Scores




Psychopharmacology is the scientific study describing the use of medications in treating mental disorders.
The complexity of the field requires continuous learning in order to keep current with new advances, as well as an extensive understanding of basic psychopharmacology, basic neuroscience, clinical medicine, the differential diagnosis of mental disorders, and treatment options.
Psychopharmacologists are required to understand all the clinically relevant principles of pharmacokinetics, i.e. what the body does to medication, as well as pharmacodynamics, i.e. what the medications do to the body.
This particularly refers to understanding the potential benefits and adverse effects of different pharmacotherapeutic agents prescribed for the range of cognitive and emotional conditions and possessing the diagnostic and treatment skills as applied to the selective use of psychotherapies.
Psychopharmacologists also must be capable of building and utilizing an effective communication with their patients regarding the therapy.
Basically, any physician who treats patients with psychotropic medication can be called a psychopharmacologist. This includes physicians who have a high level of understanding and expertise in pharmacology, including psychopharmacology, as well as psychiatrists who have an even higher level of understanding and expertise in psychopharmacology.
Selecting and using psychotherapeutic agents for a therapy of mental conditions is complex, so both physicians and psychiatrists could benefit from algorithms and tools that could support the decision-making process.
Use of algorithms in medical practice is valuable to help avoid the cognitive lapses which are common when solving problems which rely on uncertain data or many possible choices that could influence the decision-making process.
PsychoPharm Research app was created to solve this problem. Developed by Joongheum Park MD, an internal medical physician, the app aims to provide a mobile, interactive version of medical decision support trees for psychopharmacology developed by the Psychopharmacology Algorithm Project at the Harvard Medical School Department of Psychiatry, which is founded by Dr. David Osser, an Associate Professor of Psychiatry at Harvard Medical School.
PsychoPharm Research app is available for free download and use, however, only for iOS devices.
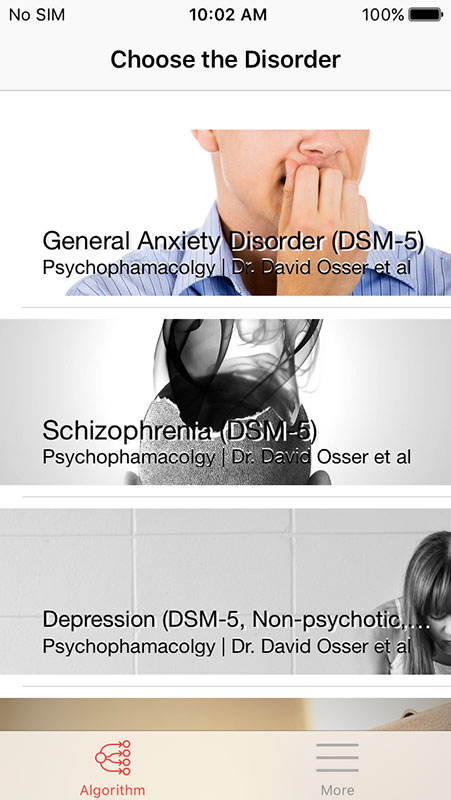
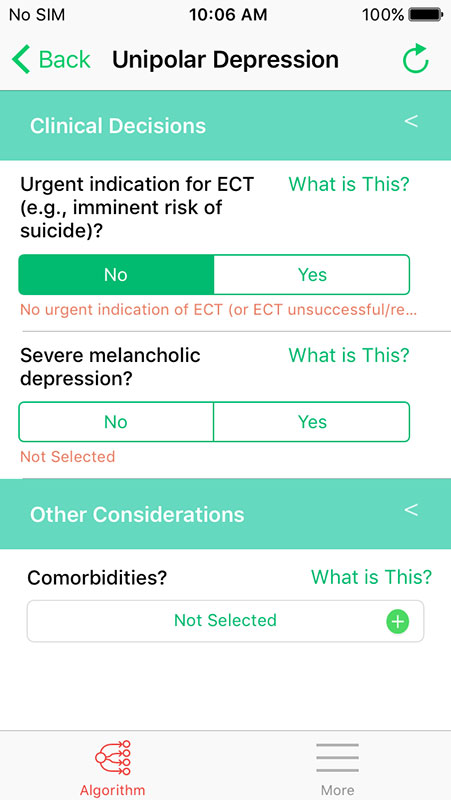
Upon opening the app, you'd notice its clean and simple design. The app's functionality is also straightforward.
