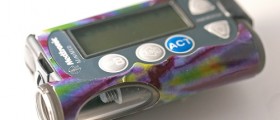
Many diabetics are very happy with insulin pumps. Living with an insulin pump, however, takes a little adjustment.
Insulin-dependent diabetics who aren't on a pump typically take a long-lasting or "slow" insulin to prevent spikes in blood glucose levels during the night. In this United States, this is usually one injection of Levemir every 24 hours or an injection of Lantus every 12 hours. The new insulin Toujeo is three times as concentrated, and is used in a much small dosage once a day. Some people can't afford Lantus or Levemir and take Humulin or "N."
They also take a short-acting or "fast" insulin before every meal to keep blood sugar levels down after meals. How much short-acting insulin a diabetic takes is usually determined by a sliding scale. Diabetics (are supposed to) take their blood sugar levels before a meal, and take more short-acting insulin if their blood sugar levels are high and less short-acting insulin if their blood sugar levels are low. Diabetics can also take more insulin to cover the added carbohydrates in a dessert, but this isn't a good idea, since even "fast" insulin isn't as fast as the insulin released by the body, and blood sugar levels inevitably soar after any meal containing carbohydrates.
An insulin shot releases a lot of insulin into a single location. There can be allergic reactions to chemicals used to stabilize insulin in the vial, which interfere with the body's ability to absorb the injected insulin. It's possible to get a bubble of insulin beneath the skin. There's always some loss of insulin any time more than seven units (0.07 ml) of insulin is injected in the same location, and many diabetics inject up to 25 units of fast insulin and even 100 units of slow insulin in a single shot. Every time insulin is injected, a little is lost. This isn't a problem with the insulin pump.
A reality about diabetics is that most diabetics don't like to do blood sugar testing, pricking the skin, putting blood on a slide, and waiting for a glucometer to give them a blood sugar level. This is still necessary at least once a day with even the most modern insulin pump, but some models give instant readouts of blood sugar levels without finger sticks. Moreover, because the insulin pump is measuring glucose in venous blood and the glucometer uses peripheral blood, the insulin pump gives a more accurate reading, and the insulin pump gives better blood sugar control.
What are the disadvantages of an insulin pump?
- They are expensive. It usually costs $5,000 to get started, and about $2,000 a year for supplies.
- Diabetics must be under the care of an endocrinologist, not a primary care physician who specializes in diabetes, to the the pump.
- Insulin pumps don't use long-lasting insulin. Any mistakes in diet or programming cost immediate problems that aren't necessarily easy to correct.
- If the catheter comes loose, you don't get insulin. Diabetic ketoacidosis can result.
- Insulin is constantly available to keep fat locked in fat cells. It's not unusual for users to gain weight, on average about 4-5 kilos (9-11 pounds).
- Contact with water requires removal and reattachment of the pump. Contact sports require similar precautions.
- Insulin pumps are preprogrammed to release more insulin about two hours before the user usually wakes up to cover increased blood sugar levels caused by the "dawn phenomenon." When the user has been awake all night, the dawn phenomenon doesn't occur, but the insulin is still released. This can cause dangerously low blood sugar levels.
- The injection site can become infected.
- Neither multiple daily injections nor an insulin pump will give diabetics perfect control over blood sugar levels. However, glycosylated hemoglobin (HbA1C) levels are usually better with the pump than with multiple daily injections.
- David S. Schade, MD and Virginia Valentine, CNS, BC-ADM, CDE. To Pump or Not to Pump. Diabetes Care. doi: 10.2337/diacare.25.11.2100 Diabetes Care November 2002 vol. 25 no. 11 2100-2102.
- Photo courtesy of SteadyHealth