There are six diseases included in the group of myeloproliferative disorders and they are:
- chronic myelogenous leukemia (CML),
- polycythemia rubra vera (PRV),
- chronic idiopathic myelofibrosis,
- essential thrombocythemia (ET),
- chronic neutrophilic leukemia, and
- chronic eosinophilic leukemia.
This group of diseases is characterized by overproduction of certain types of blood cells that are made in the bone marrow.
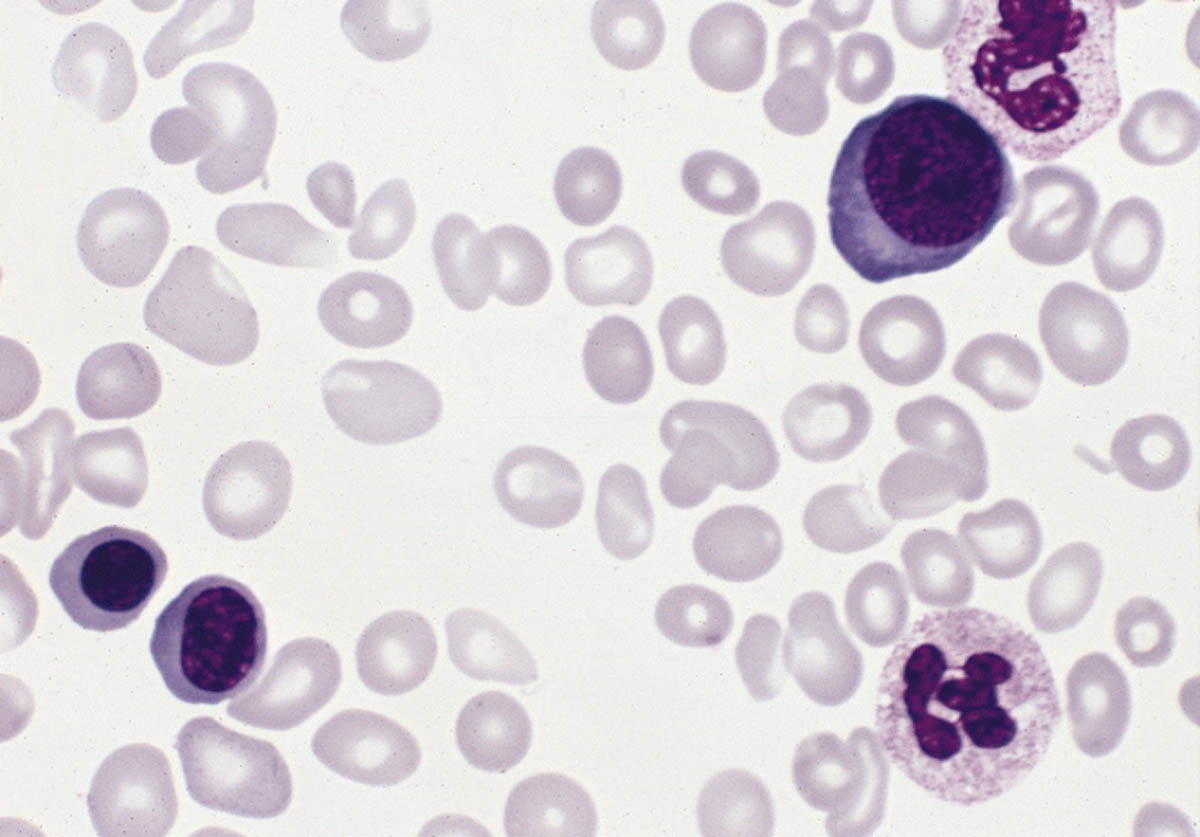
Polycythemia vera (PV) is a disease in which body makes too many red blood cells, making blood too thick. This is resulting from the excess production by the bone marrow. The overproduction of the red blood cells is the most dramatic, but the production of the white blood cells and platelets is also elevated in most cases. Polycythemia Vera primarily affects middle-aged or elderly people. It occurs more frequently in men than women, and rarely in patients under 40 years of age. It is not yet known what causes it.
