Hello,
I am about to under go Anterior Cervical Discectomy Fusion with Cadaver bone and a metal plate in one week. I began with severe pain in my left arm and shoulder and numbness, tingling and pain in my left forearm and thumb. I also have a reduction in strength in my left arm and hand. The only thing that could control my pain was percocet. After four weeks with no improvement I was scheduled for an MRI. The MRI showed disc degeneration at C6 and C7. The Disc at C7 was herniated to the point that it is compressing the spinal cord. My Neurosurgeon is recommending that I have ACDF at C5-6 and C6-7. I am a very active person and I'm very concerned about my recovery time. After reading the posts here, I see that it varies from person to person. Some are doing well in two weeks and others take months. Since there seems to be so much difference, I was wondering if others would find it helpful if I shared my pre and post op experience. I'm willing to share my age, weight, etc to give others an idea what they might face. This is a very scary experience and I'm just thinking that as much information as possible might be helpful to others.
I am about to under go Anterior Cervical Discectomy Fusion with Cadaver bone and a metal plate in one week. I began with severe pain in my left arm and shoulder and numbness, tingling and pain in my left forearm and thumb. I also have a reduction in strength in my left arm and hand. The only thing that could control my pain was percocet. After four weeks with no improvement I was scheduled for an MRI. The MRI showed disc degeneration at C6 and C7. The Disc at C7 was herniated to the point that it is compressing the spinal cord. My Neurosurgeon is recommending that I have ACDF at C5-6 and C6-7. I am a very active person and I'm very concerned about my recovery time. After reading the posts here, I see that it varies from person to person. Some are doing well in two weeks and others take months. Since there seems to be so much difference, I was wondering if others would find it helpful if I shared my pre and post op experience. I'm willing to share my age, weight, etc to give others an idea what they might face. This is a very scary experience and I'm just thinking that as much information as possible might be helpful to others.
Loading...
Thank you for sharing your personal experience with us. I wish all go well with you.
Loading...
3 Days Pre-Op
Today is Monday and my surgery is scheduled for Thursday. Here is my baseline information:
Male, 53
Height: 5ft, 11 3/4 in
Weight: 220lb (approx 30lb overweight)
Non-smoker
Profession: IT Services Manager (computer work)
Up to this point, I've been fairly active - bicycling, walking and martial arts class three times a week.
Hypertensive: medicated to 150/90
Symptoms and treatment:
I've had intermittent symptoms for about four to five years that I've put down to muscle pulls etc.: pain in my shoulder, bicep, neck and forearm. Eight weeks ago, I was digging two, two foot deep post holes in rocky ground and began to experience pain in my left deltoid and bicep muscle which I put down to a "pinched nerve". I also noticed that I was experiencing numbness in my forearm and thumb. The pain became quite severe and my doctor put me on percocet and a taper dose of prednesone (4 pills for 3 days, then 3 for 3 days, etc). I took the percocet only to get sleep and the pain began to get better. By the time the prednesone reached to 2 pills per day level, the pain was back with a vengeance. I was also now experiencing weakness in my arm and wrist and shoulder and neck pain (rather like someone trying to drive a spike into my shoulder blade). I went back to the doctor and was given an increased dosage of Prenesone and percocet and scheduled for an MRI. The Prednesone began to have an effect on the inflammation almost immediately. By the time I had the MRI (five days later) I was able to control most of the pain with advil and only take the percocet to sleep. The results of the MRI caused my doctor to refer me to a neurosurgeon immediately with "major degeneration of the disc and vertebrae at C3 through C7". The Neurosurgeon let me see my MRI film and they were pretty scary: the disk at C7 is herniated to the point of compressing the spinal cord. The disc at C6 is also herniated. The vertebrae at C6 and C7 are also eroded and unstable. The neurosurgeon performed a couple of test for strength and sensitivity on my left and right sides and said that to avoid permanent nerve damage, I should have immediate surgery. With surgery, the prognosis is 90%+ chance of restoring strength and sensitivity on the left side and eliminating the pain.
