Hernias occur when one part of the body protrudes through a gap or opening into another part. Although a hernia can develop almost anywhere, most of them happen in the abdominal area.
These include hiatal hernias (also known as diaphragmatic hernias), inguinal hernias, umbilical hernias, and others. Most of these small hiatal hernias don't cause any problems. Patients might even be unaware of the hernia unless a doctor discovers it when checking for some other condition. However, a large hiatal hernia can allow food and acid to back up into the esophagus, leading to heartburn and chest pain. Medications can usually alleviate these symptoms, although very large hiatal hernias may require surgical repair. Research has confirmed that hiatal hernia is a very common condition; by age 60, up to 60 percent of people have it to some degree.
 Types of hiatal hernia
Types of hiatal hernia
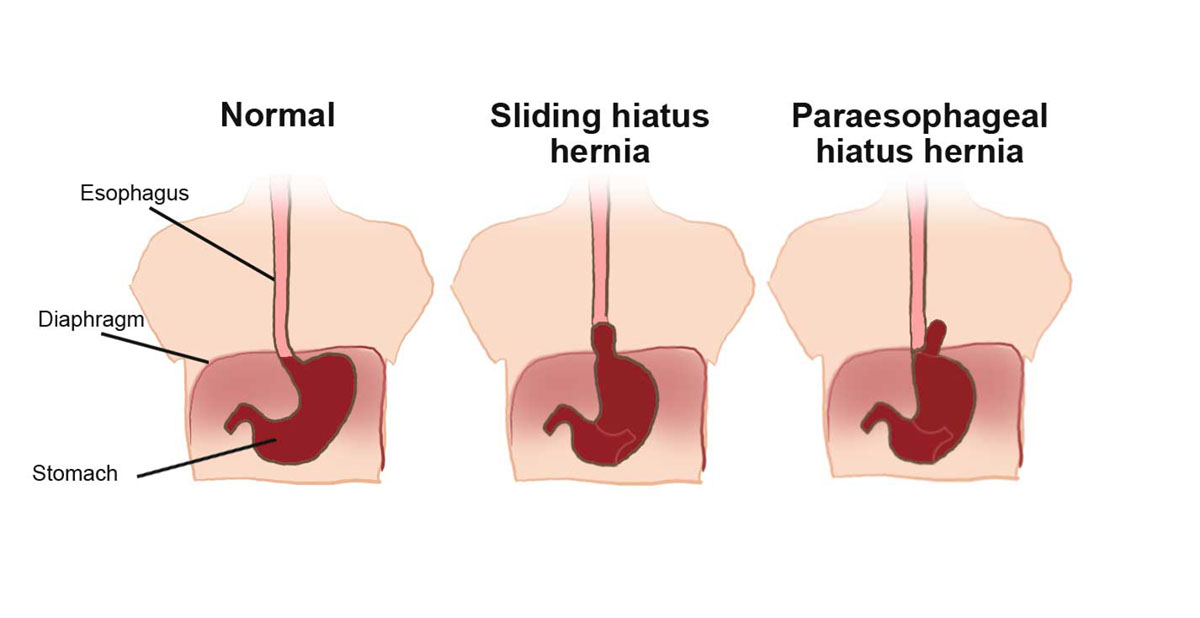
There are two main types of hiatal hernia: sliding and fixed.
* The sliding type of hiatal herbia: As its name implies, the sliding type of hiatal hernia occurs when the junction between the stomach and esophagus slides up through the esophageal hiatus.
This most commonly happens during moments of increased pressure in the abdominal cavity.
* The fixed type of hiatal hernia: Unlike the previous type, with fixed hiatal hernia there is no sliding up and down. A portion of the stomach remains permanently stuck in the chest cavity.
Possible causes of hiatal hernia
The chest cavity and abdomen are separated by the diaphragm, a large dome-shaped organ responsible for normal breathing. The esophagus (food pipe) passes into the stomach through an opening in the diaphragm. Hiatal hernias occur when the muscle tissue surrounding this opening weakens, and the upper part of the stomach bulges through the diaphragm into the chest cavity. Generally, anything that puts intense pressure on the abdomen can contribute to the formation of hiatal hernias.
