Fortunately, the prognosis for patients with SLE has greatly improved over the last few decades and now at least 80-90% of all patients survive ten years or more. Preventive measures such as influenza and pneumococcal vaccination, TB testing, healthy diet, and exercise could help improve the health status of the patient.
Incidence
Women are disproportionately affected, and SLE is most common in women of child-bearing age. The prevalence in the Unites States has been estimated as approximately 500,000, but a recent research done by the Lupus Foundation of America suggested a prevalence of as many as 2,000,000. A recent study identified a prevalence of 500 per 100,000 in women residing in the area surrounding Birmingham, Alabama.
Possible causes of SLE
Unfortunately, the etiology of SLE is still unknown. However, most experts agree that genetic predisposition, sex hormones, and environmental triggers likely result in the imbalanced immune response, which is the most characteristic sign of the disease.
Genetic predisposition: The increased percentage of two antigens in patients with SLE has been confirmed, HLA-DR2 and HLA-DR3, proving that genetics play a major part. The role ofheredity is further supported by the concordance for this illness among monozygotic twins.
Autoimmune mechanism: The origin of auto-antibodies produced in SLE is unclear. A significant role could be played by an antigen-driven process, spontaneous B-cell hyper-responsiveness, or impaired immune regulation. None of this has been proven yet.
The health status of a patient with SLE is related not only to disease activity, but to the damage that results from recurrent episodes of disease flare, as well as the adverse effects of treatment.
Symptoms of SLE
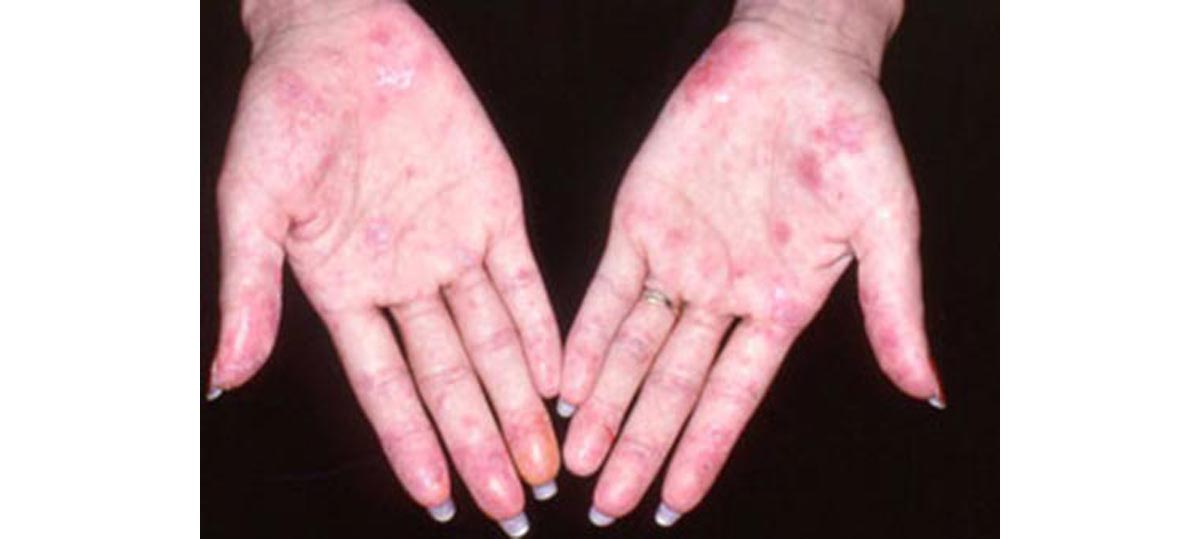
A common complaint is a photosensitive rash, often with alopecia or baldness. However, patients may exhibit signs of fever accompanied by single organ involvement, such as inflammatory serositis, glomerulonephritis, neuropsychiatric disturbance, or hematological disorders.
