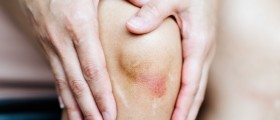
Hi there! I am 17, and my little sister who is 6 years old has developed a disease called dermatamyositis. Now, I heard that this disease is rear, and I saw a rash on her body but I still haven’t figured out what it is. IS there anybody who can explain this to me. IS there more than a rash in dermatamyositis.
Loading...
Yes, you heard well, this is very uncommon disease and it affects more women than men, in their 40s or children between 5 and 15. Dermatamyositis is an inflammatory muscle diseases marked by muscle weakness and a distinctive skin rash. The skin rash usually occurs at the same time as muscle weakness, but may precede muscle weakness by a few weeks. Weakness in muscles, such as your hips and shoulders, can lead to difficulty in getting out of chairs, climbing stairs, brushing your hair or working with your arms over your head. Weakness in your neck muscles can make it hard to hold your head up. There are treatments that can improve skins and muscle’s strength and function but there is no cure. Methods of therapy are: corticosteroids to suppress your immune system, limiting the production of antibodies and reducing skin and muscle inflammation; immunosuppressants are used if a body doesn't respond adequately to corticosteroids; antimalarial medications for a persistent rash; physical therapy to maintain and improve your strength and flexibility; over the counter pain relievers.
Loading...
Hi Big Sister;
My daughter Elizabeth was diagnozed with Dermatamyositis when she was 5 years old. She is now 20 and apart from a few scars and some atrophied muscles she looks and feels quite well. Lulu as we call her had a severe case and it seemed to keep on changing. We left the pediatrician with a 2page phoocopy of what we could expect and a prescription for steroids. Until she was about 12, she had a pretty rough time. She had regular physiotherapy visits to help prevent her muscles from contracting. At one stage, she spent about 6-8 months in a wheelchair. Fortunately it was only temporary and she has also used crutches. She has also had a variety of drugs both oral and intravenous. It really was a rough time for all of us. Swimming was beneficial. I would say that the rash is the least of problems. The weakness in the legs and arms was probably the hardest thing to deal with. Our 2nd pediatrician is Dr Tom Hurley at Suncoast Pediatrics at Kawana on the Sunshine Coast. Australia. He really helped us through a lot. Your sister may be a bit down in the dumps more than her friends. She needs lots of support and normal family life to support her through this. We were told it usually goes away around puberty and it did for Lulu. I wish your sister and your family all the best. Carol
My daughter Elizabeth was diagnozed with Dermatamyositis when she was 5 years old. She is now 20 and apart from a few scars and some atrophied muscles she looks and feels quite well. Lulu as we call her had a severe case and it seemed to keep on changing. We left the pediatrician with a 2page phoocopy of what we could expect and a prescription for steroids. Until she was about 12, she had a pretty rough time. She had regular physiotherapy visits to help prevent her muscles from contracting. At one stage, she spent about 6-8 months in a wheelchair. Fortunately it was only temporary and she has also used crutches. She has also had a variety of drugs both oral and intravenous. It really was a rough time for all of us. Swimming was beneficial. I would say that the rash is the least of problems. The weakness in the legs and arms was probably the hardest thing to deal with. Our 2nd pediatrician is Dr Tom Hurley at Suncoast Pediatrics at Kawana on the Sunshine Coast. Australia. He really helped us through a lot. Your sister may be a bit down in the dumps more than her friends. She needs lots of support and normal family life to support her through this. We were told it usually goes away around puberty and it did for Lulu. I wish your sister and your family all the best. Carol
Loading...
caroljc,
I have adult 'dm', which is like living in a different world. A website that has provided a lot of insights into this disease, a support network and some experts in the field is 'The Myosytis Association'. Google 'dermatamyositis' and they will be on the first page. They have a special section for juvenile dermatamyositis which may be very helpful.
Good luck, XD XD XD
I have adult 'dm', which is like living in a different world. A website that has provided a lot of insights into this disease, a support network and some experts in the field is 'The Myosytis Association'. Google 'dermatamyositis' and they will be on the first page. They have a special section for juvenile dermatamyositis which may be very helpful.
Good luck, XD XD XD
Loading...