Synonyms:
- Erythremia
- Osler-Vaquez Disease
- Primary Polycythemia
- Splenomegalic Polycythemia
- Vaquez-Osler Disease
- Polycythemia Rubra Vera
Bone marrow functions
Bone marrow is the body's blood-forming organ and it contains blood-forming cells called hematopoeitic precursor or stem cells. These cells have two important functions:
- self-renewal to maintain a pool of stem cells for future proliferation or growth.
- ability to mature into adult blood cells that will leave the marrow and enter the circulation.
Normal bone marrow is composed of a family of hematopoeitic clones all reproducing themselves and forming daughter cells that will, in turn, develop into red blood cells, white blood cells and platelets. The normal marrow also balances production of different cell types so they appear in the blood in their proper proportions. When something disturbs this balance, it can lead to all kinds of cells disproportions in blood. Polycythemia vera is one of those disproportions.
Possible causes of Polycythemia vera
Although the exact cause of Polycythemia vera is still unknown, there is some evidence indicating that the etiology could be in unregulated neoplastic proliferation.
The origin of the stem cell transformation remains unknown. Abnormal clone stem cells are present and they interfere with or suppress the normal stem cell growth and maturation. Progenitors of the blood cells in these patients display abnormal responses to growth factors, suggesting the presence of a defect in a signaling pathway common to different growth factors.
Although the causative genetic events are yet to be found, there are two key aspects of the biology that can identify it:
- Clonality - In Polycythemia vera, a single clone population of erythrocytes, granulocytes, B cells, and platelets arises when a hematopoeitic stem cell gains a proliferative advantage over other stem cells.
- Erythropoietin independence - Erythropoietin independence is the ability of erythroid colonies formed from the Polycythemia vera hematopoeitic stem cell to grow without erythropoietin
Symptoms of Polycythemia vera
In most cases, the affected individuals may experience:
- headaches,
- weakness,
- dizziness (vertigo),
- a ringing noise in the ear (tinnitus).
- fullness in the left upper abdomen
- red coloration, especially of the face
- shortness of breath
- breathing difficulty when lying down
- symptoms of phlebitis
In some cases, individuals with Polycythemia vera experience itching (pruritus), especially after a hot bath. They often have an abnormally enlarged spleen (splenomegaly) and/or liver (hepatomegaly). In some cases, they may also have some of the associated conditions which include:
- high blood pressure (hypertension),
- the formation of blood clots (thrombosis),
- rupturing of and loss of blood (hemorrhaging) from certain blood vessels, and
- Budd-Chiari syndrome, a rare disorder characterized by obstruction (occlusion) of veins of the liver
- vision abnormalities
- red skin spots,
- bluish skin discoloration
- fatigue
Types of Polycythemia vera
Primary polycythemia (also known as polycythemia vera)
This type of polycythemia occurs when erythrocytes are produced as a result of a proliferative abnormality of the bone marrow. This doesn’t have to mean that the problem is in the bone marrow because it can also be brought on by tumors in the kidneys since they help to regulate erythrocytes production.
Findings: There may be 8 to 9 million and occasionally 11 million erythrocytes per cubic millimeter of blood while the normal range for adults is 4-5 million. Hematocrit, the complete volume of the blood cells, may be as high as 70 to 80%. In addition, the total blood volume sometimes increases to as much as twice the normal. The entire vascular system can become filled with blood. The increased numbers of erythrocytes can increase the viscosity of the blood to as much as five times normal. Capillaries can become plugged by the very viscous blood, and the flow of blood through the vessels tends to be extremely sluggish.
Secondary polycythemia
Secondary polycythemia is caused by an increase in the production of erythropoietin that results in an increased production of erythrocytes.
Findings: There may be 6 to 8 million and occasionally 9 million erythrocytes per cubic millimeter of blood.
