i just found out that my pap smear was abnormal. could someone please tell me what this means? i know it means that my cells changed and whatnot but does this mean that i have an std?
Loading...
Hey hunny, I found this article that takes u step by step through abnormal pap smear. Hope this helps. Kee xxx
Very few experiences can be as frightening as receiving a call that your pap smear came back abnormal. Although cervical cancer is the first thing that may comes to mind, most of the time an abnormal pap smear indicates a minor problem with the cervix that may or may not need treatment.
What is the Pap smear?
During a pap smear some cells are scraped or brushed off the cervix, and prepared on a slide that can be examined under a microscope. The purpose of the Pap test is to detect changes that may lead to cervical cancer long before cancer develops. Pre-cancer of the cervix is easily treated, and almost always prevents cancer from developing.
Classification of Pap smearsThere have been many classifications of pap tests, leading to a great deal of confusion. It is much simpler to think of the pap smear as showing one of several things:
[list=] Normal, or a variation of normal, such as "irritation"
Probably normal, but there are mild changes that you should keep an eye on or evaluate further (ASCUS)
Pre-cancerous changes
Invasive cancer [/list]
No matter which classification system is being used, all pap smear reports can be thought of as belonging to one of the above groups.
Years ago, pap smears were graded on a scale from 1 to 5, with 1 being normal and 5 being cancer. There was little agreement between labs of what the numbers meant. Although this classification system is obsolete, some labs unfortunately still use this reporting system.
In order to understand how pap smears are classified, you first need to know a little more about the cervix.
What is the Normal Structure of the Cervix?
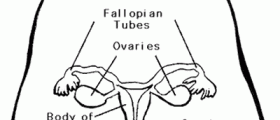
The cervix is the opening of the uterus. The outside of the cervix and the vagina are covered by a layer of flat cells called squamous cells. When a Pap smear is taken, some of these cells are scraped off to be examined under a microscope. The canal of the cervix is lined by tall column-like cells columnar cells.
Somewhere on the cervix the two cell types, squamous cells and columnar cells, meet at a place called the squamo-columnar junction. This junction may be on the outside of the cervix where it is easy to see or within the cervical canal where it may be difficult to see. The squamo-columnar junction is also called the transformation zone because the tall columnar cells are constantly being transformed into flat squamous cells. It is in this transformation zone that abnormal growth or dysplasia develops.
What is cervical dysplasia?
The term "plasia" means growth. Cervical dysplasia means disordered growth. It is easier to understand cervical dysplasia if we first examine the normal cervix. When we look at the lining of the normal cervix under a microscope we see layers of cells. The normal distribution is that the bottom layer is made of round young cells. As the cells mature they rise to the surface and flatten out, so that on the surface the cells are flat
In cervical dysplasia there is a lack of this organized growth process. In mild dysplasia (CIN I) only a few cells are abnormal, while in moderate dysplasia (CIN II) the abnormal cells involve about one-half of the thickness of the surface lining of the cervix
In severe dysplasia or carcinoma-in-situ (CIN III) the entire thickness of cells is disordered, but the abnormal cells have not yet spread below the surface. Carcinoma-in-situ means "cancer in place". If this condition is not treated, it often will grow into an invasive cervical cancer
In dysplasia and carcinoma-in-situ, all of the abnormalities are confined to the surface lining (or "skin") of the cervix. In invasive cancer, the cells are not only disordered throughout the entire thickness of the lining, but they invade the tissue underlying the surface. Invasive cancer is treated entirely differently than dysplasia
Newer classification systems
It is important to realize that the different grades of cervical dysplasia are not a stepwise progression but rather represent a description ranging from a slight irregularity in the cells to a full thickness abnormality. The most important concept is that dysplasia is limited to the "skin" of the cervix, and has not invaded into the underlying tissue. Even "carcinoma-in-situ" is not invasive cancer. In the past, there was a tendency to treat "carcinoma-in-situ" as a much more serious problem than severe dysplasia, when in fact they are essentially the same.
Because of this confusion a new classification system for cervical dysplasia was developed. Remember that "plasia" means "growth." "Neoplasia" means "new growth." The surface layer of cells ("skin") is called "epithelium." Putting this together, a new growth within the epithelium is called "intraepithelial neoplasia." If we are describing the cervix, then the term used is "cervical intraepithelial neoplasia," or "CIN."
The grades of CIN are similar to the older system, with the difference being that severe dysplasia and carcinoma-in-situ both being placed in the category of CIN III. Mild dysplasia is called CIN I and moderate dysplasia is called CIN II.
Again, you should remember that cervical dysplasia should be considered to be pre-cancerous, but not cancer. Statistically, mild dysplasia is more likely to go away without any treatment than severe dysplasia. Severe dysplasia, if left untreated, is more likely to become invasive cancer. To emphasize this, an even newer classification system was developed which simply calls dysplasia low grade (less likely to progress to cancer) or high grade (more likely to progress to cancer) if not treated. Remember, it is extremely uncommon for dysplasia to progress to cancer if it is properly treated and the women has regular follow up exams!