There are four sections on the main page covering four major psychiatric conditions, including General Anxiety Disorder, Schizophrenia, Depression, and Bipolar Mania, which is still not available (under development).
Each of these sections contains easy-to-use decision support trees based on evidence-based algorithms, tailored to help psychopharmacists decide on the first line of therapy for patients with major psychiatric complaints, as well as to solve those cases where it is necessary to change therapy after the first and second line treatments have failed or given insufficient benefit.
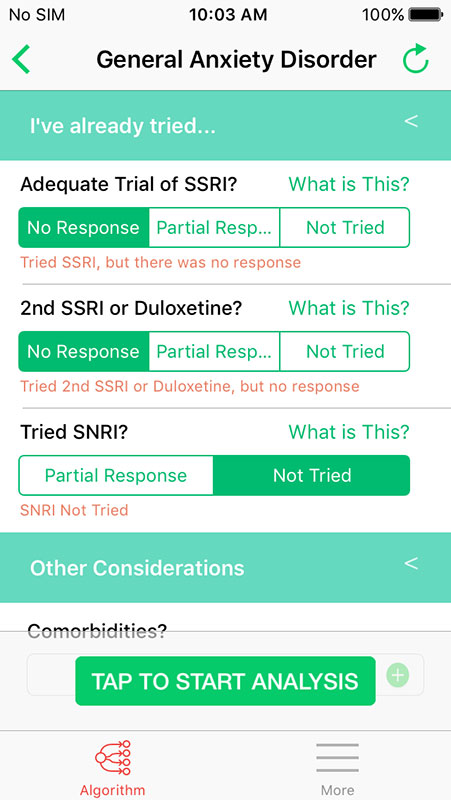
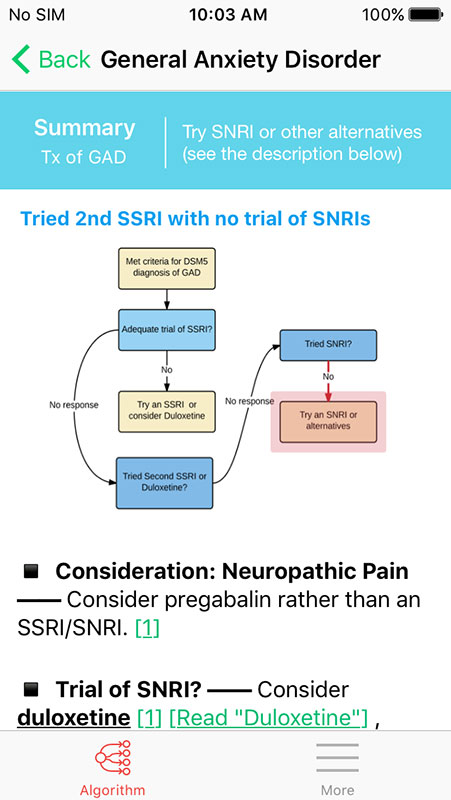
For example, in the General Anxiety Disorder section, providers will be first asked about the options they tried, such as an adequate trial of selective serotonin reuptake inhibitors (SSRIs), either trial or as the 2nd line with Duloxetine, or serotonin-norepinephrine reuptake inhibitors (SNRIs).
Each question can be answered with multiple-choice options, usually with No response, Partial response, and Not tried.
