Psoriasis is a chronic skin disease affecting the life cycle of skin cells. Simply put, psoriasis represents a speeding up of the usual replacement processes of the skin.
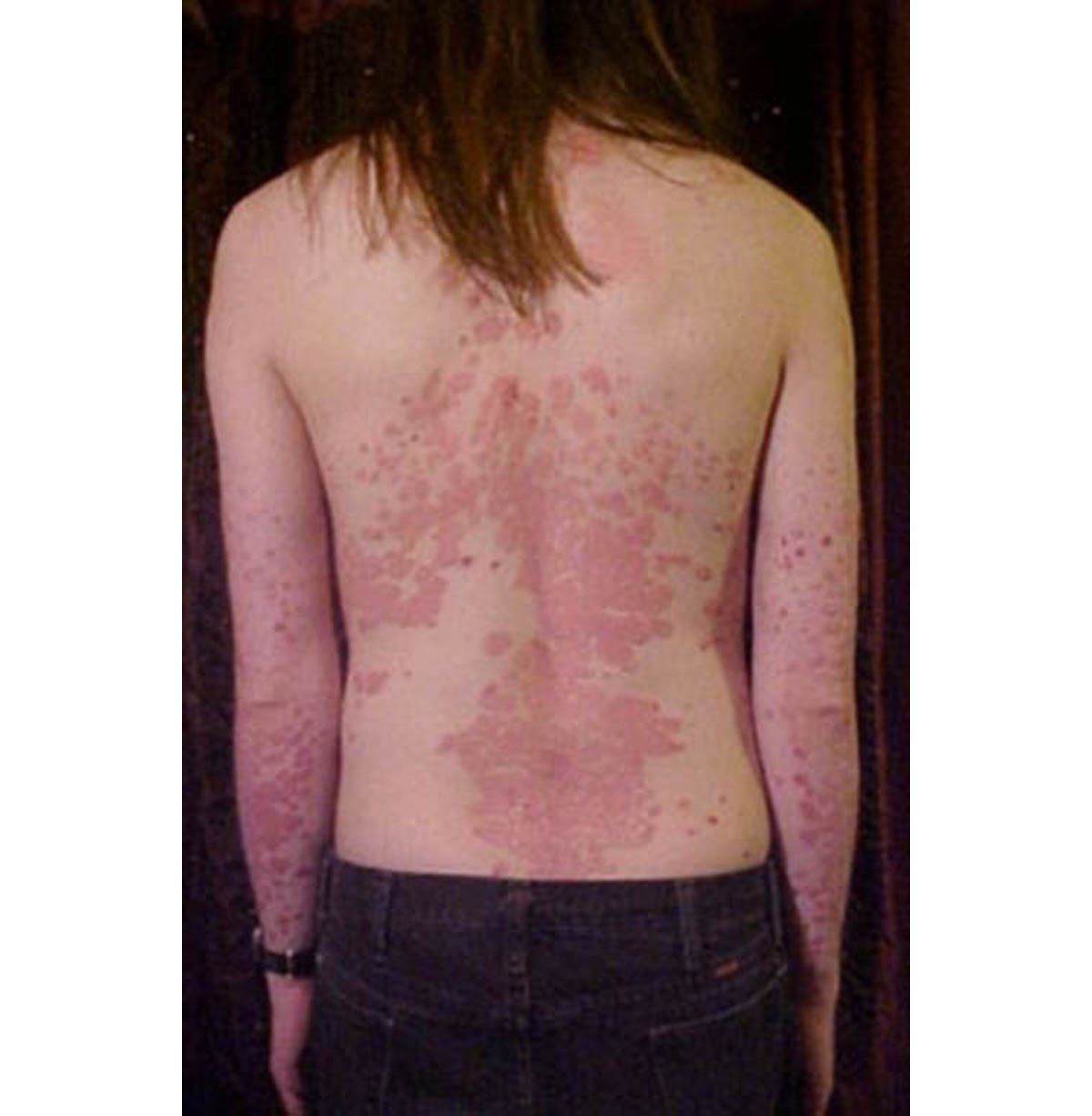
While normally new cells take between 21 and 28 days to move from the lowest skin layer where they're produced to the outermost layer where they die and flake off (the usual replacement processes of the skin), with psoriasis, this process is accelerated and lasts only a few days ( 2 – 6 days).
