What is a "Pap" smear?
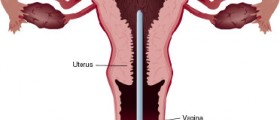
A "Pap" smear test, invented by and named for the doctor Georgios Papanikolaou, is a procedure performed for cervical screening that is used to detect precancerous and/or cancerous changes that may occur on the opening of the uterus, called the cervix.
The test is performed by inserting a medical instrument known as a speculum into the vaginal canal. This device is made from a specific non-allergy metal, plastic, or silicone. The speculum was developed to be inserted into the vagina and then opened and locked into position so that the doctor performing the test can insert a wooden or plastic spatula or brush to collect the cells at the outer lining of the cervix.
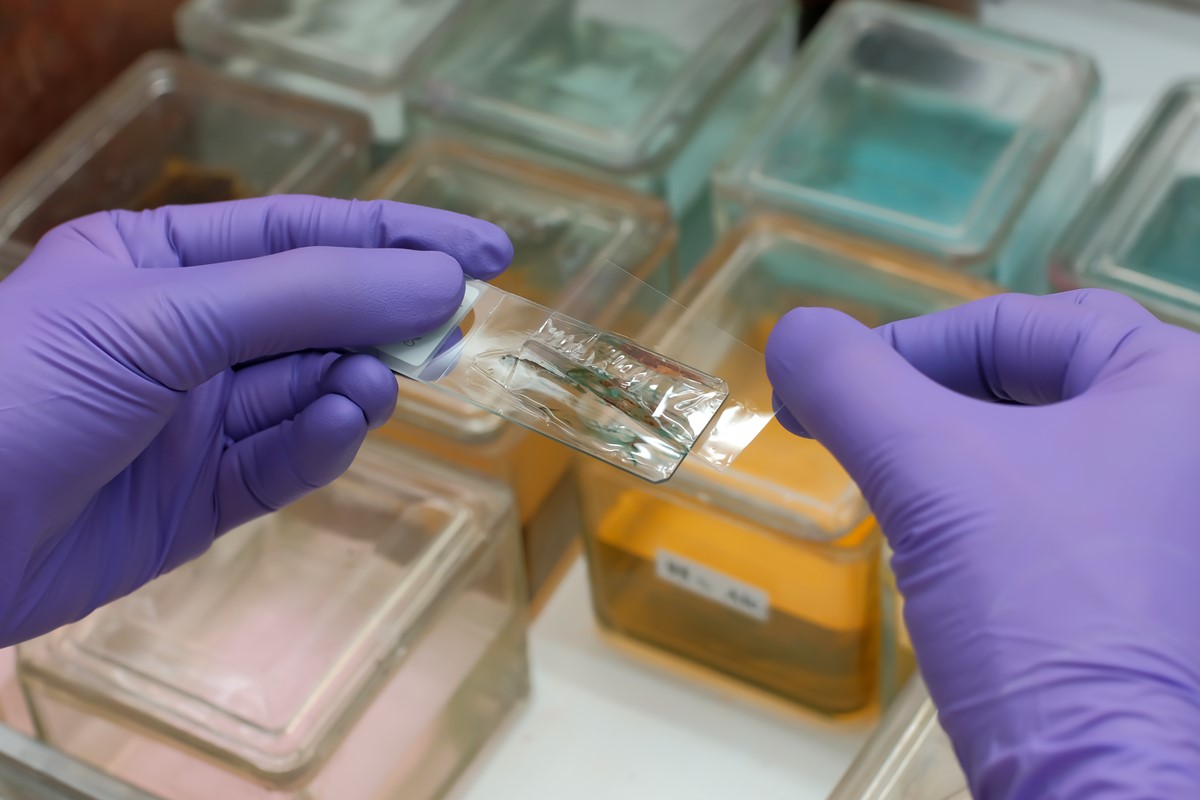
The "Pap" test may also detect any infections present as the cells that are collected around the cervix may also demonstrate inflammatory changes or present with an overgrowth of bacterial or fungal organisms. This scenario would otherwise not have been detected in cases where the patient didn't present with any signs and symptoms of an active infection.
When is a "Pap" smear done?
The recommended time to screen patients for cervical issues by performing a "Pap" smear test in the United States is from 21 until 65 years of age. In other countries, however, "Pap" smear screening is not recommended for non-sexually active women.
The frequency of how often the test should be done is every two to four years, but if any abnormalities are discovered then the test is repeated after six to 12 months depending on the severity of the pathology.
Why can the procedure hurt?
Patient and healthcare-dependent factors include:
- First-time patients not knowing what to expect may be anxious and this causes one to become tenser. This also increases the tension in the muscles of the pelvic floor which can make insertion of the speculum more difficult thus causing more pain and increased anxiety to the patient.
- Using a larger speculum for a smaller patient.
- Not using enough water-based lubricant on the speculum for easier insertion.
- A healthcare professional performing the procedure not using the correct technique or not working delicately enough.
Physiological (non-abnormal) reasons for discomfort when performing the procedure include:
- The cervix is full of nociceptors (pain nerves) so the brush being used to scrape the cells off cervix, which has to be performed with a bit of pressure to make sure that the correct specimen is obtained, may cause more discomfort.
Pathological reasons for the pain experienced may include:
- Infection or inflammation of the vagina (vaginismus) or cervical stenosis can cause the vaginal canal to be more sensitive.
What measures can be taken to help reduce pain?
Informing the patient that this may be a slightly uncomfortable procedure will already help prepare them for this possibility. Having someone supporting the patient also helps to reduce any fears and anxious feelings the patient may have.



_f_280x120.jpg)