Table of Contents
Many type 2 diabetics bemoan the possibility of "having to" go on insulin injections to control their blood sugar levels. Insulin, however, is the only medication for diabetes that always lowers blood sugar levels (if you take enough), and it is the only medication that can, paradoxically, preserve the ability of the beta cells of the pancreas to continue to make at least small amounts of insulin to prevent complete dependence on insulin injections.
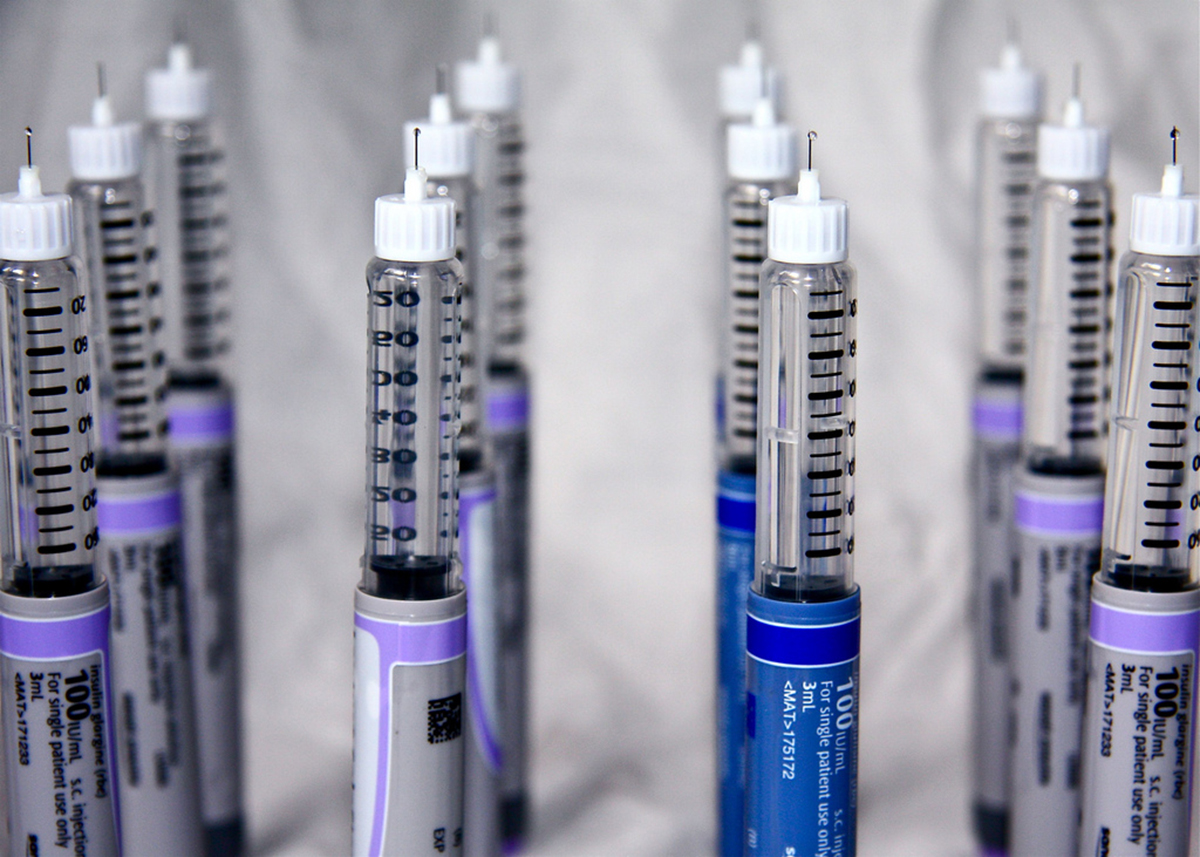
Exercise and Diet Seldom the Entire Answer for Diabetes
Exercise, especially resistance exercise, can make a huge difference in blood sugar control. When you work out muscles hard enough that they begin to break down, they repair themselves with the help of amino acids to rebuild muscle fibers plus glucose and water from the bloodstream to make glycogen. It's the glycogen that "pumps up" new muscle, and to get enough glucose to make glycogen after a strenuous workout, muscles temporarily (for an hour or two) become 50 times more sensitive to insulin.
But for keeping your blood sugar levels constantly below the 170 mg/dl (10 mmol/liter) at which permanent damage starts, chances are that exercise and diet just aren't going to work for you. Some kind of medication is needed.
Not Every Medication that Lowers Your Blood Sugar Is Helpful in Diabetes
There is a very simple way, at least in the early stages of diabetes, to get blood sugar levels down. Take a medication such as glipizide, which is also known as Glucotrol, to force your pancreas to make more insulin. More insulin goes into circulation, and blood sugar levels go down. Your diabetes may be at least temporarily "controlled," but the underlying problem can get worse.
High blood sugar levels (above 170 mg/dl or 10 mmol/L) cause fat cells, liver cells, and cells in the muscles to shut down some of the receptor sites for the blood sugar glucose. This keeps the cell from being flooded with sugar it would have to burn with the release of potentially toxic free radicals of oxygen. When these cells don't take in as much sugar as they normally do, it stays in the bloodstream, and the pancreas tries to normalize blood sugar levels by releasing still more insulin.
The extra insulin wins out and cells all over the body are forced to absorb more sugar from the bloodstream, but the extra insulin production causes a phenomenon known as beta-cell depletion. Essentially, the insulin-making cells of the pancreas begin to burn out under the extra burden of producing insulin forced by the medication. By the time that diabetes is diagnosed, typically about 85% of beta cells no longer function properly.
See Also: Insulin Pump for Type 1 and Type 2 Diabetes
Other medications for diabetes have equally harmful side effects. The thiazolidinedione drugs Actos and Avandia cause fat cells to multiply--even in bone and brain. The glucagon-like peptide-1 agonist Byetta increases the risk of horrific skin reactions and pancreatic cancer. Even a generally useful drug like metformin can cause vitamin B deficiency.
- Rister, R. Healing without Medication. Basic Health Books, 2003.
- Photo courtesy of Heather Aitken by Flickr : www.flickr.com/photos/feathy123/3949274968
- Photo courtesy of geralt by Pixabay : pixabay.com/en/insulin-insulin-syringe-syringe-113200/


Your thoughts on this