The following classification of eleven symptoms can help doctors tell the difference between people who have lupus and people who have other connective tissue disorders:
- Rash, extremely specific because it is butterfly–shaped, spread over the cheeks and across the bridge of the nose
- Kidney problems (protein leak)
- Central nervous system problems
- Blood problems (anemia)
- Problems with the immune system (risk of infection)
- Discoid rash (scaly, disk-shaped sores on the face, neck and/or chest)
- Sensitivity to sunlight
- Oral ulcers
- Arthritis (pain, stiffness in joints)
- Serositis (inflammation of the lining around the heart, lungs, abdomen)
- Antinuclear antibodies (auto-antibodies that react against the body's own cells)
Other symptoms include:
- Muscle aches
- Nausea
- Vomiting and diarrhea
- Anemia
- Fatigue
- Fever
- Skin rash
- Swollen glands Lack of appetite
- Sensitivity to cold (known as Raynaud's phenomenon)
- Weight loss
Diagnosis of Lupus
X-ray imaging: Simple radiographs are not routinely useful in the diagnosis or management of SLE. X-rays, however, can be used to evaluate symptomatic patients for necrosis, characteristic for this condition. Chest x-rays and chest CT scans could also be extremely useful in telling the difference between infectious and inflammatory lung disease.
Electrocardiograms (ECG): Electrocardiograms are useful in demonstrating changes characteristic to pericarditis. It may also be required to exclude myocardial infarction in SLE patients with chest pain.
EEG, CT, and MRI: Electroencephalograms could be very useful in evaluating patients with possible neuropsychiatric lupus. They are abnormal in 75% of patients with acute diffuse cerebral dysfunction. Brain CT scans are also nonspecific and have proven less sensitive than MRI in evaluating the central nervous system. MRI is now recognized as the most sensitive technique to identify bone necrosis.
Biopsies: Biopsies are also commonly required for SLE diagnosis. Occasionally, biopsies of the skin are useful to distinguish cutaneous manifestations of lupus from coincidental skin diseases. Renal biopsies are most useful when evaluated by light microscopy, immuno-fluorescence, electron microscopy, WHO classification, NIH activity and chronicity indices.
SLE Treatment
Management of SLE can be a challenge. Treatment depends on symptoms and their severity. Careful and frequent medical evaluation is therefore important for monitoring symptoms and adjusting treatment as necessary.
Conservative therapy – medications
Conservative treatment is appropriate for patients with muscle or joint pain, fatigue, skin manifestations, and other non-life-threatening features. These options include:
- Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen (Motrin®, Advil®) and naproxen (Naprosyn®)
- Anti-malarial medications such as Hydroxychloroquine (Plaquenil®).
More aggressive therapy is required for life-threatening manifestations such as kidney inflammation, lung or heart involvement, and central nervous system symptoms. Treatment in these circumstances might involve:
- High doses of corticosteroids such as Prednisone® (Deltasone)
- Other immunosuppressive drugs such as Azathioprine (Imuran®), Cyclophosphamide (Cytoxan®), and Cyclosporine (Neoral®, Sandimmune®)
Prognosis
Although the treatment for SLE has improved and long-term survival has increased significantly, it still remains a chronic disease that can limit activities. Very often the quality of life is compromised by symptoms like fatigue and joint pain, which are not life-threatening. The best way to control lupus is to take all your medications as prescribed, visit your physician regularly, and learn as much as you can about both the condition and the medications.
Simply maintaining an active lifestyle will usually help keep joints flexible and may prevent cardiovascular complications. Patients with lupus should avoid excessive sun exposure because the ultraviolet rays can cause a skin rash to flare. Wearing simple protective clothing and using sunscreen when going outside should protect against such complications.
There are several controversies about pregnancy and lupus. Young women with lupus who wish to have a baby should carefully plan their pregnancies with, of course, detailed guidance of their doctor. Although it could be very complicated, it would help to time the pregnancy for a period when the disease is least active. While carefully monitoring the pregnancy, pregnant woman should also avoid certain medications such as Cyclophosphamide, Cyclosporine, and mycophenolate.
READ Ten Advances In The Fight Against Lupus
Estrogen and lupus
There is a possibility that the use of estrogen may induce or worsen lupus. Fortunately, recent research has shown that estrogen can actually trigger some mild or moderate flares of lupus, but does not cause severe exacerbation of the symptoms. However, since estrogen can increase the risk of blood clots, it should be avoided by patients with lupus.

