Guillain-Barre syndrome can affect anybody; it can strike at any age and both sexes are equally prone to the disorder. The syndrome is rare, afflicting only about one person in 100,000.
Usually Guillain-Barre occurs a few days or weeks after the patient has had symptoms of a viral infection. It is not so hard to recognize the symptoms of a respiratory or gastrointestinal viral infection. Occasionally surgery or vaccinations will trigger Guillain-Barre syndrome as well. This disorder can develop over the course of hours or days, or it may take up to 3 to 4 weeks for symptoms to become apparent. Most people reach the stage of greatest weakness within the first 2 weeks after symptoms appear. By the third week of the illness 90 percent of all patients are at their weakest.
 What is Guillain-Barre syndrome?
What is Guillain-Barre syndrome?
Guillain-Barre syndrome is a disorder in which the body’s immune system attacks part of the peripheral nervous system, usually within days or weeks of contracting a bacterial or viral infection.
The first symptoms of this disorder include varying degrees of weakness or tingling sensations. These symptoms most commonly occur in the legs. In many instances the weakness and abnormal sensations spread to the arms and upper body while the disease progresses. These symptoms can increase in intensity until certain muscles cannot be used at all.
When Guillain-Barre syndrome is severe the patient could be almost totally paralyzed. In these cases the disorder is life threatening. Guillain-Barre syndrome has the potential to interfere with breathing and, at times, with blood pressure or heart rate. That is why Guillain-Barre syndrome is considered to be a medical emergency. Such a patient is often put on a respirator to assist with breathing.
Patients should also be watched closely for problems such as an abnormal heart beat, infections, blood clots, and high or low blood pressure. Most patients can recover from even the most severe cases of Guillain-Barre syndrome. However, some patients continue to have a certain degree of weakness long after the disease has run its course.
Causes of Guillain-Barre syndrome
No one yet knows why Guillain-Barre syndrome strikes some people and not others. Moreover, nobody knows exactly what sets the disease in motion. What scientists do know is that the body’s immune system begins to attack the body itself. It causes what is known as an autoimmune disease. Usually the cells of the immune system attack only foreign material and invading organisms but with the Guillain-Barre syndrome the immune system starts to destroy the myelin sheath that surrounds the axons of many peripheral nerves.
This disease could even destroy the axons themselves. Axons are long, thin extensions of the nerve cells, which carry nerve signals. The myelin sheath surrounding the axon speeds up the transmission of nerve signals and allows the transmission of signals over long distances of the body. In diseases in which the peripheral nerves’ myelin sheaths are injured or degraded, the nerves cannot transmit signals as efficiently as they should.
That is why the muscles begin to lose their ability to respond to the brain’s commands. These commands should be carried through the nerve network. The brain also receives fewer sensory signals from the rest of the body. This then results in an inability to feel textures, heat, pain, and other sensations.
Alternately, the brain may receive inappropriate signals that result in tingling, crawling skin feelings, or even painful sensations. Because the signals to and from the arms and legs must travel the longest distances they are most vulnerable to interruption due to Guillain-Barre syndrome. Therefore, muscle weakness and tingling sensations usually first appear in the hands and feet, after those areas they could progress upwards.
When Guillain-Barre is preceded by a viral or bacterial infection, it is possible that the virus has changed the nature of the cells in the nervous system. That is why the immune system treats them as foreign cells. It is also possible that the virus makes the immune system itself less discriminating about what cells it recognizes as its own. Guillain-Barre syndrome allows some of the immune cells, such as certain kinds of lymphocytes and macrophages, to attack the myelin. Sensitized T lymphocytes cooperate with B lymphocytes to produce antibodies against components of the myelin sheath. That may contribute to destruction of the myelin.
Scientists are still investigating these and other possibilities to find why the immune system goes awry in Guillain-Barre syndrome as well with other autoimmune diseases. The cause and course of Guillain-Barre syndrome is an active area of neurological investigation, and has been for a long time. This topic incorporates the cooperative efforts of neurological scientists, immunologists, and virologists.
Diagnosis of Guillain-Barre syndrome
Guillain-Barre is called a syndrome rather than a disease because it is not clear whether or not a specific disease-causing agent is involved. A syndrome is a medical condition characterized by a collection of symptoms that the patient feels. It is also characterized by signs which a doctor can observe or measure. The signs and symptoms of the syndrome can be quite varied, so doctors may on rare occasions find it difficult to diagnose Guillain-Barre. This is especially difficult in its earliest stages.
The problem is that several disorders have symptoms similar to those found in Guillain-Barre. Therefore, doctors can only examine and question patients carefully before making a diagnosis. Collectively, the signs and symptoms form a certain pattern that helps doctors differentiate this syndrome from other disorders. For example, physicians will note whether the symptoms appear on both sides of the body that is most common in Guillain-Barre syndrome, and the quickness with which the symptoms appear.