As of this point, 9 weeks from the onset of the major symptoms, the pain is down to a manageable level with tylenol/advil every four hours. Weakness and numbness are constant on the left side. I have two doctors appointment before the surgery; one with my doctor and one with the neurosurgeon. More to come each day.
Today is Monday and my surgery is scheduled for Thursday. Here is my baseline information:
Male, 53
Height: 5ft, 11 3/4 in
Weight: 220lb (approx 30lb overweight)
Non-smoker
Profession: IT Services Manager (computer work)
Up to this point, I've been fairly active - bicycling, walking and martial arts class three times a week.
Hypertensive: medicated to 150/90
Symptoms and treatment:
I've had intermittent symptoms for about four to five years that I've put down to muscle pulls etc.: pain in my shoulder, bicep, neck and forearm. Eight weeks ago, I was digging two, two foot deep post holes in rocky ground and began to experience pain in my left deltoid and bicep muscle which I put down to a "pinched nerve". I also noticed that I was experiencing numbness in my forearm and thumb. The pain became quite severe and my doctor put me on percocet and a taper dose of prednesone (4 pills for 3 days, then 3 for 3 days, etc). I took the percocet only to get sleep and the pain began to get better. By the time the prednesone reached to 2 pills per day level, the pain was back with a vengeance. I was also now experiencing weakness in my arm and wrist and shoulder and neck pain (rather like someone trying to drive a spike into my shoulder blade). I went back to the doctor and was given an increased dosage of Prenesone and percocet and scheduled for an MRI. The Prednesone began to have an effect on the inflammation almost immediately. By the time I had the MRI (five days later) I was able to control most of the pain with advil and only take the percocet to sleep. The results of the MRI caused my doctor to refer me to a neurosurgeon immediately with "major degeneration of the disc and vertebrae at C3 through C7". The Neurosurgeon let me see my MRI film and they were pretty scary: the disk at C7 is herniated to the point of compressing the spinal cord. The disc at C6 is also herniated. The vertebrae at C6 and C7 are also eroded and unstable. The neurosurgeon performed a couple of test for strength and sensitivity on my left and right sides and said that to avoid permanent nerve damage, I should have immediate surgery. With surgery, the prognosis is 90%+ chance of restoring strength and sensitivity on the left side and eliminating the pain.
As of this point, 9 weeks from the onset of the major symptoms, the pain is down to a manageable level with tylenol/advil every four hours. Weakness and numbness are constant on the left side. I have two doctors appointment before the surgery; one with my doctor and one with the neurosurgeon. More to come each day.
Loading...
2 Days Pre-Op
I already had a physical scheduled for today with my regular doctor so I kept that appointment. My blood pressure is now VERY high 152/104. My doctor has me on increased meds for my BP. He let me know that if my pressure doesn't come down into the low 90's by Thursday, they will probably postpone my surgery.
My doctor confirmed that I've lost .25 to .5 inch of height, based on old physicals. This is due to the disc compression in my cervical spine.
From this, I can anticipate that I will probably experience some degree of muscle pain and stiffness in my neck after the surgery. After all, they will be expanding my neck back to close to it original length. This will stretch the muscles in my neck which will cause soreness, stiffness and my even contribute to difficulty in swallowing.
I have a list of questions I will be asking my neurosurgeon in my pre-op meeting tomorrow, which I will post after the meeting with his answers.
The Pain in my shoulder/neck/arm is manageable right now and, with tylenol/advil is down to a dull ache. It's the numbness and weakness in my arm and hand that is driving my crazy. When they drew blood this morning in my physical I could barely squeeze the foam ball. Creepy.
I already had a physical scheduled for today with my regular doctor so I kept that appointment. My blood pressure is now VERY high 152/104. My doctor has me on increased meds for my BP. He let me know that if my pressure doesn't come down into the low 90's by Thursday, they will probably postpone my surgery.
My doctor confirmed that I've lost .25 to .5 inch of height, based on old physicals. This is due to the disc compression in my cervical spine.
From this, I can anticipate that I will probably experience some degree of muscle pain and stiffness in my neck after the surgery. After all, they will be expanding my neck back to close to it original length. This will stretch the muscles in my neck which will cause soreness, stiffness and my even contribute to difficulty in swallowing.
