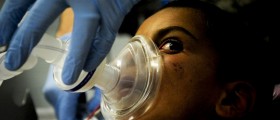
A research team from Georgetown University Medical Center conducted the study, funded by the National Multiple Sclerosis Society and the National Institutes of Health and found that certain general anesthesia drugs decreased feelings of pain during surgery but caused pain afterward.
The researchers discovered that it is the noxious type of anesthesia that causes inflammation and discomfort during the post-surgical recovery period. This type of drug, used in most general anesthetics, acts on the peripheral nervous system while others act on the central nervous system (the brain and spinal cord) instead.
The research team focused on two receptors specific to nerve cells in the peripheral nervous system - TRPV1 and TRPA1. These two receptors are usually triggered at the same time and can be stimulated by eating foods such as garlic, wasabi, and mustard. Most forms of general anesthetic drugs activate this mustard-oil receptor.
The researchers found direct involvement between general anesthetic drugs and TRPA1 when laboratory mice with no TRPA1 genes experienced no pain or inflammation when under the influence of these drugs.
Inflammation in the nerves was greater when the general anesthetic used is a pungent chemical irritant instead of a non-pungent inhaled drug.
When these drugs are administered, many chemicals get released throughout the body. This process recruits immune cells to the affected tissue generating inflammation and pain even after a patient wakes from surgery.
The researchers believe that these findings will make room for improvement when administering general anesthetic drugs. Not all such drugs activate TRPA1 but those that don’t may prove to be less effective.
The researchers discovered that it is the noxious type of anesthesia that causes inflammation and discomfort during the post-surgical recovery period. This type of drug, used in most general anesthetics, acts on the peripheral nervous system while others act on the central nervous system (the brain and spinal cord) instead.
The research team focused on two receptors specific to nerve cells in the peripheral nervous system - TRPV1 and TRPA1. These two receptors are usually triggered at the same time and can be stimulated by eating foods such as garlic, wasabi, and mustard. Most forms of general anesthetic drugs activate this mustard-oil receptor.
The researchers found direct involvement between general anesthetic drugs and TRPA1 when laboratory mice with no TRPA1 genes experienced no pain or inflammation when under the influence of these drugs.
Inflammation in the nerves was greater when the general anesthetic used is a pungent chemical irritant instead of a non-pungent inhaled drug.
When these drugs are administered, many chemicals get released throughout the body. This process recruits immune cells to the affected tissue generating inflammation and pain even after a patient wakes from surgery.
The researchers believe that these findings will make room for improvement when administering general anesthetic drugs. Not all such drugs activate TRPA1 but those that don’t may prove to be less effective.
Loading...