Vasculitis is a general term for a group of uncommon diseases that feature inflammation of the blood vessels. The blood vessels of the body are referred to as the vascular system.
The blood vessels are composed of arteries that pass oxygen-rich blood to the tissues of the body and veins which return oxygen-depleted blood from the tissues to the lungs for oxygen. Vasculitis is a medical condition that is characterized by inflammation in and damage to the walls of various blood vessels.
Each of the members of the broader vasculitis "family" are defined by certain patterns of distribution of blood vessel involvement, particular organ involvement, and laboratory test abnormalities.
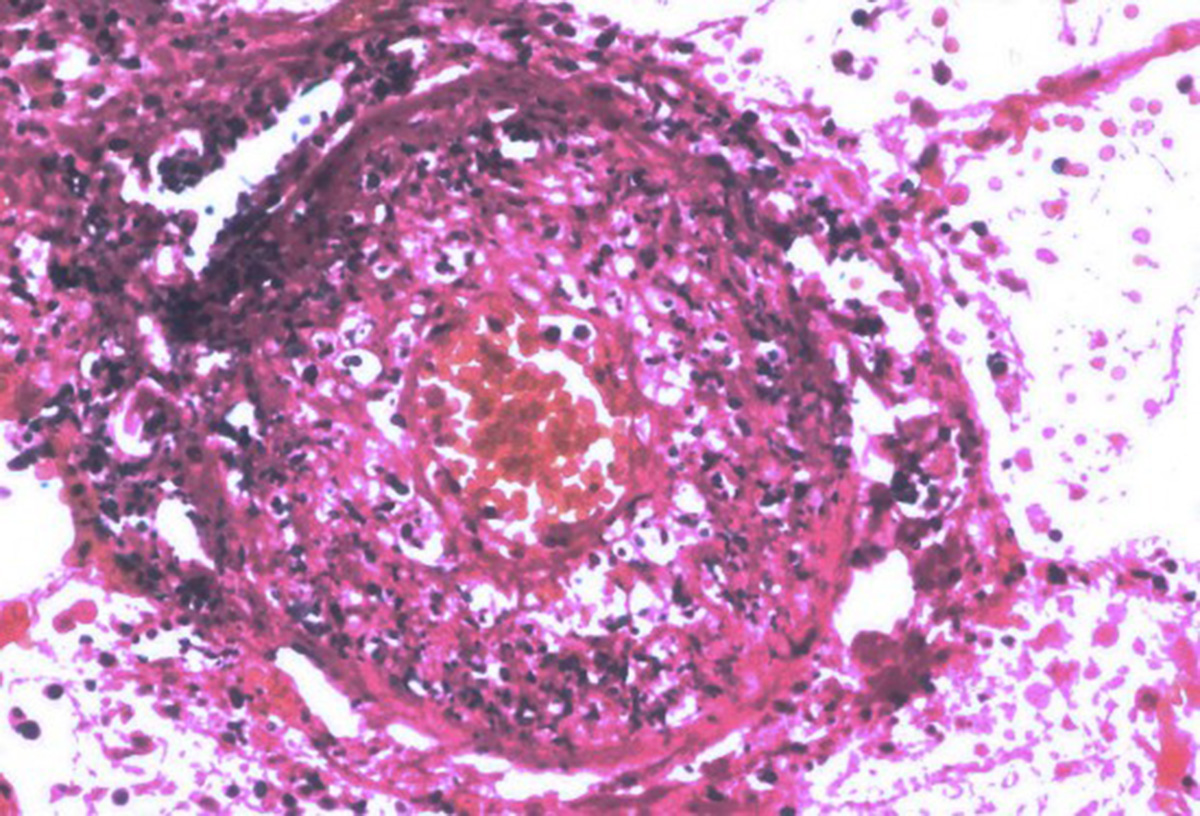
The word vasculitis is derived from the Latin "vasculum", meaning vessel and the suffix "- itis", which means inflammation. Another term for vasculitis is angiitis. When the arteries are the inflamed blood vessels, the condition is also referred to as arteritis. When the veins are inflamed, it is referred to as venulitis. There are many types of vasculitis, and vasculitis can affect people of all ages. Some age groups are affected more frequently than others, depending on the type of vasculitis. However, all types of vasculitis are rare. Though some forms of vasculitis improve on their own, others require ongoing medical treatment — often including taking medications for an extended period of time.