I have a list of questions I will be asking my neurosurgeon in my pre-op meeting tomorrow, which I will post after the meeting with his answers.
The Pain in my shoulder/neck/arm is manageable right now and, with tylenol/advil is down to a dull ache. It's the numbness and weakness in my arm and hand that is driving my crazy. When they drew blood this morning in my physical I could barely squeeze the foam ball. Creepy.
Loading...
You may want to consider autologous blood transfusion as a mean to lower your blood pressure to an acceptable level prior to your surgery. During this procedure, a volume of blood is removed each day prior to the surgery and stored until it is needed. By reducing your total blood volume each day, your blood pressure will also be reduced.
Loading...
Thanks! Very interesting suggestion that I wouldn't have even thought of. Much Appreciated!
Loading...
One thing I found out... The enormouse pain we all have suffered makes our blood pressures go up! A doctor finaly told me that is why mine was so high pre-op and post-op. It is now settling down after 6 months.
And, yes, please share for others. This site sure helped me understand what I was feeling and I was able to interact with ppl who cld answer my questions when doctors would not. Just make sure to let ppl know that what you are going to go through is not what they can expect but one of the many possable ways they may experience it.
GOOD LUCK tomm.!!!!
Rob
And, yes, please share for others. This site sure helped me understand what I was feeling and I was able to interact with ppl who cld answer my questions when doctors would not. Just make sure to let ppl know that what you are going to go through is not what they can expect but one of the many possable ways they may experience it.
GOOD LUCK tomm.!!!!
Rob
Loading...
Good thing you got in quickly for the surgery. I do believe the longer the nerve root is compromised, the more difficulty you'll have in recovery. Oh, and it's interesting that when I was in the ICU after surgery, they constantly monitor your blood pressure and mine spiked up whenever I had to move due to the pain. Pain definitely increases your BP!
I had ACDF for levels C5-7 with bone graft and plate. Those 3 discs had collapsed somewhere between my MRI and actual surgery. I also have stenosis. The neurosurgeon was all pumped up to tell me I'd be an inch taller after surgery, but I believe my neck "settled" after just a few days because I was 5'11" before and after (and since I'm a woman, didn't really need to be any taller :-) )! I felt immediately better after surgery. The 7 wk recovery (so far) has been an incredible test of patience since I'm used to being physically active - but I have been lifting 40 lb. objects the last couple of weeks and haven't had a problem. I have more problems when I just sit around too long. Movement has definitely been my friend. Keep up the good attitude and hoping your surgery is as successful as mine has been. I know I've been fortunate, but it somehow balances out the misfortune of having 10 years of pain from disc degeneration and stenosis.
I had ACDF for levels C5-7 with bone graft and plate. Those 3 discs had collapsed somewhere between my MRI and actual surgery. I also have stenosis. The neurosurgeon was all pumped up to tell me I'd be an inch taller after surgery, but I believe my neck "settled" after just a few days because I was 5'11" before and after (and since I'm a woman, didn't really need to be any taller :-) )! I felt immediately better after surgery. The 7 wk recovery (so far) has been an incredible test of patience since I'm used to being physically active - but I have been lifting 40 lb. objects the last couple of weeks and haven't had a problem. I have more problems when I just sit around too long. Movement has definitely been my friend. Keep up the good attitude and hoping your surgery is as successful as mine has been. I know I've been fortunate, but it somehow balances out the misfortune of having 10 years of pain from disc degeneration and stenosis.
Loading...
1 Day Pre-Op
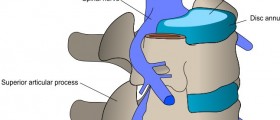
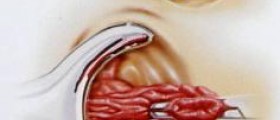
I just returned from my pre-op surgical consult and pre-admission to the hospital. The meeting with my surgeon went very well and he was very forth coming with information and had no hesitation answering my questions. My neurosurgeon, once again, ran through the procedure: This is surgery under general anesthetic (I will be unconscious). They will make a small incision in my neck about two inches long and move the muscles, veins, arteries, trachea and esophagus out of the way to expose the spinal column. They will cut out the disk between C5 and C6 and put in a piece of cadaver bone. He will remove osteophyetes from the foramina and then repeat the procedure between C6 and C7. Then he will place a titanium metal bracket from C5 to C7 and screw it in place. They will then close the incision.
