Depending on the material that you read, there are a few different scales that exist to describe the progression of Alzheimer’s Disease. What is generally accepted in medicine is the 3-stage model of this disease. Each stage breaks the disease up into different symptoms and gives a rough estimate of how long each phase should last. Here, we will cover what are the symptoms to watch out for with each of the separate stages and what steps you can take to try to avoid progressing into the more severe stages.
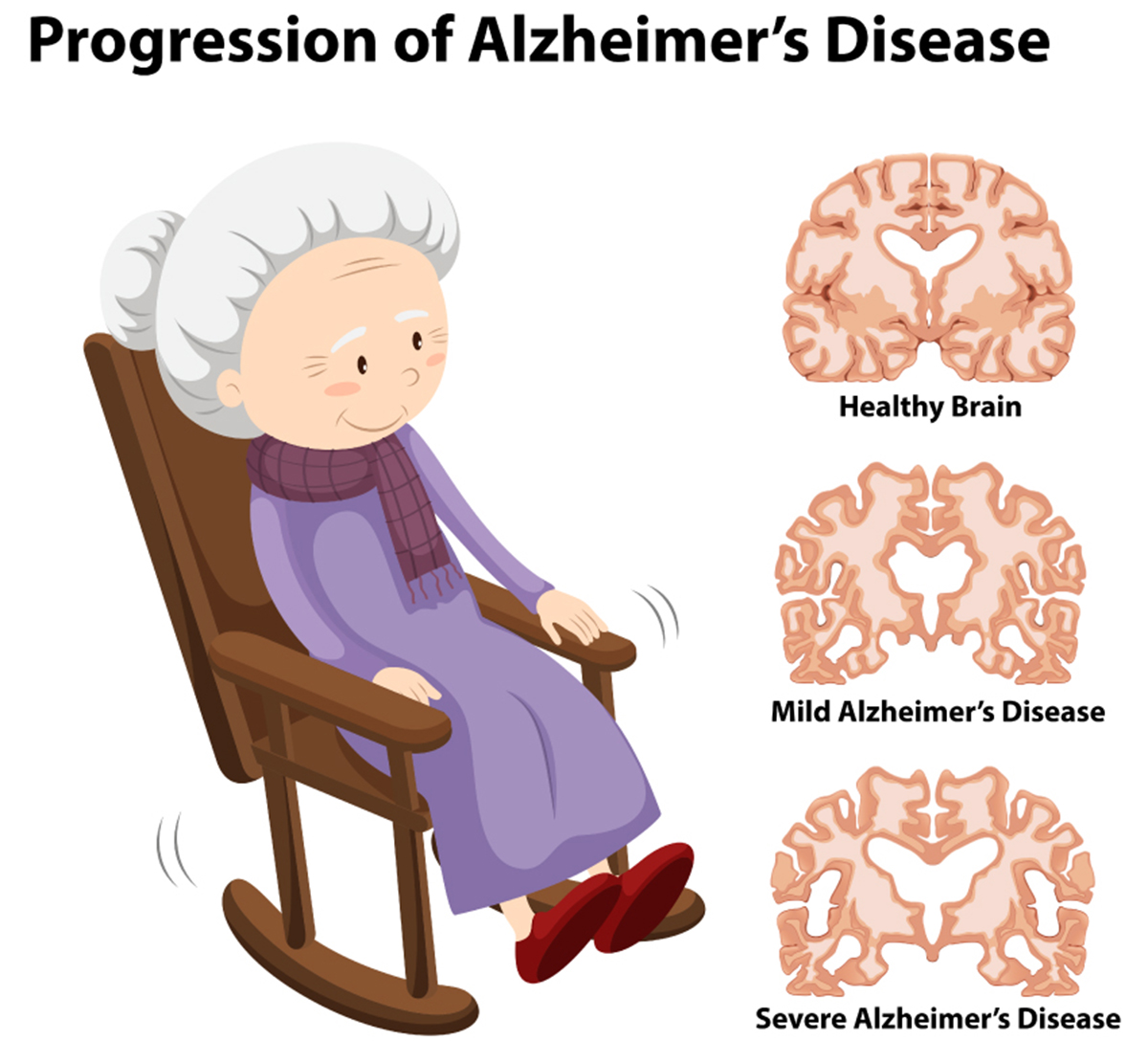
Stage 1: Mild cognitive impairment
This just means that you are not as mentally sharp as you once were but this is a very subjective kind of feeling. As most doctors have only a few minutes of time to interact with patients they may be meeting for this first time, it is something that can be quite hard to diagnose without the testimony of family and friends who have a better idea of what you are like normally.