Read More: AIHA - Autoimmune Haemolytic Anaemia
Possible symptoms of vasculitis
The signs and symptoms of vasculitis vary depending on which vessels and, as a result, which organ systems, are affected. However, general signs and symptoms that most people with vasculitis experience include:
- Fever
- Fatigue
- Weight loss
- Muscle and joint pain
- Loss of appetite
Classification
According to the size of the blood vessels which are affected, this disorder could be divided into three groups:
- Large vessel vasculitis
- Medium vessel vasculitis
- Small vessel vasculitis
Each of these is associated with its own definining characteristics.
Large vessel vasculitis
Takayasu arteritis
This is the most common form of large vessel vasculitis and it primarily affects the aorta and its main branches. There are 6 criteria of which three must be present for the diagnosis to be made. They are:
- Onset < 40 years
- Claudication of the extremities — meaning pain in the arms and legs that strikes when the patient is actively moving them
- Decreased pulsation of one or both brachial arteries
- At least 10 mmHg systolic difference in both arms
- Bruit (more commonly known as a murmur in layman's terms) over one or both carotid arteries or abdominal aorta
- A narrowing of the aorta
Giant cell (temporal) arteritis
This is one form of vasculitis that affects both large and medium vessels, primarily affecting the cranial branches of the arteries arising from the aortic arch. Three out of 5 criteria should be present for diagnosis to occur:
- Pain and a decreased pulse of temporal artery
- ESR > 50 mm/h
- A biopsy of the affected artery which shows necrotizing arteritis with prominent mononuclear cells or multinucleated giant cells
- Onset > 50 years
- Localized headache
- Jaw claudication — pain while moving the jaw
- Pain and stiffness in the neck and shoulders
Medium vessel vasculitis
Polyarteritis nodosa
We are talking about one type of vasculitis and aneurysm formation affecting both medium and small arteries. At least 3 out of 10 criteria should be present for diagnosis to occur:
- Mononeuropathy (damage of a single nerve) or polyneuropathy (damage of multiple nerves)
- Diastolic blood pressure > 90 mmHg
- Elevated serum BUN Or serum creatinine
- Hepatitis B infection
- Unexplained weight loss
- The skin rash livedo reticularis, a lace-like rash pattern specifically associated with blood flow problems
- Testicular pain
- Myalgias (muscle pain), weakness
- Arteriographic abnormalities
- Polymorphonuclear cells in arterial wall
Granulomatosis with polyangiitis (Formerly known as Wegener's granulomatosis)
We are talking about one systemic vasculitis of the medium and small arteries. At least 2 out of 4 criteria should be present:
- Microscopic hematuria or RBC casts
- Granulomatous inflammation in the vessels wall
- Nasal or oral inflammation
- Abnormal CXR with nodules, infiltrates, cavities
Kawasaki disease
This is one type of vasculitis which usually affects children below the age of five. The large, medium, and small vessels, prominently the coronary arteries, are affected in Kawasaki disease. Diagnosis requires a fever for five days or more with at least 4 out of 5 criteria:
- Erythema (redness) of the palms and soles
- A polymorphous rash
- Cervical lymphadenopathy
- Bilateral conjunctiva injection
- Fissured lips
Small vessel vasculitis
Churg-Strauss arteritis
This form of arteritis affects medium and small vessels with vascular and extravascular granulomatosis. It is important to know that at least 4 criteria must be present in order to set the right diagnosis:
- Asthma
- Eosinophilia > 10% on CBC
- Mononeuropathy or polyneuropathy
- Migratory or transient pulmonary opacities on CXR
- Paranasal sinus abnormalities
- Eosinophils in artery wall
Microscopic polyangiitis
This specific condition affects capillaries, venules, or arterioles.