So, based on all that, here are the questions I asked and his answers:
Q: I am assuming I will be entabated (breathing tube inserted down my airway)?
A: Yes. That's standard for this kind of surgery.
Q: So I can expect my throat to be sore and possibly have difficulty swallowing and speaking?
A: Your throat will definitely be sore, but the degree varies from person to person. Some people have no trouble speaking right away and others find it more difficult.
Q: What about swallowing?
A: Again, it varies. Definitely soft foods for a few days, or even the first week. Take it at your own pace.
Q: Will I need and NG (nasal-gastric) tube?
A: No. There's no reason for that.
Q: Will I need to wear a collar?
A: Yes. I'll want you to wear one for about the first four weeks. The muscles in your neck are going to sore and we will want to keep your neck in a stable position.
Q: Will it be a hard collar or soft collar?
A: It will be a hard collar, but you don't have to wear it all the time. You don't have to wear it when you're sleeping or showering or if you if you're watching TV and your resting your head.
Q: Will I need physical therapy?
A: Yes, you'll need physical therapy because we're going to be stretching our your neck muscles. They're going to be sore and stiff so, we'll have you in physical therapy after about two weeks.
Q: When are will I be able to drive?
A: You can drive as soon as you are off the narcotic pain medication.
Q: Will I need to stay in the hospital over night?
A: Well, that will be partially up to you. After you are ready to come out of post-op, we'll move you to a room for a few hours. At that time I'll discuss with you whether or not you should go home. I think it's a good idea to stay overnight; we can manage your pain and watch you. But, if you feel comfortable enough you can certainly go home.
Q: How long before I can start doing some light exercise? Like riding a bicycle or Bowling or something mildly aerobic?
A: Well, we want you to be up and moving as soon as possible, so I'd say you can start doing something aerobic pretty much as soon as you're comfortable.
Q: I've read that it takes three months for the fusion to complete, is that right.
A: It's actually more like six months. You and I will be meeting every few weeks to take X-Rays and look at the progress. I would say that we should see a good beginning to the fusion at three months.
Q: I've read about something called "Adjacent Disc Degeneration" that can happen from ACDF. Is that something to be concerned about?
A: There is a lot of conjecture in the medical field about this. This is where the disc adjacent to the fusion, either above or below, deteriorates over time. At this time we believe the people who are primarily at risk for this are post menopausal women over 50, or anyone who has osteoperosis.
Q: So, what will happen if you find something unexpected once you get to the spine and vertebrae.
A: That's very unlikely. MRI's are very comprehensive and revealing. Typically we might find a calcified disc that I might have to grind out or a herniation that protrudes more than is shown on the MRI, but nothing really out of the ordinary.
These were all of the questions that I asked.
At my pre-admission, the hospital screened me for any preexisting conditions that might effect my surgery, took some blood for a clotting test and did an EKG. One other thing they did was take my blood pressure, which was again very high. I was informed by the nurse that if my systolic was over 100 they would have to postpone and reschedule my surgery. They will make that decision tomorrow. I've taken my BP this evening and I'm now well below 100 so it will probably be a go. If not I will post tomorrow with a status, other wise it will be a day or two until I post again
I just returned from my pre-op surgical consult and pre-admission to the hospital. The meeting with my surgeon went very well and he was very forth coming with information and had no hesitation answering my questions. My neurosurgeon, once again, ran through the procedure: This is surgery under general anesthetic (I will be unconscious). They will make a small incision in my neck about two inches long and move the muscles, veins, arteries, trachea and esophagus out of the way to expose the spinal column. They will cut out the disk between C5 and C6 and put in a piece of cadaver bone. He will remove osteophyetes from the foramina and then repeat the procedure between C6 and C7. Then he will place a titanium metal bracket from C5 to C7 and screw it in place. They will then close the incision.
