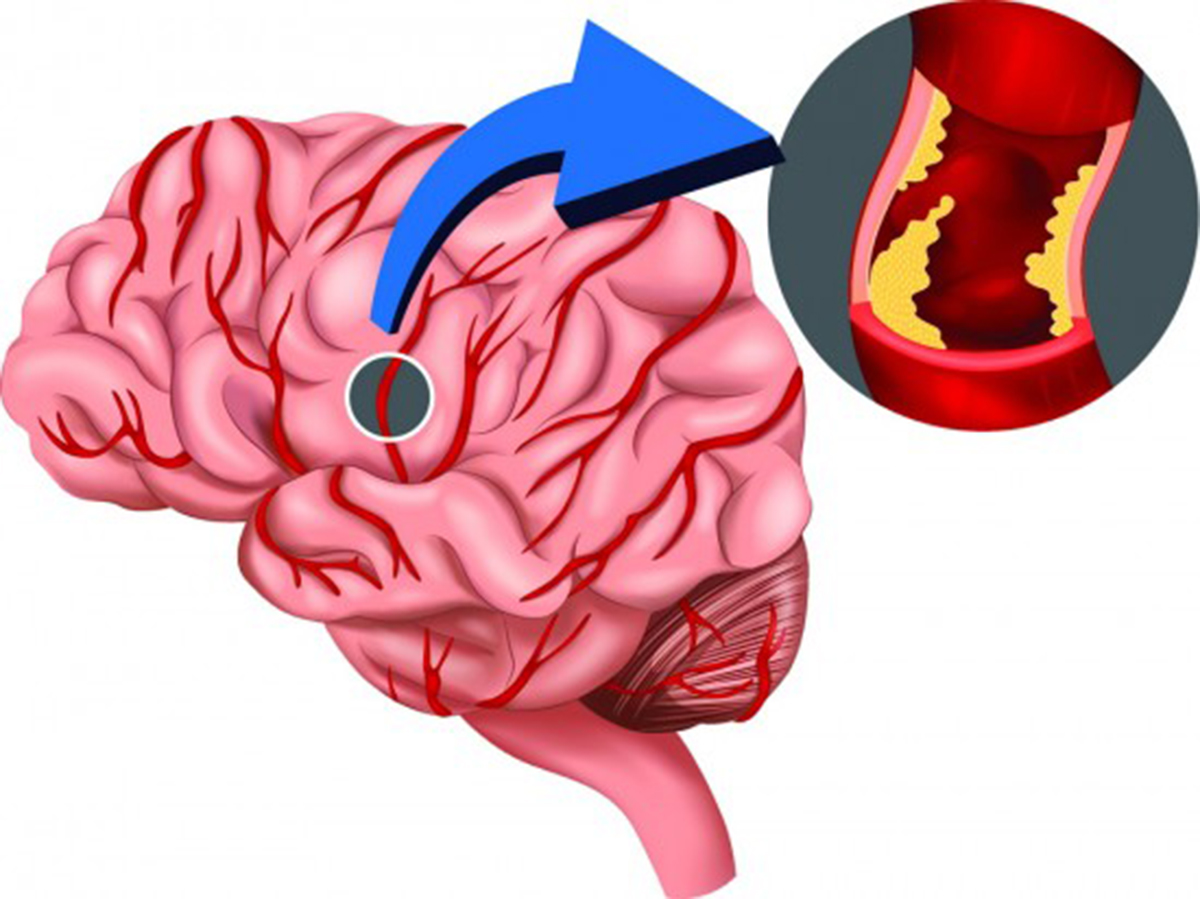
It occurs when a thrombus (blood clot) blocks a blood vessel in the brain, causing ischemia, necrosis, and death. There are several possible complications associated with stroke, such as paralysis, vision problems, behavioral changes, memory loss, and many other.
The best possible way to prevent or to reduce the risk of stroke is to use medications that destroy blood clots before they cut off of the vessel wall and start circulating. Thrombolytic therapy is of proven benefit for selected patients with ischemic stroke. Can all stroke patient use thrombolytic therapy, and are there any possible side effects? What are the most commonly used thrombolytics?
Thrombosis
Thrombosis is the formation of a blood clot (thrombus) inside a blood vessel. The most serious complication of thrombosis is obstructing the flow of blood through the circulatory system. This complication is also called embolisation, and therefore the whole process is called thrombo-embolism. A clinical rule known as Virchow's triad states that thrombosis is caused by one of these three abnormalities:
- Blood composition
- Quality of vessel wall
- Nature of blood flow
The formation of a thrombus is usually caused by an injury to the vessel's wall, by either trauma or infection. A slowing or stagnation of blood has also been known to induce thrombosis .
