Table of Contents
Psoriasis is a skin condition that is characterized by the development of raised plaques on the surface of the skin. The plaques can occur anywhere in the body and are often reddish in appearance. The exact cause as to why this condition occurs in some people is unknown, although a genetic component has been identified over the last few years. This genetic component is only one part of the puzzle though, since it may be present in a number of people who never manifest any clinical symptoms of the disease. It is likely a combination of external factors or triggers is needed to activate this gene in the body.
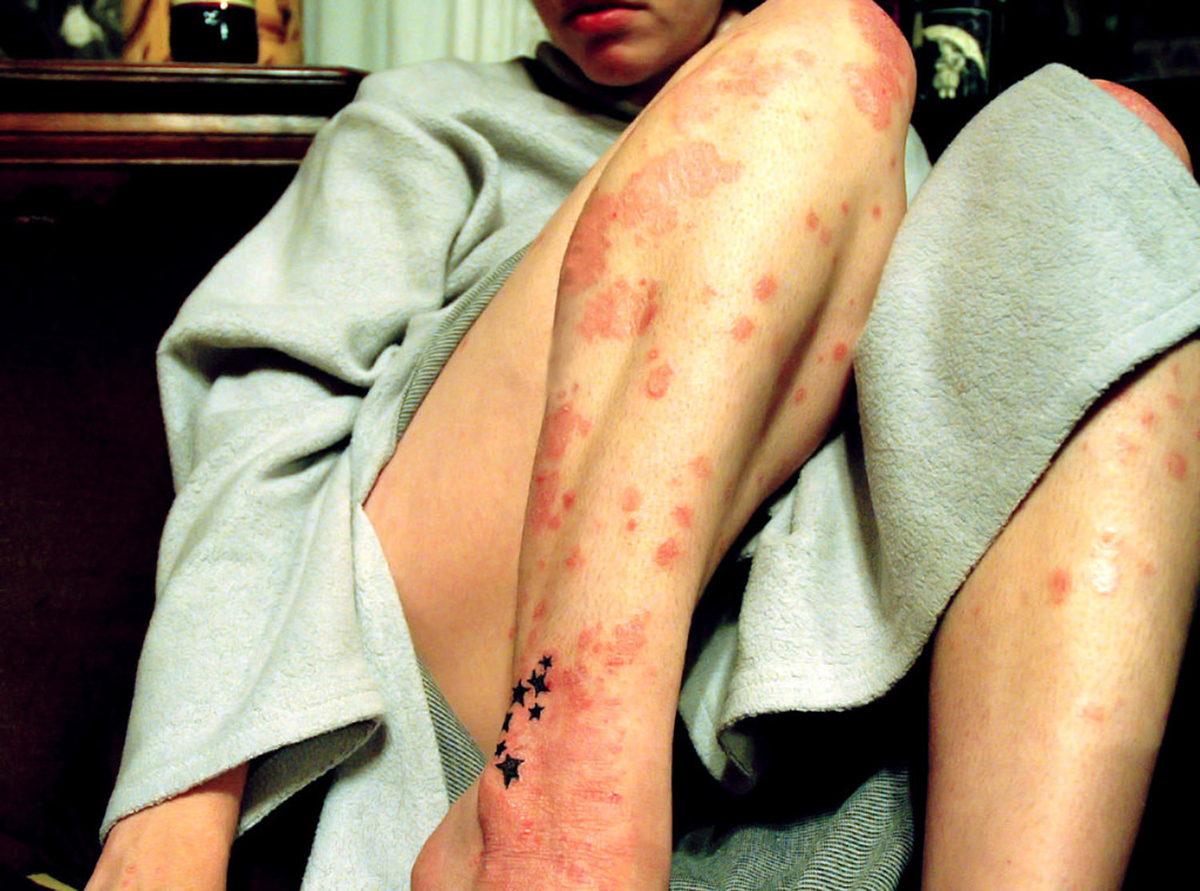
What Goes Wrong In Psoriasis?
Our skin is made up of a number of layers and during the normal life cycle of a cell, it moves up through these layers, eventually being shed off and replaced by other skin cells. The time taken for this entire process is greatly reduced in patients suffering from psoriasis.
Thus, dead and non-vital cells accumulate at the top layer faster than they can be shed off leading to the formation of a raised plaque. The underlying skin starts to become reddish as the body increased blood flow to the area in an effort to keep the cells nourished for as long as possible.
How Is Psoriasis Related To Dental Problems?
The gums are technically part of the skin that covers our body and the same cellular malfunction that occurs elsewhere can occur here as well. In rare cases, psoriasis will begin with the appearance of plaques on the lips, gums, tongue and the inside of the cheeks. There are also documented cases of psoriasis in which there were never any other clinical symptoms elsewhere on the body.
Psoriasis also puts the patient at an increased amount of risk for the development of other dental problems. The incidence of geographic tongue and fissured tongue is much higher in people suffering from psoriasis, although the exact link has been hard to define.
Psoriasis And Gum Disease
Investigation into a link between psoriasis and gum disease is not a recent occurrence. Researchers have been finding evidence of increased incidence of gum disease in psoriasis patients and vice-versa as well, however they were never able to prove a cause-and-effect relationship between the two.
The current state of understanding is also pretty similar. Both the diseases seem to be occurring as an exaggerated response of the immune system in which an inordinate amount of damage occurs to the normal bystander cells.
READ Biologics - New Treatment Hope For Psoriasis Sufferers
One line of thinking suggests that an improvement in psoriasis can be seen by getting treatment for infected gums. This is because the pro-inflammatory mediators released from the gums lead to stress on a jumpy immune system. As a result, when dead skin cells start to accumulate near the top layers of the skin, the body goes into overdrive to try and reverse the situation.
Anecdotal evidence exists about people who found that their psoriasis improved dramatically after getting their infected teeth extracted or after getting gum treatment.
- www.colgate.com/en/us/oc/oral-health/conditions/immune-disorders/article/how-to-treat-your-psoriasis-mouth-symptoms-0715
- www.dentalhealth.org/news/details/644
- Photo courtesy of mysiann: www.flickr.com/photos/mysiann/489536302/
- Photo courtesy of thecampbells: www.flickr.com/photos/thecampbells/3350877893/
- Photo courtesy of mysiann: www.flickr.com/photos/mysiann/489536302/

