Table of Contents
Raymond decided he would spend Memorial Day painting the ceiling of his kitchen. Holding his arms over his head he had a massive, widowmaker heart attack. Over the next 13 hours 13 clots formed in every chamber of his heart. There was simply no way he should survive, but he did for another 10 years, dying of other causes at the age of 80.
Fifteen years later, Raymond's son Robert was on a 15-mile (25 km) hike when he became dehydrated and also had a widowmaker. Cardiac catheterization would reveal later that arteries on the left and right sides of Robert's heart were blocked 98% and 95% respectively, but a year and a half later, Robert was capable of running a block down the street to catch a bus.
What is it that allows some people to survive "unsurvivable" heart disease? In these fortunate few, who are numerous enough that many of us know someone with a similar story, collateral circulation, the appearance of new blood vessels built by stem cells--even without stem cell transplants and without stem cell stimulation--makes all the difference. And "off the shelf" stem cell treatments, a kind of therapy abandoned for several years but once again under intensive investigation, may make the kind of recovery Raymond and Robert enjoyed naturally available for many more people.
Stem Cells Enable the Heart to Repair Itself
There is strong evidence that severely damaged blood vessels can regenerate themselves with the help of adult stem cells. Stem cells are cells that can transform (the technical term is "differentiate") themselves into whatever kinds of cells are needed to repair a tissue.
Smaller numbers of stem cells, however, continue to exist inside the body even into old age. These cells can differentiate into different forms, although not with the full potential of young stem cells. Stem cells in bone marrow, for instance, can make new bone, new blood vessels, or new fat cells. And stem cells are found in compartments in tissues all over the body.
See Also: Could A New Stem Cell Therapy Regenerate Damaged Hearts?
How Do We Know Stem Cells Can Repair the Heart?
In the late 2000's, researchers at ten hospitals across the USA conducted a clinical trial in which a specialized kind of stem cells known as mesenchymal stem cells (cells that can produce various kinds of connective tissue) were harvested from the bone marrow of healthy volunteers who had the type O-negative blood type, that is, from volunteers whose blood can be transfused to any other blood type. These stem cells were purified to make a preparation called Prochymal, cultured in the lab to increase their numbers, and then injected into some of the volunteers who had had heart attacks in the 10 days before the procedure. The stem cells were injected into an artery in the leg or arm. It was not necessary to deliver them directly to the heart. Some of the volunteers received stem cells, while others received a placebo. Both groups received the same care for the next six months.
The patients who had received stem cells were four times as likely to have greater heart function (ejection fraction) six months after transfusion, and only one-fourth as likely to suffer dangerous arrhythmias.
- Hare JM1, Traverse JH, Henry TD, Dib N, Strumpf RK, Schulman SP, Gerstenblith G, DeMaria AN, Denktas AE, Gammon RS, Hermiller JB Jr, Reisman MA, Schaer GL, Sherman W. A randomized, double-blind, placebo-controlled, dose-escalation study of intravenous adult human mesenchymal stem cells (prochymal) after acute myocardial infarction. J Am Coll Cardiol. 2009 Dec 8.54(24):2277-86. doi: 10.1016/j.jacc.2009.06.055.
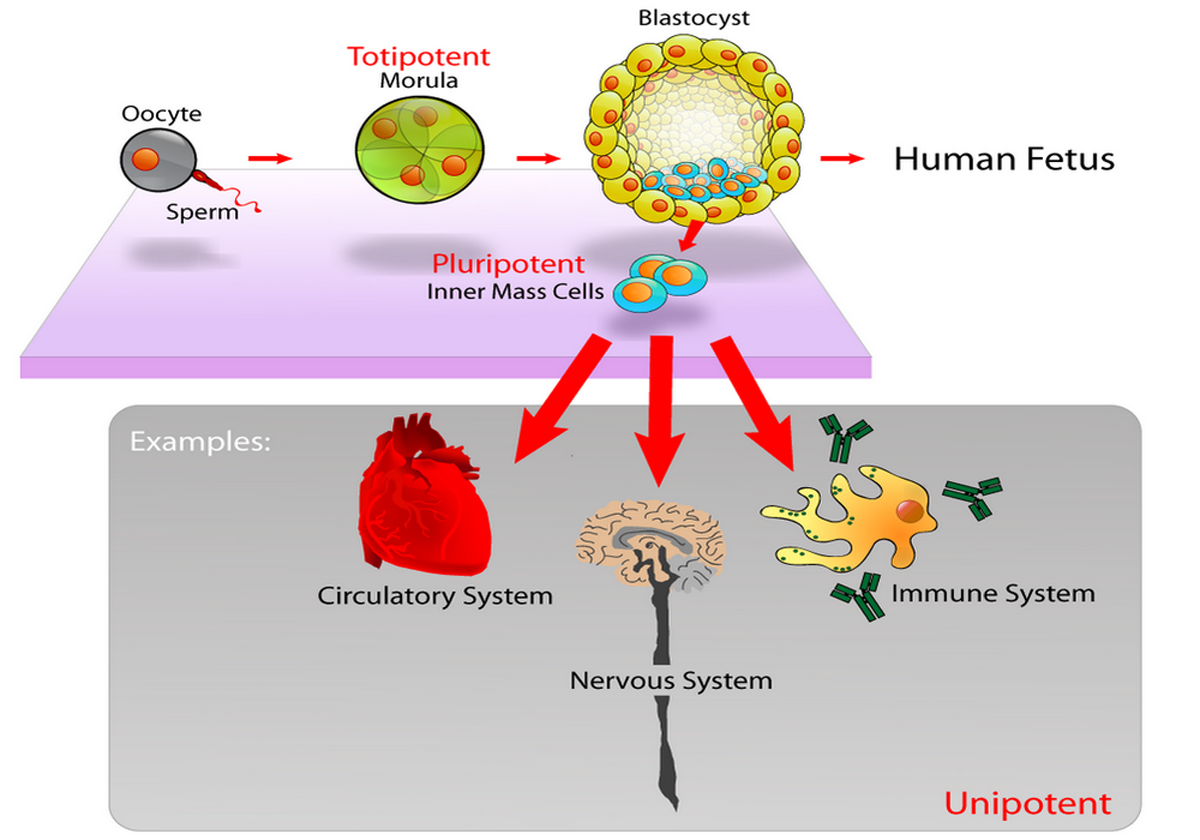
- Photo courtesy of Mike Jones by Wikimedia Commons : en.wikipedia.org/wiki/Stem_cell#mediaviewer/File:Stem_cells_diagram.png
- Photo courtesy of Lwp Kommunikáció by Flickr : www.flickr.com/photos/lwpkommunikacio/12971583774


Your thoughts on this