So, based on all that, here are the questions I asked and his answers:
Q: I am assuming I will be entabated (breathing tube inserted down my airway)?
A: Yes. That's standard for this kind of surgery.
Q: So I can expect my throat to be sore and possibly have difficulty swallowing and speaking?
A: Your throat will definitely be sore, but the degree varies from person to person. Some people have no trouble speaking right away and others find it more difficult.
Q: What about swallowing?
A: Again, it varies. Definitely soft foods for a few days, or even the first week. Take it at your own pace.
Q: Will I need and NG (nasal-gastric) tube?
A: No. There's no reason for that.
Q: Will I need to wear a collar?
A: Yes. I'll want you to wear one for about the first four weeks. The muscles in your neck are going to sore and we will want to keep your neck in a stable position.
Q: Will it be a hard collar or soft collar?
A: It will be a hard collar, but you don't have to wear it all the time. You don't have to wear it when you're sleeping or showering or if you if you're watching TV and your resting your head.
Q: Will I need physical therapy?
A: Yes, you'll need physical therapy because we're going to be stretching our your neck muscles. They're going to be sore and stiff so, we'll have you in physical therapy after about two weeks.
Q: When are will I be able to drive?
A: You can drive as soon as you are off the narcotic pain medication.
Q: Will I need to stay in the hospital over night?
A: Well, that will be partially up to you. After you are ready to come out of post-op, we'll move you to a room for a few hours. At that time I'll discuss with you whether or not you should go home. I think it's a good idea to stay overnight; we can manage your pain and watch you. But, if you feel comfortable enough you can certainly go home.
Q: How long before I can start doing some light exercise? Like riding a bicycle or Bowling or something mildly aerobic?
A: Well, we want you to be up and moving as soon as possible, so I'd say you can start doing something aerobic pretty much as soon as you're comfortable.
Q: I've read that it takes three months for the fusion to complete, is that right.
A: It's actually more like six months. You and I will be meeting every few weeks to take X-Rays and look at the progress. I would say that we should see a good beginning to the fusion at three months.
Q: I've read about something called "Adjacent Disc Degeneration" that can happen from ACDF. Is that something to be concerned about?
A: There is a lot of conjecture in the medical field about this. This is where the disc adjacent to the fusion, either above or below, deteriorates over time. At this time we believe the people who are primarily at risk for this are post menopausal women over 50, or anyone who has osteoperosis.
Q: So, what will happen if you find something unexpected once you get to the spine and vertebrae.
A: That's very unlikely. MRI's are very comprehensive and revealing. Typically we might find a calcified disc that I might have to grind out or a herniation that protrudes more than is shown on the MRI, but nothing really out of the ordinary.
These were all of the questions that I asked.
At my pre-admission, the hospital screened me for any preexisting conditions that might effect my surgery, took some blood for a clotting test and did an EKG. One other thing they did was take my blood pressure, which was again very high. I was informed by the nurse that if my systolic was over 100 they would have to postpone and reschedule my surgery. They will make that decision tomorrow. I've taken my BP this evening and I'm now well below 100 so it will probably be a go. If not I will post tomorrow with a status, other wise it will be a day or two until I post again
Loading...
Day of Surgery
My Surgery was scheduled for 7:30AM, which means that I have to be at the hospital at 6AM. Pre-Op is a breeze. For anyone who hasn't been in for General Surgery before, the will take you into a room where you will get undressed - put on the infamous paper gown that ties in the back. My experience, for pre-op was not at all unpleasant. I was introduced to the Anesthesiologist, the Surgical nurse and m neurosurgeon. Expect that they will all ask you the same questions, again and again. This is a good thing. They are making sure they hear the same information and are all on the same page.
I've only ever had a one general surgery, and I was a light weight where the anesthetic was concerned, and this was no different. The pre-op nurse gave me some phentanol via IV and I barely remember going into the OR. I can remember them putting the mask on me as saying breath deeply and I was waking up in post-op.
