Cerebral or brain aneurysm is a cerebrovascular disorder in which weakness in the wall of a cerebral artery or vein causes a localized dilation or ballooning of the blood vessel. The problem is that some brain aneurysms are large enough to put pressure on the surrounding brain tissue or they can rupture at a weak spot in the artery wall, causing a massive bleeding in that specific area of the brain.
People of all ages can have a brain aneurysm, but they mostly develop as a result of the aging process. They are usually discovered in people ages 35 to 60. Women are slightly more likely to develop an aneurysm than men.
Types of aneurysms
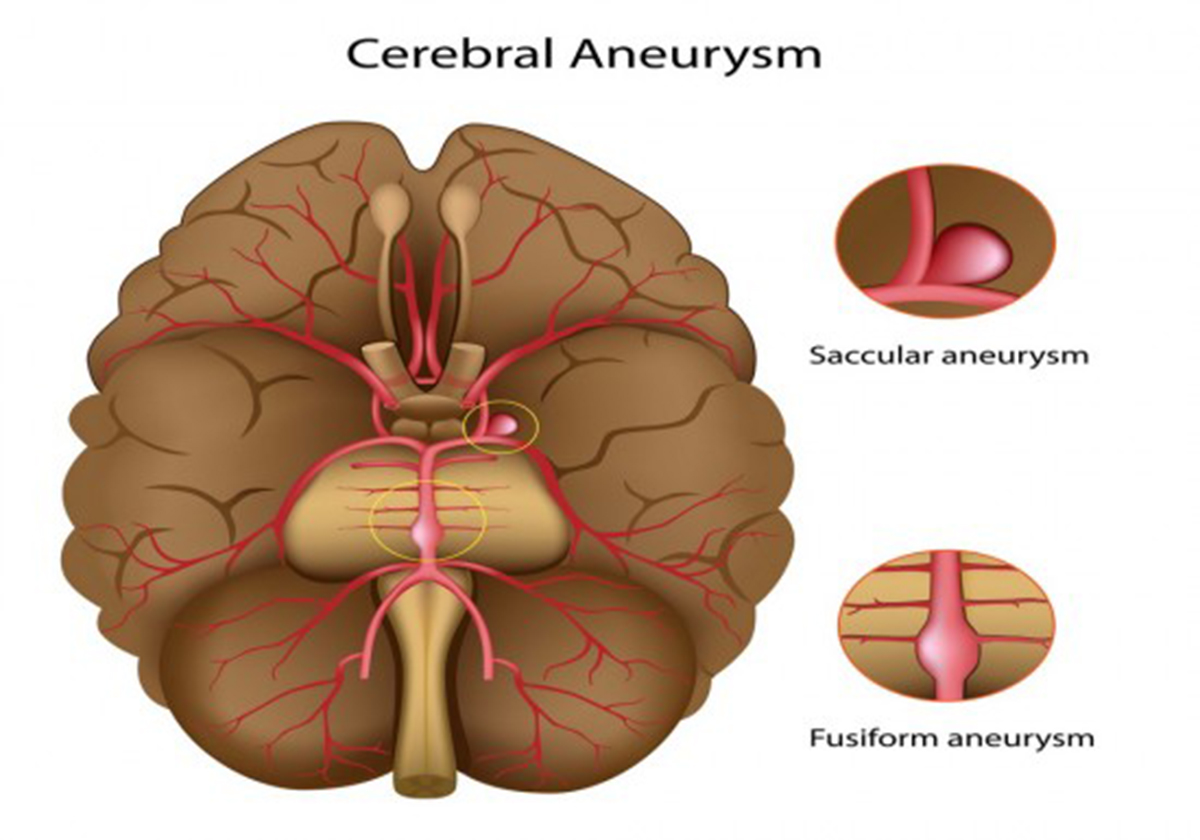
There are three types of cerebral aneurysm.
A saccular aneurysm is a rounded or a pouch-like sac of blood that is attached by a neck or stem to an artery or a branch of a blood vessel. It is also known as a berry aneurysm because it resembles a berry. This is the most common form of cerebral aneurysm and is typically found on arteries at the base of the brain.
Saccular aneurysms most often occur in adults. A lateral, or dissecting aneurysm appears as a bulge on one wall of the blood vessel, while a fusiform aneurysm is formed by the widening along all walls of the vessel.
