 What causes heart disease?
What causes heart disease?
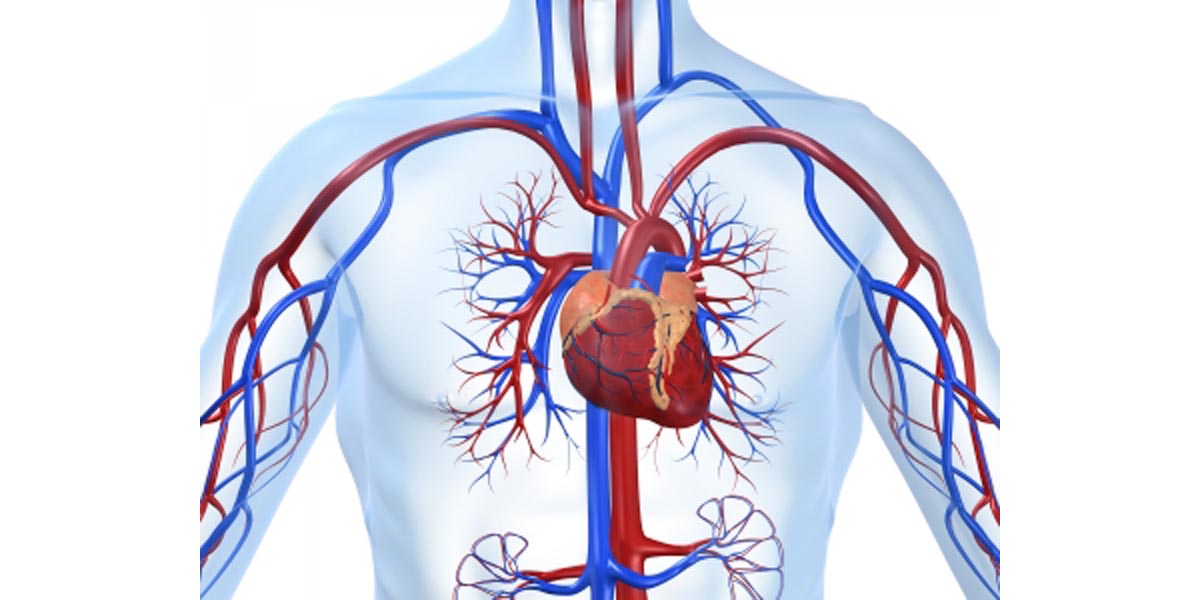
This buildup is called an atherosclerotic plaque and the condition of having these plaques in ones arteries is called atherosclerosis, which means “hardening of the arteries”. The buildups constrict the arteries and make it harder for blood to flow through them.
Usually, patients have atherosclerosis in the major arteries all over the body, not only in the heart. This means that the heart has to work extra hard to pump blood to the body. The plaques in the coronary arteries (the arteries around the heart muscle) constrict the blood flow to the heart muscle and can cause oxygen deficiency, which causes symptoms of angina like chest pain and shortness of breath.
Plaques are also sensitive to rupture or can dislodge and completely block the artery. If a blockage happens in a coronary artery a heart attack is the result. Blockages or ruptures in arteries of the brain result in a stroke.
There are also diseases that result from atherosclerosis in peripheral arteries like e.g. intermittent claudication, a condition in which atherosclerosis interferes with the blood flow to the legs. It causes severe pain in the legs with walking that goes away when resting.
What is chelation therapy?
Chelation therapy is the intravenous infusion with an artificial amino acid called ethylene-diamine-tetra-acetic-acid or short EDTA. The therapy has been developed in the 1940s as a therapy for heavy metal poisonings like e.g. with lead, or mercury, as EDTA can bind heavy metals. The heavy metals that are bound to the EDTA can then be safely excreted by the kidney. This therapy is also used for cases of radiation poisoning in which radioactive substances were accidentally ingested.
As it was recognized that atherosclerotic plaques contain calcium in the 1960s, a hypothesis was formed that EDTA, which can also bind calcium, might be able to dissolve existing atherosclerotic plaques or at least prevent their formation and thus prevent the progression of existing atherosclerosis.
