Scores




Overview
The Human Dx Project is a platform designed to be a world-wide solution for physicians to consult with each other about difficult diseases. Inspired by projects like the Human Genome Project, the main aim of this application is to create specific algorithms that can create a comprehensive diagnosis based on the most common symptoms present in each case.
Features
When a user downloads the app, it is a very simple process of creating a profile. A user will need to verify their telephone number and then input a code sent via text message to verify their account. Once you get that far, you arrive at a page where you are required to enter your credentials and select the community and clinical role you are involved with.
Various options in the community are possible from the pull-down menu and users are able to select from groups such as physicians or medical students, nursing staff, and pharmacists so consultations can be an aggregation of all pertinent medical information.
This is useful because a nurse may be more of an expert on describing symptoms due to their constant interactions with a patient throughout the day while a pharmacist can comment on the most common medications used to treat each disease as well as some of the most common side effects to educate patients on prior to writing a prescription.
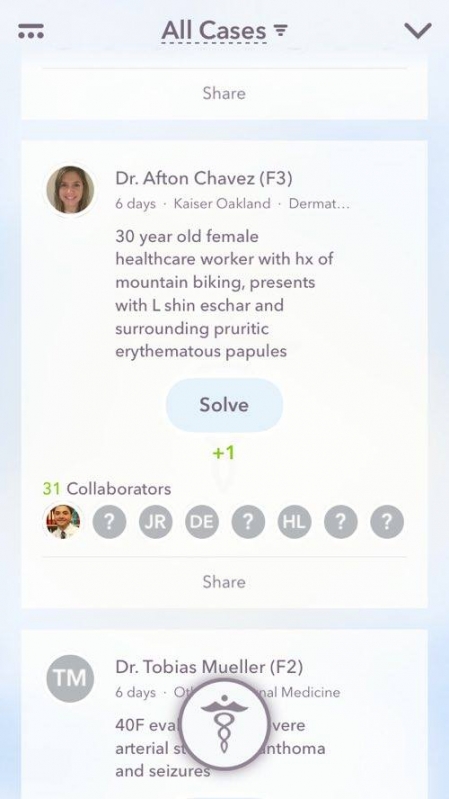
Once you maneuver through the background information, you will come to a page where you are able to either input patient information to help solve a case you are struggling with or solve cases poses by other colleagues using this platform.
If you choose to solve cases, you will be directed to a basic prompt and then open a page describing the chief complaint and pertinent findings from the physical examination. After reading through the case, a user is asked to start building their differential diagnoses in order to learn more information about the case. After inputting a few differentials, key lab results are reveals to help you narrow down your differentials or correct them based on new findings.
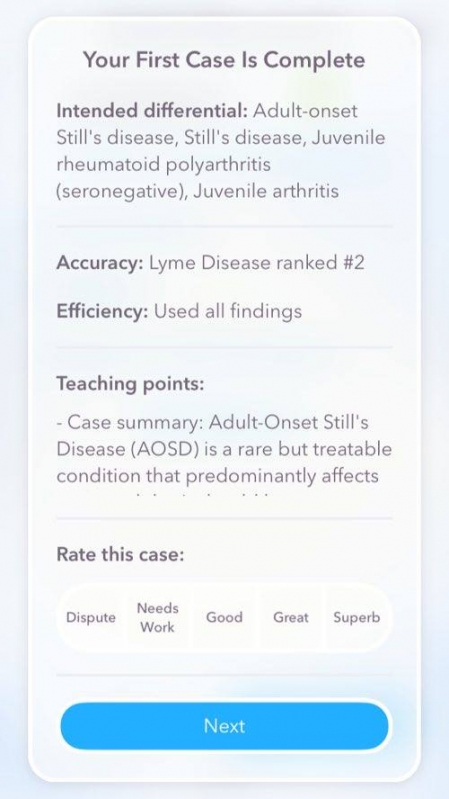
Once you work through the case, you submit your finalized differential diagnoses and then receive a comprehensive breakdown of what other colleagues selected as common differentials based on the presenting information as well as how accurate your problem solving was.
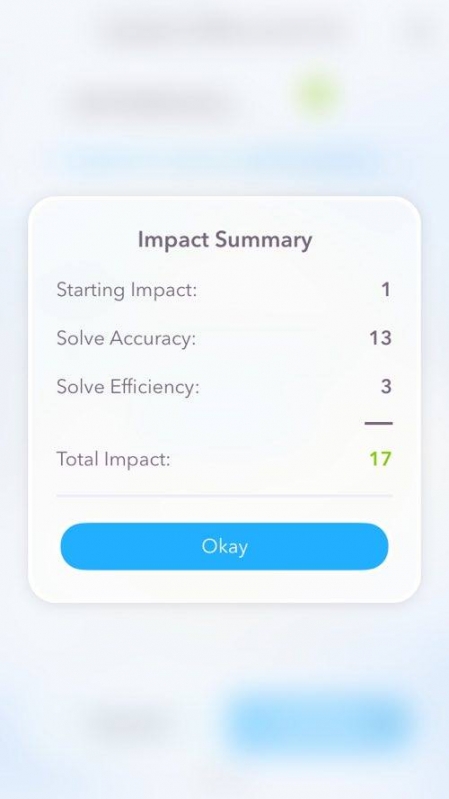
At the end of the case, you receive an impact score out of 20 to rank your effectiveness during the case. This format is a very useful set-up because it helps physicians read through common presentations and open their minds to thinking about other diseases they may not have even considered based on the presentations. The teaching points also help physicians to refresh their understanding of diseases that they may rarely come into contact with based on the departments they are working in.
Having an application that attempts to combine all common symptoms to suggest a specific disease will help create associations for students and young residents to remember to consider this disease based on presenting symptoms.
The set-up of the application is also a good practice to make young physicians think when they are considering possible diagnoses for a patient. There is an unfortunate trend in medicine that patients may be tested with an array of lab studies and diagnostic testing before a physician starts to narrow down what the final diagnosis may be. This can subject patients to harmful radiation or potentially invasive procedures just to give physicians some type of direction for their management.
This may ‘work’ in a system where insurance covers the cost of these procedures but once you start to consider co-payment cases or countries that may not have the financial flexible to afford all these tests, physicians are forced to think much more critically in order to order tests that are only absolutely necessary.
I was taught that imaging studies should not be a tool to diagnose a disease, they should be used as a way to determine the level of therapy that a patient would need.
For example, a physician should be able to diagnose pneumothorax with their stethoscopes and percussion and only need a chest X-ray in order to confirm their effectiveness in management, not a scenario where a physician orders a chest X-ray and sees it for the first time and then begins their management.
If a physician is able to associate specific presentations with a disease, they will be able arrive at a diagnosis more rapidly and cut down on time until management and even potentially the length of time a patient must stay hospitalized.
Verdict:
For- Helps physicians collaborate on difficult cases to help patients .
- It is free and easy to use.
- Useful tool for medical students or young residents to study new material.
- Good to see how your diagnostic skills are compared to colleagues using the platform to determine areas you still need to improve on .
- Useful to have a database of common symptoms associated with diseases.
- Patients may not present with specific symptoms mentioned in the app so useful more as a supplement rather than a gold-standard to help in diagnostics.
- Only available on iPhones so limits the reach of application if a medical professional uses an Android.












_f_280x120.jpg)























Your thoughts on this
Loading...