Hello Big Sister
Iam a 23 year old From Canada and I was diagnosed with dermatomyositis 3 years ago. Now I am what they call a " A typical patient" I went from working 8 to 10 hour days to not being able to walk, talk or even eat in less then 3 months. My first signs were major pain in my major muscles starting with my thighs and lower back then it moved into my shoulders then eventually i couldn't walk proper. By the time I got to a doctor that figured out what was wrong with me I couldn't talk. When the doctor was looking for symtoms he was checking the area around my finger nails and around my eyes and on my eyelids for any signs of a rash. He said that a rash on the body is very unlikly. After all was figured out I was on Major doses of steriods for a year and a half with a pickline and pump attached and as of right now I have to take a anti rejection drug to help my body with the steriods. IF anyone has any questions on anything i went through please ask you can reach me at
and my name is Robbie
***this post is edited by moderator *** *** private e-mails not allowed **
Please read our Terms of Use
Iam a 23 year old From Canada and I was diagnosed with dermatomyositis 3 years ago. Now I am what they call a " A typical patient" I went from working 8 to 10 hour days to not being able to walk, talk or even eat in less then 3 months. My first signs were major pain in my major muscles starting with my thighs and lower back then it moved into my shoulders then eventually i couldn't walk proper. By the time I got to a doctor that figured out what was wrong with me I couldn't talk. When the doctor was looking for symtoms he was checking the area around my finger nails and around my eyes and on my eyelids for any signs of a rash. He said that a rash on the body is very unlikly. After all was figured out I was on Major doses of steriods for a year and a half with a pickline and pump attached and as of right now I have to take a anti rejection drug to help my body with the steriods. IF anyone has any questions on anything i went through please ask you can reach me at
and my name is Robbie
***this post is edited by moderator *** *** private e-mails not allowed **
Please read our Terms of Use
Loading...
A few things you may not know that I have learned from experience, as I am 13 and have Dermatomyositis.
Dermatomyositis is abbreiveated "DMS". I am SO glad I learned that...it makes life a lot easier sometimes! Juvenile DMS is abbreviated JDMS.
JDMS is an autoimmune disease...the immune system attacks itself.
"The immune system is a group of cells which normally protects the body from infections. In autoimmune diseases, these cells are signaled or triggered to "turn on" their infection-fighting process, but then can't turn it off. The process then ends up damaging the body rather than protecting it. One way the immune system cells fight infection is by a process called inflammation (in-flah-MAY-shun). But when the cells can't "turn off" the inflammation process, tissues are damaged" -
The two main doctors your sis will most likely be seeing are neurologists & rhuematologists. DMS can affect the joints....seriously, it can! that is my main problem, but if you look on the net, you don't find anything about it, except what I've posted! It is even considered a form of arthritis by the Arthritis Foundation. It is also considered a form of muscular dystrophy by the Muscular Dystrophy Association. It affects the muscles, skin & joints. Depending on what seems to be her biggest problem, the amount of time your sis will spend there will vary. My RA NEVER told me to see a neuro doc! He didn't tell me anything! DON'T LET THAT HAPPEN TO YOU! I learned the hard way...a 10 year old fighting for her life, learning from what little she could juice out of others, posing as an adult on online forums!
MOST CASSES ARE IN NO WAY LIFE THREATENING!!! Mine was the "rare" "exception". Story of my life. But don't freak out...what you will see on the net with either underrate it or overrate it....EVER CASE IS DIFFERENT.
Oy...it's hard to think through the flashbacks...
Find someone good to draw her blood...ask around...I reccomend you NOT go to the university...usually it's students drawing the blood there...I've had some nasty experiences that way. Usually there is a miracle trouble-shooter out there...you just need to find him/her. For 2 years I was getting blood AT LEAST twice a week...and going to the U, well, it made it feel like twice a day...and I spent all my time dreading my veins being blown, (including on my hands), and being bruised badly all over. So, yeah...don't let that happen!
"Juvenile dermatomyositis (der-MA-toe-My-o-SY-tis)(JDMS) is a disease that causes a skin rash and weak muscles in children. JDMS is different from dermatomyositis in adults, and from polymyositis (PAH-lee-My-o-SY-tis), a disease that usually affects adults.
The skin rash and weak muscles of JDMS are caused by inflammation in the blood vessels that lie under the skin and in the muscles. This is called vasculitis. Since blood vessels run throughout the body, JDMS can also affect other areas such as the digestive tract. Usually, the worst symptoms are in the skin and muscles.
JDMS is often called an autoimmune disease. The immune system is a group of cells which normally protects the body from infections. In autoimmune diseases, these cells are signaled or triggered to "turn on" their infection-fighting process, but then can't turn it off. The process then ends up damaging the body rather than protecting it.
One way the immune system cells fight infection is by a process called inflammation (in-flah-MAY-shun). But when the cells can't "turn off" the inflammation process, tissues are damaged. In JDMS, blood vessels in the skin and muscles are inflamed. An inflamed muscle will feel weak or sore, while inflamed skin will have a rash.