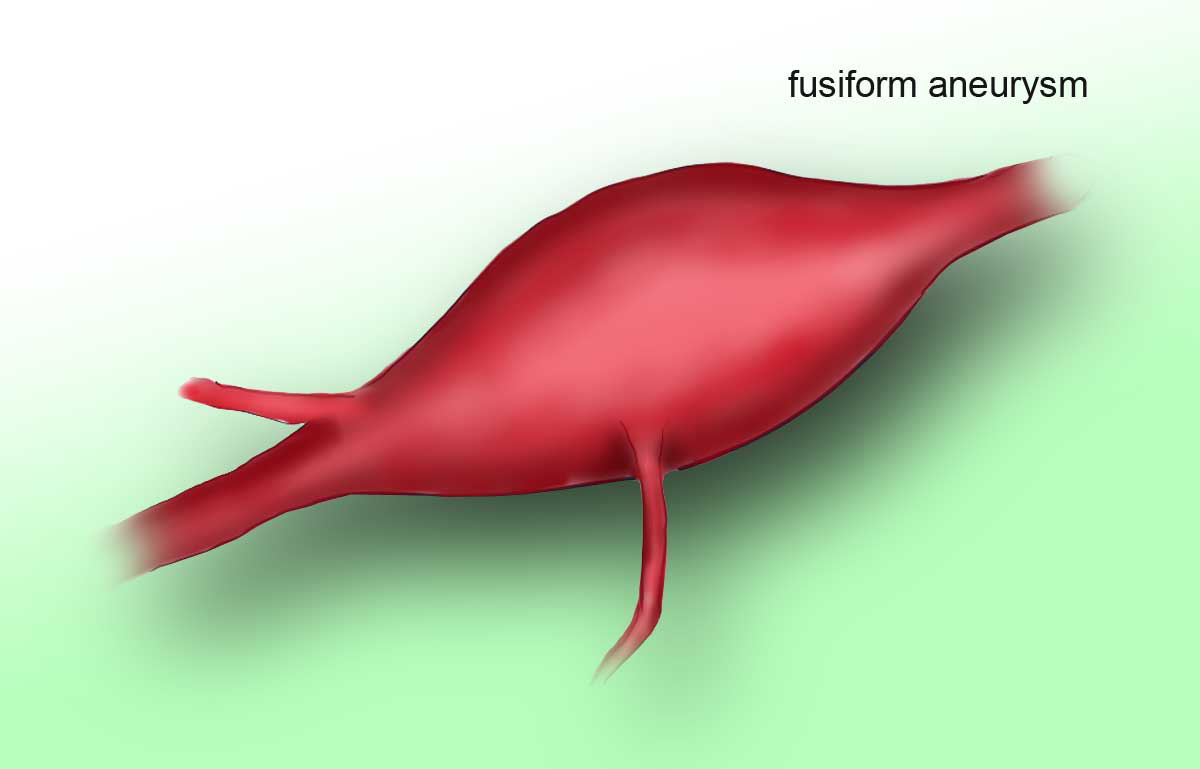
Incidence and risk factors
All cerebral aneurysms have the potential to rupture and cause bleeding within the brain.
The incidence of reported ruptured aneurysm is about 10 in every 100,000 persons per year which means about 27,000 patients per year in the U.S, most of them being between ages 30 and 60.
There are a few factors which are clearly associated with an increased risk of rupture:
- Gender – As we already stated, females are more likely to develop an aneurysm
- Hypertension
- Smoking
- Alcohol abuse,
- Drug abuse
Symptoms of brain aneurysm
Most cerebral aneurysms do not show symptoms until they either become very large or burst. As the aneurysm gets bigger, it may start pressing on the surrounding tissue and nerves.
The symptoms may include:
- pain above and behind the eye
- numbness
- weakness, or paralysis on one side of the face
- dilated pupils
- vision changes
When an aneurysm hemorrhages, patient may experience:
- a sudden and extremely severe headache
- double vision
- nausea
- vomiting
- stiff neck, and
- a loss of consciousness
Other signs that a cerebral aneurysm has burst include:
- nausea and vomiting associated with a severe headache
- a drooping eyelid
- sensitivity to light, and
- a change in mental status or level of awareness
Possible causes
Most brain aneurysms develop as a result of the wear and tear on arteries that comes with aging. Several researches proved that brain aneurysms aren't present at birth (congenital), as it was once commonly believed. However, some people may have a predisposition to developing an aneurysm. Cerebral aneurysms are also more common in people with certain genetic diseases, such as connective tissue disorders and polycystic kidney disease, and certain circulatory disorders, such as arteriovenous malformations.
Sometimes a blow to your head or an infection in an artery can weaken an artery wall and result in an aneurysm. Other causes include:
- high blood pressure
- tumors
- atherosclerosis and other diseases of the vascular system
- cigarette smoking, and
- drug abuse
Some experts believe that the oral contraceptives may also increase the risk of developing aneurysms.
Associated conditions
Conditions that have been associated with the increased incidence of cerebral aneurysms are:
- Anomalous vessels
- Coarctation of the aorta
- Polycystic kidney disease
- FMD
- Connective tissue disorders such as Marfan, Ehlers-Danlos syndrome and others…
- High-flow states such as vascular malformations, fistulae…
- Spontaneous dissections
Localization of aneurysms
It is proven that aneurysms commonly arise at the bifurcations of the major arteries. Most of the aneurysms arise on the circle of Willis, located on the brain base.
