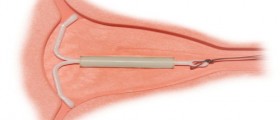
An intrauterine device is an excellent and very effective contraceptive method with a low failure rate. It is a small T-shaped device inserted in to the uterine cavity.
Intrauterine devices are the preferred method of contraception immediately after delivery. After delivery, the uterus is very thick and the chance of perforation during insertion is very small. Lochia is a straw colored/blood stained discharge from the placental site. This discharge is profuse soon after delivery and it actually washes off potentially harmful microorganisms, thus preventing pelvic inflammatory disease. Actual placement soon after delivery is very easy for the obstetrician.
Many women prefer an intrauterine device to oral contraceptive tablets simply because of the convenience. The failure rate due to non-compliance is the biggest drawback of the pill. Hormone-impregnated implants have the same convenience. But some women may get excessive menstrual bleeding with hormonal intrauterine devices.
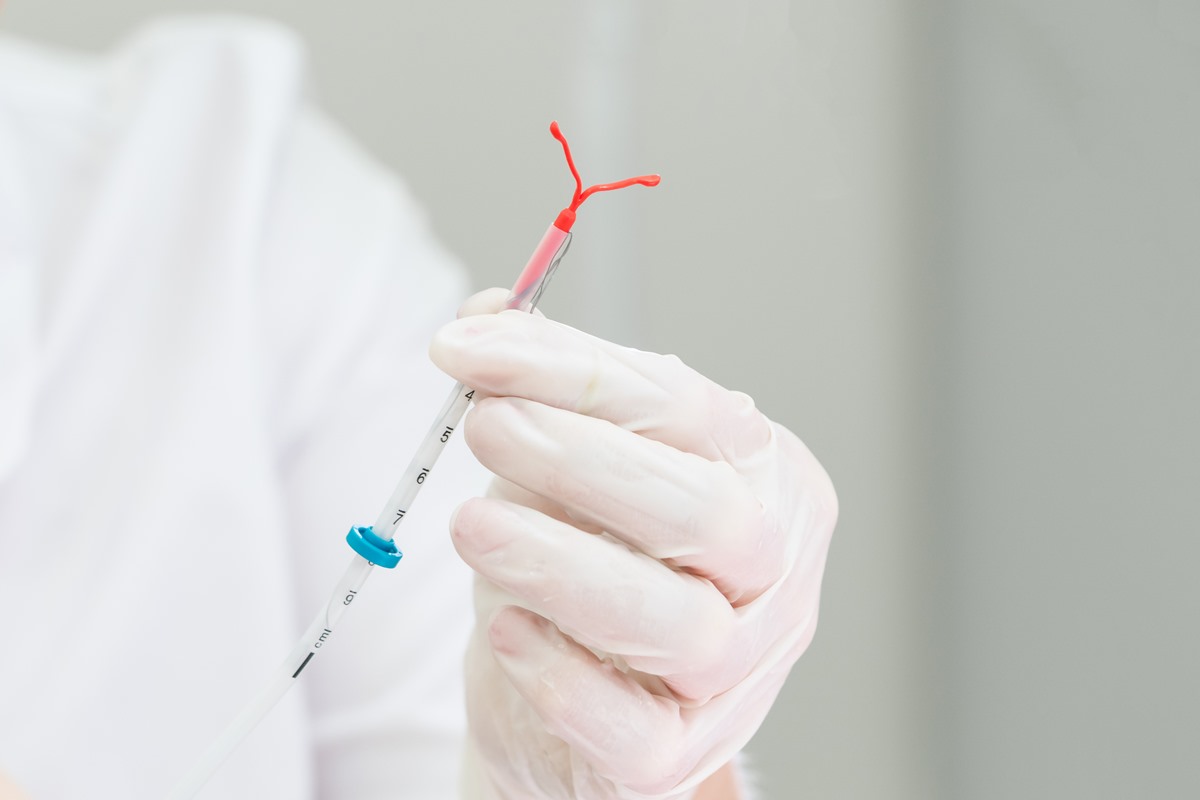
The position of the intrauterine device is of critical importance. The gynecologist uses a speculum to insert the intrauterine device. The T-shaped part should be placed against the uterine fundus with the ends of the two arms of the T in the two cornua. Cornua are the two corners where the two fallopian tubes join the uterus. The pacient should be able to feel the IUD's string.
There are various types of intrauterine devices. Generally intra uterine contraceptive devices can be categorized as non-hormonal and hormonal. Non-hormonal intrauterine devices are very cheap. They do not interfere with the menstrual cycle. After the usual period of lactation related amenorrhea, menstruation will recommence. Hormone-releasing types have the additional effect of inhibiting the menstrual cycle. Women who suffered from severe endometriosis benefit from this type of intrauterine device.
Both types of intrauterine device may host infections. Pelvic inflammatory disease is the result. It presents as lower abdominal pain, pain during sex, fever, nausea and vomiting. There can be a foul-smelling or just smelly discharge also.
Urinary tract infections commonly accompany pelvic inflammatory disease. Dysuria may divert the doctor's line of thought. An examination to confirm the absence of any visible cervical lesion is a must. A pap smear, human papillomavirus screening, a high vaginal swab for culture, full urine report and urine culture are essential investigations.
An ultrasound scan may show a thin layer of free fluid in the pouch of Douglas. This fluid is the inflammatory exudate. A course of antibiotics and pain killers usually settles the matter.
Any lower abdominal pain should be investigated. Vaginal discharge may suggest something sinister like cervical cancer. Get a pap smear done at least annually. Dysuria may also be due to urinary calculus. A full urine report is a reliable investigation. Excessive irregular bleeding may be due to endometrial cancer. Get an ultrasound scan to measure the endometrial thickness. Consult your gynecologist regularly.
- "IUD (intrauterine device)". Contraception guide. NHS Choices. Retrieved 2 March 2014. "the intrauterine device, or IUD (sometimes called a coil)"
- Photo courtesy of SteadyHealth