As a result of this speeding process, cells build up rapidly and form thick silvery scales and itchy, dry, red patches on the surface of the skin. This process is the same wherever it occurs on the body and it could appear on the elbows, knees, lower back and scalp, although any part of the body can be affected.
Psoriasis symptoms
Psoriasis symptoms can range from a few spots of dandruff-like scaling, being just a nuisance to major eruptions covering large areas that are painful, disfiguring and disabling.
Most types of psoriasis go through cycles, flaring for a few weeks or months, then improving or going into complete remission but eventually returning in most of the cases.
The most common psoriasis symptoms include:
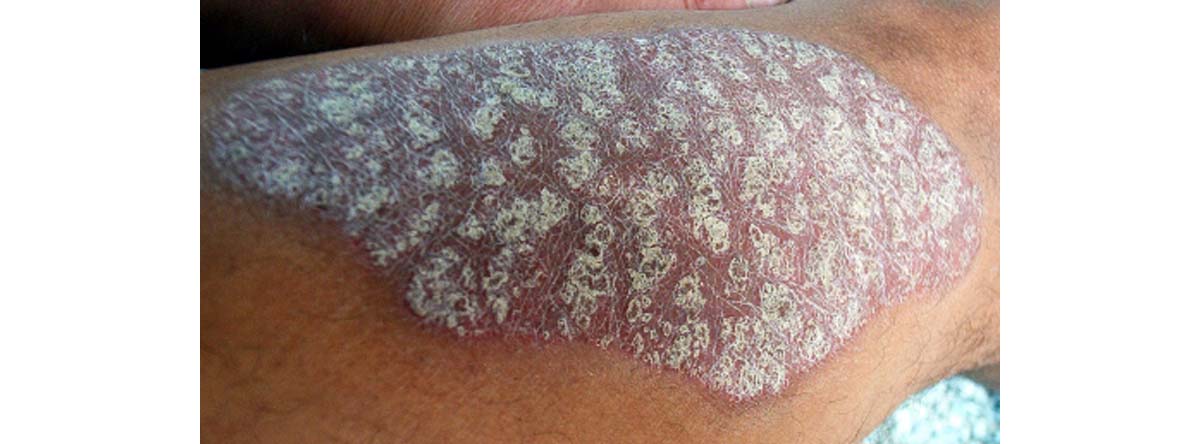
Red patches of skin covered with silvery scales (the silvery white scales are the accumulation of the skin cells waiting to be shed while the redness occurs due to the increase in blood vessels required to support the increase in cell production)
- Small scaling spots (most often seen in children)
- Dry, cracked skin that may bleed
- Itching, burning or soreness
- Thickened, pitted or ridged nails
- Swollen and stiff joints
The symptoms usually appear in areas of trauma, repeat rubbing, use, or abrasions.
Psoriasis can have other health effects. According to the National Psoriasis Foundation, around 10 to 30 percent of people with psoriasis will also develop psoriatic arthritis and the sufferers also have increased chances of developing cardiovascular disease and other systemic health problems.
Incidence
Psoriasis affects around 1%-3% of the U.S. population. In numbers, it is between 7.5 and 8.5 million people in the U.S. alone and about 125 million people worldwide. Caucasians seem to be more prone to this skin disorder than African Americans, who have about half the rate of psoriasis as Caucasians.
Is psoriasis contagious?
Psoriasis is not contagious and cannot be caught from other people by skin-to-skin contact or any other away but genetically. Psoriasis can’t be transferred from one part of the body to another.