Physiologicpolycythemia: A type of secondary polycythemia in which the production of erythropoietin increases appropriately. It occurs in individuals living at high altitudes (4275 to 5200 meters), where oxygen availability is at much smaller concentration than at the sea level. Such people may have 6 to 8 million erythrocytes per cubic millimeter of blood.
Other causes of secondary polycythemia include
- smoking, renal or liver tumors,
- heart or lung diseases that result in hypoxia.
- endocrine abnormalities, prominently including pheochromocytoma and adrenal adenoma with Cushing's syndrome are also secondary causes.
- athletes and bodybuilders who abuse anabolic steroids or erythropoietin may develop secondary polycythemia.
Relative polycythemia
Relative polycythemia is an apparent rise of the erythrocyte level in the blood but the problem isn't in the bone marrow or erythropoietin but the reduced blood plasma. It can be caused by burns, dehydration and stress.
Diagnosis of polycythemia
While the diagnosis can be made simply based on the blood counts, most hematologists follow the guidelines of the Polycythemia Vera Study Group and run certain diagnostic tests. If the Study Group findings are present, then a diagnosis can be made with certainty
Category A
- Total red blood cell mass - In males, greater than or equal to 36 mL/kg; in females, greater than or equal to 32 mL/kg
- Arterial oxygen saturation greater than or equal to 92%
- Splenomegaly
Category B
- Thrombocytosis with platelet count greater than 400,000/mL
- Leukocytosis with a white blood cell count greater than 12,000/mL
- Increased leukocyte alkaline phosphatase greater than 100 U/L
- Serum vitamin B-12 concentration greater than 900 pg/mL or binding capacity greater than 2200 pg/mL
The major diagnostic issue related to PV is distinguishing it from other, more common forms of erythrocytosis,.
The criteria that must be met for a diagnosis of polycythemia vera and the incidence of these abnormalities at diagnosis are a demonstration of increased red cell mass combined with an enlarged spleen (splenomegaly) which presents 75% of cases or any two other features of pluripotential precursor cell involvement, such as:
- increased platelet counts (35-50%),
- neutrophilia (50-80%),
- increased leukocyte alkaline phosphate activity (80%), or
- increased vitamin B12 binding protein (67%).
Complications
The increased blood volume and increased circulating red cell mass play a key role in the symptoms and complications experienced in cases of uncontrolled polycythemia vera. Thrombosis and hemorrhage are the major complications.
Thrombosis
Thrombosis may be arterial (coronary, cerebral, peripheral vascular) or venous (involving peripheral, hepatic or portal veins). Small vessel insufficiency produces cyanosis (slightly bluish, grayish or dark purple discoloration), pain in fingers and toes, or gangrene of the digits.
Hemorrhage
Mild hemorrhagic phenomena such as nosebleeds, bleeding gums and easy bruisability are common. There may even be some more serious problems with bleeding such as:
- black tarry stool,
- hemostatsis (stagnation of blood-lack of circulation),
- menorrhagia (excessive menstrual bleeding) or
- coughing up blood which can originate from the mouth, larynx, trachea, bronchi in 10% of patients.
Read More: Gene Therapy Beats Leukemia In Eight Days
Treatment
Since this condition cannot be cured, the treatment focuses on symptoms and reducing thrombotic complications by reducing the erythrocyte levels.
Phlebotomy
Bloodletting or phlebotomy is one form of the treatment, which often may be combined with other therapies. The purpose of phlebotomy is to reduce the red blood cell mass, that is the total number of circulating red blood cells, and to do it rather quickly, at least in the beginning when the hematocrit is high.
Chemotherapy
This form of therapy for polycythemia may be used sparingly, when the rate of bloodlettings required to maintain normal hematocrit is not acceptable.
Other therapies include
- interferon injections,
- anagrelide
- en.wikipedia.org/wiki/Polycythemia_vera
- www.acor.org
- Photo courtesy of udt007us on Flickr: www.flickr.com/photos/udt007us/2722592614/
- Photo courtesy of

