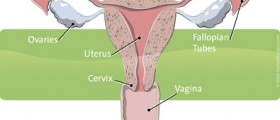
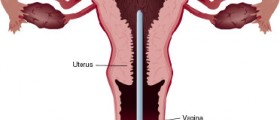
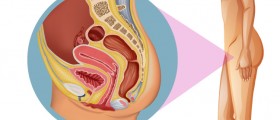
Endometrial hyperplasia is a clinical condition that patients should not ignore yet the pathology of this condition does not always lead to cancer. Endometrial hyperplasia is a cascade of numerous histological changes to the tissue in the endometrium. At the start, these changes are often minor and resemble the normal tissue of the inner uterus but as this condition goes unchecked, patients become more likely to start to notice precancerous lesions.
The one thing to keep in mind with this condition is the fact that endometrial hyperplasia usually starts as unchecked secretions of estrogen hormone into the uterus. This can either be exogenous or endogenous and women will often present at first with painless vaginal bleeding.
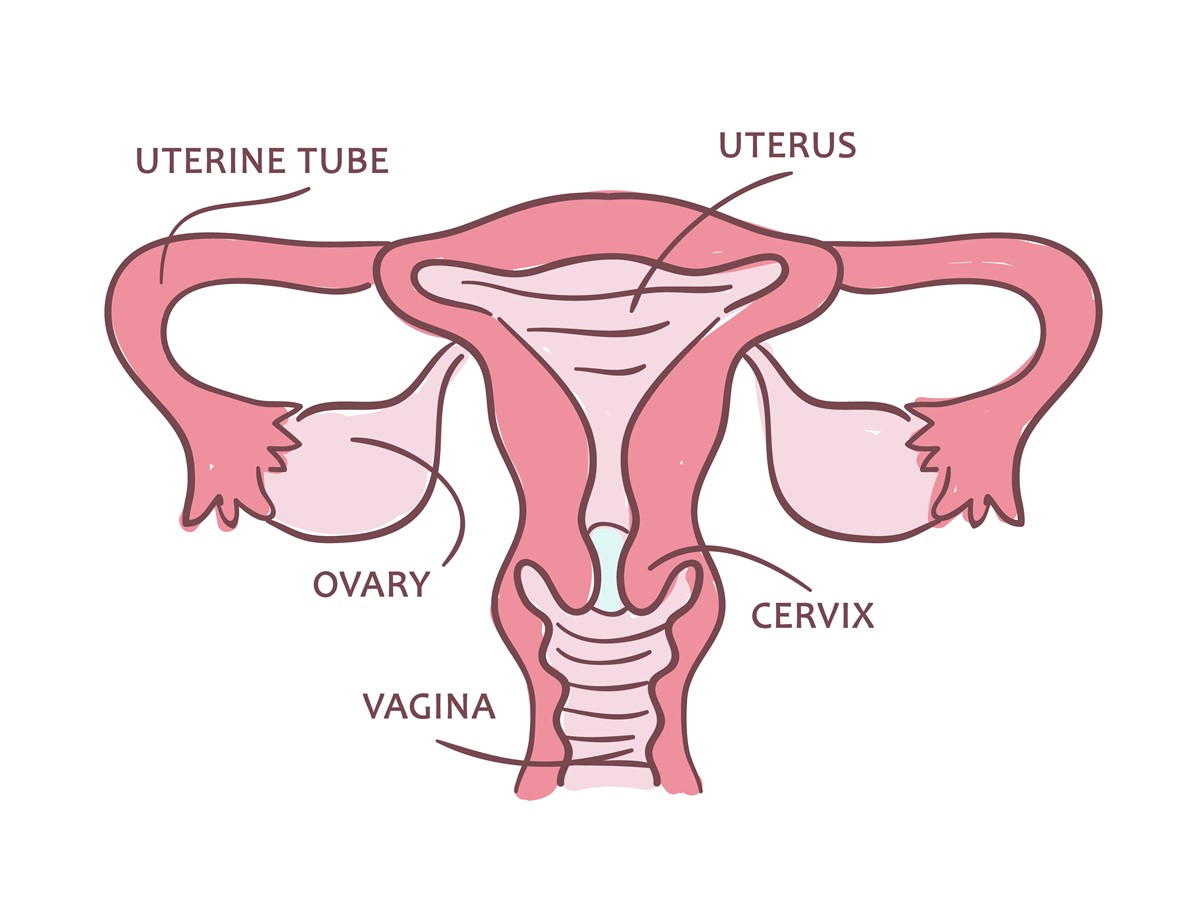
Endometrial hyperplasia is a disease spectrum that can be sub-classified into 3 smaller categories:
- Simple hyperplasia is the first category and the tissue of the hyperplastic cells is almost identical to normal tissue and the risk of progression to cancer is almost impossible.
- Complex hyperplasia is the next category and histological changes are more evident but there is only a mild risk of eventually developing cancer.
- Atypical hyperplasia is the last category and this is where the glandular tissue is most bizarre. This is also the category that possesses the biggest risk to eventually developing endometrial carcinomas.
When patients notice this abnormal bleeding, the most paramount thing to do is go to your local gynecologist and get this symptom worked-up. A physician should perform a biopsy in order to determine the type of histology at the tissue level and women should also have transvaginal ultrasounds done to determine if there is abnormal masses that could indicate some type of female organ cancer in the ovaries or uterus.
Endometrial hyperplasia management depends entirely on the age, the fertility status and the desire for future pregnancies of the patient. If the patient is in menopause or no longer wants to have more children, the definite treatment to avoid further malignant transformation would be to have a total hysterectomy. When the entire uterus is removed, excessive estrogen will be unable to effect the tissue any longer and the woman's risk of cancer is essentially nil.
If the woman is at a younger age and still wishes to have children in the future, the situation becomes slightly more complicated yet not impossible. Progestogens are the first-line treatment for patients falling under this category. This will help suppress the high levels of estrogen circulating around the body and may help the tissue from undergoing hyperplastic changes. [1]
The severity of the endometrial hyperplasia seems to depend on the age of when symptoms first appear. In epidemiological studies, it was determined that women in their 50s typically have milder forms of the disease while those in their 60s have variations that are more likely to progress to cancer.
Although endometrial cancer is the most common type of gynecological cancer in the female population (22.3/100,000 patients), a diagnosis of endometrial hyperplasia is not a guarantee that you will be having cancer in your future. [2]
- Photo courtesy of SteadyHealth