NOTE: Juvenile dermatomyositis (JDMS) affects 3,000 to 5,000 children in the United States. While certain signs and symptoms are common in most children with JDMS, the disease affects different children in different ways."
"The symptoms of juvenile dermatomyositis often appear gradually. At times, there may be a more acute, or intense, onset of symptoms. The following are the most common symptoms of juvenile dermatomyositis. However, each child may experience symptoms differently. Symptoms may include:
* fever
* rash around the eyelids and/or knuckles and finger joints; a rash may also occur on the elbows, knees, and ankles
* muscle weakness
* fatigue
* malaise
* muscle pain and tenderness
* irritability
* weight loss (due to difficulty swallowing)
* joint pain and inflammation
* calcium deposits under the skin (calcinosis)
* mouth ulcers
Symptoms of juvenile dermatomyositis may resemble other medical conditions or problems. "
"Some children with this disease may become sick over a short period of time and others much more gradually over many months and even years. A young child will often complain of general symptoms of feeling unwell and is likely to be irritable, get tired easily and sometimes may refuse to walk. An older child will complain of pain in the arms and legs and weakness. This weakness may be limited to getting out of bed, getting up from sitting on the floor or trying to squat. If the disease is worse, a child may also have difficulty walking or sometimes breathing.
The other main symptom is a rash. This is often noticed over the eyelids, cheeks, upper chest, knuckles of the hands, elbows and knees. The rash is often scaly and reddened in children with fair skin and scaly and darkened in children with darker skin. Puffiness or swelling may occur around the eyes and face.
More rarely, a child's voice may change to sound more nasal in quality. A child may also have difficulty swallowing or complain of pain in the chest or stomach.
For most children it takes some time for these symptoms to develop and so it is some time before a diagnosis can be reached. This should not affect your child's response to treatment. As the disease affects each child differently, not all children will have all of the symptoms above or suffer them to the same degree.
How is it diagnosed?
When a child with these problems is seen, several tests will be carried out to confirm a diagnosis and also to understand the severity of the disease. The results will provide vital information for your child's doctor to plan the treatment. These tests include:
*
Blood tests to measure the level of inflammation and to calculate how much muscle damage has occurred;
*
An MRI scan or ultrasound (a special form of x-ray) may be carried out to look at how inflamed the muscles appear. A scan is generally taken of your child's thigh;
*
For some children, a muscle biopsy may be needed. This involves a small operation whereby a tiny piece of muscle is removed for examination under the microscope.
What does treatment involve?
If this condition is not treated, the muscles may become severely weakened over time and may be permanently damaged. The skin and gut may become inflamed and, rarely, even ulcerated if treatment is delayed. There are several forms of treatment which all work together to minimise any pain and damage.
Medication:
The most important and most effective treatment for this condition is through medication - in the right dosage. This will reduce the inflammation and help prevent further muscle damage. Generally, treatment starts with a course of steroids either by drip (into the vein) or by mouth, and improvements are usually seen within a few days. Usually other medicines such as methotrexate or cyclosporin are added to help reduce the inflammation. These are much slower acting but have far fewer side-effects than steroids in the long-term. For most children, these improvements mean increased muscle strength, endurance and general well being. Some children may develop inflammation in their joints (arthritis) and need anti-inflammatory treatment for this. Most children will also be given calcium and vitamin D supplements while they are on steroids to help keep their bones strong and to prevent osteoporosis.
The treatment usually needs to continue for at least two years. During this time children are slowly tapered off their steroids and any other medications which are no longer necessary. Sometimes if there is a flare up of the disease, medication will need to be increased for a period of time in order to control the inflammation. Flares up in disease are sometimes associated with a viral infection or period of illness from another cause.
In the long term, most children's conditions improve greatly with this treatment. Many will eventually make a full recovery although this may take several years. For some children who suffer a more severe form of the condition, they will need to be treated for many years and they may be left with some permanent disabilities.
Will the drugs cause side effects?
Most medications used for this condition have associated side effects. Through careful monitoring and regular visits to your child's specialist clinic, many of these side effects can be minimised. When steroids are used, the key effects noticed are weight gain and change of body shape. These will disappear as your child's treatment is reduced or finished. Other side effects may include raised blood pressure or thinning of the bones (osteoporosis). Side effects to the liver and kidneys can also occur with some drugs. Checking your child's blood pressure, urine and blood regularly will help monitor the side effects and will help your child's doctor use the lowest possible dose of drugs while keeping the disease under control.
