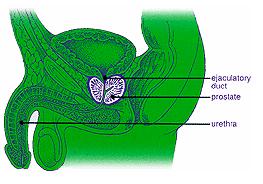
What Are The Functions Of The Prostate?
The prostate produces semen, the fluid that helps nourish and transport sperm. It also assists with ejaculation because of the squeezing contractions of the prostate during orgasm.[1]
It is proven that the prostate goes through two main periods of growth:
- The first period of growth occurs early in male puberty, when the prostate doubles in size.
- This second phase of prostate growth often results in what constitutes an enlarged prostate. As the prostate becomes larger, the layer of tissue surrounding it stops it from expanding, causing the prostate to press against the urethra. This process is most noticeable in middle age and beyond.
What Is Prostatitis?
Prostatitis is a term used to describe an inflammation or infection of the prostate. Since women do not have a prostate gland, it is a condition only found in men. These prostate infections are usually caused by bacteria, but there is also a nonbacterial form of the disease.
There are several risk factors associated with a prostate infection and the most common factors that increase a man's risk include the following [2]:
- A recent urinary tract infection or a problem with your urinary tract
- Having an indwelling urinary catheter
- Having a prostate biopsy
- Prior sexually transmitted diseases such as gonorrhea or Chlamydia
- Having HIV or AIDS
- Anal sex
- Injuring your pelvis
- Smoking
- Excess alcohol consumption
Prostatitis is the most common genitourinary infection in men under the age of 50. The problem is that, although this infection isn't too serious, if left untreated, it can spread to other structures such as the testicles and epididymis and, in severe cases, destroy the prostate gland.
Risk factors for chronic prostatitis include being middle-aged (30 to 50 years of age), having prostatitis in the past and having other painful abdominal conditions, such as irritable bowel syndrome (IBS). Sexual abuse is also a risk factor for chronic prostatitis. [2]
Signs And Symptoms Of Prostatitis
An inflamed prostate can cause a variety of symptoms and the most common ones are [2]:
1. Recurrent urinary tract infections
2. Frequent and urgent urination
3. Difficult or painful urination
4. Urinating at night
5. Fever and chills
6. Generalized sense of ill health
7. Painful ejaculation
8. Bloody semen
9. Sexual dysfunction
10. Pain in the lower back, pelvis, or perineum
Types Of Prostatitis
Depending on what caused it and how long it lasts, there are four types of prostatitis:
1. Acute bacterial prostatitis – This is a form of prostatitis that is relatively easy to diagnose because of the characteristic symptoms. Men with this disease often have chills, fever, pain in the lower back and genital area, and increased urinary frequency especially during the night.
2. Chronic bacterial prostatitis – Recurrent urinary tract infections in men that are spread from a chronic infection in the prostate.
In this case, the symptoms of prostate infection are mildly expressed or there are no symptoms at all. The most common symptoms are simple urinary tract infection symptoms such as painful urinating or burning sensations.
3. Chronic non-bacterial prostatitis – The fact is that chronic prostatitis not caused by bacterial infections is a poorly understood form of the disease. Symptoms can vary in intensity significantly, from mild discomfort to totally debilitating. If we talk about the mechanism of the infection, it can be inflammatory or non-inflammatory. In the inflammatory form, the urine and semen show no evidence of any known infecting organisms and in the non-inflammatory form, no evidence of inflammation, including infection-fighting cells, is present. This is very confusing for scientists. So, some of them even suggested autoimmune theories about the chronic non-bacterial prostatitis.
The most probable suggested causes for non-bacterial prostatitis are:
- Heavy lifting.
- Certain occupations - driving a truck or operating heavy machinery.
- Physical activity – Excessive exercise, especially cycling, may irritate your prostate gland.
- Pelvic muscle spasms.
- Structural abnormalities of the urinary tract.
4. Asymptomatic inflammatory prostatitis - This is a very dangerous form of the disease because there are no symptoms that could indicate the presence of a prostate infection. There is no pain or discomfort but there are white blood cells in the semen, which can be found with a lab analysis.
Diagnosis Of Prostatitis
The patient's reported symptoms and the doctor's physical findings are enough to form a diagnosis of prostatitis in most cases. But sometimes, prostatitis can be difficult to diagnose, primarily because its signs and symptoms often resemble several those signs seen in other conditions. Rectal examination is also a very good diagnostic method because the swollen prostate can be felt under the fingers. It can also be very sore.
A culture of the prostate fluids can also be taken in order to find the presence of microorganisms. This culture is taken by squeezing the gland slightly or via digital massage. When the prostate is inflamed, the fluid should contain a large number of white blood cells.
If the doctor still has some doubts, they may insert a special instrument called a cystoscope through the penis to view the prostate directly from the inside.
Treatment Of Prostatitis
Medications for prostatitis
Depending on the type of prostatitis you have, certain medications may help you get rid of or control your symptoms. These medications include [2]:
1. Antibiotics – Only used in cases of bacterial infection. Before the use of antibiotics, samples of prostatic fluid are tested to determine which bacterium is causing the infection and which drugs should be prescribed to fight the specific bacterium. The treatment may last 4 to 12 weeks, depending on how severe the infection is.
2. Alpha-blockers
3. Pain relievers
4. Muscle relaxants
Acute prostatitis is usually treated with painkillers and a two to four-week course of antibiotics. However, if you're very ill or unable to pass urine, a hospital stay may be needed.
Chronic prostatitis is usually treated with:
- Over the counter painkillers, or if your symptoms are severe, stronger painkillers, such as amitriptyline and gabapentin,
- A medication called an alpha-blocker, to help relax the muscles in the prostate gland and the base of the bladder.