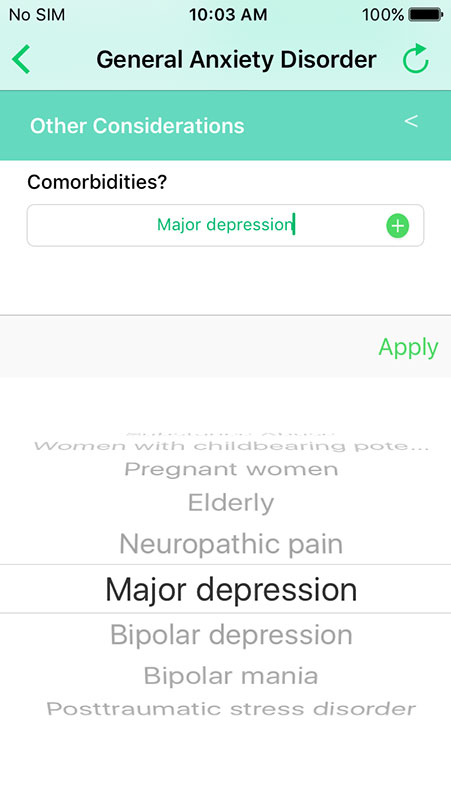
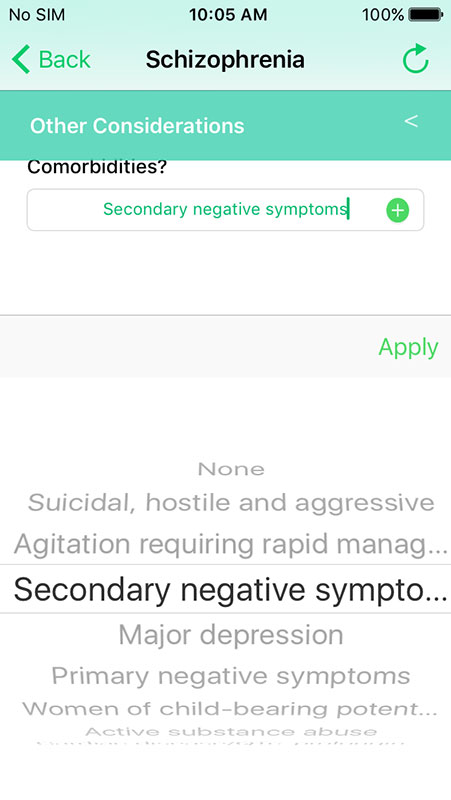
Providers can also add other considerations, i.e. comorbidities, such as substance abuse, pregnancy, advanced age, neuropathic pain, and more.
After completing all steps, users should tap on the green button that generates after choosing a sufficient number of options. The app then opens a new page with an algorithm displayed, as well as further considerations and medication information, which is interlinked.
All information provided in the app is well-referenced and linked to resource materials at various websites, including PsychoPharm website, NCBI NIH, Google Scholar, etc.
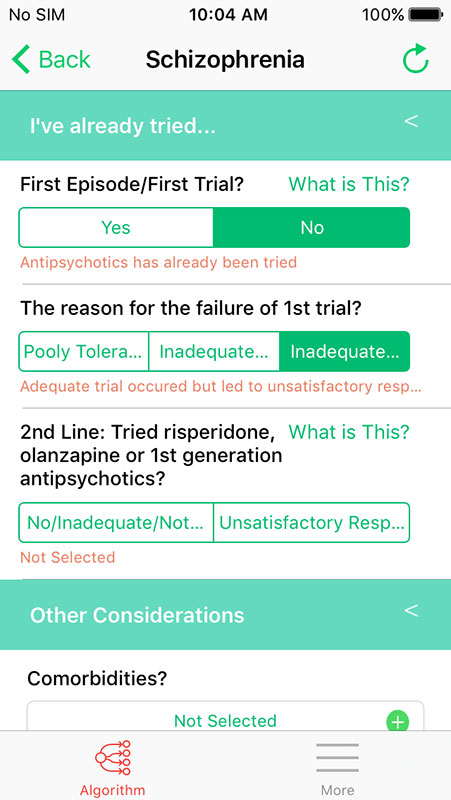
In a similar fashion, providers will be taken through the other two algorithms. For schizophrenia, providers would be asked if there was a first trial, the reasons for the failure of the first trial, if they tried 2nd line with risperidone, olanzapine, or first-generation antipsychotics, or 3rd line if the 2nd line gave an unsatisfactory response, or if they tried augmenting it with other drugs.
Algorithm for Depression requires answering questions if a patient is at risk of suicide or suffering from severe melancholic depression if there was an adequate trial of SSRIs, or venlafaxine or mirtazapine if there's a melancholic depression, if atypical features are present, and so on.
Everything works smoothly in the PsychoPharm Research app' thanks to its easy-to-use interface that enables physicians and psychiatrists making quick decisions at the point of care, although the app creator advises against it. He suggests using the app for educational purposes only.
I would, however, recommend PsychoPharm Research app as a must-have tool for any primary care physician and psychiatrist who need to make important decisions on first, second and third line treatment options for patients with depression, schizophrenia or general anxiety disorders.
Benefit: Any physician who treats patients with psychotropic medication would benefit from this app, particularly psychiatrists and primary care physicians
Verdict:
For- Easy to use
- Interactive decision support trees for treatment of major psychiatric conditions
- Well-referenced and evidence-based resource
- Not available for Android







































Your thoughts on this
Loading...