I am a 46 year old male in good health although I could lose 20 pounds or so. I am going to be one of the "unique" stories you will find. I will post what I can and be looking for specific questions that I will answer as quickly as possible. These types of sites have been quite helpful to me and I want to return the favor and provide hope to those that may be a little discouraged at the moment. I don't know how much the site will allow me to write but I want to be as specific as possible so similarities can be realized.
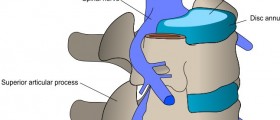
I had a ACDF (C5/6 and C6/7) last November 13th so I guess it ahs been about 9 weeks or so. I had NO pain and NO symptoms prior to surgery. In December of 2007, I hurt my lower back playing racquetball after hitting the back wall. Having my share of aches and pains playing this game, I was surprised when it did not go away. In March of 2008 I went to see my doctor and he ordered a lumbar x-ray which came back negative. Then he ordered a lumbar MRI (first time and it scared the c**p out of me) which also came back fine. Then he proceeds to tell me how I could have injured my upper-back/neck and the pain was being "transferred" to my lower back. I thought he was nuts but after some further discussions I agreed to go because I had the highest faith in him. I still remember the day I got home from the gym (racquetball) and heard the message on the recorder from the doctor that the results from the cervical MRI had come back and there was something we needed to "chat" about. It turns out that I had severe stenosis and other medical terms going on where my spinal cord was being compressed by my vertebrae and disks. He said I needed to go talk to a NS and see what was going on.
In early April, I went to one of the best NS here. Since I had turned in my films upon my arrival, the doctor had already put them on the wall and had been looking at them. He was amazed when they called me back and saw me pain free. He was further bewildered when I had told him that I had no symptoms and really had no idea what was going on. He put me through a range of exercises which I completed with no problems. He informed me that my pictures looked "ugly" and that I had some serious compression on my spinal cord but that for me to have no pain and no symptoms was incredible. When I asked him the possible cause, he said "well it can be a tumor, it could be MS, or it could be the result of an injury, either recent or years ago". Of course this upset me and pretty much kicked my legs out from under me. He said based on my pictures I should be having surgery within a week but with no pain or symptoms, it was decided to wait a 5 or 6 months and take another MRI. This of course was only if no pain or symptoms presented themselves.
Meanwhile, I scheduled another appointment with my doctor who saw that I was upset with what the NS had said. He asked a Radiologist to take another look at the pictures who confirmed that the problem was injury related (at some time during my 45 years on planet earth). We decided to take the "wait and see" approach. I continued all of my physical activities as usual.
On a 15-hour flight to Asia in July, I was about 10 hours into it when I went to stretch out in my seat. As I pressed the back of my head against the seat back, I felt a sort of "jolt" down my left arm. Although unusual, as well as un-nerving at the time, it never happened again. But in August I started noticing a similar sensation as I would reach for something with my right hand (particularly picking something up off the floor) I would get a "tingle" down my left arm and hand. Nothing to get to worried about and I knew my follow-up MRI was in a few weeks. To be continued....
Continued.....
I had a followup MRI (the new advanced "3T") completed in October. It showed increased pressure against my spinal cord at C5/6 and C6/7 to the point that discoloration (actual signal disruption) could be observed. The NS, the one I had seen in March, informed me that I was "one bad cough or wrong sneeze from severing my spinal cord" and that the time for surgery was now!!! This was a little un-nerving since I had been playing racquetball 2 days before and playing touch football with my nephews the previous weekend. I told the NS I wanted to get a second opinion.
