"Super-bug" - MRSA or methycillin-resistant Staphylococcus aureus
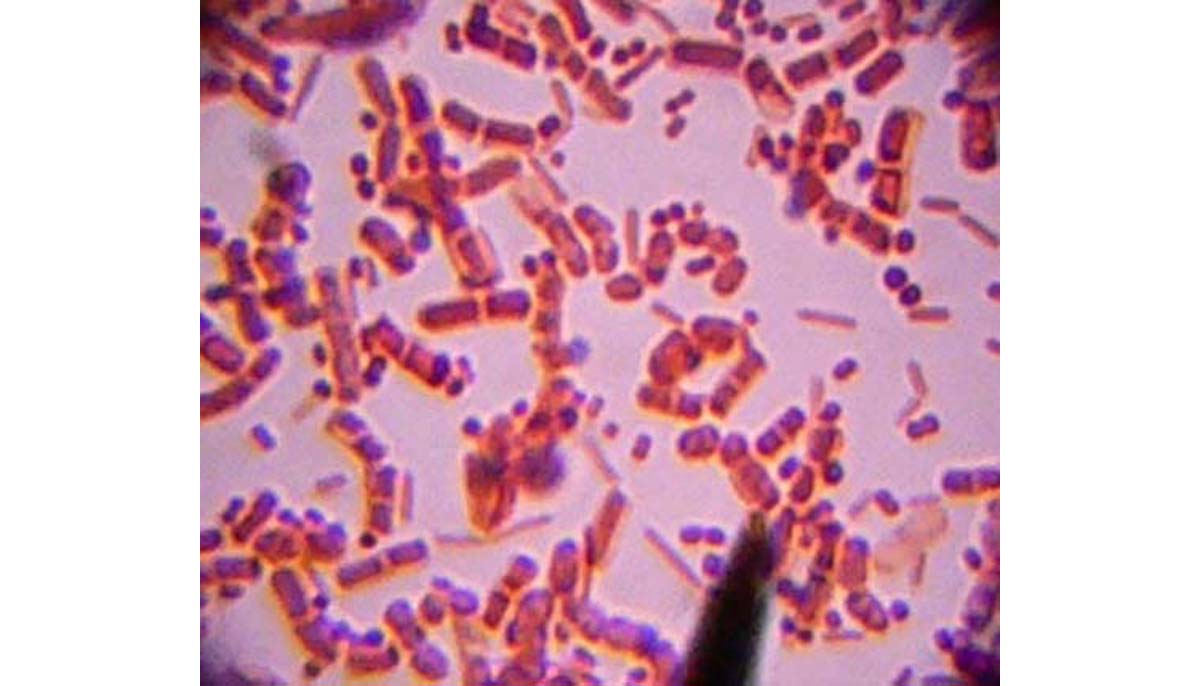
Just as doctors are about to get the MRSA epidemic under control, however, a new super-bug is taking its place. This bacterium is known as Clostridium difficile. It infects one in five people admitted to the hospital, over 3,000,000 people every year just in the USA. And one in four people who develops symptoms dies of the infection.
Clostridium difficile: From Everyday Bug to Superbug
Clostridium has always been a difficult bacterium to treat. A hundred years ago, this bacterium was a dreaded source of post-surgical infection, especially after appendectomies.
The Clostridium bacterium normally lives in the human colon. About 2 to 5 per cent of all the bacteria in a healthy colon can be Clostridium. Up to 50 per cent of healthy people have this bacterium in the gut. The bugs are kept in check by the symbiotic or healthy bacteria that also live there, such as Lactobacillus. When something kills off the healthy bacteria, however, Clostridium is free to multiply.
This normally harmless bacterium can cause devastation in the lining of the colon. It releases toxins that can cause bloating, constipation, diarrhea, and abdominal pain. When the toxins get into bloodstream circulation, they can cause flu-like symptoms.
In the old days of abdominal surgery, the problem that precipitated overgrowth by Clostridium was simple sanitation. Surgical instruments used on the last patient that were not thoroughly cleaned could introduce so many new bacteria to the next patient that an untreatable infection resulted. An excruciating death from peritonitis was a frequent complication of even simple abdominal surgery, such as removing an appendix.
Nowadays, surgical instruments are usually clean, but hospital floors are not. The longer a person has to stay in the hospital, the more likely he or she is to be infected. People at greatest risk for Clostridium infection are those who have to go to the hospital the most frequently. These include people with cancer, pregnant women experiencing complications, burn victims, people in the intensive care unit (ICU), and people who have cancer.
The bacterium can be transmitted by anything that touches a bedpan, urinal, or the floor, and from the hands of hospital care personnel. The Clostridium bacterium can live for up to 5 months on a clean floor. The bacteria are usually deposited there with feces and stay on the surface despite repeated cleaning.
