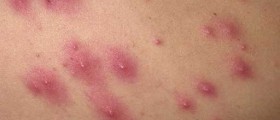
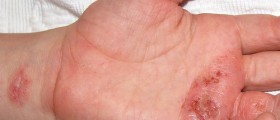
I am really concerned about a few things here. I had sex with a girl over a month ago and within the last week, I have noticed constant itching literally all over my body, but mostly around my pelvic area (inner thigh, on penis and scrotum). I see these tiny red bumps around my body spread out and not in lines or clusters. Eventually during the day, they stop itching and at one instance I placed some hydrocortisone cream on them and they stopped itching.
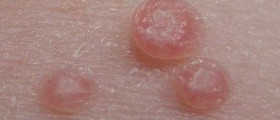
Last week, I noticed a puss, cyst like bump on my penis (on the top layer, not head of penis). It's not too big or anything, but you can notice it from afar looking at it in the mirror. It becomes itchy at times but then stops itching later. I then notice these smooth-like surface bumps on my scrotum. It's too hard to see, but it looks like two to three bumps together. It too itches for a little bit and stops itching, and they are spread out on my scrotum. It's only like two on the scrotum. They are very smooth surfaced, and they don't hurt but itch from time to time.
What's wrong with me? I soon am going to pay a visit to Patient First and see if they can diagnose this. I am getting worried here. Any ideas what this could be? My anus also has been itching a couple times as well. But only a couple bumps are there. Any information? I am including pictures here:
***this post is edited by moderator *** ***explicit and graphic content*** Please read our Terms of Use
Scabies? Genital warts? Molluscum Contagiosum? And how bad will this be on my life?
Thanks.
Loading...
Lichen simplex chronicus (also known as "Neurodermatitis"[1]) is a skin disorder characterized by chronic itching and scratching. The constant scratching causes thick, leathery, brownish skin.
Causes
This is a skin disorder characterized by a self-perpetuating scratch-itch cycle:
It may begin with something that rubs, irritates, or scratches the skin, such as clothing.This causes the person to rub or scratch the affected area. Constant scratching causes the skin to thicken.The thickened skin itches, causing more scratching, causing more thickening.Affected area may spread rapidly through the rest of the body.
The skin may become leathery and brownish in the affected area. This disorder may be associated with atopic dermatitis (eczema) or psoriasis. It may also be associated with nervousness, anxiety, depression, and other psychological disorders.
Source: http://en.wikipedia.org/wiki/Lichen_simplex_chronicus
LSC is thickening of the skin, with an increase in skin markings, that develops as a physiological cutaneous response to repetitive scratching or rubbing. LSC is a secondary rather than a primary process: that is, pruritus precedes the appearance of LSC.
Patients usually report that pruritus is worse in the night when they are about to go to sleep and when they are still or quiet. During the daytime, when patients are occupied with other affairs, the urge to scratch is minimal or nonexistent.
LSC can occur on any body area that the patient can reach to scratch, particularly the scalp, nape of neck, extensor surface of forearms and elbows (Figure 4), vulva and scrotum, outer aspect of the upper medial thighs, knees, lower legs, ankles and, rarely, the hands (Figure 5). It can be associated with erosion and xerosis (Figure 6). There can be overlap between LSC, xerosis, and amyloidosis (Figure 7). LSC that occurs on and around the genitals of men can be marked by striking erythema (Figure 8).
Plaques of LSC average 3 to 6 cm in diameter. These plaques often have 3 zones. A 2- to 3-cm–wide peripheral zone that is minimally hyperkeratotic may have isolated prurigo nodularis papules. The middle zone has lenticular and hemispheric prurigo papules that may be eroded. The central zone of LSC exhibits the most pronounced hyperkeratosis and pigmentary alteration, especially hyperpigmentation.
Treatment
As a first-line treatment, I advise patients to stop scratching and offer advice on how to decrease the sensation of itching. To try to break the itch-scratch cycle, I initially prescribe a topical corticosteroid of the most potent type; if it is effective, I taper to a less potent corticosteroid. I also tell patients that ice is one of the most effective antipruritic agents and that application of crushed ice in a plastic bag to an area of LSC for 5 to 10 minutes often can reduce the urge to scratch.
As adjuvants to ice and corticosteroids, I prescribe topical doxepin, topical tacrolimus or pimecrolimus, and lidocaine. Menthol, phenol, pramoxine, capsaicin cream, and vitamin D3 ointment can also be used to reduce pruritus. Occlusion of the medication, in particular by the use of corticosteroid-impregnated tape (eg, flurandrenolide [Cordran] tape), can increase the potency and enhance delivery of the antipruritic therapy and provide a physical barrier to scratching.
If plaques occur on the body and do not respond to topical treatments, I inject triamcinolone, 3 mg/mL, into the lesions. LSC may become secondarily infected if erosions develop after it is scratched; in this case, it should be treated with topical mupirocin. Cases of LSC unresponsive to other therapies can be treated with UV-B phototherapy.5 I do not find that oral antihistamines are effective for LSC. No therapy has a 100% success rate, but treatment often decreases the urge to scratch.
Source: http://www.consultant360.com/content/skin-disorders-older-adults-dermatoses-related-scratching-rubbing-and-impaired-epidermal-int
Loading...