I went to see a second neurosurgeon, another top-rated NS having completed over 1,500 of these operations (I'll call him NS2) and he was also amazed at the contradiction between the pictures and my lack of pain or symptoms. However, he expressed the same problem, the same suregery, and the same need for immediate action. The one thing that was a complete 180 from the first NS was the post-op program. The first neurosurgeon, the one I saw in March, had told me I would be looking at wearing a hard collar for 4-6 weeks, a soft collar for another 2-3 weeks, no driving for 2 months and no flying for 6 months. Now N2 is telling me that he would not have me wearing a collar, and that if I felt up to it (which he knew I wouldn't due to the pain I would be experiencing). Now although I liked what NS2 was saying, I didn't want to take the preferred route but wanted the best one. After intense research on many sires such as this one, I discovered there are actually 2 distinct "schools of thought" on this one and it just depended on which one the particular NS prescribed to. There is plenty of discussion boards disuccing this. I decided to go with NS2 and surgery was scheduled for November 13th.
Surgery was pretty much as planned. I did elect to stay a second night in the hospital (thank goodness for good health insurance) and I think this helped facilitate my good recovery. They kept me pretty well drugged in the hospital with morphine etc but discovered that my body does not process dilaudid (10 times stronger than morphine) so that was not providing any relief. The next 2 weeks at home was pretty much what everyone else has described: sleepless nights, meds every 4 hours, terrible neck, shoulder, and arm pains, bladder fluctuations, and so on. There was plenty of Icey-Hot being used on the arms and across the shoulders. I stayed in the guest room so I would not keep my wife awake and she would not wake me up if I was fortunate enough to doze off. In week 3, I started taking an Ambien to help me get some quality sleep. I think this started to play a major role as well. I figured it couldn't be any worse than the Percocet/Soma I was taking in the middle of the night when I was unable to sleep and experiencing the pain. During my first post-op appointment (week 3), the NS said the wound was healing fine and there was really no restrictions he was placing on my activities.....that I would know my thresholds. I drove home from the appointment as I was not under any meds at the time. Pretty much had all ROM in my neck.
At week 4 I was working (via remote access) from my dining room table. 2-3 hours at a time but I was still able to manage 40 hours or so within the 5 days. I was climbing up and down the ladder and unloading boxes and totes out of the attic to retrieve the Christmas decorations. Still taking meds occasionally, usually to address minor pains from possibly over doing a little the previous day. Pain now was primarily in my biceps and triceps from time to time.
At week 5 I am driving into work (desk job) and working a full week. But I did make it habit to get up and walk the facility frequently. Also walking 1-2 miles in the neighborhood. I resumed my normal amount of driving.
On week 6, I am on a 6-hour flight to the northeast for the holidays. No problem with the flight but I noticed as I spent time in the cold sightseeing (9 degrees and wind chill of -10) that I was frequently experiencing severe headaches. Never had migraines but if this is what they are like, I have empathy for those that do. Once I returned to a warmer climate, this went away immediately.
Week 7 to the present has been pretty much my pre-surgery routine (no racquetball until May though per NS2). Flying and driving at will. Hiking 5-7 miles when I want to. Using light weights to regain muscle mass in my arms.
Next week, I have my 2nd post-op visit with operating NS. Strangely enough, he (at least his staff) has informed me that I do not need to have a x-ray (or MRI) completed yet. However, my personal physician has offered to order one for me. I will be returning to the 16 hour flights and my travels through Asia in mid February and want to confirm that things are aligned and "fusing" as desired. It should be an interesting meeting with the NS2.
I'm sorry this has been so long but I think that it is important to provide as much information so that others can see similarities to what they may be experiencing. From what I have read on these sites, I am damn lucky. Lucky to have discovered the problem to begin with (my personal doctor probably saved my life, if nothing else saved me from being paralyzed in the next 6-12 months). Lucky that I have had very little complications. The only symptoms I have had the last 3-4 weeks is a numbness/tingling in my neck between the incision site and my chin (may take up to a year to completely go away) and a numbness/tingling in my left hand (fingertips and thumb). I do carry a percocet in my pocket every day, but more days than not, I do not end up needing it.
