Temporomandibular joint syndrome (TMJ syndrome) is a notable myofascial pain-dysfunction syndrome- one very painful condition often misidentified and mistreated.
Most experts identify 3 distinct causes of pain at the TMJ, which collectively fall under the term of TMJ syndrome.
- Myofascial pain dysfunction (MPD) syndrome
It is about pain at the TMJ due to various causes of increased muscle tension and spasm. Most experts believe that this syndrome is a physical manifestation of psychological stress. No primary disorder of the joint itself is present.
- Internal derangement (ID)
This is condition where the problem lies within the joint itself. Several researches done in the past have proven that problem is most commonly with the position of the articulating disc
- Degenerative joint disease
This is condition caused by arthritic changes which result after degeneration of the articulating surfaces.
Incidence of the condition
TMD is a commonly seen condition in primary care and dentistry practice. Between 5% and 10% of Americans may sufficiently fulfill the criteria to merit a diagnosis of TMD. Some experts believe that 80 percent of the American population or approximately 10 million people have some form of abnormality of the temporomandibular joint, however only 40 percent or approximately 5 million Americans suffer symptoms severe enough to require medical treatment.
Normal anatomy of the temporomandibular joint
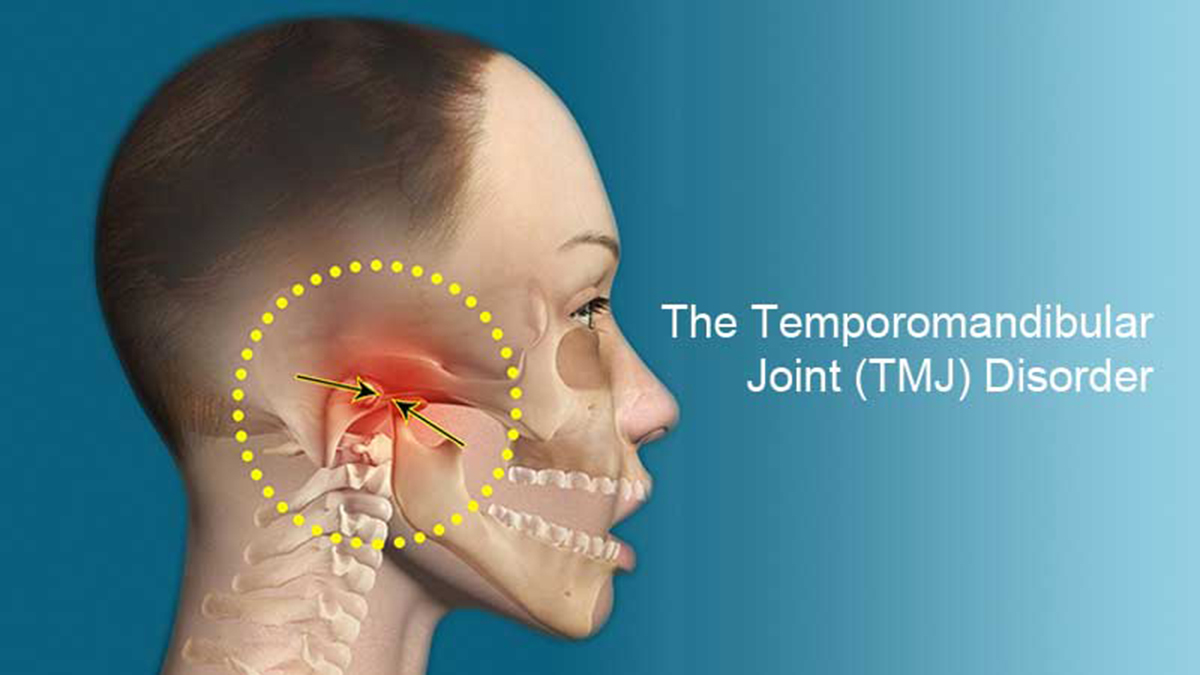
Well, everyone knows that human has 2 temporomandibular joints -one on the right and one on the left. They connect the skull to the lower jaw bone so as to allow the mouth to open and close. If we talk about the shape of the joint –then we should know that the TMJ is a gliding joint, formed by the condyle of the mandible and the squamous portion of the temporal bone. The articular surface has two parts - a convex articular eminence anteriorly and a concave articular fossa posterior. Although not too many people know about this- articular surfaces of the mandible and temporal bone are separated by an articular disk, which divides the joint cavity into 2 small spaces.