There is a known genetic tendency, which means that it may be passed from parents to their children. Psoriasis even tends to run in some families, with around 30% of people having a family history of the condition. Certain genes have also been identified as being linked to psoriasis but it takes a trigger for psoriasis to develop and the triggers range from a throat infection, injury to the skin, certain drugs to physical or emotional stress.
Causes
Psoriasis was previously thought to be a condition of the upper most layer of the skin, however, the newer researches have found that the changes in the skin begin in the immune system when certain immune cells (T cells) are triggered to become overactive. It is not known what triggers the immune reaction but these T cells produce inflammatory chemicals leading to the rapid growth of skin cells causing psoriatic plaques to form.
What kind of doctor to see about psoriasis?
Different kinds of physicians treat psoriasis. You can choose to visit dermatologists (for the diagnosis and treatment), family physicians, internal medicine physicians, rheumatologists (for the treatment of joint disorders related to psoriasis and psoriatic arthritis), and other medical doctors or turn to alternative medicine practitioners such as acupuncturists, holistic practitioners, chiropractors, and nutritionists.
The treatment is dependant on the type of psoriasis a person has and on the severity. There is a rule to always keep your skin moisturized as it is more comfortable that way.
Treatment
There is no cure but psoriasis treatments may offer significant relief with the symptoms in most of the cases.
There are four categories of treatments:
1. Topical therapies - applied directly to the skin in forms of creams, lotions, ointments, mousse and gels. They include Vitamin D analogues, coal tar preparations, topical steroids, dithranol and vitamin A analogues. Some are available over-the-counter, while others require a prescription from a doctor. Topical therapies are effective for mild cases of psoriasis.
2. Phototherapy - the treatment with ultraviolet light (UVB, UVA, and laser). Phototherapy requires attending the phototherapy centre 2 or 3 times a week for several weeks if you are receiving UV therapy.
3. Systemic medications are reserved for people with moderate to severe psoriasis and for those who haven’t responded to other treatments. Most commonly used drugs are Methotrexate, which slows down the rate at which the skin cells are dividing in psoriasis; Ciclosporin, which suppresses the immune system; Acitretin, which slows down the rate at which skin cells are dividing in psoriasis, and calms inflammation and Hydroxycarbamide that slows down the rate at which the skin cells are dividing in psoriasis. These drugs can have severe side effects and patients need to be closely monitored while using them.
BIOLOGIC INJECTIONS (BIOLOGICS) - New Treatment Hope For Psoriasis
In the past few years, there has been a development of a new wave of drug treatments known as biologics. These medications are set to do what no previous treatment could do -- address the root of the problem by influencing the immune system.
Researchers and dermatologists claim that this new treatment has made life much more tolerable for patients.
Biologics are based on natural processes, made from human or animal proteins. They are very similar to chemicals already present in the human system. Biologics work by blocking the action of certain immune cells (T cells) or the chemicals released by them, which play a part in causing psoriasis. The use of these drugs has showed that they have significantly fewer side effects than traditional systemic therapy.
Characteristics of biologics
They are injections, received either by a doctor or by yourself at home, depending on the medication or by infusion somewhere between twice-weekly to once every other week.
- Are effective for treating psoriasis and/or psoriatic arthritis for many patients, but not for all
- Short-term side effects are mild
- Long-term side effects are not known yet, being investigated
- They are expensive (cost around $10,000 per year)
- Periodic evaluations are necessary for patients undergoing biologic treatment to check for possible infections or potential cancers
Who can use biologics?
Biologics are a good option for those who have not responded to other conventional treatments, who have experienced harmful side effects from other treatments or who can't take other medications due to their health problems.
What are the side effects?
Common side effects for all biologics include respiratory infections, flu-like symptoms and injection site reactions (swelling, itching or rash). These side effects are generally mild and tolerable, so patients can continue taking them.
