Guillain-Barre Syndrome is a condition where the body mistakenly produces antibodies that destroy nerves that supply muscles of the body. The exact mechanism is not known, but it has been noted to be associated with recent infections, such as respiratory or gastrointestinal (stomach).
It occurs worldwide and is relatively rare, and the incidence increases with age, with a predilection for males.

Clinical Presentation
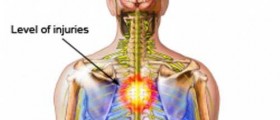
Guillain-Barre Syndrome mostly presents with a weakness that starts at the toes and progressively rises in both legs equally (ascending). It may progress to involve the arms and breathing muscles. It tends to affect mostly the nerves that supply the muscles, with sparing sensation, but 80 percent of patients will have some tingling in their legs and arms. There is the loss of deep tendon reflexes (ankle and knee reflexes).
The weakness can vary from mild difficulty in walking to difficulty in breathing and swallowing. The weakness occurs progressively over about two weeks and usually by the fourth week the weakness reaches its peak, and may remain here for some weeks and gradually recover in the same fashion that occurs. If the weakness is still progressing by the eighth week, this is now termed chronic inflammatory demyelinating polyradiculoneuropathy (CIDP).
Variants
- Acute inflammatory demyelinating polyneuropathy (AIDP) -This is the most common variant, and its presentation is as described above.
- Acute motor axonal neuropathy (AMAN) - Most of these cases have been associated with diarrhea caused by Campylobacter jejuni infection. In this variant, there is only weakness, and there are no sensory symptoms.
- Acute motor and sensory axonal neuropathy -This is a is similar to AMAN, and with profound weakness and loss of sensation
- Miller Fisher Variant - In this variant, the weakness starts with weakness in the facial muscles than in the arms and legs. (Almost reverse to AIDP), but weakness in the arms and legs is not as profound.
Diagnostic Evaluation
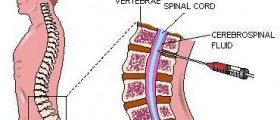
The diagnosis is usually made from history and clinical examination. The doctor may also do a spinal tap (lumbar puncture) to get the fluid that surrounds the spine, to check for abnormalities and antibodies.
Treatment
Most of the care is supportive. Thirty percent of patients will require to be connected to a ventilator if their breathing muscles are weak. Most patients will be admitted to a higher care ward such as an ICU, to monitor, their vitals closely.
Treatment such as plasma exchange (plasmapheresis) can be done in severe cases. Plasmapheresis is thought to remove the antibodies that damage the nerves from the patient's blood. Another form of treatment is an infusion of Intravenous immune globulin (IVIG). These medications are noted to shorten the disease duration and shorten hospital stays. The mode of treatment is dependent on the severity and availability, but most of these treatments are given to patients who present within four weeks. It has been noted that the benefit from either treatment is equal.
Prognosis
Poor prognostic factors include older age, need for ventilator support, preceding diarrheal illness and the rapidity of weakness. By six months, 85 percent of patients will be able to walk, and 60 percent will be back at normal strength by one year.
- Medscape
- Uptodate
- Photo courtesy of SteadyHealth










_f_280x120.jpg)
