There are several possible causes of folliculitis — a condition in which the hair follicles become inflamed. Folliculitis can be caused by an fungal or bacterial infection, occlusion, irritation and specific skin diseases.
This condition can affect both women and men at any age and it can develop on any part of the body where hair follicles are present, but is most likely to occur on the scalp, face, or parts of the arms, armpits, or legs if they’re not usually covered by clothing. In short, folliculitis is an inflammation of one or more hair follicles and it can occur anywhere on the skin. [1]
 Possible causes of folliculitis
Possible causes of folliculitis
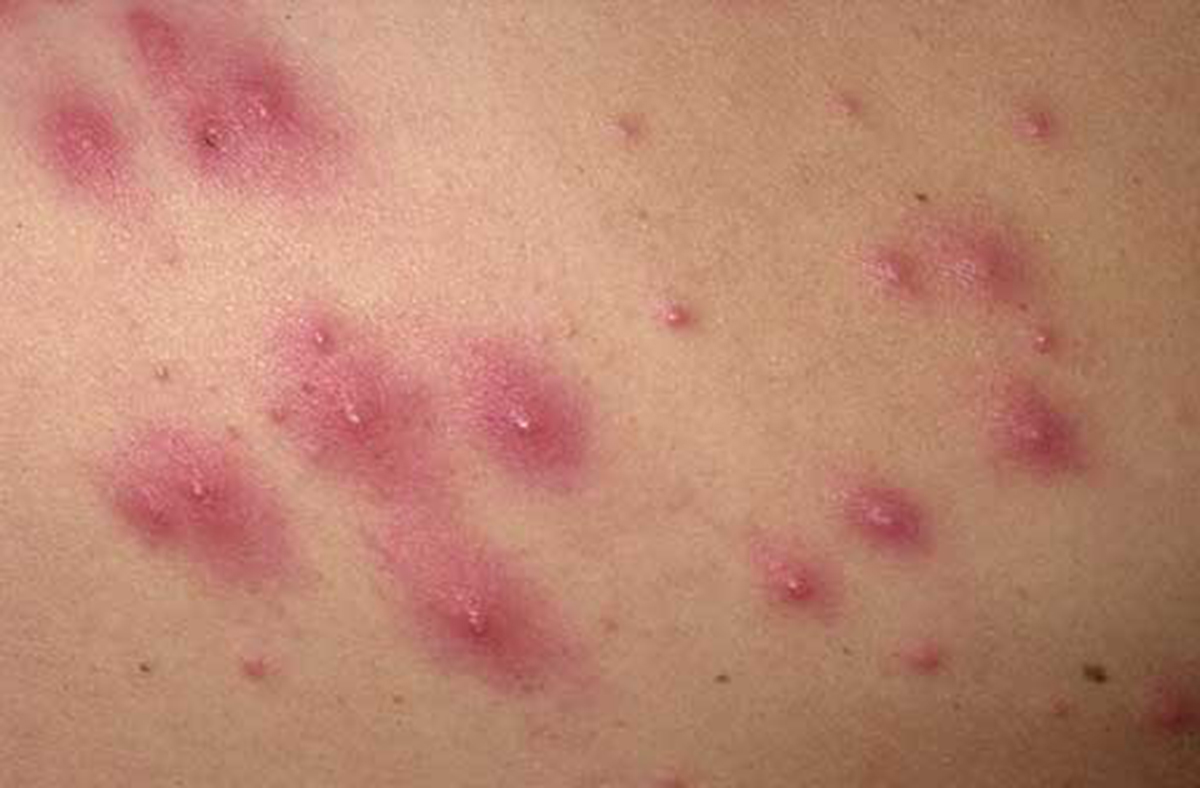
Folliculitis can develop when bacteria, such as Staphylococcus or Pseudomonas, enter the body through a cut, scrape, surgical incision, or other breaks in the skin near a hair follicle. Folliculitis often strikes on areas of the skin that are shaved, due to careless shaving or mistakes while shaving.
A folliculitis infection due to yeast and fungi can occasionally appear as well, especially in immunocompromised patients.
Scratching the affected area can trap fungi or bacteria under the fingernails and spread the infection to hair follicles on other parts of the body, making the condition somewhat "contagious", if proper care is not taken. The fact that the bacteria that cause folliculitis are contagious also means that a person who has folliculitis can infect others who live in the same household, through the sharing of towels or bed sheets, for instance. [1]
Signs, symptoms, and treatment of folliculitis
The symptoms of folliculitis may vary, depending on the type of infection. There are two types of folliculitis:
- The superficial form of folliculitis
- And the deep form of folliculitis
In the superficial forms of the disorder, small pimples develop around one or more hair follicles. Deep folliculitis, which affects the entire hair follicle, can cause more severe signs and symptoms, including fever, pain, large masses, and permanent hair loss. The types presented below are usually in the superficial group, but superficial folliculitis can progress into the deeper form.
The types of superficial folliculitis
1. Pseudomonas folliculitis
The bacterium P. aeruginosa that causes this type of folliculitis can be found in a wide range of environments, including wooden hot tubs, whirlpools, saunas, swimming pools, water slides, and physiotherapy pools.