In Post-Op, I could speak normally immediately. Then some issues began to come out. It turns out that once they began the surgery, what they thought was moderate cervical degeneration, turned out to be very advanced degeneration. The disc at C7 was calcified and had to be drilled out. There were major bone spurs into the nerve roots and the spine. The disc at C6 was partially calcified and actually had a calcified shield across the front of the disc. Consequently my 2hour surgery actually lasted close to four.
Very little pain coming out of the anesthetic. Unfortunately, I then began to have problems with a reaction to anesthetic. I was unable urinate right away and when they helped me stand to attempt it, my heart rate shot up to over 130. My BP, high before the surgery, was now back up to 150/117. The doctor and I decided it would be a good idea for me to spend the night, rather than go home.
After moving to my room, my family came into visit and brought their dinner. I was actually able to eat small amounts of regular food with no issues. Other than the high pulse rate and the BP, the only other problem I've had is a bit a pain from the entibation. I will periodically get a severe pain in my chest, which coughing makes go away. The nurses and doctors have told me that this is normal and that I should force my self to cough a minimum of every hour. The breathing tube causes mucus to form in the bronchia that you will need to cough out. More to come later.
My Surgery was scheduled for 7:30AM, which means that I have to be at the hospital at 6AM. Pre-Op is a breeze. For anyone who hasn't been in for General Surgery before, the will take you into a room where you will get undressed - put on the infamous paper gown that ties in the back. My experience, for pre-op was not at all unpleasant. I was introduced to the Anesthesiologist, the Surgical nurse and m neurosurgeon. Expect that they will all ask you the same questions, again and again. This is a good thing. They are making sure they hear the same information and are all on the same page.
I've only ever had a one general surgery, and I was a light weight where the anesthetic was concerned, and this was no different. The pre-op nurse gave me some phentanol via IV and I barely remember going into the OR. I can remember them putting the mask on me as saying breath deeply and I was waking up in post-op.
In Post-Op, I could speak normally immediately. Then some issues began to come out. It turns out that once they began the surgery, what they thought was moderate cervical degeneration, turned out to be very advanced degeneration. The disc at C7 was calcified and had to be drilled out. There were major bone spurs into the nerve roots and the spine. The disc at C6 was partially calcified and actually had a calcified shield across the front of the disc. Consequently my 2hour surgery actually lasted close to four.
Very little pain coming out of the anesthetic. Unfortunately, I then began to have problems with a reaction to anesthetic. I was unable urinate right away and when they helped me stand to attempt it, my heart rate shot up to over 130. My BP, high before the surgery, was now back up to 150/117. The doctor and I decided it would be a good idea for me to spend the night, rather than go home.
After moving to my room, my family came into visit and brought their dinner. I was actually able to eat small amounts of regular food with no issues. Other than the high pulse rate and the BP, the only other problem I've had is a bit a pain from the entibation. I will periodically get a severe pain in my chest, which coughing makes go away. The nurses and doctors have told me that this is normal and that I should force my self to cough a minimum of every hour. The breathing tube causes mucus to form in the bronchia that you will need to cough out. More to come later.
Loading...
1 Day Post Op
The night in the hospital was completely uneventful. The pain meds and muscle relaxants helped me to sleep just fine and I was able to sleep almost flat. One thing I forgot to mention was that about eight hours after the surgery they wanted an X-Ray. I was able to walk, with some assistance, to X-Ray and back. No problems at all. The nurse keeps changing out my ice packs for the back of my neck.
Morning was fine, another round of antiboitic via IV (3rd so far) and my wife stopped by at 8AM. I was able to order scrambled egg whites, toast, and yogurt for breakfast. I had no trouble eating it or keeping it down. Multiple trips to the bathroom to urinate and my BP is back into the 150/90 range (normal for me). My doctor stopped by to visit and gave me my next appointment and instructions:
Next appointment is in five days at which time the steri-strips will come off my incision.
I can move around the house and sleep without the collar but, driving and anything where I am "out and about" I need to where the collar.
No lifting of anything more than 8-10 lbs. Still not much pain on the percocet and valium.
