Problems may also occur in every other organ system. Patients reported problems in the digestive tract, heart, and genitals. People with diabetes can develop nerve problems at any time, but the longer a person has diabetes, the greater the risk of developing some. Fifty percent of diabetics have some form of neuropathy; we should all strive to learn more about it.
What is diabetic neuropathy?
Diabetic neuropathy is damage to nerves throughout the body that appears in people who have diabetes. Most people report some kind of numbness, pain and weakness, but not all who suffer from neuropathy exhibit these symptoms. The highest rates of neuropathy are among people who have had the disease for at least 25 years of life. Diabetic neuropathy also appears to be more common in people who have had trouble controlling their blood glucose levels, as well as in those with high levels of blood fat and high blood pressure, in overweight people, and in people over the age of 40.
The most common type is peripheral neuropathy, also called distal symmetric neuropathy, which affects the arms and legs, but actually there are three types of diabetic neuropathy: peripheral, autonomic, and focal.
Peripheral neuropathy reduces a person’s ability to sense pain, touch, temperature, and vibration in certain parts of the body. Because of this problem, a patient may sometimes experience problems with movement and muscle strength. It most often affects the feet and lower legs, and may contribute to the development of serious foot problems. Most common problems are ulcers, infection, and bone and joint deformities. It is the most common type of diabetic neuropathy.
Autonomic neuropathy is caused by damage to the nerves that control the involuntary, or autonomic, functions of the body such as heartbeat, blood pressure, sweating, digestion, urination, and some aspects of sexual function. It is also common in people with diabetes, but not as common as peripheral neuropathy is.
Focal neuropathy is far less common than peripheral neuropathy and autonomic neuropathy. Unlike these other forms, focal neuropathy usually develops suddenly. Focal diabetic neuropathy is sometimes called mono-neuropathy, since it affects a single nerve. Most often, this singe nerve affected will be in the wrist, thigh, or foot. It may also affect the nerves of the back and chest, and those that control eye muscles as well.
Causes of diabetic neuropathy
The causes of neuropathy are probably different for different varieties of the condition. Researchers are studying the effect of glucose on nerves to find out exactly how prolonged exposure to high glucose causes this problem. Nerve damage is likely due to a combination of metabolic factors, abnormal blood fat levels, neurovascular factors, autoimmune factors, mechanical injury to nerves, and/or lifestyle factors such as smoking or alcohol use.
Symptoms of diabetic neuropathy
Symptoms depend primarily on the type of neuropathy, but also on which nerves are affected. Some people have no symptoms at all, while for others numbness, tingling, or pain in the feet is often the first sign. A person can experience both pain and numbness, although symptoms are minor at first.
Since most nerve damage occurs over several years, mild cases may go unnoticed for a long time. Symptoms may involve the sensory or motor nervous system, as well as the involuntary, or autonomic, nervous system.
In some people, mainly those with focal neuropathy, the onset of pain may be sudden and severe according to type of their neuropathy. Symptoms may include numbness, tingling, or pain in the toes, feet, legs, hands, arms, and fingers. Patients could also experience wasting of the muscles of the feet or hands, indigestion, nausea, or vomiting, diarrhea or constipation, and dizziness or faintness due to a drop in postural blood pressure. Some people also report problems with urination, erectile dysfunction or vaginal dryness, and weakness.
Types of diabetic neuropathy
Neuropathy affects nerves throughout the body depending of the type. Some researchers classify diabetic neuropathies as peripheral, autonomic, proximal, and focal. Each affects different parts of the body in different ways; peripheral neuropathy causes either pain or loss of feeling in the toes, feet, legs, hands, and arms, while autonomic neuropathy causes changes in digestion, bowel and bladder function, sexual response, and perspiration, as well as nerves that serve the heart and control blood pressure. Proximal neuropathy causes pain in the thighs, hips, or buttocks and leads to weakness in the legs, while focal neuropathy results in the sudden weakness of one nerve, or a group of nerves, causing muscle weakness or pain.