People with active infections may not be eligible for some biologics. If a major infection develops during the treatment, the patient should temporarily stop taking biologics. In some cases, screening for tuberculosis (TB) or other infections is required before undergoing treatment with certain biologics.
How can you get a biologic medication?
Biologics are available only by prescription. Some can be given only in a doctor's office while others can be self-administered.
How expensive are biologics?
Because biologics are very complex and expensive to make (it takes decades of research and development before they are approved for patient use), they also have a high cost. It takes $10,000 or more per year depending on the dose and the frequency of treatment.
Biologics are, however, more affordable than ultraviolet therapy, another leading treatment for medium-to-severe cases of psoriasis.
Certain insurance companies will fully cover for a biologic, others partially while some patients will have to pay the total cost out of their pockets.
Biologics manufacturers have special programs to help patients with insurance issues or may even offer discounted prices for people who meet certain income and financial requirements. This is why it is essential patients obtained all the necessary information from their doctors’ offices to check where they stand.;
Currently, five biologics are approved by the U.S. Food and Drug Administration for treatment of psoriasis, and three of those five are approved for psoriatic arthritis.
They are Amevive, Enbrel, Humira, Remicade, and Raptiva for psoriasis with Enbrel, Remicade, and Humira being approved for the treatment of psoriatic arthritis too.
Amevive -- prescribed for adults with moderate to severe plaque psoriasis who are also candidates for phototherapy or other systemic treatments. Patients with a history of malignancy or recurrent infections should not undergo this treatment.
Enbrel -- prescribed for adults with moderate to severe plaque psoriasis who are also candidates for phototherapy or other systemic treatments; for patients with active psoriatic arthritis as it helps stop or slow the damage to joints caused by this disease; for use in children as young as 4 for juvenile rheumatoid arthritis, but not for treating psoriasis or psoriatic arthritis in children. People with active serious infections or a history of recurrent infections, heart failure, multiple sclerosis or other types of demyelinating neurologic diseases should not undergo this treatment.
Raptiva -- prescribed for adults with moderate to severe plaque psoriasis who are also candidates for phototherapy or other systemic treatments. It is not necessary for patients to try or fail other medications before being put on Raptiva. People taking vaccines or those with active serious infections should not start Raptiva.;
Remicade -- prescribed for people with severe psoriasis and active psoriatic arthritis. People with active serious infections or a history of recurrent infections, heart failure, multiple sclerosis or other types of demyelinating neurologic diseases should not undergo this treatment.
Humira -- prescribed for people with moderate to severe psoriasis and active psoriatic arthritis. People with active serious infections or a history of recurrent infections, heart failure, multiple sclerosis or other types of demyelinating neurologic diseases should not undergo this treatment.
Caution is advised against all the drugs for the elderly due to their already present risk of infections.
The impact of these drugs on pregnant and breastfeeding women or developing fetuses is not known. Therefore, the drugs should only be given to pregnant or nursing women if there is a clear medical need, and if this decision is reached by a patient and doctor together.
Read More: The Ten Most Common Psoriasis Triggers
Coping With Psoriasis Treatment
What psoriasis sufferers need to understand is that treating this disease requires patience and commitment. It is essential to strike a balance between the amount your psoriasis symptoms bother you and the difficulties imposed by treating them. If one treatment doesn’t work for you, others may work quite well and have fewer side effects.
Don’t agree to any treatment your doctor suggests unless you can really stick to it.
For example, don't agree to three times a week phototherapy sessions if you know that you can’t make all of them or to using coal tar in your hair every night if you can't stand that mess.
The most frustrating fact about psoriasis treatment is that once effective treatment may not stay effective forever. This is very discouraging and many sufferers just give up after having another flare.
It is important to keep trying as there are other treatments and combinations of treatments that can be used. It is crucial you learned about all of them and discussed your options with your doctor.

