Scores




Substance misuse (or abuse) can be defined as the use of alcohol or drugs in a manner, situation, amount, or frequency that could cause harm to the user or to those around them (their families, partners, friends, etc.).
Alcohol and drug abuse and related substance use disorders affect millions of Americans and force enormous costs on our society. The financials, however, are not the only reason for concern. The bigger problem is the public health.
It is estimated that every day, more than 115 Americans die after overdosing on opioids, including prescription pain relievers, heroin, and synthetic opioids such as fentanyl. Drug overdose fatalities reached a record of 52,404 deaths in 2015 and have gone up another 21 percent in 2016.
There are indications that alcohol abuse is on the upswing again, at least among middle-aged Americans. It kills far more Americans than opioid use disorder, contributing to 88,000 deaths in the United States each year.
The medical system has been struggling to effectively combat the substance abuse epidemic for years. But despite all the efforts, more people are dying from drug and alcohol abuse than motor vehicle accidents.
Obviously, this problem is in desperate need of new solutions and approaches, especially in primary care clinics and emergency departments.
Overcoming substance abuse disorders and addiction is complex and requires a multidisciplinary approach, a comprehensive support system, and access to the best tools available.
With the help of such holistic approach, which includes abstinence from substance use, therapies to address co-occurring conditions, and developing healthy coping skills, recovery is possible.
A comprehensive support system from family, friends, and healthcare professionals also plays an important role in recovery.
Of course, patients also need to be activated in their recovery process. Brief, point-of-care interventions including shared decision making and motivational interviewing, have been gaining a lot of attention and research in recent years.
One of the most popular tools for this purpose is SBIRT, which is short for Screening, Brief Intervention, and Referral to Treatment for Substance Use.
SBIRT is a comprehensive, evidence-based approach to the delivery of early intervention and treatment to help identify and reduce dependence on alcohol and illicit drugs.
It is designed for health and social care workers helping them reach individuals who use substances, including those who may not yet meet criteria for alcohol or drug use disorders.
Components of SBIRT include screening for hazardous drinking and drug use and associated problems, delivering brief motivational interviewing-based interventions for patients (at low to moderate risk), and providing information on addiction specialty care for patients with significant problems.
Though SBIRT is a widely-trained and readily available skill, it failed to reach the expectations, because trainees often demonstrate classroom skill proficiency, but fail to use SBIRT in clinical settings.
The solution may be using the point-of-care mobile apps that could help providers learn how to use the method and apply newly learned SBIRT skills.
One of these apps was created by the University of California San Francisco (UCSF) in partnership with the Substance Abuse and Mental Health Services Administration (SAMHSA), and it's called OHN SBIRT app.
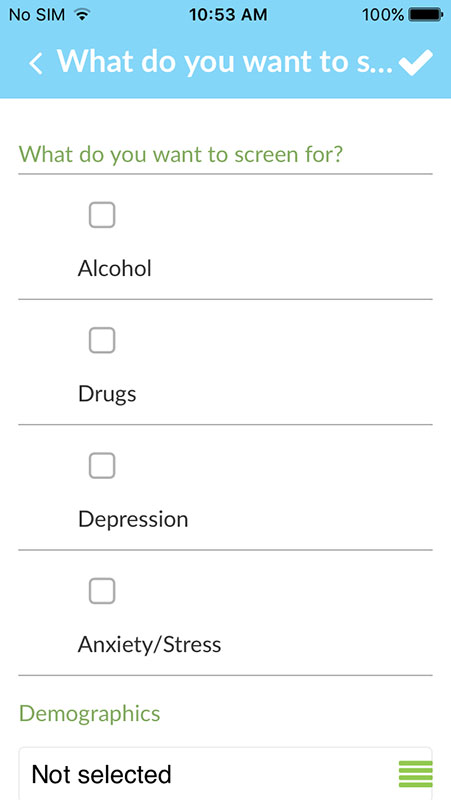
The app makes it easy for healthcare providers to use clinically validated SBIRT method, including questionnaires to screen patients for alcohol or substance abuse, as well as for depression or anxiety, and guidelines for intervention and referral when appropriate.
OHN SBIRT app requires users to log in or register an account, if they don't have one, by providing a couple of details about themselves and their job.
Upon downloading and setting things up, the app would open the homepage that features four sections, including Review, Apply, Reports, and Tools.