The symptoms of this kind of folliculitis are characteristic and they appear about 12 to 48 hours after being exposed to the causative bacteria — usually, eruptions involve the trunk and the upper parts of the arms and legs. The rash may be more severe in areas covered by a swimsuit, because those parts of the skin were exposed to the contaminated water for a longer period of time. Pseudomonas folliculitis never occurs on the palms of the hands and soles of the feet, since there are no hair follicles in those areas.
Patients with Pseudomonas folliculitis will complain of numerous red, round, itchy bumps that later may develop into small pus-filled blisters. They may even experience a headache, nausea, vomiting, abdominal cramps, and sore throat may accompany the rash, rhinitis, sore eyes, and fever.
Treatment: Pseudomonas folliculitis can be diagnosed with a culture from pus-filled pimples on the skin. This type of folliculitis rarely requires medical treatment, as the rash associated with this infection will usually go away on its own. Occasionally, the doctor may prescribe an oral or topical "anti-itch" medication to help relieve any unbearable itching you may be suffering from. [2]
2. Barber's itch
This type of folliculitis is characterized by itchy, white, pus-filled lumps in the area where men can grow a beard. It usually occurs when hair follicles that have been irritated by shaving become infected with Staphylococcus aureus bacteria. Although these bacteria live on your skin all the time, they cause problems when they enter the body through a cut.
Treatment: In most cases, the doctor will advise you not to shave the affected area until the infection heals. This precaution is usually enough but if the problem persists, you may need topical or oral antibiotics.
3. Tinea barbae
Unlike the previous types, tinea barbae is caused by a fungus. Tinea is actually a group of diseases caused by a fungus, and this includes ringworm, athlete's foot, and jock itch, but tinea also develops in the beard area in men.
Tinea is characterized by itchy, white bumps and the surrounding skin also may become reddened.
Tinea infections are usually not serious, but they can be uncomfortable. You can get them by touching an infected person, from damp surfaces such as shower floors, or even from a pet.
Treatment: This infection it is usually effectively treated with oral antifungal medications. Over-the-counter creams and powders will get rid of many tinea infections, particularly athlete's foot and jock itch. Other cases require prescription medicine. [3]
4. Pseudofolliculitis barbae
This is also an inflammation of the hair follicles in the beard area. It is called pseudofolliculitis because it develops when shaved hairs curve back into the skin, leading to inflammation and dark raised scars. Pseudofolliculitis barbae is a disorder that occurs mainly in African American men because their beard is typically curly and curly hairs that are cut too short may curve back into the skin and cause inflammation. [1]
Treatment: Experts claim that the best treatment for this condition is prevention and it includes simple shaving with an electric razor. When using the razor, it is best to use also a shaving gel instead of cream, and shave in the direction of the hair growth.
5. Pityrosporum folliculitis
This condition is very common, especially among young and middle-aged adults. This type of folliculitis produces chronic, red, itchy pustules on the back and chest and sometimes on the neck, shoulders, upper arms and face. It's caused by an overgrowth of fungus that leads to a fungal infection called Malassezia furfur.
This condition is commonly misdiagnosed as acne vulgaris and it can persist for years. Because of its common misdiagnosis with acne vulgaris, you should know that Pityrosporum folliculitis does not respond well to typical acne medications; making this itself a sign of Pityrosporum folliculitis. [4]
Treatment: Topical or oral antifungal medications are the most effective treatments for this type of folliculitis. It is proven that antibiotics aren't helpful in treating pityrosporum folliculitis and may even make the infection worse. Oral antifungals are the most effective treatment and result in rapid improvement.
5. Herpetic folliculitis
Herpes folliculitis is a rare manifestation of a herpes virus infection and it is often misdiagnosed. Sometimes the virus called Herpes Simplex can enter the skin through small lesions made by shaving. From there, herpes can spread to the surrounding follicles. However, recently it has been suggested that herpetic folliculitis is more common in infections with varicella zoster (VZV) than in those with herpes simplex viruses (HSV-1 and -2). [5]
Treatment: The doctor may prescribe an oral antiviral medication such as acyclovir, famciclovir or Valacyclovir. These drugs can clear the infection, but they also may cause side effects such as a headache, diarrhea, nausea and abdominal pain.
The types of deep folliculitis
1. Gram-negative folliculitis
Gram-negative bacteria include Escherichia coli, Pseudomonas aeruginosa, Serratia marcescens, Klebsiella and Proteus species. This type of folliculitis is usually found around the area of the upper lip under the nose, to the chin and cheeks and occurs most commonly in people who have been using antibiotics with a long-term treatment of acne with tetracycline or topical antibiotics. It is proven that antibiotics alter the normal balance of bacteria in the nose, leading to an overgrowth of harmful organisms — gram-negative bacteria.
Gram-negative folliculitis is a pustular rash and is very similar to acne. For this reason, it is often mistaken as a worsening of acne as it usually occurs in patients with existing acne [6]:
- In about 80% of patients, Gram-negative folliculitis causes superficial pustules with relatively few papules and comedones. These lesions are usually caused by Klebsiella, Escherichia and Serratia species.