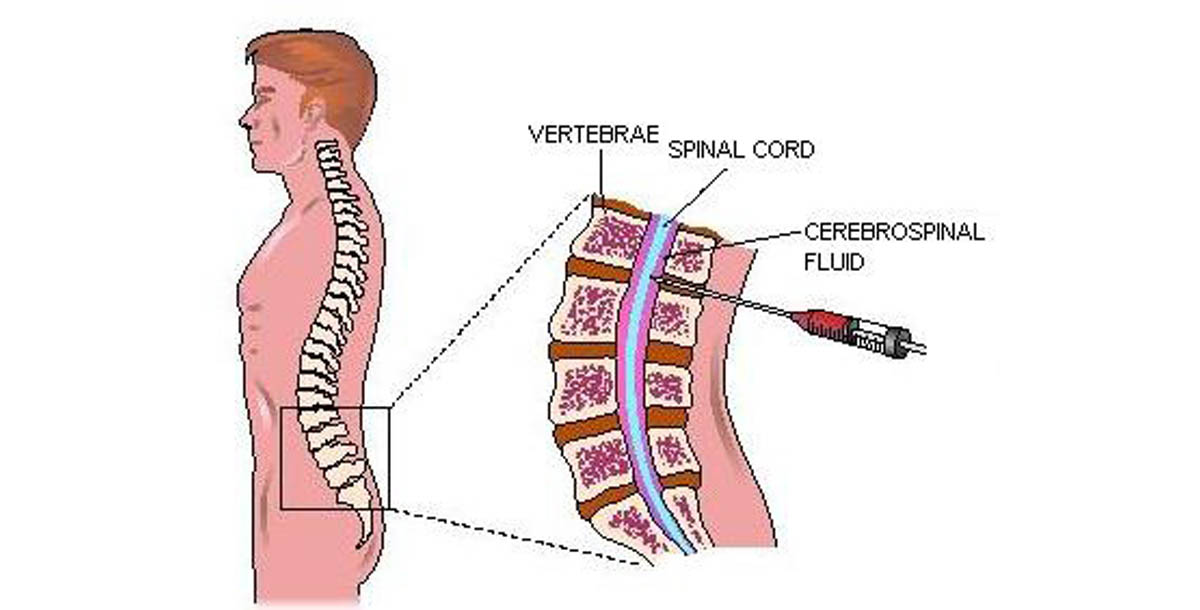
It is important to know that in other disorders, muscle weakness may progress over months rather than days or weeks. In Guillain-Barre syndrome, reflexes such as knee jerks are usually lost. Because the signals traveling along the nerve are slower, a nerve conduction velocity test can give doctor clues to aid the diagnosis. In Guillain-Barre patients, the cerebrospinal fluid that bathes the spinal cord and brain contains more protein than usual so a physician may decide to perform a spinal tap - a procedure in which the doctor inserts a needle into the patient’s lower back to draw cerebrospinal fluid from the spinal column.
Read More: AIHA - Autoimmune Haemolytic Anaemia
Treatment of Guillain-Barre syndrome
There is no known cure for the Guillain-Barre syndrome but there are supportive treatments that lessen the severity of the illness and accelerate the path to recovery in most patients. There are also a number of ways to treat the complications of Guillain-Barre. Currently, plasmapheresis and high-dose immunoglobulin therapy are used as the best treatment option. Both of them are equally effective, but immunoglobulin is easier to administer for most doctors.
Plasmapheresis is a method by which whole blood is removed from the body and processed. This way red and white blood cells are separated from the plasma, or liquid portion of the blood. The blood cells are then returned to the patient without the plasma, which the body quickly replaces. Scientists still do not know exactly why plasmapheresis works. However, this technique seems to reduce the severity and duration of the Guillain-Barre episode. This may be because the plasma portion of the blood contains elements of the immune system that may be toxic to myelin.
In high-dose immunoglobulin therapy, doctors give intravenous injections of the proteins. The immune system naturally produces these proteins in small quantities to attack invading organisms. Investigators have found that giving high doses of these immunoglobulin to Guillain-Barre patients can lessen the immune attack on the nervous system. Investigators do not know why or how this works, although there are several hypotheses proposed.
The use of steroid hormones has also been tried as a way to reduce the severity of Guillain-Barre syndrome. However, controlled clinical trials have demonstrated that this treatment is not only ineffective, but may even have a deleterious effect on Guillain-Barre syndrome.
The most critical part of the treatment of this syndrome consists of keeping the patient’s body functioning during recovery of the nervous system.
This can sometimes require placing the patient on a respirator, a heart monitor, or other machines to assist body function during recovery. The need for this sophisticated machinery is one of the reasons why Guillain-Barre syndrome patients are usually treated in hospitals. In the hospital, doctors can also look for and treat the many problems that can afflict any paralyzed patient. These are complications such as pneumonia or bed sores that can strike over the course of the illness.
Often, even before recovery begins, caregivers may be instructed to manually move the patient’s limbs. This is recommended to help keep the muscles flexible and strong, because muscles begin to atrophy without movement. Later, as the patient begins to recover limb control, physical therapy for Guillain-Barre syndrome begins.
Carefully planned clinical trials of new and experimental therapies are the key to improving the treatment of these patients. Such clinical trials begin with the research of basic and clinical scientists who identify new approaches to treating patients with the disease. The problem is, the Guillain-Barre syndrome can be a devastating disorder because of its sudden and unexpected onset. In addition, recovery is not necessarily quick, so patients usually reach the point of greatest weakness or paralysis days or weeks after the first symptoms occur. Symptoms then stabilize at this level for a period of days, weeks, or months. The recovery period may be as short as a few weeks or as long as a few years, where about 30 percent of those with Guillain-Barre still have a residual weakness after 3 years.

