Table of Contents
This can be caused directly by some drug, toxin, blood parasite virus or some other known cause, or it can be an unexplained immune mediated reaction.
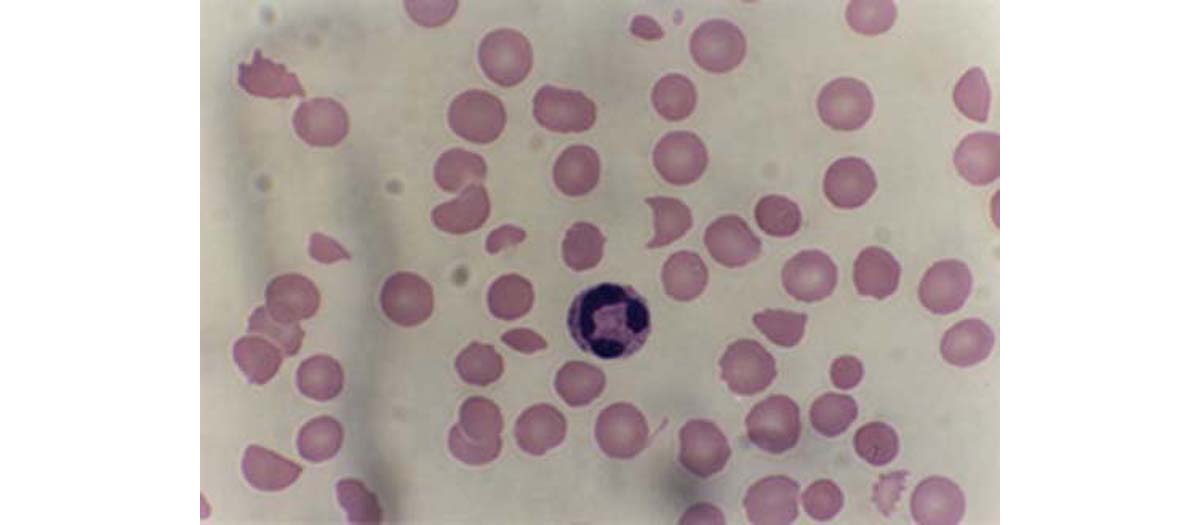
Incidence
Hemolytic anemia represents approximately 5% of all anemias. The overall incidence of death is caused by this disorder is low. However, older patients and patients with cardiovascular impairment are at an increased risk. Most of the disorders that lead to hemolysis are not specific to any race or gender.
Signs and symptoms of autoimmune hemolytic anemia
Since there is often some kind of underlying disorder behind this type of anemia, symptoms are usually caused by both anaemia and the underlying disorder. It is also important to know that patients with minimal haemolytic anaemia can be asymptomatic.
Severe anaemia, especially of sudden onset, may cause:
- tachycardia,
- dyspnoea,
- angina
- weakness
- tiredness
- faintness
- dizziness
- general pallor and pale conjunctivae
- tachycardia
- tachypnoea – fast breathing
- hypotension
- mild jaundice may occur due to haemolysis.
- dark urine
When destruction persists for a few months or longer, the spleen may enlarge, resulting in a sense of abdominal fullness and discomfort.
- www.nlm.nih.gov
- www.hcd2.bupa.co.uk
- en.wikipedia.org/wiki/Autoimmune_haemolytic_anaemia