Physiotherapy:
Dermatomyositis can cause the muscles to become weakened and develop scars (muscle fibrosis) which could lead to your child having bent, stiff joints which will be difficult to move. The joints of the knees, ankles, elbows and wrists are most often affected. Physiotherapy can help.
At the beginning of treatment, your child's physiotherapist will teach you and your child very gentle stretching exercises to improve and maintain the range of movement of the joints. Sometimes your child may need splints to strengthen affected joints.
At a later stage, your child's physiotherapist will teach you and your child an exercise programme that will help your child's muscles recover and strengthen. You will be asked to encourage your child to do these exercises when you return home with help from a local physiotherapist.
Occupational Therapy:
If your child has difficulty moving his or her joints, particularly the arms and hands, occupational therapy may be useful. This will help your child find ways of carrying out daily tasks without causing any more pain or damage.
What is the outlook?
Many children eventually completely recover from this disease, although for some it may take a long time for this to happen. The aim is always to keep the disease under control in order to prevent long-term problems associated with muscle weakness and stiffened joints.
Some children do get a complication where chalky material (calcium) appears under the skin. This is called calcinosis. This usually happens later in the disease, sometimes after the muscles have become better. There is no known effective treatment for this though diagnosing and treating the dermatomyositis at an early stage may help prevent it. Surgery to remove the lumps is rarely required.
In general with modern treatment the outlook for this disease is good. Most children grow up to be healthy adults who are able to study, work and have families. "
Children and adults with dermatomyositis may develop calcium deposits, which appear as hard bumps under the skin or in the muscle (called calcinosis). Calcinosis most often occurs 1-3 years after the disease begins. These deposits are seen more often in children with dermatomyositis than in adults.
I haven't had that yet.... but that's just me...and I'm just reaching 3 years post dx (diagnoses...another term you may come to know well)
most people do take steroids first. Me, it didn't work, and I take methotrexate. Methotrexate is a form of chemotherapy, which if you take will most likely be in small doses you will be able to take through pills, and will have very minimal side effects. Me, not so lucky, I get it injected weekly...first day tired, second day nauseated, third day both but cut in half, fourth, going "Wow! I'm starting to feel better!" Fifth, feel fully recovered, sixth, living my life, seventh, REPEAT. But, most likely that will never happen, and even if it does, you learn how to deal with it...it's just a part of life, and you learn to plan things around it, and pull through.
" Immunosuppressant drugs, such as azathioprine and methotrexate, may reduce inflammation in people who do not respond well to prednisone. Periodic treatment using intravenous immunoglobulin can also improve recovery. Other immunosuppressive agents used to treat the inflammation associated with dermatomyositis include cyclosporine A, cyclophosphamide, and tacrolimus. Physical therapy is usually recommended to prevent muscle atrophy and to regain muscle strength and range of motion. Many individuals with dermatomyositis may need a topical ointment, such as topical corticosteroids, for their skin disorder. They should wear a high-protection sunscreen and protective clothing. Surgery may be required to remove calcium deposits that cause nerve pain and recurrent infections. " -(same link)
My doctor never told me there were options, until he got to the point where he was saying "Don't worry, things will be okay" with an extremely obvious "I hope I'm not lying" look, before he told me about an experimental treatment, rather than one of the already available proven treatments such as IVIG.
Here's some links & other stuff from the net
" * Dermatomyositis is an inflammatory muscle disease, like polymyositis; however, it has a somewhat severe onset and affects both children and adults. Clinical features of dermatomyositis include all those of polymyositis, plus a variety of skin manifestations, such as:
* Rashes: Dermatomyositis is characterized by a rash accompanying or, more often, preceding muscle weakness by a year or more. A patchy, red-to-purple rash may be found on the back of the shoulders and neck (shawl sign), front of the neck and upper chest (V-sign), face and forehead.
* Gottron’s papules: Lacy, pink or violet areas (raised or scaly) found symmetrically on the knuckles, elbows, knees and ankles are characteristic or diagnostic for dermatomyositis.
* Eyelids: purplish discoloration of the eyelids with swelling around the eyes
* Dystrophic cuticles: changes around the bed of the nails especially in the hands
* Calcium deposits: Calcification is hardening of skin and muscles as a result of calcium salt deposits. Calcification doesn’t often occur in adults, but children with dermatomyositis may develop calcium deposits years after the disease starts. Deposits usually occur in the shoulder, pelvis, hip, calf and thigh and may severely limit motion." -
"Although dermatomyositis may occur at any age, it mostly affects adults in their late 40s to early 60s or children between 5 and 15 years of age. Women have dermatomyositis more often than men do. Dermatomyositis in children is distinct from the adult form. The disease usually develops over weeks or months.