Types of thrombosis
There are two general types of thrombosis, and they are:
1. Venous thrombosis
- Deep venous thrombosis
- Portal vein thrombosis
- Renal vein thrombosis
- hepatic vein thrombosis
- upper extremity vein thrombosis
- Subclavian vein thrombosis
2. Arterial thrombosis
- Myocardial infarction
- Stroke
- Thoracic outlet syndrome
Types of stroke
Generally, strokes can be classified into two major types:
- Ischemic –caused by thrombosis, embolism, or systemic hypoperfusion
- Hemorrhagic –caused by intra-cerebral hemorrhage, subarachnoid hemorrhage, subdural hemorrhage, or epidural hemorrhage
Ischemic stroke: Ischemicis the most common type of stroke. Studies have shown that it is the cause of approximately 80% of all strokes. Although there are several different types of ischemic stroke, the mechanism is simple; a blood vessel becomes occluded and the blood supply to a part of the brain is totally or partially blocked.
Hemorrhagic stroke: During a hemorrhagic stroke, a blood vessel in the brain ruptures or bleeds, unlike with the ischemic type.The consequence is almost the same – it interrupts the brain's blood supply because the bleeding vessel can no longer carry the blood to its target tissue. Also, there is one more complication: the blood released from the vessel irritates brain tissue, causing additional symptoms. This is why hemorrhagic strokes are considered to be more dangerous than the ischemic type.
Stroke treatment
Because of different mechanisms of strokes, the treatments can be different:
1. Ischemic Stroke
The best possible acute treatment is a FDA-approved clot-busting drug called tPA. This medication should be administered within three hours from the onset of symptoms.
As far as preventative treatment is concerned, simple antiplatelet agents such as Aspirin, and anticoagulants such as warfarin are probably the best option. They work by interfering with the blood's ability to clot, and can play an important role in preventing stroke. There is also a procedure called carotid endarterectomy, during which blood vessel blockage is surgically removed from the carotid artery. And of course, there are always stents – steel screens implanted into the vessel to remove the blockage.
2. Hemorrhagic Stroke
For hemorrhagic stroke, probably the best option is surgery, either placing a metal clip at the neck of the aneurysm, or removing the abnormal vessels. Sometimes endovascular procedures could also be used. (They are less invasive then other methods.) They involve using a catheter introduced through a major artery into the leg or arm.
Stroke symptoms
The symptoms of a stroke depend primarily on which part of the brain is affected. However, there are symptoms found in most stroke cases, such as:
- muscle weakness affecting one, two or all extremities
- numbness
- reduction in sensory or vibratory sensation
When the cranial nerves are affected, the most common symptoms are:
- altered sense of smell, taste, hearing, or vision
- drooping eyelid
- decreased reflexes
- decreased sensation of the face
- balance problems
- altered breathing and heart rate
When should stroke patients receive thrombolytics?
Thrombolytic therapy has its own strict indications – it should be limited to patients with acute ischemic. Only these patients should use it and only these patients can benefit from it. They have shown improved combined mortality and disability outcomes when treated with thrombolytics. On the other hand, studies have shown that treating patients with tPA outside these strict indications in fact increases morbidity and mortality.
Some of the most effective and most commonly used thrombolytics are:
- Activase (alteplase - tissue-type plasminogen activator, or t-PA)
- Eminase (anistreplase)
- Retavase (reteplase)
- Streptase (streptokinase)
- TNKase (tenecteplase)
- Abbokinase (urokinase)
Streptokinase: An enzyme produced by beta-haemolytic streptococcus, streptokinase is used as an effective and cheap clot-dissolving medication in some cases of myocardial infarction (heart attack) and pulmonary embolism. It works by activating plasminogen through cleavage to produce plasmin.
Urokinase: An enzyme also called urokinase-type Plasminogen Activator! It represents one blood enzyme, serine protease, originally isolated from human urine. The primary physiological target substance is plasminogen. Activation of plasminogen into the plasmin in fact triggers a natural body proteolysis cascade, which is the best possible way to resolve a blood clot.
Tissue plasminogen activator: Similarly to Urokinase, this enzyme converts plasminogen to plasmin, a fibrinolytic enzyme.
Reteplase: Also known as Retavase, this thrombolytic drug can effectively brake blood clots. Chemically, it is a recombinant non-glycosylated form of human tissue plasminogen activator (see above) produced in the bacterium Escherichia coli. Reteplase can penetrate inside the big thrombi, and help resolve those hidden places on thrombi that couldn’t be reached with other medications!
Tenecteplase: Like the previous medications, Tenecteplase is also an enzyme used as a thrombolytic drug, a tissue plasminogen activator (tPA) produced by recombinant DNA technology using an established mammalian cell line. Recent studies have shown that Tenecteplase is one of the most effective thrombolytics in the treatment of heart attack, especially if it is used soon after the attack.


Your thoughts on this