A detached retina is a medical emergency. Without a connection to the greater bloodstream, the rods and cones of the retina quickly die. Repairing a detached retina, however, is a tricky operation.
The retina is a thin layer of cells that generate electrical signals when they are activated by light. It lies on top of the choroid, a membrane filled with blood vessels and cells that make the pigments that the retina uses to detect light. The retina may become dislodged, or detached from the retina when:
- A hole in the retina lets the vitreous fluid inside the eyeball leak behind it.
- Inflamed fibers on the surface of the retina cause it to "bunch up" and tear away from the membrane behind it.
- The blood vessels in the retina exude proteins that cause them to twist, turn, and eventually break, leaking blood into the eye, depriving the retina of oxygen and nutrients.
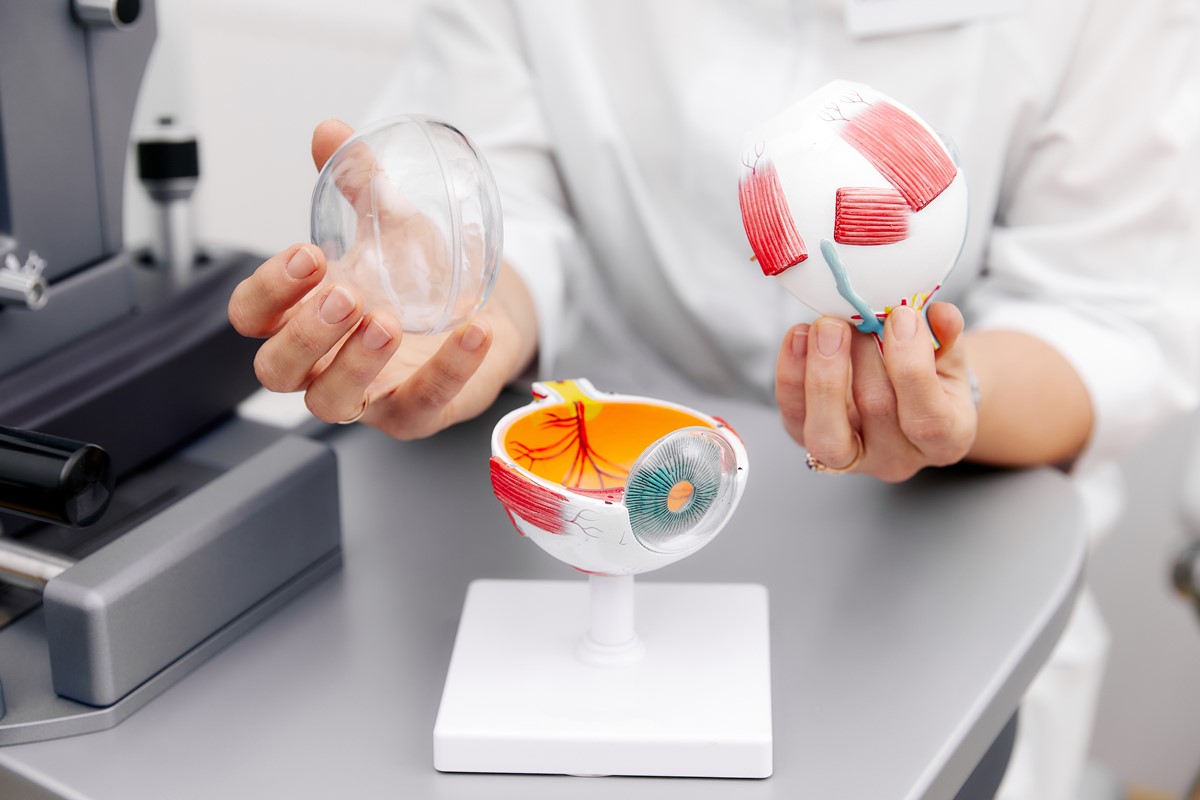
All of these events can occur without detachment of the retina. About 6 percent of the population has holes in the retina that do not interfere with vision. Certain groups of people are more prone to detached retinas than others.
- People who are extremely nearsighted (myopic) are at greater risk of RD. In nearsightedness, the eyeball is elongated, and there is greater stress on the ligaments under the choroid. In this group, RD will most commonly occur between the ages of 25 and 45.
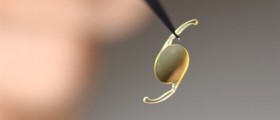
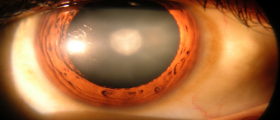
- People who have cataract surgery are more prone to RD, especially if they had removal of the lens without implantation of a new one. Without a replacement lens, the structures in the front of the eye can pull against those behind the retina. Even with a replacement lens, poor wound healing can have a similar effect. In this group, RD most commonly occurs during the first year after cataract surgery.
- Only about 10 to 20 percent of cases of RD result from injury to the eye. These are most common in people under the age of 40.
Retinal detachment is treated with laser or cryotherapy (with a freezing proble) to create a small scar that will reattach it. You may have a permanent blind spot at each site of reattachment, but you could have no vision at all without the treatment. To hold the retina in place while the scar is forming, the surgeon may remove the vitreous fluid in the eye and replace it with a bubble of an oil called sulphahexafluoride (SF6), air, or both. This procedure is known as pneumatic retinopexy.
This process ideally increases pressure inside the eye just enough, usually, to keep the retina in contact with the choroid until scar tissue can make the bond permanent. An air bubble slowly dissipates on its own, while an oil bubble has to be removed in a separate procedure after the scar has healed. This bubble isn't the same density as the eye's naturally occurring fluids. As the eye regenerates vitreous fluid, the bubble will move to the top of the eye, and the boundary between the natural fluid and the injected air or oil will appear wavy.
There are more frequent complications with oil than with air.
The good news about this wavy line is that it will eventually go away even without further surgical intervention. The bad news is that this process can take up to a year.
And when it comes to cataract surgery, many people aren't happy with the results if they are already farsighted. Unless you get a bifocal lens replacement, and most insurance companies in the US aren't going to pay for it, you will find that you can have either great long-distance vision or great up-close vision, but not both. You're like to have to wear glasses for some activities, although there's no doubt that it's better to replace cataracts than not.
- Kierstan Boyd. Retinal Detachment: Torn or Detached Retina Treatment. American Academy of Ophthalmology. http://www.aao.org/eye-health/diseases/detached-torn-retina-treatment. 1 March 2016. Accessed 22 August 2016.
- Photo courtesy of SteadyHealth