Anterior circulation aneurysms
Approximately 85% of all intracranial aneurysms arise on the anterior or carotid circulation. Common locations are:
- The anterior communicating artery (30-35%),
- The internal carotid artery at the posterior communicating artery origin (30-35%), and
- The MCA bifurcation (20%).
Posterior circulation aneurysms
About 15% of all intracranial aneurysms arise on the posterior or vertebrobasilar circulation.
Miscellaneous locations
Saccular aneurysms are uncommon in locations other than the circle of Willis, the MCA bifurcation, or the pericallosal artery origin.
Subarachnoid hemorrhage
The Subarachnoid hemorrhage or bleeding is the most common clinical manifestation of the brain aneurysm. The most widely used clinical method for grading the clinical severity of SAH is the Hunt and Hess scale. The grades are:
- Grade 0 - Unruptured aneurysm
- Grade 1 - Asymptomatic or minimal headache and slight nuchal rigidity
- Grade 1A - No acute meningeal or brain reaction but with fixed neurological deficit
- Grade 2 - Moderate-to-severe headache, nuchal rigidity, no neurological deficit other than cranial nerve palsy
- Grade 3 - Drowsiness, confusion, or mild focal deficit
- Grade 4 - Stupor, moderate-to-severe hemiparesis, possible early decerebrate rigidity, and vegetative disturbances
- Grade 5 - Deep coma, decerebrate rigidity, and moribund appearance
Screening and diagnosis
There is a great chance that the aneurysm will go undetected, especially, if it didn’t rupture. However, after an aneurysm has ruptured, there are a number of ways to confirm the diagnosis. Besides a physical a neurological exam which includes checking memory and concentration, vision, hearing, balance, coordination and reflexes may be performed. Other tests include:
Computerized tomography (CT).
A head CT scan can reveal the presence of a suspected aneurysm and show whether blood has leaked from the artery into brain. Similar to an X-ray, a CT scan shows a more detailed image of the brain than a conventional X-ray because it uses the computer based reconstructions. Some scans involve the use of a contrast dye injected into the vein. Known as CT angiography, this test produces an even more detailed image.
Magnetic resonance imaging (MRI).
This is probably the best possible diagnostic tool for the detection of aneurysms. This type of imaging uses a magnetic field and radio waves to create detailed, cross-sectional images of brain. When this diagnostic test involves the use of a contrast, it's known as magnetic resonance angiography.
Cerebral arteriogram.
During this invasive procedure, a doctor inserts a thin, flexible tube called catheter into a large artery usually located in the groin region and then guides it. The catheter passes your heart and enters the cerebral arteries in your brain. A cerebral arteriogram provides a clear picture of the arterial blood flow in your head.
Cerebrospinal fluid analysis.
This procedure, also known as a spinal tap, involves the use of a needle to extract a small amount of the fluid that protects your brain and spinal cord called liquor. Analysis of the fluid can detect brain hemorrhage very easily because in the presence of a hemorrhage it should be red. In patients with a suspected subarachnoid hemorrhage, this procedure is usually done in a hospital.
Possible complications of brain aneurysms
A brain aneurysm that bursts can cause
- a stroke,
- a permanent nerve damage or
- death.
A ruptured aneurysm on the surface of the brain causes a subarachnoid hemorrhage - bleeding into the space between your brain and your skull. Other possible complications include:
- Fluid buildup in the brain (hydrocephalus)
- Narrowing of the arteries (vasospasm), which can lead to a lack of blood flow to the parts of the brain (ischemic stroke)
Treatment of brain aneurysms
Two surgical options are available for treating cerebral aneurysms, both of which carry some risk for the patient.
Micro-vascular clipping
It is one of the most effective methods and it involves cutting off the flow of blood to the aneurysm. The neurosurgeon isolates the blood vessel that feeds the aneurysm and places a small, metal clip on the aneurysm, halting its blood supply. Clipping proved to be highly effective, depending on the location, shape, and size of the aneurysm. In general, it is proven that aneurysms that are completely clipped surgically do not return.
Occlusion
During this procedure the surgeon clamps off the entire artery that leads to the aneurysm.
This procedure is often performed when the aneurysm has damaged the artery. An occlusion is sometimes accompanied by a bypass.
Endovascular embolization
Endovascular embolization is an alternative to surgery. It is done by inserting a catheter into an artery and guiding it, through the body to the site of the aneurysm. Using a guide wire, detachable coils or small latex balloons are passed through the catheter and released into the aneurysm. The coils or balloons fill the aneurysm, block it from circulation, and cause the blood to clot, which effectively destroys the aneurysm.
Prevention
There are no known ways to prevent a cerebral aneurysm from forming. However, people with a diagnosed brain aneurysm should carefully control high blood pressure, stop smoking, and avoid cocaine or other stimulant drugs use. Women should consult with their doctors on the use of oral contraceptives.
- en.wikipedia.org/wiki/Brain_Aneurysm
- www.mayoclinic.com
- www.ninds.nih.gov