Examples of situations that lead to increased pressure are:
* persistent or severe coughing or vomiting
* pregnancy
* straining while going to the bathroom
* lifting heavy objects
Hiatal hernia and gastro-esophageal reflux
Hiatal hernia can cause or contribute to gastro-esophageal reflux. This happens when a hernia slightly displaces the lower esophageal sphincter. This sphincter is nothing more than a circular band of muscle around the bottom of the esophagus. Normally, the diaphragm is aligned with the lower esophageal sphincter, relaxing to allow food and liquid to flow into the stomach during swallowing.
When this happens the diaphragm supports and puts pressure on the sphincter to keep it closed when not swallowing. However, a hiatal hernia raises the sphincter above the diaphragm, in turn reducing pressure on the valve which causes the sphincter muscle to open at the wrong time. This process allows stomach acid to flow up into the esophagus, often with uncomfortable symptoms.
Symptoms of hiatal hernia
In most cases, a hiatal hernia by itself causes no symptoms. The underlying processes at work in the body can lead to unpleasant sensations, however.
Some people with a hiatal herbia may experience:
* Chest pain or pressure
* Frequent belching
* Frequent episodes of heartburn
* Difficulty swallowing
* Coughing
* Hiccups
* Chronic pain
Diagnosis of hiatal hernia
Because it is often confused with heartburn, doctors often discover a hiatal hernia while trying to determine the cause of heartburn or chest or upper abdominal pain. There are several diagnostic methods that have the potential to discover this problem. These include:
* Barium X-ray: During this diagnostic test, the patient drinks a liquid containing barium that coats the upper digestive tract to provide a clear silhouette of the esophagus on an X-ray.
* Endoscopy: The doctor passes a thin, flexible tube with a fiber-optic light and video camera system down the patient’s throat to check for inflammation in this exam.
Possible complications
Large hiatal hernias can create lesions in the upper stomach which can sometimes bleed and lead to iron deficiency anemia from chronic blood loss. In some cases, the part of the stomach that protrudes into the chest cavity becomes twisted or cuts off blood flow to the rest of the stomach, in turn leading to severe chest pain and difficulty swallowing.
The most common complication of a hiatal hernia is probably gastro-esophageal reflux disease (GERD). Recurrent GERD itself can lead to complications, which include:
* Difficulty swallowing: Stomach acid backing up into the esophagus can lead to serious inflammation and scarring. This situatio can also narrow the opening of the esophagus, making it hard for a patient to swallow.
* Barrett's esophagus: This condition occurs from repeated, long-term exposure to excessive stomach acid. Cells similar to those in the stomach lining develop in the lower esophagus as a result, which represents a great risk for developing esophageal cancer.
* Esophageal cancer: Unfortunately, the prognosis for this condition is often poor. An esophageal tumor makes swallowing increasingly difficult, and eventually impossible.
Read More: Hernia Operation: Recovery After Hernia Surgery
Medications for people with a hiatal hernia
* Antacids: Some over-the-counter antacids can neutralize the acidity in the esophagus and provide relief from heartburn.
* H-2 blockers: These medications reduce the amount of acid secreted by the stomach by blocking histamine receptors. Some of the most commonly used include famotidine (Pepcid®), cimetidine (Tagamet®), ranitidine (Zantac®) and nizatidine (Axid®). Some patients may experience side effects such as bowel changes, dry mouth, dizziness, or drowsiness.
* Proton pump inhibitors (PPIs): These are the most effective drugs for the treatment of GERD because they block acid production and allow time for damaged esophageal tissue to heal. Some of the most commonly used are lansoprazole (Prevacid®), pantoprazole (Protonix®), rabeprazole (Aciphex®), Omeprazole (Prilosec®) and esomeprazole (Nexium®).
Surgical repair of hiatal hernias
Only a few people with a hiatal hernia may need surgery because it is usually considered only when medications and lifestyle changes fail to relieve severe reflux symptoms.
The operation may involve pulling the stomach down into the abdomen and making the opening in the diaphragm smaller. In some cases, this is done using a single incision in your chest wall or abdomen. In other cases, a surgeon may insert instruments and a fiber-optic camera through several small incisions in the abdomen. The operation is then called laparoscopic surgery.