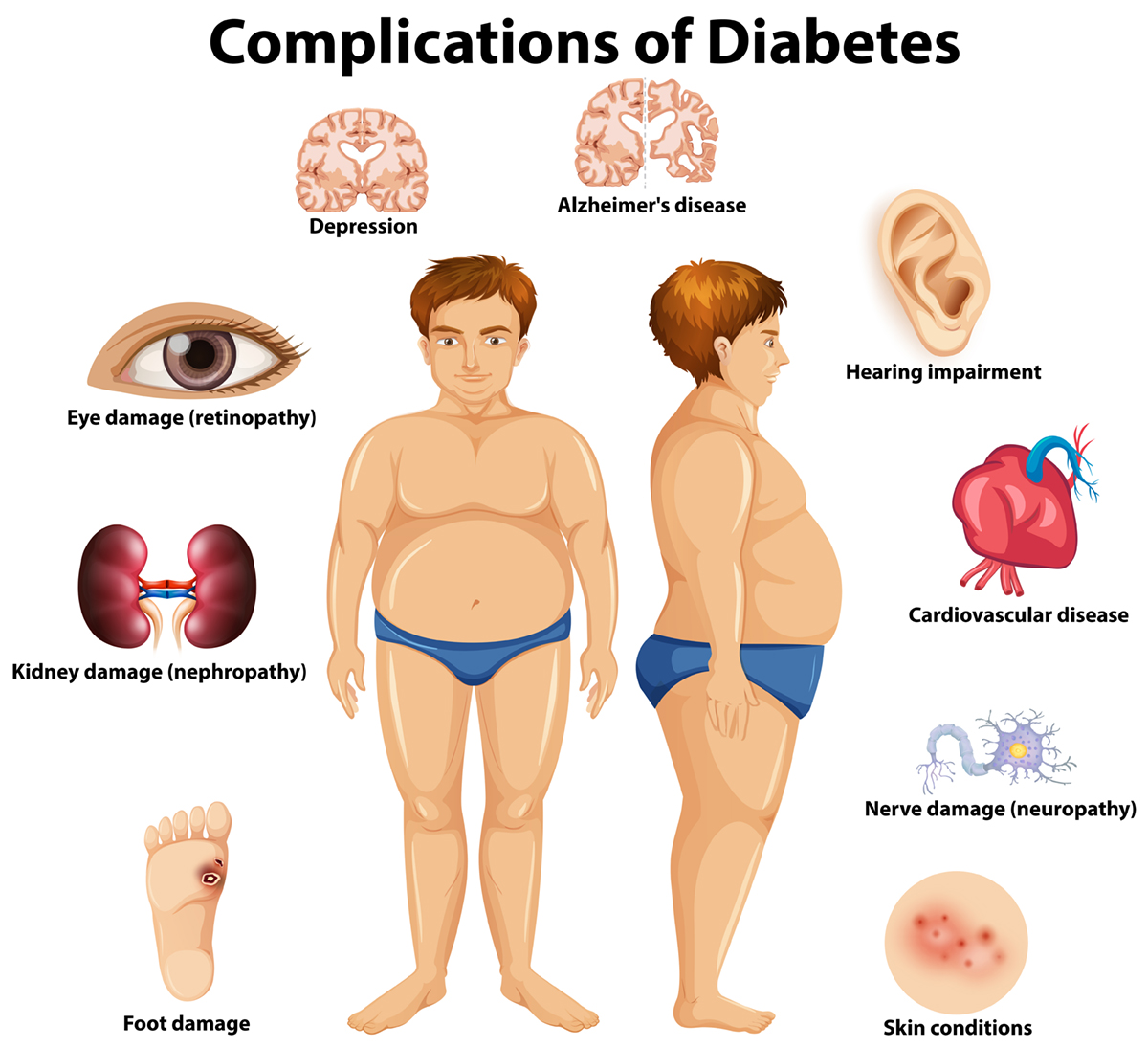
Peripheral neuropathy affects:
- toes
- feet
- legs
- hands
- arms
Autonomic neuropathy affects:
- heart and blood vessels
- digestive system
- urinary tract
- genitals
- sweat glands
- eyes
Proximal neuropathy affects:
- thighs
- hips
- buttocks
Focal neuropathy affects:
- eyes
- facial muscles
- ears
- pelvis and lower back
- thighs
- abdomen
How to prevent diabetic neuropathy?
