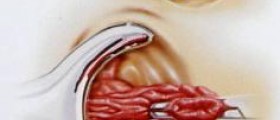
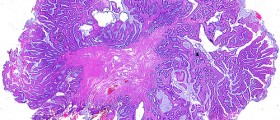
The walls of the veins become enlarged and thin, and are easily irritated when feces are passed. The surgery that is performed to remove these inflamed clusters is known as a hemorrhoidectomy.
Why Is A Hemorrhoidectomy Performed?
A hemorrhoidectomy is performed to relieve the adverse symptoms that accompany hemorrhoids, such as pain, bleeding and anal protrusion of the hemorrhoid. Surgery is chosen particularly after other treatments, which include dietary modifications and certain medications, fail to provide an effective cure.

Other reasons why a hemorrhoidectomy may be the only suitable option include:
- Persistent feeling of heaviness even after emptying the bowels.
- Mucus discharge
- Extremely large internal hemorrhoids.
- Large external hemorrhoids that cause difficulty in cleaning the anal area.
- Both external and internal hemorrhoids that are causing severe discomfort.
Procedure
A hemorrhoidectomy is performed under general anesthesia and is therefore a painless procedure. It may be performed using a scalpel (surgical knife), a cautery pencil (an electric tool) or a laser. Incisions are given with the help of either of these instruments in the tissue surrounding the hemorrhoids. The inflamed veins are tied up to prevent any bleeding, and the hemorrhoids are removed. The operated area may be sutured shut or left open and covered with medicated gauze.
- Stapled Hemorrhoidopexy
This involves removing and closing the hemorrhoidal tissue with the help of a circular stapling device. No incisions are made, and the hemorrhoid is simply lifted and stapled back in place. It is a less painful procedure. However, it is more expensive and most patients need a follow-up surgery.
- Rubber-band Ligation
In this procedure, the base of the hemorrhoid is tied with a rubber band. This cuts off its blood supply and eventually causes the hemorrhoid to shrink and die, and ultimately fall off.
Recovery After Hemorrhoidectomy
Surgery most often completely cures a hemorrhoid. However, maintaing your diet and daily bowel habits play a major role in long-term recovery.
The surgical removal of hemorrhoids has a 95% rate of full recovery and no recurrence. However, rubber band ligation involves a 30 to 50% chance of recurrence within a period of five to 10 years.
Pain is a common symptom that may persist for some time after the surgery. This occurs due to the tightening and relaxation of the anus. You will be given narcotics and analgesics for relief. Moreover, stool softeners should be taken to avoid the formation of very hard stools, so that the need to strain while defecating is avoided. Soaking in warm water may also provide some comfort from the post-surgical pain.
Recovery from a hemorrhoidectomy is mostly uncomplicated, with a high percentage of successful cases and no hemorrhoidal recurrences. Experienced surgeons have reported a less than 5% chance of any post-surgery complication. A complete recovery is usually expected within two weeks, after which the patient can fully resume his daily activities, taking the obvious precautions.
Risks And Complications
A hemorrhoidectomy may involve the following risks and complications:
- Hematoma (collection of blood in the operated area)
- Bowel incontinence
- Infections
- Fecal Impaction
- Stenosis (narrowing of the anal canal)
- Rectal proplapse (rectal lining falls out of the opening of the anus)
- Recurrence