The night in the hospital was completely uneventful. The pain meds and muscle relaxants helped me to sleep just fine and I was able to sleep almost flat. One thing I forgot to mention was that about eight hours after the surgery they wanted an X-Ray. I was able to walk, with some assistance, to X-Ray and back. No problems at all. The nurse keeps changing out my ice packs for the back of my neck.
Morning was fine, another round of antiboitic via IV (3rd so far) and my wife stopped by at 8AM. I was able to order scrambled egg whites, toast, and yogurt for breakfast. I had no trouble eating it or keeping it down. Multiple trips to the bathroom to urinate and my BP is back into the 150/90 range (normal for me). My doctor stopped by to visit and gave me my next appointment and instructions:
Next appointment is in five days at which time the steri-strips will come off my incision.
I can move around the house and sleep without the collar but, driving and anything where I am "out and about" I need to where the collar.
No lifting of anything more than 8-10 lbs. Still not much pain on the percocet and valium.
Loading...
2 Days Post Op
This is my first full day at home. I'm taking my pain meds regularly and I'm honestly not having any trouble breathing, eating or sleeping. I swap out ice packs for the back of my neck about every 1 to 2 hours. That really seem to help. I don't really seem to have much trouble moving my neck - no movement restriction - that I've noticed yet. So, far the worst part has been the pain around the incision and the pain that I have to cough away from being intabated. But even that is going away. I'm dozing a lot, which is to be expected I suppose because of the trauma to my body. Neck mucsle are still quite sore.
I was able to do a bit over a 1/4 mile on the treadmill in about 11 minutes today. I was advised by my doctor to get some activity everyday. I took a nap after, but I did it.
All, in all, this has not been as hard as I anticipated. It's still early in the recovery process, but I plan to just keep taking it easy and do a little bit more every day. More to come.
This is my first full day at home. I'm taking my pain meds regularly and I'm honestly not having any trouble breathing, eating or sleeping. I swap out ice packs for the back of my neck about every 1 to 2 hours. That really seem to help. I don't really seem to have much trouble moving my neck - no movement restriction - that I've noticed yet. So, far the worst part has been the pain around the incision and the pain that I have to cough away from being intabated. But even that is going away. I'm dozing a lot, which is to be expected I suppose because of the trauma to my body. Neck mucsle are still quite sore.
I was able to do a bit over a 1/4 mile on the treadmill in about 11 minutes today. I was advised by my doctor to get some activity everyday. I took a nap after, but I did it.
All, in all, this has not been as hard as I anticipated. It's still early in the recovery process, but I plan to just keep taking it easy and do a little bit more every day. More to come.
Loading...
3 Days Post Op
Sleeping is actually much easier than I expected. I have pillows to support my head and I'm able to sleep on my side. I generally feel the best when I wake up in the morning. I'm trying to go as long as possible without a pain pill and want to try to get to just Tylenol. I'm not pushing it, I'll play it by ear. I have started to have some twinges down both my right and left arm. Based on the the amount of degeneration they discovered, I expect that this should be normal. After the intense pain I was in before, if I have to live with a few twinges I will be very happy.
During the day, I spend the majority of my time in a recliner with my neck supported and an Ice pack on my neck and shoulders. The Ice really does help.
Tomorrow, I'll be adding a bit more exercise - a second short walk.
Once again, with proper pain management, the pain is controllable. Oh, and I already have significantly decreased numbness in my right arm. Prior to surgery, I had severe numbness on the left side from mid forearm to the tip of my thumb. Immediately after surgery, I noticed a marked decrease in the numbness. I also have not had a reoccurrance of the shooting pain in my forearm and thumb and fingers.
My arm and hand feel stronger, but I don't know for sure if the strength is better. I'll have to wait a few weeks to actually test my lifting and grip strength, but it feels stronger.
Sleeping is actually much easier than I expected. I have pillows to support my head and I'm able to sleep on my side. I generally feel the best when I wake up in the morning. I'm trying to go as long as possible without a pain pill and want to try to get to just Tylenol. I'm not pushing it, I'll play it by ear. I have started to have some twinges down both my right and left arm. Based on the the amount of degeneration they discovered, I expect that this should be normal. After the intense pain I was in before, if I have to live with a few twinges I will be very happy.
