What is the Pancreas?
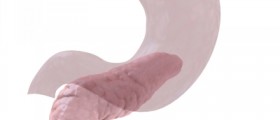
The pancreas is a six-inch long tadpole-shaped organ located behind the stomach. It plays a vital role in converting ingested food into fuel for use by the cells of the body, as well as regulating blood glucose levels.
What are its Functions?
The exocrine glands of the pancreas produce juices that contain various digestive enzymes. These juices are secreted into the duodenum and assist in the breakdown of fats, proteins and carbohydrates.
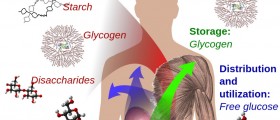
The endocrine function of the pancreas is due to specialized cells known as "Islets of Langerhans"'. These cells produce the hormones insulin and glucagon, which help to lower and raise blood sugar levels according to the needs of the body.
What is a Total Pancreatectomy?
A pancreatectomy is a surgical procedure that involves the partial or complete removal of the pancreas.
The gallbladder, common bile duct, some parts of the stomach and small intestine, and the spleen are removed as well.
Why is it required?
This operation is primarily performed in order to remove tumors in the head or body of the pancreas. It may be used to treat chronic pancreatitis when other treatments do not respond.
A total pancreatectomy may also be required to treat the following conditions:
- Severe trauma and inflammation
- Necrotizing pancreatitis
- Neoplasms or adenocarcinomas
- Severe hyperinsulinemic hypoglycemia
- Cystadenomas (mucinous/serous) or cystadenocarcinomas
- Acinar cell or neuroendocrine tumors (tumors of the Islet cells)
- Ampullary or duodenal cancer
- Cancer of the distal (lower portion) of the bile duct
- Papillary cystic neoplasms
- Lymphomas
It is now very rarely used to treat exocrine cancers of the pancreas, since no significant advantages of the procedure were seen.
What Adjustments need to be made to Live without Pancreas?
Life after a total pancreatectomy is certainly possible. However, after the pancreas is totally removed, certain lifestyle changes need to be made. These include the following:
- Diabetes
Since the Islet cells are removed, there is no production of insulin or glucagon. This means that the body cannot manage or maintain blood glucose levels on its own. Thus, the development of diabetes is a huge concern. Management involves taking insulin by injection for the whole life and following a diabetic diet.
- Vaccines
Due to some medical reasons, the spleen is usually removed along with the pancreas. Since the spleen will be excised, the doctor may recommend certain vaccines prior to the operation. The patient is also put on prophylactic antibiotics to prevent any infection.
- Weight Loss
Losing 10-15 pounds after the surgery is very common. This loss will be compensated once appetite returns and normal nutritional intake is resumed.
- Pancreatic Enzyme Insufficiency
Pancreatic enzyme replacement therapy will be prescribed by the physician to help aid the digestion of food. Pancreatic enzyme pills may also be taken to help with the digestion of specific foods.
- Delayed Gastric Emptying
This implies that the stomach takes longer than usual to empty its contents. This might cause nausea, vomiting and heartburn, and the condition is known as "gastric ileus" (temporary paralysis of the stomach). After a few weeks or months, this condition is inherently resolved as the stomach begins to adapt and heal. However, always consult a surgeon if the problem persists.
- Exercises
Certain post-operative exercises may speed up the recovery and ease any persisting pain. These include deep-breathing and progressive relaxation techniques while lying on your back, such as ankle flexes, knee bends and crossed-leg muscle contractions.
It may take a few weeks or a few months to regain normal stomach function and alleviate symptoms such as diarrhea and pain. General recommendations include eating small and frequent meals, starting meals with a protein portion and staying hydrated.
- pancreasmd.org/education_home.html
- http://www.surgery.ucsf.edu/conditions--procedures/pancreatectomy.aspx
- https://www.medstarhealth.org/Pages/Services/Cancer-Care/Pancreatic-Cancer/Diagnosis-and-Treatments/Surgery/Total-Pancreatectomy.aspx
- http://www.mdguidelines.com/pancreatectomy
- Photo courtesy of SteadyHealth