The therapy today consists of 5-30 session of an intravenous (I.V.) infusion of EDTA that takes about 2-4 hours in the first month. 30 sessions is the most common regimen. Most patients are recommended to return for once monthly follow-up treatments. The therapy is also usually accompanied by life-style changes like smoking cessation, better nutrition (less saturated fats, more fruit and veggies, vitamin supplements), regular exercise and an attempt to lose weight.
What evidence is available for its efficacy or lack thereof?
Many chelation therapists report that their patients feel better and show better heart function after therapy. There are also numerous reports of patients who claim they owe their life to this miracle drug. Can these claims be substantiated scientifically or are they due to the lifestyle changes that usually accompany the therapy or the expectation of the patient that a therapy that costs $3000-5000 and that is not covered by any insurance, has to be doing some good?
In the 1960, scientists have done a small study with 30 patients. However, two patient died during the study and there was no benefit seen for the 28 others, so the study was stopped prematurely.
In 2002, a study was published in the Journal of the American Medical Association (JAMA 2002;287:481-486). In this study, 84 coronary artery disease patients were followed for 27 weeks. It was a double–blind, placebo-controlled study, i.e. one group of patients received the I.V. chelation therapy, and the other half of patients received just IV fluid without EDTA in it (placebo).
A study is called double –blind, if neither the patients nor the doctors know who received the medication and who received placebo, to avoid psychological effects of expecting the drug to work. This kind of study is the scientific gold-standard to figure out whether a drug works or not.
The patients in the JAMA-study were asked to sit on an exercise bike while having an electrocardiogram (ECG) done at the start and end of the 27-week study. The time it took from the start of the exercising to the time point when the patient’s ECG showed signs of ischemia, which is oxygen deficiency in the heart, was measured. The patients were also asked to fill out a quality of life questionnaire at the start and end of the study. After 27 weeks, no difference was found between the placebo and chelation-therapy group.
It is, however, possible that there are benefits of chelation therapy, but the benefits are too small to be detected in this relatively small study. For that reason there is currently a large study underway, funded by the National Institutes of Health that involves 2372 patients over 50 years with coronary artery disease. This study is large enough to be able to conclusively show whether chelation therapy has any small or moderate effects on this disease.
The Trial to Assess Chelation Therapy (TACT) was a significant study initiated to evaluate the efficacy and safety of chelation therapy in patients with heart disease. Conducted between 2003 and 2012, it was a randomized, double-blind, placebo-controlled trial involving over 1,700 participants with a history of myocardial infarction. The primary aim was to assess whether intravenous chelation therapy with disodium EDTA, combined with oral vitamins and minerals, could reduce cardiac events compared to a placebo.
The results of TACT showed a modest reduction in cardiovascular events among the chelation group, particularly notable in diabetic patients. However, the study faced criticism for methodological issues, including inconsistent participant follow-up and a high dropout rate. Despite its findings, the medical community remains cautious, and chelation therapy for heart disease is not widely accepted or recommended as a standard treatment due to lingering questions about its efficacy and safety.
Read More: Statin: Drug for Heart Disease
What are the risks and side effects of chelation therapy?
As with all drugs, EDTA-therapy is not without side effects, some of them severe. The biggest risk with chelation therapy is that of acute kidney failure that might lead the patient to require either dialysis for the rest of his life or a kidney transplant. Other side effects reported with chelation therapy are bone marrow depression, shock, low blood pressure (hypotension), convulsions, irregular heart beat, allergic reactions, and respiratory arrest. There are a number of deaths each year in the USA that are linked with chelation therapy.
No, it is not true. The AHA opposes this treatment because it has no proven effect, there is scientific evidence that it has no effect, and it is not considered safe. If it were safe and effective, it might actually be able to increase the income of heart specialists, as it could be used for people who don’t have severe enough symptoms to require surgery. One session of chelation therapy cost between $50 and $100, it could be done on as many patients at a time as fit in the practice of the heart therapist, and the patients would come back at least for 30 sessions. A surgery, however, can always only be done on one patient at a time.
- www.americanheart.org/presenter.jhtml?identifier=3000843
- www.mayoclinic.com/health/chelation-therapy/MY00159
- en.wikipedia.org/wiki/Chelation_therapy
- www.skepdic.com/chelate.html


Your thoughts on this