This stage will typically last around 7 years.
During this phase, patients are likely to have only a slight memory decline. If you are stressed out from work, without sleep or may even have just forgotten your morning cup of coffee, there is a good chance that you can fall into this category already without having AD so do not be too worried if you find yourself more forgetful than usual at times.
What you can do to stop this
A detailed family history of possible cases of AD is the best bet to have an early diagnosis of the disease. If you think that you may be having a harder time than normal trying to remember simple things, ask your partner to record things that seem difficult and visit with a neurologist in order to begin therapy for the disease.
The goal of therapy at this stage is to diagnose the disease as early as possible.
Stage 2: Mild Alzheimer’s disease
By this stage, it is becoming more obvious to doctors that there is a pathological process that is occurring. Stage 2 is a period that typically lasts 2 years on average and marked with more noticeable declines in everyday tasks that were once simple for you.
For example, parts of your brain that help with reading and object recognition are mostly influenced in this stage. As a result, symptoms will manifest like substantial reading difficulty, inability to recognize and name common objects, navigation may become problematic.
Often the case, these patients are brought into the ER Departments by ambulance due to wandering around the streets trying to find their way home. A simple trip to the grocery store can become quite stressful for not only the patient but also the family as they worry about where their loved one has gone.
What you can do to stop this
By the time memory impairment begins to set in, you need to begin medical therapy in order to help improve the quality of life. There are medications like memantine (Originally, Axura, Ebixa, Namenda and other brand names) or donepezil (Aricept) that are on the market that can help with memory problems associated with AD. This will be a temporary fix but can dramatically prolong the number of quality life years in a patient suffering from AD.
Stage 3: Moderate Alzheimer’s disease
As we approach this stage, symptoms will only become more severe. Patients will now have problems with the front part of their brains so it will be hard for them to make good decisions. The front part of our brains is responsible for judgment and attention. Patients at this stage of the disease will have a noticeably different personality and it will be hard to help them focus their attention.
This stage also lasts about 2 years before progressing further.
How to help cope with this stage
At this stage, there are still medications that can help improve some of the symptomatic complaints of the patient but it will be harder with the behavioral changes that are associated with this stage. This is a stage where family and friends can help benefit the patient the most. Understand that the behavioral changes are part of the scope of the disease and be patient with the fits of aggression that could manifest with this stage. Meeting with a psychologist can help teach you strategies or techniques that can help reduce the changes in behavior and provide support when your partner may be hard to manage.
Stage 4: Severe Alzheimer’s disease
When it comes to stage 4, most patients do not survive until this stage so most medical centers will group moderate and severe Alzheimer’s Disease together, hence the 3-stage model. There are some slight differences in these two conditions so it is important to be aware of symptoms at this stage as well. By this stage, the disease has spread to the last part of the brain that had not yet been affected, the occipital lobe. This portion of the brain is responsible for vision so visual acuity will be dramatically reduced by this stage. This stage lasts about 3 years in most patients who reach this phase of the disease.
How to cope with this stage
This is considered to be the terminal stage of AD so patients will not have a dramatic improvement.
As of now, there is still no cure for AD so the only help you can provide is support and comfort. Sometimes, that can be even more meaningful for the patient and family than medications.


Your thoughts on this