So the best advice I can give is:
- STAY POSITIVE
- FIND A TRUST A GOOD DOCTOR
- GET A SECOND OPINION
- GET PLENTY OF REST
AND AGAIN STAY POSITIVE !!!
I had a ACDF (C5/6 and C6/7) last November 13th so I guess it ahs been about 9 weeks or so. I had NO pain and NO symptoms prior to surgery. In December of 2007, I hurt my lower back playing racquetball after hitting the back wall. Having my share of aches and pains playing this game, I was surprised when it did not go away. In March of 2008 I went to see my doctor and he ordered a lumbar x-ray which came back negative. Then he ordered a lumbar MRI (first time and it scared the c**p out of me) which also came back fine. Then he proceeds to tell me how I could have injured my upper-back/neck and the pain was being "transferred" to my lower back. I thought he was nuts but after some further discussions I agreed to go because I had the highest faith in him. I still remember the day I got home from the gym (racquetball) and heard the message on the recorder from the doctor that the results from the cervical MRI had come back and there was something we needed to "chat" about. It turns out that I had severe stenosis and other medical terms going on where my spinal cord was being compressed by my vertebrae and disks. He said I needed to go talk to a NS and see what was going on.
In early April, I went to one of the best NS here. Since I had turned in my films upon my arrival, the doctor had already put them on the wall and had been looking at them. He was amazed when they called me back and saw me pain free. He was further bewildered when I had told him that I had no symptoms and really had no idea what was going on. He put me through a range of exercises which I completed with no problems. He informed me that my pictures looked "ugly" and that I had some serious compression on my spinal cord but that for me to have no pain and no symptoms was incredible. When I asked him the possible cause, he said "well it can be a tumor, it could be MS, or it could be the result of an injury, either recent or years ago". Of course this upset me and pretty much kicked my legs out from under me. He said based on my pictures I should be having surgery within a week but with no pain or symptoms, it was decided to wait a 5 or 6 months and take another MRI. This of course was only if no pain or symptoms presented themselves.
Meanwhile, I scheduled another appointment with my doctor who saw that I was upset with what the NS had said. He asked a Radiologist to take another look at the pictures who confirmed that the problem was injury related (at some time during my 45 years on planet earth). We decided to take the "wait and see" approach. I continued all of my physical activities as usual.
On a 15-hour flight to Asia in July, I was about 10 hours into it when I went to stretch out in my seat. As I pressed the back of my head against the seat back, I felt a sort of "jolt" down my left arm. Although unusual, as well as un-nerving at the time, it never happened again. But in August I started noticing a similar sensation as I would reach for something with my right hand (particularly picking something up off the floor) I would get a "tingle" down my left arm and hand. Nothing to get to worried about and I knew my follow-up MRI was in a few weeks. To be continued....
Continued.....
I had a followup MRI (the new advanced "3T") completed in October. It showed increased pressure against my spinal cord at C5/6 and C6/7 to the point that discoloration (actual signal disruption) could be observed. The NS, the one I had seen in March, informed me that I was "one bad cough or wrong sneeze from severing my spinal cord" and that the time for surgery was now!!! This was a little un-nerving since I had been playing racquetball 2 days before and playing touch football with my nephews the previous weekend. I told the NS I wanted to get a second opinion.
I went to see a second neurosurgeon, another top-rated NS having completed over 1,500 of these operations (I'll call him NS2) and he was also amazed at the contradiction between the pictures and my lack of pain or symptoms. However, he expressed the same problem, the same suregery, and the same need for immediate action. The one thing that was a complete 180 from the first NS was the post-op program. The first neurosurgeon, the one I saw in March, had told me I would be looking at wearing a hard collar for 4-6 weeks, a soft collar for another 2-3 weeks, no driving for 2 months and no flying for 6 months. Now N2 is telling me that he would not have me wearing a collar, and that if I felt up to it (which he knew I wouldn't due to the pain I would be experiencing). Now although I liked what NS2 was saying, I didn't want to take the preferred route but wanted the best one. After intense research on many sires such as this one, I discovered there are actually 2 distinct "schools of thought" on this one and it just depended on which one the particular NS prescribed to. There is plenty of discussion boards disuccing this. I decided to go with NS2 and surgery was scheduled for November 13th.
