Research studies were trying to determine whether use of general anesthesia for heroin detoxification is better then other methods of detoxification. It turned out it wasn’t better but only more expensive and could, however, lead to adverse life threatening events.
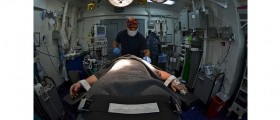
Anesthesia-assisted opioid detoxification involves administering an opioid antagonist drug to neutralize the effects of heroin while the patient is unconscious from general anesthesia. It was supposed to be a fast, painless way to withdraw from heroin. However, this treatment is expensive, not covered by insurance, and lacks good evidence to support efficacy. There are also significant concerns about health risks.
However, medically supervised heroin withdrawal is still plagued by patient discomfort and high dropout rates.
Researchers from Columbia Universityhad conducted a randomized controlled trial between 2000 and 2003 to evaluate the safety, tolerability, and efficacy of anesthesia-assisted rapid opioid detoxification. The trial showed that only 11 percent of patients continued in treatment for 12 weeks and had less than two opioid-positive urine tests, indicating a high rate of relapse to heroin use. The anesthesia procedure was associated with 3 potentially life-threatening adverse events: severe pulmonary edema and aspiration pneumonia, diabetic ketoacidosis, and a bipolar mixed state requiring hospitalization.
Researchers feel that the study demonstrates no benefit of anesthesia over a safer, cheaper, and potentially outpatient alternative using buprenorphine as a bridge to naltrexone treatment.
Anesthesia-assisted opioid detoxification involves administering an opioid antagonist drug to neutralize the effects of heroin while the patient is unconscious from general anesthesia. It was supposed to be a fast, painless way to withdraw from heroin. However, this treatment is expensive, not covered by insurance, and lacks good evidence to support efficacy. There are also significant concerns about health risks.
However, medically supervised heroin withdrawal is still plagued by patient discomfort and high dropout rates.
Researchers from Columbia Universityhad conducted a randomized controlled trial between 2000 and 2003 to evaluate the safety, tolerability, and efficacy of anesthesia-assisted rapid opioid detoxification. The trial showed that only 11 percent of patients continued in treatment for 12 weeks and had less than two opioid-positive urine tests, indicating a high rate of relapse to heroin use. The anesthesia procedure was associated with 3 potentially life-threatening adverse events: severe pulmonary edema and aspiration pneumonia, diabetic ketoacidosis, and a bipolar mixed state requiring hospitalization.
Researchers feel that the study demonstrates no benefit of anesthesia over a safer, cheaper, and potentially outpatient alternative using buprenorphine as a bridge to naltrexone treatment.
Loading...