































Your thoughts on this
Loading...