During the day, I spend the majority of my time in a recliner with my neck supported and an Ice pack on my neck and shoulders. The Ice really does help.
Tomorrow, I'll be adding a bit more exercise - a second short walk.
Once again, with proper pain management, the pain is controllable. Oh, and I already have significantly decreased numbness in my right arm. Prior to surgery, I had severe numbness on the left side from mid forearm to the tip of my thumb. Immediately after surgery, I noticed a marked decrease in the numbness. I also have not had a reoccurrance of the shooting pain in my forearm and thumb and fingers.
My arm and hand feel stronger, but I don't know for sure if the strength is better. I'll have to wait a few weeks to actually test my lifting and grip strength, but it feels stronger.
Loading...
4 Days Post Op
While it's still early in the day, I thought I'd start my post. Excellent nights sleep last night. Only very mild discomfort. I woke feeling better than I have since long before the surgery. Still taking it easy and not trying to push it too hard. I plan on taking this entire week off of work and then, since I can, work from home part time next week.
After being awake for about an hour - and having my coffee - I was able to do 1/2 mile on the tread mill at a fairly slow rate, 2mph. It took me 15 minutes but felt good to get some movement. I wore my collar while on the treadmill, just in case. I still don't trust my stability completely so I kept my hands on the rails the entire time.
After the tread mill, I had breakfast of oatmeal and high fiber yogurt. Then I took a muscle relaxant. I took a shower and got dressed and then also took a pain pill, the first one today.
Still not much pain, but I am experiencing a few "twinges" down either arm and in both shoulders. Since I'm currently fairly pain free, I'm hoping I stay that way. However, I am aware that I had symptoms on an off for years and I probably have some permanent nerve damage. How severe the damage is, only tiime will tell. Right now I'm VERY happy with the results. More to come.
While it's still early in the day, I thought I'd start my post. Excellent nights sleep last night. Only very mild discomfort. I woke feeling better than I have since long before the surgery. Still taking it easy and not trying to push it too hard. I plan on taking this entire week off of work and then, since I can, work from home part time next week.
After being awake for about an hour - and having my coffee - I was able to do 1/2 mile on the tread mill at a fairly slow rate, 2mph. It took me 15 minutes but felt good to get some movement. I wore my collar while on the treadmill, just in case. I still don't trust my stability completely so I kept my hands on the rails the entire time.
After the tread mill, I had breakfast of oatmeal and high fiber yogurt. Then I took a muscle relaxant. I took a shower and got dressed and then also took a pain pill, the first one today.
Still not much pain, but I am experiencing a few "twinges" down either arm and in both shoulders. Since I'm currently fairly pain free, I'm hoping I stay that way. However, I am aware that I had symptoms on an off for years and I probably have some permanent nerve damage. How severe the damage is, only tiime will tell. Right now I'm VERY happy with the results. More to come.
Loading...
5 Days Post-Op
Recovery is progressing. I'm still not in a lot of pain. I am, however, beginning to experience some of the old pain in my left arm. It's nothing like what I experienced before surgery and it is more than bearable.
I only had to use two muscle relaxents and three pain pills, yesterday. I also was able to do .5 miles on the treadmill, without much problem at all. I ended up taking two naps yesterday.
I've managed to do .65 miles today in 15 minutes and I started adding in some VERY light weights. I have to 5lb hand weights so I did 50 curls on each arm. That did get my shoulders aching a bit. Prompting me to take a muscle relaxant.
Tomorrow is my first post-op doctors appointment. More to come them.
Recovery is progressing. I'm still not in a lot of pain. I am, however, beginning to experience some of the old pain in my left arm. It's nothing like what I experienced before surgery and it is more than bearable.
I only had to use two muscle relaxents and three pain pills, yesterday. I also was able to do .5 miles on the treadmill, without much problem at all. I ended up taking two naps yesterday.
I've managed to do .65 miles today in 15 minutes and I started adding in some VERY light weights. I have to 5lb hand weights so I did 50 curls on each arm. That did get my shoulders aching a bit. Prompting me to take a muscle relaxant.
Tomorrow is my first post-op doctors appointment. More to come them.
Loading...