Hypersensitivity vasculitis
This specific vasculitis occurs usually due to a hypersensitivity reaction to a known drug. There is presence of skin vasculitis with palpable petechiae or purpura. At least 3 out of 5 criteria should be present at the time of diagnosis:
- Age > 16
- Use of possible triggering drug in relation to symptoms
- Palpable purpura
- A papular rash
- Skin biopsy showing neutrophils around vessels
Henoch-Schönlein purpura
It is important to note that this specific purpura is due to the systemic vasculitis due to tissue deposition of IgA-containing immune complexes. Biopsy of lesions shows inflammation of small vessels. It is also important to know that this is the most common vasculitis in children. Presence of 3 or more criteria guaranties a diagnosis sensitivity of 87%:
- Hematuria — blood in the urine
- Onset < 20 years
- No new medications
- Palpable purpura
- Bowel angina
- GI bleed
Essential cryoglobulinemic vasculitis
This is vasculitis occur most often due to a hepatitis C infection, and causes immune complexes of cryoglobulins - proteins that consists of immunoglobulins and complement and precipitate in the cold while dissolving upon warming them up!
Possible causes of vasculitis
Every patient should know that the vascular system is a very complicated system; an intricate network of blood vessels, from veins and arteries to capillaries. One interesting thing to know about the size of the blood network is that if all blood vessels were laid end to end, they would extend over a length of nearly 60,000 miles. It is well known that the arteries deliver oxygen-rich blood, while the veins return blood with increased amounts of carbon dioxide — a waste product of the metabolism — to the heart.
The capillaries, the smallest blood vessels in the body, connect the veins and the arteries and permit the transfer of fluids and nutrients to and from the surrounding tissues. Although some things are still unknown, it has been proven that, in the case of vasculitis, the blood vessels become inflamed, which can cause the layers of the blood vessel wall to thicken. Logically, this process narrows the blood vessels and leads to the reduction of the amount of blood and therefore oxygen and vital nutrients. These forms of vasculitis are called primary vasculitides.
Forms of vasculitis for which an underlying disease, such as an infection, is the cause are called secondary vasculitides. For instance, most cases of cryoglobulinemia vasculitis are the result of the hepatitis C virus, and the hepatitis B virus. Vasculitis can also occur as the result of some diseases of the immune system, such as rheumatoid arthritis, lupus and Sjogren's syndrome.
Forms of vasculitis for which an underlying disease, such as an infection, is the cause are called secondary vasculitides. For instance, most cases of cryoglobulinemia vasculitis are the result of the hepatitis C virus, and the hepatitis B virus. Vasculitis can also occur as the result of some diseases of the immune system, such as rheumatoid arthritis, lupus and Sjogren's syndrome.
Diagnosis
- Lab tests. Basic lab tests may include a CBC, chem-7, muscle enzyme, liver function tests, ESR, hepatitis seroloties, urinalysis, CXR, and EKG.
- Electromyography. It is useful if a systemic vasculitis is suspected and neuromuscular symptoms are present.
- Arteriography. This method is helpful in vasculitis affecting the large and medium vessels but not helpful in small vessel vasculitis.
- Tissue biopsy. This is the gold standard of diagnosis when biopsy is taken from the most involved area.
Treatment
It is difficult to tell what the best possible treatment for this condition is simply because the treatment regimen depends on type of vasculitis, the severity of every individual case and general health of the patient. Treatments are generally directed toward stopping the inflammation and suppressing the immune system. Although some types of vasculitis are self-limiting and improve on their own, it is important to know that some of the cases involve taking one or more of the following medications:
- Corticosteroids
Several researches done in the past have proven that treatment for many types of vasculitis consists of doses of a corticosteroid drug such as Prednisone or methylprednisolone. These medications are made to suppress patient’s inflammatory response and reduce the inflammation! The fact is that, after the first month, doctor may gradually begin to lower the dose until patient reaches the lowest dose of corticosteroids he or she need to control inflammation.
- Cytotoxic drugs
Unfortunately- some cases of vasculitis that are severe or that don't respond well to corticosteroids may need treatment with cytotoxic drugs. Most commonly used medications of this kind are Azathioprine (Imuran) and Cyclophosphamide (Cytoxan). These drugs suppress the inflammation in your blood vessels.
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
Several researches done in the past have proven that NSAIDs, such as Aspirin and ibuprofen (Advil, Motrin, others), can be effective in treating mild symptoms of some types of vasculitis, such as polymyalgia rheumatica or Kawasaki disease.
- Photo courtesy of Yale Rosen by Flickr : www.flickr.com/photos/pulmonary_pathology/3791887586/
- en.wikipedia.org/wiki/Vasculitis
- www.mayoclinic.com/health/vasculitis/DS00513
- www.medicinenet.com