The best way to prevent neuropathy is to keep blood glucose levels as close to nominal as possible. Maintaining safe blood glucose levels protects nerves throughout the body.
Diagnosis of diabetic neuropathy
You may be diagnosed with diabetic neuropathy based on symptoms and physical exam results. During the exam, the doctor may check blood pressure and heart rate, muscle strength, reflexes, and sensitivity to position, vibration, temperature, or simply apply a light touch and observe the way you experience it. The doctor may also perform other tests to help determine the type and extent of nerve damage and determine which type of diabetic neuropathy you might have.
A comprehensive foot exam assesses skin, circulation, and sensation; this test can be taken during a routine office visit. To assess protective sensation or feeling in the foot, the doctor will attach nylon monofilament to a wand, and then touch the foot. Those who cannot sense pressure from the monofilament have lost protective sensation. These people are at risk for developing foot sores that may not heal properly.
Other tests include checking reflexes and assessing vibration perception. These diagnostic methods are more sensitive than touch pressure.
Nerve conduction studies examine the transmission of electrical current through nerve. With this test, an image of the nerve conducting an electrical signal is projected onto a screen. Nerve impulses that seem slower or weaker than usual indicate possible damage or neuropathy. This test allows the doctor to assess the condition of all the nerves in the arms and legson a case by case basis.
Electromyography is a common diagnostic method which shows the response of muscles to nerve signals. The electrical activity of the muscle is displayed on a screen. A response slower or weaker than usual suggests damage to the nerve or muscle, which might determine if you have some type of diabetic neuropathy.
Quantitative sensory testing uses the response to stimuli, such as pressure, vibration, and temperature, to check for neuropathy. A check of heart rate variability shows how the heart responds to deep breathing and to changes in blood pressure and posture, which might also change due to diabetic neuropathy.
Ultrasound uses sound waves to produce an image of internal organs, and the ultrasound of the bladder, for example, can show how this organ preserves a normal structure and whether the bladder empties completely after urination.
Nerve or skin biopsy involves removing a sample of nerve or skin tissue for examination by microscope to diagnose neuropathy.
Read More: Diabetic Gastroparesis: Causes, Symptoms and Treatment
Treatment of diabetic neuropathy
The first step is to bring blood glucose levels within the normal range, in order to prevent further nerve damage. Patients may need glucose monitoring, meal planning, exercise, and possibly oral drugs or insulin injections to control their blood glucose levels. Although symptoms may get worse when blood glucose is under control at the beginning, over time, maintaining lower blood glucose levels helps lessen the symptoms of diabetic neuropathy. More importantly, good blood glucose control may also help prevent or delay the onset of further problems the patients might also have.
Additional treatment depends on the type of nerve problem and symptom. If you want to get appropriate treatment you must first talk to your doctor to determine the exact type of your diabetic neuropathy.
Foot care is another important part of treatment because people with neuropathy need to inspect their feet daily for any injuries. Your doctor should explain all this to you. Untreated injuries increase the risk of infected foot sores and possibly even amputation, which you surely wish to avoid.
Treatment may also includes pain relief and other medications as needed, depending on the type of nerve damage. Keep in mind that smoking significantly increases the risk of foot problems, so if you’re a smoker, ask your health care provider for help in quitting.
- en.wikipedia.org/wiki/Diabetic_neuropathy
- http://www.mayoclinic.com/health/diabetic-neuropathy/DS01045Photo courtesy of GovernmentZA by Flickr : www.flickr.com/photos/governmentza/8286152103/