Possible etiology of the TMJ
The pathophysiology is not entirely understood, but it is believed that TMJ dysfunction syndrome is caused by both local insults and systemic disorders. There are many possible causes of this syndrome and that’s why, most of the experts claim that the etiology of TMJ includes trauma to the head, systemic disease, dental malocclusion, stress and/or some joint poor alignment resulting from and abnormal relationship between the spine, pelvis and other extremities and the base of the skull. But, there is also a big group of experts which believe in theory known as the "TMJ Triad. What exactly is "TMJ Triad" about? Well, the factors which build this theory are:
- a predisposition, genetic or acquired
- alterations of the bony and soft tissues
- personality line which predispose to a psychological dependence
Several researches done in the past have came to the conclusion that the primary cause of TMJ is dental malocclusion. This is about the improper juxtaposed upper and lower teeth. Logically- the poorly aligned teeth cause displacement of the mandibular condyle. What's next- through chewing and other dental movements - stress and pressure is placed on the soft tissue around the temporomandibular joint. How emotional problems could be the cause of temporomandibular joint syndrome? Although it might sound confusing- the explanation is rather easy! Emotional problems can lead to bruxism and bruxism results when the patient unconsciously develops an uncontrollable clenching and grinding of the teeth. Although people aren’t aware of this fact- it is proven that bruxism can result in severe damage to the teeth, the condyle and muscular balance around the joint. It is also proven that clenching could also be possible cause. Someone who clenches continually things such as chewing gum, a pen or pencil, or fingernails is at risk for developing TMJ syndrome! The constant pounding on the joint causes the pain.
Some experts say that disease called rheumatoid arthritis could also be blamed! Rheumatoid arthritis causes inflammation and, as it progresses, the disease can cause destruction of cartilage and erode bone, deforming joints. It is important to know that chronic rheumatoid arthritis is a inflammatory disorder with a persistent symmetric joint involvement.
Symptoms of temporomandibular joint dysfunction
Identification of TMJ symptoms is crucial because it could easily be misdiagnosed. The most common symptoms include:
- pain in and around the joint
Pain is the most common symptom. Pain is usually localized in and around the joint; however it can be diffused in adjacent areas and even in areas as remote as the back and shoulders. Pain associated with TMJ is usually quite severe and can be the primary cause of attendant headaches.
- crepitus of the joint
Crepitus is the customary popping and clicking experienced in the joint.
- presence of trismus and related difficulties
Trismus often occurs and the TMJ victim experiences spasm in the chewing muscles. This symptom includes difficulties in opening and closing the mouth, with associated pain.
- middle ear disorders
Victims also tend to develop middle ear problems. Tinnitus, dizziness, balance problems and feelings of fullness are directly connected to middle ear.
- headaches
- difficulties in speaking
Other related conditions which can develop include:
- odontalgia
- diplopia
- vertigo
Diagnosis of temporomandibular joint syndrome
Physical:
- Observation
Logically, all possible cases of asymmetry, muscle hypertrophy, malocclusion of jaw, abnormal dental wear, and missing teeth should be evidenced and noted!
- Palpation
Every doctor should know that the this joint is best palpated laterally as a depression just below the zygomatic arch, 1-2 cm anterior to the tragus. While palpating, doctor should feel for muscle spasm, muscle or joint tenderness, and joint sound. Muscles located in this area are masseter, temporalis, medial pterygoid, lateral pterygoid, and sternocleidomastoid.
- Auscultation
A joint movements causing the sounds sound can be auscultated.
Lab Studies:
Blood work is required if systemic illness is suspected to be the cause of TMD.
- CBC is done if infection is suspected.
- Rheumatoid factor (RF), ESR, antinuclear antibody (ANA), and other specific antibodies are checked
- Uric acid should be checked for gout and pseudogout
Imaging Studies:
Patients should know that there is a variety of new imaging techniques are being used and perfected to study TMJ.
- Conventional radiography is the most utilized imaging study. Radiographic findings in TMJ may show erosions, osteophytes, subchondral bony sclerosis…
- Ultrasound allows visualization of the morphological elements and the functions of the TMJ, articular disk, mandibular condyle, and lateral pterygoid muscle
- CT scan can explore both bony structures and muscular soft tissues.
- MRI could also be beneficial in setting the right diagnosis!
Read More: Arthrocentesis - Joint fluid aspiration
Treatment of temporomandibular joint syndrome
Most TMJ disorders are self-limiting and do not get worse. Simple treatment, involving self-care practices, rehabilitation aimed at eliminating muscle spasms, and restoring correct coordination, is all that is required. Nonsteroidal anti-inflammatory analgesics (NSAIDs) should be used on a short-term, regular basis and not on an as needed basis.
Medications
Commonly used medications include NSAIDs, muscle relaxants, and tricyclic antidepressants. More recently, injections of Botulinum toxin have been used, in some cases as an adjunct to arthrocentesis.
- Ibuprofen and naproxen are commonly used NSAIDs.
- Muscle relaxants are diazepam, Methocarbamol, and Cyclobenzaprine
- Tricyclic antidepressants, in low doses, have been used effectively for a long time in chronic painful conditions. Most commonly used are Amitriptyline and Nortriptyline…
- Botulinum toxin is used both as a single treatment
Surgical Care
The treatment of chronic TMD is difficult, and at some time during the course of the disease surgical options are discussed with the patient. Some of the surgical options are:
- Arthrocentesis
Needle is inserted gently in the superior joint space and a small amount of saline is injected to distend the joint space, after which the fluid is withdrawn and evaluated.
- Arthroscopic surgery
Indications include internal derangements, adhesions, fibrosis…
- Open surgery
Open surgery was the main surgical option in the couple of years ago and the most common procedure was disk repositioning and plication;