- In about 20% of patients with Gram-negative folliculitis, lesions are deep, nodular and cyst-like. These are caused by Proteus species, which are able to invade deeply into the skin and create pus-filled abscesses and cysts.
Treatment: This type of folliculitis is usually treated with:
- Antibiotics to which the organisms are sensitive (eg ampicillin, trimethoprim)
- Isotretinoin (Accutane®) which appears to act by suppressing sebum production and drying out the mucous membranes, especially the nasal mucous membranes, which is where causative bacteria are found
2. Boils and carbuncles
Boils occur when hair follicles become deeply infected with staphylococcus bacteria. Boils look like a painful pink or red bump about a centimeter in diameter. The surrounding skin may also be red and swollen. A carbuncle is actually a cluster of boils that often occurs on the back of the neck, shoulders or thighs, especially in older men and represent a deeper and more severe infection than a single boil.
Treatment: A doctor should drain every large boil or carbuncle by making a small incision in the tip. This usually relieves pain, speeds recovery and helps lessen the scarring. Sometimes the antibiotics for boils are recommended to help heal severe or recurrent boil infections.
3. Eosinophilic folliculitis
This type of folliculitis is characterized by recurring patches of inflamed, pus-filled sores, primarily on the face and sometimes on the back or upper arms. The exact cause of eosinophilic folliculitis isn't known, but it is most commonly seen in HIV positive people. However, there are three types of eosinophilic folliculitis:
- Classic
- Infancy-associated
- Immunosuppression-associated (mostly HIV-associated)
Treatment [7] :
- Topical corticosteroids are often the treatment of choice. Patients should know that steroids may have serious side effects and should be used for as brief a time as possible.
- Topical tacrolimus seems to be useful initial therapy as well.
- Oral indometacin (50-75 mg/day) is an effective treatment of classic EPF although it can induce peptic ulcers.
- For treatment of HIV-associated eosinophilic folliculitis (when topical corticosteroids and indometacin do not work) other treatment options, such as cetirizine 20-40 mg/day, metronidazole 250 mg three times a day, itraconazole starting at a dosage of 200 mg/day and increasing to 300-400 mg/day, and topical permethrin should be considered.
- If these treatments do not work phototherapy with UVB is the 'gold standard' of treatment and is often curative.
- ART should also be considered as one of the primary treatments for patients with HIV who suffer form eosinophilic folliculitis.
Risk factors for developing folliculitis
There are some conditions which can make a person more prone to developing folliculitis. They include:
- Acne or dermatitis
- Trauma to your skin from surgery
- Long-term antibiotic therapy for acne
- Topical corticosteroid therapy
- Diabetes, chronic leukemia, organ transplantation and HIV/AIDS
- Obesity — folliculitis is more common in people who are overweight
- Living in a warm, humid climate
- Using a hot tub, whirlpool, or swimming pool that is not properly treated with chlorine.
- Wearing tight clothes.
- Use or work around substances that can irritate or block the follicles
- Have an infected cut, scrape, or surgical incision.
Diagnosis of folliculitis
- Detailed patients history and examination
To diagnose folliculitis, the doctor will examine the patient’s skin and ask questions about his health and activities.
- Culture of the fluid in pimples
The doctor may perform tests to find out what is causing folliculitis and to make sure that the patient isn’t suffering from some other condition such as impetigo or heat rash. Examining a sample of the fluid in the pimples can help determine whether bacteria are causing the infection.
- Skin biopsy
If a fungus is suspected, the doctor will take a tissue sample, or biopsy, of the infected area.
Possible complications if left untreated
Mild cases of folliculitis usually do not cause any complications, and can resolve in its own. However, the infection may recur or spread, leading to large, itchy patches.
Complications of the more serious folliculitis infections may include:
- Cellulitis
This is a very serious bacterial infection. It is characterized by swollen, red area of skin that feels hot and tender. It may spread rapidly on legs, arms or face.
- Furunculous
This is also a serious condition which occurs when a number of very painful boils develop under the skin.
- Scarring
The serious types of folliculitis may leave thick, raised scars or patches of skin that are darker than normal. Destruction of the hair follicle can also lead to permanent hair loss.
READ Follicle Hormone: Effects on Pubertal Maturation
Alternative treatment
Eating a balanced diet, including protein, complex carbohydrates, healthy fats, fresh fruits and vegetables, and drinking eight to 10 glasses of water a day may stimulate the body's immune system and shorten the course of the infection.
- Garlic (Allium sativum) and goldenseal (Hydrastis canadensis), both antiseptic agents against staphylococcal infections, should be taken.
- Echinacea (Echinacea spp.) is also helpful in modulating immune function.
- Warm compresses made with white vinegar and water may help relieve itching and aid the healing process
- Burow’s solution (solution of aluminium triacetate; available as OTC) may help relieve itching and aid the healing process.
Daily doses of zinc, vitamin C and bioflavinoids can also strengthen the body's infection-fighting ability.
In some cases, a laser hair removal may be the only option. Laser treatment destroys the hair follicles so they can't become infected.