Periods of remission, during which signs and symptoms of dermatomyositis improve spontaneously, may occur. (this happened to me). Treatment can improve your skin and your muscle strength and function."
"Typically, your immune system works to protect your healthy cells from attacks by foreign substances, such as bacteria and viruses. If you have dermatomyositis, an unknown cause seems to trigger your immune system to begin producing autoimmune antibodies (also called autoantibodies) that attack your body's own tissues. Small blood vessels in muscular tissue appear to be particularly affected. Destruction of these blood vessels eventually leads to degeneration of muscle fibers. Many people with dermatomyositis show a detectable level of autoantibodies in their blood. It's unclear whether these autoantibodies are involved in causing dermatomyositis." (same link as above)
"21 June 1993
Summary The frequency and features of joint involvement were evaluated in 29 patients with polymyositis/dermatomyositis (PM/DM); eight of them (27.5%) presented arthritis. Mean age was 30 years, and mean disease duration was 5.3 years. Oligoarthritis was observed in 5 cases, while 3 presented polyarthritis; in most cases arthritis was concurrent with the musculocutaneous picture. On comparing the 8 arthritis patients with the remaining 21, no significant clinical or serological differences were found. However, males predominated in the arthritis group, 75% vs 19% (p<0.05). Arthritis responded favourably to underlying disease treatment and articular sequelae were not observed."
~SUPPORT GROUPS~
If you EVER need more information or someone to talk to, PLEASE feel free to email me...I have more information than the entire web probably has put together.. Its been 3 years since my muscle biopsy and dx now...it's been a long and scary road, and I'm still fighting. I'll help you on your road in any way I can...just let me know =)
Alex, 13 years old, JDMS warrior for 3+ years & founder of Awareness Angels as well as many other charities/etc
***edited by moderator*** web addresses not allowed *** private e-mails not allowed ***
Please read our Terms of Use
Dermatomyositis is abbreiveated "DMS". I am SO glad I learned that...it makes life a lot easier sometimes! Juvenile DMS is abbreviated JDMS.
JDMS is an autoimmune disease...the immune system attacks itself.
"The immune system is a group of cells which normally protects the body from infections. In autoimmune diseases, these cells are signaled or triggered to "turn on" their infection-fighting process, but then can't turn it off. The process then ends up damaging the body rather than protecting it. One way the immune system cells fight infection is by a process called inflammation (in-flah-MAY-shun). But when the cells can't "turn off" the inflammation process, tissues are damaged" -
The two main doctors your sis will most likely be seeing are neurologists & rhuematologists. DMS can affect the joints....seriously, it can! that is my main problem, but if you look on the net, you don't find anything about it, except what I've posted! It is even considered a form of arthritis by the Arthritis Foundation. It is also considered a form of muscular dystrophy by the Muscular Dystrophy Association. It affects the muscles, skin & joints. Depending on what seems to be her biggest problem, the amount of time your sis will spend there will vary. My RA NEVER told me to see a neuro doc! He didn't tell me anything! DON'T LET THAT HAPPEN TO YOU! I learned the hard way...a 10 year old fighting for her life, learning from what little she could juice out of others, posing as an adult on online forums!
MOST CASSES ARE IN NO WAY LIFE THREATENING!!! Mine was the "rare" "exception". Story of my life. But don't freak out...what you will see on the net with either underrate it or overrate it....EVER CASE IS DIFFERENT.
Oy...it's hard to think through the flashbacks...
Find someone good to draw her blood...ask around...I reccomend you NOT go to the university...usually it's students drawing the blood there...I've had some nasty experiences that way. Usually there is a miracle trouble-shooter out there...you just need to find him/her. For 2 years I was getting blood AT LEAST twice a week...and going to the U, well, it made it feel like twice a day...and I spent all my time dreading my veins being blown, (including on my hands), and being bruised badly all over. So, yeah...don't let that happen!
"Juvenile dermatomyositis (der-MA-toe-My-o-SY-tis)(JDMS) is a disease that causes a skin rash and weak muscles in children. JDMS is different from dermatomyositis in adults, and from polymyositis (PAH-lee-My-o-SY-tis), a disease that usually affects adults.
The skin rash and weak muscles of JDMS are caused by inflammation in the blood vessels that lie under the skin and in the muscles. This is called vasculitis. Since blood vessels run throughout the body, JDMS can also affect other areas such as the digestive tract. Usually, the worst symptoms are in the skin and muscles.