- Occasionally, a four- to six-week course of antibiotics, such as Ciprofloxacin.
Exercises, home remdies, and alternative treatments for prostatitis
1. Exercises for the prostate – These include stretching and relaxing the lower pelvic muscles.
2. Biofeedback - This technique teaches you how to control certain body responses, including relaxing your muscles.
3. Sitz baths - Exposing the perineum to very hot water for 20 minutes or longer often relieves pain.
4. Prostate massage and Kegels for men - Kegel exercises increase pelvic circulation and improve muscle tone.
5. Frequent ejaculation - Ejaculating two or three times a week is often recommended for patients with prostatitis, especially when taking antibiotics.
Surgical Procedures
If a patient has a bacterial form of prostatitis and antibiotics haven't improved the symptoms, surgery may be recommended to open any blocked ducts that may have been confirmed. It is very important to know that surgery is not a treatment for nonbacterial prostatitis. Men may require surgery to treat urinary retention caused by chronic bacterial prostatitis. Surgically removing scar tissue in the urethra often improves urine flow and reduces urinary retention. [3]
Alternative Treatment
Prostate drainage method
This is a treatment that was first popularized in the Philippines. It is performed by inserting a finger into the rectum at regular intervals to increase pressure on the prostate and at the same time, an antibiotic treatment is given. [4]
Acupuncture and Chinese herbal medicine
These traditional Asian forms of medicine can also be effective in treating prostatitis. They may improve urinary flow and decrease swelling and inflammation. [4] At worst, they may subjectively improve the symptoms of men with non-bacterial chronic prostatitis.
Adequate nutrition
- The patient should eat whole, fresh, unrefined, and unprocessed foods, including fresh fruits, vegetables, whole grains, soy, beans, seeds, nuts, olive oil, and cold-water fish.
- Every patient with prostatitis should definitely avoid sugar, dairy products, refined foods, fried foods, junk foods, and caffeine.
- Some would go so far as to suggest to drink 50% of your body weight in ounces of water daily, but although proper hydration is very important, drinking excessive amounts of water can also be dangerous.
Nutritional Supplements for prostatitis
Although it is not well understood how they work, some natural remedies have helped men manage the symptoms of prostatitis.
Many natural supplements are intended to provide nutritional support. Some of the most common supplements are [5]:
- Bromelain helps fight inflammation - Take 400 mg 3 times daily away from meals.
- Proteolytic enzymes – They have anti-inflammatory properties and can increase the effectiveness of antibiotics.
- Vitamin C - Take 500-1000 mg 3 times daily. (Vitamin C stops the growth of E. coli, the most common bacteria involved in bacterial prostatitis).
- Vitamin E - Take 400 IUs daily.
- Flaxseed meal – Take 2-4 tablespoons daily. Flaxseed meal is a good choice because of its fiber, lignan, and vitamin content.
- Probiotics - Supplement with probiotics, such as acidophilus, if taken with antibiotics, can be beneficial for the intestinal flora. Preliminary studies suggest that taking an antibiotic followed by probiotics can help prevent the progression of prostatitis.
- Quercetin – A natural supplement with strong anti-inflammatory properties. May help reduce pain and symptoms of chronic nonbacterial prostatitis. In one study, combining quercetin with bromelain and papain produced even greater effects.
- Selenium - It is an antioxidant, more effective when taken with vitamin E.
- Zinc - Take 30 mg daily. Zinc is vital to the health of the prostate, which concentrates and secretes zinc. Zinc also prevents infections. It is believed to play a critical role in cell growth and differentiation, in regulating normal cell death, as well as in building the immune response. A few preliminary studies suggest that taking zinc with antibiotics works better than antibiotics alone for reducing the symptoms of prostatitis. Be careful with high doses of zinc.
Herbal Natural Supplements
Herbal medicines are very good and effective and what's best about them is that they usually do not have side effects when used appropriately and at suggested doses. Several herbs may be used to treat prostatitis and associated urinary tract infections [5]:
- Bearberry acts as a diuretic and antiseptic for the urinary tract system.
- Echinacea and goldenseal are used to treat infections because of their antiviral and antibacterial properties.
- Flower pollen extract – This herbal supplement has been used in Europe for over three decades to treat prostatitis. However, keep in mind that flower pollen is not the same as bee pollen.
- Pellitory of the Wall - Has anti-inflammatory action in the urinary tract.
- Saw palmetto - Provides several beneficial effects on the prostate and the urinary tract. Saw palmetto can interact with some medications, including hormone replacement therapies and blood thinners, so consult your doctor first before you try it.
- African pygeum - May help reduce urinary symptoms of benign prostatic hyperplasia (enlarged prostate) and both bacterial and nonbacterial prostatitis in men with mild-to-moderate urinary symptoms.
- Stinging nettle - May help maintain prostate health and is rich in numerous vitamins and minerals vital to good health. Stinging nettle can interact with some medications, including those taken diabetes and high blood pressure.
READ Prostatitis cure & treatment
Several other herbs that have been used to treat prostatitis include:
- Uva ursi (Arctostaphylos uva ursi): diuretic, urinary antiseptic
- Goldenseal (Hydrastis canadensis): diuretic, antiseptic, antimicrobial
- Coneflower (Echinacea purpurea): improves immune function
- Corn silk (Zea mays): diuretic, soothing demulcent
There is one other thing that every patient with prostatitis should know and keep in mind. Various herbs and supplements may interact adversely with drugs used to treat prostatitis. Therefore, you should talk to your GP or family doctor about possible interactions before the use of any of those herbs.