Surgery was pretty much as planned. I did elect to stay a second night in the hospital (thank goodness for good health insurance) and I think this helped facilitate my good recovery. They kept me pretty well drugged in the hospital with morphine etc but discovered that my body does not process dilaudid (10 times stronger than morphine) so that was not providing any relief. The next 2 weeks at home was pretty much what everyone else has described: sleepless nights, meds every 4 hours, terrible neck, shoulder, and arm pains, bladder fluctuations, and so on. There was plenty of Icey-Hot being used on the arms and across the shoulders. I stayed in the guest room so I would not keep my wife awake and she would not wake me up if I was fortunate enough to doze off. In week 3, I started taking an Ambien to help me get some quality sleep. I think this started to play a major role as well. I figured it couldn't be any worse than the Percocet/Soma I was taking in the middle of the night when I was unable to sleep and experiencing the pain. During my first post-op appointment (week 3), the NS said the wound was healing fine and there was really no restrictions he was placing on my activities.....that I would know my thresholds. I drove home from the appointment as I was not under any meds at the time. Pretty much had all ROM in my neck.
At week 4 I was working (via remote access) from my dining room table. 2-3 hours at a time but I was still able to manage 40 hours or so within the 5 days. I was climbing up and down the ladder and unloading boxes and totes out of the attic to retrieve the Christmas decorations. Still taking meds occasionally, usually to address minor pains from possibly over doing a little the previous day. Pain now was primarily in my biceps and triceps from time to time.
At week 5 I am driving into work (desk job) and working a full week. But I did make it habit to get up and walk the facility frequently. Also walking 1-2 miles in the neighborhood. I resumed my normal amount of driving.
On week 6, I am on a 6-hour flight to the northeast for the holidays. No problem with the flight but I noticed as I spent time in the cold sightseeing (9 degrees and wind chill of -10) that I was frequently experiencing severe headaches. Never had migraines but if this is what they are like, I have empathy for those that do. Once I returned to a warmer climate, this went away immediately.
Week 7 to the present has been pretty much my pre-surgery routine (no racquetball until May though per NS2). Flying and driving at will. Hiking 5-7 miles when I want to. Using light weights to regain muscle mass in my arms.
Next week, I have my 2nd post-op visit with operating NS. Strangely enough, he (at least his staff) has informed me that I do not need to have a x-ray (or MRI) completed yet. However, my personal physician has offered to order one for me. I will be returning to the 16 hour flights and my travels through Asia in mid February and want to confirm that things are aligned and "fusing" as desired. It should be an interesting meeting with the NS2.
I'm sorry this has been so long but I think that it is important to provide as much information so that others can see similarities to what they may be experiencing. From what I have read on these sites, I am damn lucky. Lucky to have discovered the problem to begin with (my personal doctor probably saved my life, if nothing else saved me from being paralyzed in the next 6-12 months). Lucky that I have had very little complications. The only symptoms I have had the last 3-4 weeks is a numbness/tingling in my neck between the incision site and my chin (may take up to a year to completely go away) and a numbness/tingling in my left hand (fingertips and thumb). I do carry a percocet in my pocket every day, but more days than not, I do not end up needing it.
So the best advice I can give is:
- STAY POSITIVE
- FIND A TRUST A GOOD DOCTOR
- GET A SECOND OPINION
- GET PLENTY OF REST
AND AGAIN STAY POSITIVE !!!
Loading...
I think that there are reasons for some people to have to wear the hard collar. One case is like in my recovery where my NS had to protect another disk that was not operated on just below the 2 he did fix.
Thank you for contributing.
Rob
Thank you for contributing.
Rob
Loading...