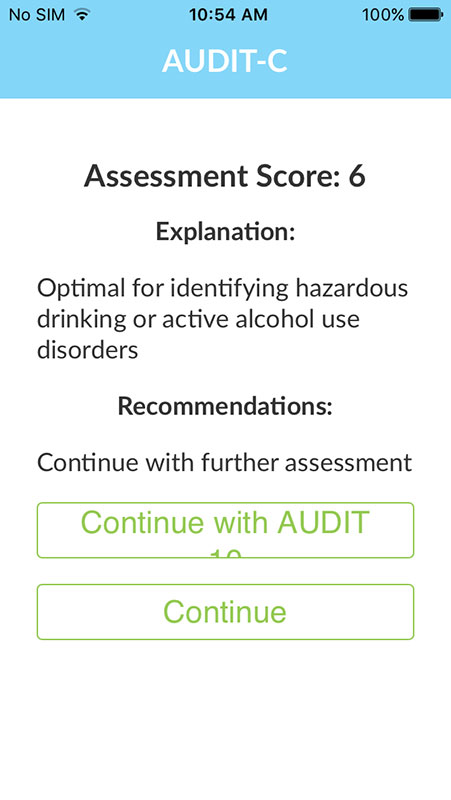
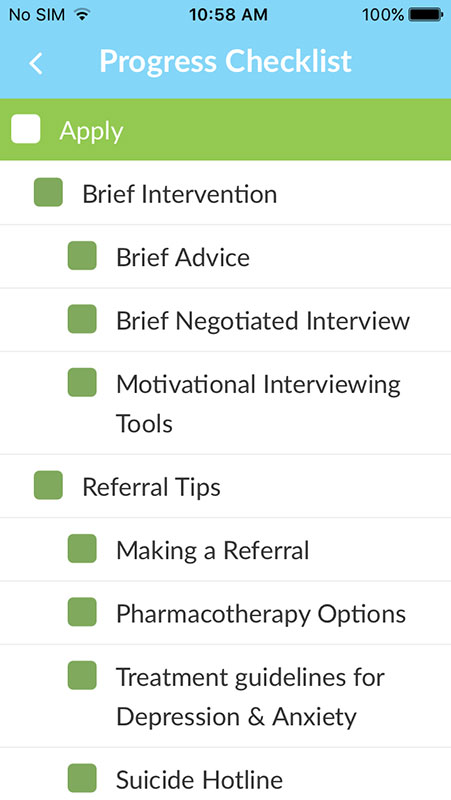
The OHN SBIRT app basically walk users through each step of typical SBIRT interaction from patient screening to brief intervention and referral to treatment and then help them apply the method to their clinical practice.
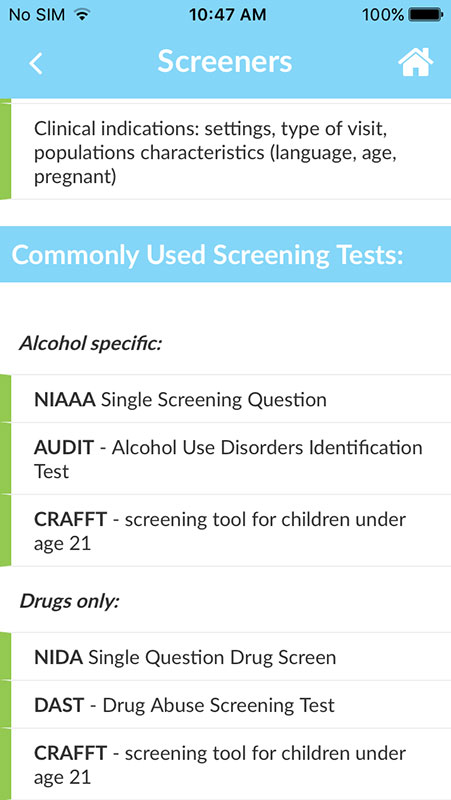
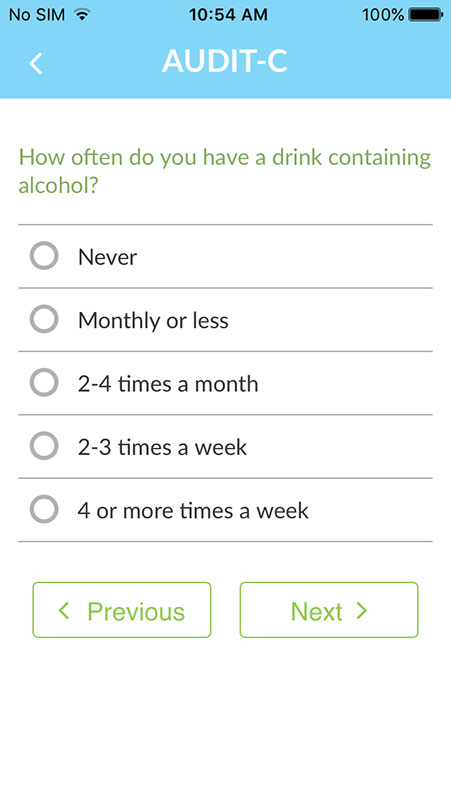
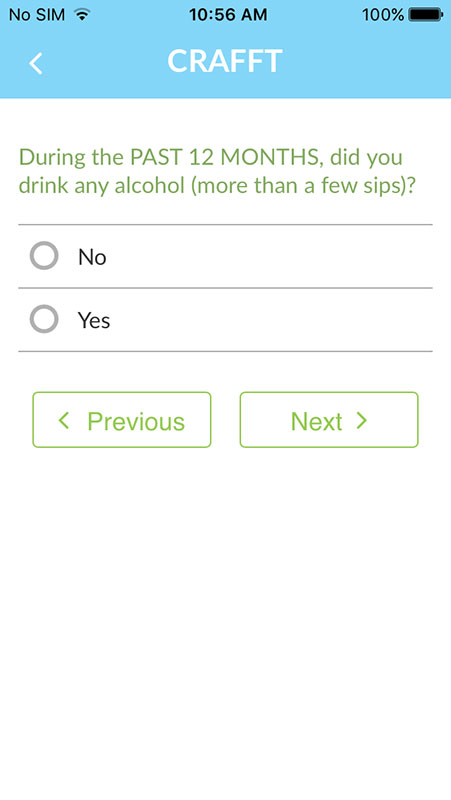
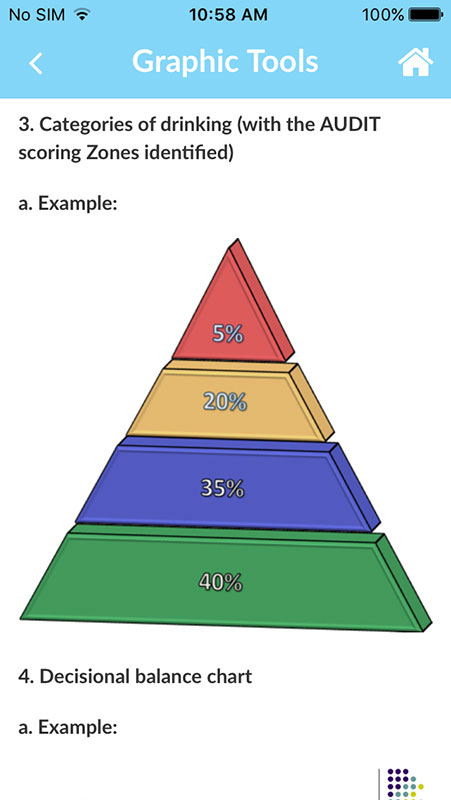
It also provides a lot of background information, such as the evidence behind the SBIRT methodology (the app uses validated screening tools such as the AUDIT, DAST, and CRAFFT), or the information on the current epidemiology of alcohol and drug abuse, helping users understand the substance abuse crisis plaguing the population.
The app also provides social support and follow-up questionnaires at the end of the app that allow providers trained in SBIRT to track their progress.
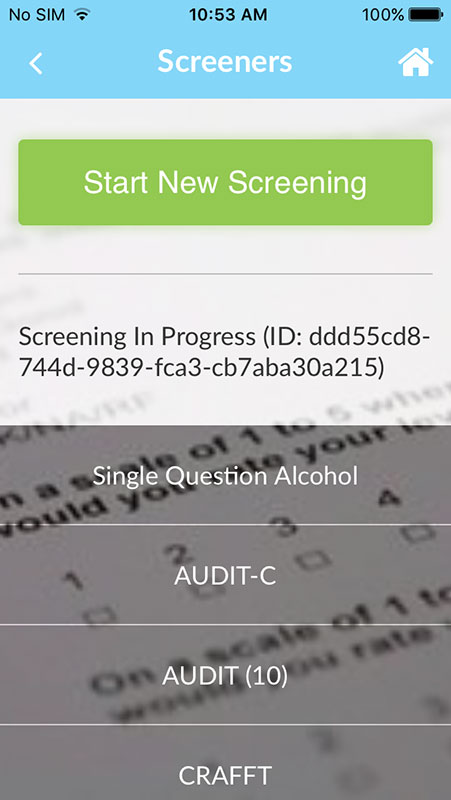
OHN SBIRT app can be used as the point of care tool because it has built-in screening sections making it easy to use the app at a patient's bedside, even if you don't have extensive SBIRT training.
Overall, OHN SBIRT app is an indispensable tool for all providers who have received training in SBIRT, but it can be useful even to novice users to guide them step-by-step through the SBIRT interaction at the point of care.
Benefit: This is a valuable app for all healthcare providers who may identify problematic substance use and need to provide screening services to their patients, to intervene and refer them to the treatment services
Verdict:
For- Easy-to-use interface that guides users through the entire SBIRT interaction
- Utilizes a validated and evidence-based approach to substance use
- Includes videos and narrated modules explaining SBIRT evaluations
- Links to referral centers and social support
- Not available for Android






















































Your thoughts on this
Loading...