JDMS is often called an autoimmune disease. The immune system is a group of cells which normally protects the body from infections. In autoimmune diseases, these cells are signaled or triggered to "turn on" their infection-fighting process, but then can't turn it off. The process then ends up damaging the body rather than protecting it.
One way the immune system cells fight infection is by a process called inflammation (in-flah-MAY-shun). But when the cells can't "turn off" the inflammation process, tissues are damaged. In JDMS, blood vessels in the skin and muscles are inflamed. An inflamed muscle will feel weak or sore, while inflamed skin will have a rash.
NOTE: Juvenile dermatomyositis (JDMS) affects 3,000 to 5,000 children in the United States. While certain signs and symptoms are common in most children with JDMS, the disease affects different children in different ways."
"The symptoms of juvenile dermatomyositis often appear gradually. At times, there may be a more acute, or intense, onset of symptoms. The following are the most common symptoms of juvenile dermatomyositis. However, each child may experience symptoms differently. Symptoms may include:
* fever
* rash around the eyelids and/or knuckles and finger joints; a rash may also occur on the elbows, knees, and ankles
* muscle weakness
* fatigue
* malaise
* muscle pain and tenderness
* irritability
* weight loss (due to difficulty swallowing)
* joint pain and inflammation
* calcium deposits under the skin (calcinosis)
* mouth ulcers
Symptoms of juvenile dermatomyositis may resemble other medical conditions or problems. "
"Some children with this disease may become sick over a short period of time and others much more gradually over many months and even years. A young child will often complain of general symptoms of feeling unwell and is likely to be irritable, get tired easily and sometimes may refuse to walk. An older child will complain of pain in the arms and legs and weakness. This weakness may be limited to getting out of bed, getting up from sitting on the floor or trying to squat. If the disease is worse, a child may also have difficulty walking or sometimes breathing.
The other main symptom is a rash. This is often noticed over the eyelids, cheeks, upper chest, knuckles of the hands, elbows and knees. The rash is often scaly and reddened in children with fair skin and scaly and darkened in children with darker skin. Puffiness or swelling may occur around the eyes and face.
More rarely, a child's voice may change to sound more nasal in quality. A child may also have difficulty swallowing or complain of pain in the chest or stomach.
For most children it takes some time for these symptoms to develop and so it is some time before a diagnosis can be reached. This should not affect your child's response to treatment. As the disease affects each child differently, not all children will have all of the symptoms above or suffer them to the same degree.
How is it diagnosed?
When a child with these problems is seen, several tests will be carried out to confirm a diagnosis and also to understand the severity of the disease. The results will provide vital information for your child's doctor to plan the treatment. These tests include:
*
Blood tests to measure the level of inflammation and to calculate how much muscle damage has occurred;
*
An MRI scan or ultrasound (a special form of x-ray) may be carried out to look at how inflamed the muscles appear. A scan is generally taken of your child's thigh;
*
For some children, a muscle biopsy may be needed. This involves a small operation whereby a tiny piece of muscle is removed for examination under the microscope.
What does treatment involve?
If this condition is not treated, the muscles may become severely weakened over time and may be permanently damaged. The skin and gut may become inflamed and, rarely, even ulcerated if treatment is delayed. There are several forms of treatment which all work together to minimise any pain and damage.
Medication:
The most important and most effective treatment for this condition is through medication - in the right dosage. This will reduce the inflammation and help prevent further muscle damage. Generally, treatment starts with a course of steroids either by drip (into the vein) or by mouth, and improvements are usually seen within a few days. Usually other medicines such as methotrexate or cyclosporin are added to help reduce the inflammation. These are much slower acting but have far fewer side-effects than steroids in the long-term. For most children, these improvements mean increased muscle strength, endurance and general well being. Some children may develop inflammation in their joints (arthritis) and need anti-inflammatory treatment for this. Most children will also be given calcium and vitamin D supplements while they are on steroids to help keep their bones strong and to prevent osteoporosis.
The treatment usually needs to continue for at least two years. During this time children are slowly tapered off their steroids and any other medications which are no longer necessary. Sometimes if there is a flare up of the disease, medication will need to be increased for a period of time in order to control the inflammation. Flares up in disease are sometimes associated with a viral infection or period of illness from another cause.
In the long term, most children's conditions improve greatly with this treatment. Many will eventually make a full recovery although this may take several years. For some children who suffer a more severe form of the condition, they will need to be treated for many years and they may be left with some permanent disabilities.