Antibiotics for Clostridium difficile Overgrowth: Both Cause and Cure
In the modern era, antibiotic treatment is usually what caused Clostridium infections. Antibiotics kill the friendly symbiotic bacteria. Sometimes all that is needed to stop Clostridium is to stop the antibiotics.
If the Clostridium is an antibiotic-resistant strain, however, stopping antibiotics has no effect—and traditional antibiotics have little effect, either. Symptoms of Clostridium poisoning may not start until 3 or 4 weeks after the patient is discharged from the hospital and after antibiotics have been discontinued.
Certain antibiotics are more likely to cause problems with Clostridium than others. The most common triggers for Clostridium infection are:
- Amoxicillin,
- Ampicillin, and/or
- Clindamycin.
Even a single dose of the drugs is enough to kill the bacteria that keep the superbug in check. Erythromycin, azithromycin, clarithromycin, and penicillin are also problematic.
The first sign is usually green, putrid diarrhea. The infection can release toxins that paralyze the colon so that diarrhea stops and the abdomen becomes swollen. There can be fever up to 105º F (40.5º C), and there can be bleeding as the lining of the colon is dissolved.
What Makes this Superbug Super
When doctors talk about the superbug form of Clostridium difficile, they are referring to infections that do not respond to either metronidazole or vancomycin. In some cases, the superbug quickly causes low blood pressure, kidney failure, and anasarca, accumulation of fluid in all the cavities of the body. Sometimes the toxins paralyze the colon so that there is no diarrhea, and the condition is much harder to diagnose.
What Doctors Can Do About "Refractory" Clostridium Infections
The first concern in managing any severe intestinal infection of this kind is preventing dehydration. Patients will have to be admitted to the hospital where they can be given intravenous fluids with needed electrolytes. People who have serious Clostridium infections are never given anything to stop diarrhea, since diarrhea is one way the body gets rid of the infection.
The best way of describing a typical course of treatment for Clostridium is "giving you everything they've got." The doctor will probably try giving pulses of metronidazole and vancomycin. There may be treatment with Bacitracin and teicoplanin, which are newer antibiotics. If there is diarrhea, the doctor may prescribe cholestyramine, a sticky agent that traps the bacteria inside (but which cannot be given if there is no bowel movement). And there may injections of intravenous immunoglobulins to try to bolster the immune system.
Read More: MRSA - Methicillin Resistant Staphylococcus Aureus Fact sheet
Preventing Clostridium difficile Infections
Once you have a severe Clostridium infection, you will need a doctor's help, in the hospital, just to survive. There are things you can do, however, that reduce your risk of infection.
There is a strain of yeast usually sold to brewers and bakeries known as Saccharomyces boulardii. In a health food store it might just be labeled Sb. This yeast interferes with the release of toxins by Clostridium.
Often Sb alone is enough to stop the diarrhea and abdominal pain that come after the use of antibiotics. And one clinical study found that it reduced the risk of developing diarrhea in the hospital by more than 60 per cent.
Sb is not found in any of the probiotic yogurts you can find in the market. It is not in Yoplait Plus or Dan-Active. You will probably have to take Sb capsules, which you can buy at a health products store. Just be sure to inform your physician of what you are doing so he or she can coordinate your treatment with your probiotic consumption.
- Bleichner G, Bléhaut H, Mentec H, Moyse D. Saccharomyces boulardii prevents diarrhea in critically ill tube-fed patients. A multicenter, randomized, double-blind placebo-controlled trial. Intensive Care Med. 1997 May.23(5):517-23.
- de Lalla F, Nicolin R, Rinaldi E, Scarpellini P, Rigoli R, Manfrin V, et al. Prospective study of oral teicoplanin versus oral vancomycin for therapy of pseudomembranous colitis and Clostridium difficile-associated diarrhea. Antimicrob Agents Chemother. Oct 1992.36(10):2192-6.
- Greenstein AJ, Byrn JC, Zhang LP, et al. Risk factors for the development of fulminant Clostridium difficile colitis. Surgery. May 2008.143(5):623-9.
- Grundfest-Broniatowski S, Quader M, Alexander F, et al. Clostridium difficile colitis in the critically ill. Dis Colon Rectum. Jun 1996.39(6):619-23.
- Indra A, Lassnig H, Baliko N, et al. Clostridium difficile: a new zoonotic agent?. Wien Klin Wochenschr. Feb 2009.121(3-4):91-95.
- Juang P, Skledar SJ, Zgheib NK, et al. Clinical outcomes of intravenous immune globulin in severe clostridium difficile-associated diarrhea. Am J Infect Control. Mar 2007.35(2):131-7.
- McFarland LV. Antibiotic-associated diarrhea: epidemiology, trends and treatment. Future Microbiol. Oct 2008.3:563-78.

