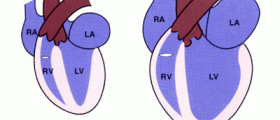
Peripartum cardiomyopathy is a rare occurrence but when it does occur, it can pose a diagnostic and treatment challenge for physicians. This is a disease defined as any type of heart failure that occurs during the last month of pregnancy or within 5 months following the birth of the child.
The causes of peripartum cardiomyopathy are slightly different than a simple dilated cardiomyopathy due to the underlying pathology of what is occurring. Most dilated cardiomyopathy is caused by long-standing alcoholism or uncontrolled diabetes mellitus. Of course, this can still be possible during pregnancies but most of the time, mothers will any form of prenatal care will be under tight supervision from the doctor so blood sugar levels should be under control and patients will try their best to avoid any form of alcoholic drink for the safety of the baby.

There are several key physiological changes that occur during a pregnancy, though, that can predispose women to have a peripartum cardiomyopathy. Due to the extra weight and energy required to help a young fetus develop, the cardiac workload is much higher during the time of pregnancy compared to during the rest of a woman's life. She will also have higher levels of blood flowing through her body to bring constant nutrients and oxygen to her developing baby so these two factors can summate to lead to cardiac problems in certain individuals. Most of the time, a genetic history, previous bacterial infections or a poor diet can lead to heart muscle fatigue and a cardiomyopathy. Having multiple pregnancies at once could also lead to this condition.
Like other forms of cardiomyopathy, the first symptoms that a woman may experience would be shortness of breath and fatigue. This may be obvious when a woman is not pregnant but during pregnancy, it is common for women to be winding due to the demands of carrying an extra life so you may not even thing symptoms are out of the ordinary. As the heart starts to worsen, women may eventually start to notice palpitations, dizziness, swollen legs and arms and sudden drops in blood pressure. These are also commonly associated with pregnancy so it is quite hard to differentiate the symptoms of an underlying heart problem compared to normal physiology.
Women already have lower blood pressures during pregnancy, however, so a sudden drop in blood pressure could not only lead to potential fainting but also could compromise the health and safety of the pregnancy.
Treatment for the condition is much like the treatment for other forms of cardiomyopathy. Patients will benefit from taking B-blockers to help reduce the workload of the heart but because of the delicate nature of the blood pressure during this time, doctors will most likely need to admit a mother into the hospital. Certain medications like ACE-inhibitors or B-blockers of certain types are also contraindicated due to the damage it may cause to the fetus. It is best to try to stabilize the woman as best as possible beforehand and then try to induce the pregnancy or even do a C-section to allow more aggressive therapy once the baby is safely out of the mother. [1]
- 1.) https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2234619/
- Photo courtesy of SteadyHealth