Will the drugs cause side effects?
Most medications used for this condition have associated side effects. Through careful monitoring and regular visits to your child's specialist clinic, many of these side effects can be minimised. When steroids are used, the key effects noticed are weight gain and change of body shape. These will disappear as your child's treatment is reduced or finished. Other side effects may include raised blood pressure or thinning of the bones (osteoporosis). Side effects to the liver and kidneys can also occur with some drugs. Checking your child's blood pressure, urine and blood regularly will help monitor the side effects and will help your child's doctor use the lowest possible dose of drugs while keeping the disease under control.
Physiotherapy:
Dermatomyositis can cause the muscles to become weakened and develop scars (muscle fibrosis) which could lead to your child having bent, stiff joints which will be difficult to move. The joints of the knees, ankles, elbows and wrists are most often affected. Physiotherapy can help.
At the beginning of treatment, your child's physiotherapist will teach you and your child very gentle stretching exercises to improve and maintain the range of movement of the joints. Sometimes your child may need splints to strengthen affected joints.
At a later stage, your child's physiotherapist will teach you and your child an exercise programme that will help your child's muscles recover and strengthen. You will be asked to encourage your child to do these exercises when you return home with help from a local physiotherapist.
Occupational Therapy:
If your child has difficulty moving his or her joints, particularly the arms and hands, occupational therapy may be useful. This will help your child find ways of carrying out daily tasks without causing any more pain or damage.
What is the outlook?
Many children eventually completely recover from this disease, although for some it may take a long time for this to happen. The aim is always to keep the disease under control in order to prevent long-term problems associated with muscle weakness and stiffened joints.
Some children do get a complication where chalky material (calcium) appears under the skin. This is called calcinosis. This usually happens later in the disease, sometimes after the muscles have become better. There is no known effective treatment for this though diagnosing and treating the dermatomyositis at an early stage may help prevent it. Surgery to remove the lumps is rarely required.
In general with modern treatment the outlook for this disease is good. Most children grow up to be healthy adults who are able to study, work and have families. "
Children and adults with dermatomyositis may develop calcium deposits, which appear as hard bumps under the skin or in the muscle (called calcinosis). Calcinosis most often occurs 1-3 years after the disease begins. These deposits are seen more often in children with dermatomyositis than in adults.
I haven't had that yet.... but that's just me...and I'm just reaching 3 years post dx (diagnoses...another term you may come to know well)
most people do take steroids first. Me, it didn't work, and I take methotrexate. Methotrexate is a form of chemotherapy, which if you take will most likely be in small doses you will be able to take through pills, and will have very minimal side effects. Me, not so lucky, I get it injected weekly...first day tired, second day nauseated, third day both but cut in half, fourth, going "Wow! I'm starting to feel better!" Fifth, feel fully recovered, sixth, living my life, seventh, REPEAT. But, most likely that will never happen, and even if it does, you learn how to deal with it...it's just a part of life, and you learn to plan things around it, and pull through.
" Immunosuppressant drugs, such as azathioprine and methotrexate, may reduce inflammation in people who do not respond well to prednisone. Periodic treatment using intravenous immunoglobulin can also improve recovery. Other immunosuppressive agents used to treat the inflammation associated with dermatomyositis include cyclosporine A, cyclophosphamide, and tacrolimus. Physical therapy is usually recommended to prevent muscle atrophy and to regain muscle strength and range of motion. Many individuals with dermatomyositis may need a topical ointment, such as topical corticosteroids, for their skin disorder. They should wear a high-protection sunscreen and protective clothing. Surgery may be required to remove calcium deposits that cause nerve pain and recurrent infections. " -(same link)
My doctor never told me there were options, until he got to the point where he was saying "Don't worry, things will be okay" with an extremely obvious "I hope I'm not lying" look, before he told me about an experimental treatment, rather than one of the already available proven treatments such as IVIG.
Here's some links & other stuff from the net
" * Dermatomyositis is an inflammatory muscle disease, like polymyositis; however, it has a somewhat severe onset and affects both children and adults. Clinical features of dermatomyositis include all those of polymyositis, plus a variety of skin manifestations, such as:
* Rashes: Dermatomyositis is characterized by a rash accompanying or, more often, preceding muscle weakness by a year or more. A patchy, red-to-purple rash may be found on the back of the shoulders and neck (shawl sign), front of the neck and upper chest (V-sign), face and forehead.
* Gottron’s papules: Lacy, pink or violet areas (raised or scaly) found symmetrically on the knuckles, elbows, knees and ankles are characteristic or diagnostic for dermatomyositis.
* Eyelids: purplish discoloration of the eyelids with swelling around the eyes
* Dystrophic cuticles: changes around the bed of the nails especially in the hands
* Calcium deposits: Calcification is hardening of skin and muscles as a result of calcium salt deposits. Calcification doesn’t often occur in adults, but children with dermatomyositis may develop calcium deposits years after the disease starts. Deposits usually occur in the shoulder, pelvis, hip, calf and thigh and may severely limit motion." -
"Although dermatomyositis may occur at any age, it mostly affects adults in their late 40s to early 60s or children between 5 and 15 years of age. Women have dermatomyositis more often than men do. Dermatomyositis in children is distinct from the adult form. The disease usually develops over weeks or months.
Periods of remission, during which signs and symptoms of dermatomyositis improve spontaneously, may occur. (this happened to me). Treatment can improve your skin and your muscle strength and function."
"Typically, your immune system works to protect your healthy cells from attacks by foreign substances, such as bacteria and viruses. If you have dermatomyositis, an unknown cause seems to trigger your immune system to begin producing autoimmune antibodies (also called autoantibodies) that attack your body's own tissues. Small blood vessels in muscular tissue appear to be particularly affected. Destruction of these blood vessels eventually leads to degeneration of muscle fibers. Many people with dermatomyositis show a detectable level of autoantibodies in their blood. It's unclear whether these autoantibodies are involved in causing dermatomyositis." (same link as above)
"21 June 1993
Summary The frequency and features of joint involvement were evaluated in 29 patients with polymyositis/dermatomyositis (PM/DM); eight of them (27.5%) presented arthritis. Mean age was 30 years, and mean disease duration was 5.3 years. Oligoarthritis was observed in 5 cases, while 3 presented polyarthritis; in most cases arthritis was concurrent with the musculocutaneous picture. On comparing the 8 arthritis patients with the remaining 21, no significant clinical or serological differences were found. However, males predominated in the arthritis group, 75% vs 19% (p<0.05). Arthritis responded favourably to underlying disease treatment and articular sequelae were not observed."
~SUPPORT GROUPS~
If you EVER need more information or someone to talk to, PLEASE feel free to email me...I have more information than the entire web probably has put together.. Its been 3 years since my muscle biopsy and dx now...it's been a long and scary road, and I'm still fighting. I'll help you on your road in any way I can...just let me know =)
Alex, 13 years old, JDMS warrior for 3+ years & founder of Awareness Angels as well as many other charities/etc
***edited by moderator*** web addresses not allowed *** private e-mails not allowed ***
Please read our Terms of Use
Loading...
I found out almost 2 years ago that I have this dreaded disease, and I am 58. All my life I was thin and worked hard the last few years to stay that way. However the disease required high doses of Prednisone for almost 10 months and I blew up like a balloon. This has been very depressing for me because I find that now I can't work out like I used to.
I am looking for a support group, I know this is a rare disease but I would really like to others that have it. Does anyone have any leads? God bless you all!!! My heart goes out to the children that are dealing with this, but from what I have read, they can outgrow the disease. I sure hope so!!!!
Karen
I am looking for a support group, I know this is a rare disease but I would really like to others that have it. Does anyone have any leads? God bless you all!!! My heart goes out to the children that are dealing with this, but from what I have read, they can outgrow the disease. I sure hope so!!!!
Karen
Loading...
Dermatamyositis is an autoimmune disorder where the skin and muscles become inflamed without an obvious cause.a definitive diagnosis would require a skin and muscle biopsy.
------------------
Shine Eric
------------------
Shine Eric
Loading...
I am one of the fortunate people who have been diagnosed with dermatomyositis but I only suffer with the rash part. I think its called amyositis. The rash first started on my knuckles 16 yrs ago and has progressed to my arms, scalp,forehead and seems to be spreading to other areas of my face. It seems like sometimes the "new rash" may go away in some places. I want to know what can be done to stop the progression of the rash or is it considered like a flare up. I was about 20 when I first noticed the rash on my hands and I was formally diagnosed about 4 yrs by my dermatalogist ago at the age of 34. I am blessed that none of my muscles are involved but the rash is very embarassing. What is the next step I should take? Any other specialists out there to help?
Loading...
Symptoms are red skin, blisters, crusty skin, and hair loss of the ear tips, face, around the eyes tip of the tail, elbows and toes and legs. The skin may become scarred and hairless. The hair may regrow. Your vet must do a biopsy of the skin and muscle to verify this condition since other conditions have similar symptoms.
Loading...