The Atypical Pap (ASCUS)
This is the category that drives women crazy! This means some cells that are slightly funny looking, but not abnormal enough to call dysplasia. (ASCUS stands for "atypical cells of undetermined significance.) This category could also be called "probably normal, but I want to keep a close eye on things." There is a tremendous variation between labs on how many pap smears come back with this reading, which corresponds to the old "Class 2" classification. Some labs will be very liberal in calling normal variations "atypical," which causes women to worry needlessly. Other labs have stricter criteria for this classification.
Infection or vaginitis frequently causes this type of pap smear, so often the pap smear is repeated after the infection is treated. It is common to get this type of pap smear after treatment of the cervix for dysplasia. Since many studies show that 20% to 30% of women with this type of pap smear have dysplasia, it is a good idea to do colposcopy for pap smears that persist in showing these changes.
Often these changes will persist off and on for years, but it is important to understand that this is not a significant problem if dysplasia has been ruled out by colposcopy.
How is Dysplasia Detected?
Usually the abnormal cells are first discovered on a routine Pap test. The Pap test is a screening test that examines cells scraped off the surface of the cervix. When abnormal cells are seen on a Pap test, we must look at the cervix more closely to determine the exact nature of the abnormality. To do this we examine the cervix with a special microscope called a colposcope. This examination is called colposcopy.
How is cervical dysplasia treated?
There are many ways to treat cervical dysplasia (CIN). Factors influencing the choice of treatment for cervical dysplasia include the extent and severity of the dysplasia, the age of the woman, and whether or not she has any other gynecological problems. Often the experience of the physician or other clinician, and the availability of equipment are also major factors. The following are the most common methods of treating cervical dysplasia:
Cryotherapy
Cryotherapy, or freezing, is done by placing a probe against the cervix which cools the cervix to sub-zero temperatures. The cells damaged by freezing are shed over the next month in a heavy watery discharge. The main advantages of freezing are that it is simple to do and uses inexpensive equipment.
One problem with freezing is that the depth cannot be precisely controlled, so abnormal cells may be left behind. This is less of a problem with small areas of mild to moderate dysplasia, and more of a problem with severe dysplasia and carcinoma-in-situ.
Another problem with cryotherapy is that the cervix often heals with the squamo-columnar junction, inside the canal of the cervix, making it difficult to see and causing problems with future evaluation. In spite of these problems, most authorities agree that freezing is an acceptable treatment for small areas of mild or moderate dysplasia. Cryotherapy has a high failure rate for treating large areas of dysplasia and dysplasia that extends into the cervical canal, so other methods are preferable when they are available. Although cryotherapy is acceptable, I stopping using it many years ago because of the excellent results obtained with the laser.
Laser Treatment
The carbon dioxide laser uses a tiny beam of light to vaporize the abnormal cells. This can usually be done in the office with no or very little discomfort. The laser is directed through the colposcope so that the area and depth of treatment can be controlled precisely.
Healing after laser treatment is much faster than after freezing because dead tissue is not left behind. Studies using the latest techniques of laser treatment are showing lower failure rates with the laser than with freezing. Another important advantage is that the cervix usually heals with the squamo-columnar junction visible, so that future evaluation is easily carried out.
The major disadvantage of the laser over the cryo is that it requires sophisticated equipment, and most gynecologists do not have a laser in their office. It is much more expensive to do laser if it has to be done in the hospital. The laser is often replacing cryotherapy in centers where it is available. I believe that the laser is the treatment of choice for most cases of cervical dysplasia (CIN).
Loop Excision
Also known as "LLETZ" or "LEEP", loop excision uses a fine wire loop with electrical energy flowing through it to remove the abnormal area of the cervix. The tissue removed is sent to the laboratory for examination. This procedure, therefore, can often treat and diagnose the problem at the same time. Loop excision is commonly done under local anesthesia and usually causes little discomfort. This can often be used as a substitute for cone biopsy.
Loop excision is sometimes done during the initial colposcopy exam. The advantage of this is that the problem is treated at the time of diagnosis, so it is not necessary to wait for lab results before treatment. At other times, a tiny sample may be taken at the time of the initial evaluation. This might show that no treatment is necessary or allow a choice of other treatment methods (such as laser).
Since many women may prefer time to consider treatment options before choosing a treatment method, I prefer to evaluate the cervix by colposcopy during the first visit, and discuss treatment options at that time, rather than to treat the cervix before a woman has had time to think about her treatment choices.
There is a concern among experts that loop excision is being done for very minor abnormalities that do not require treatment. It is not unusual to see a woman who has had several loop excision procedures done when there was essentially nothing wrong with the cervix. When indicated, loop excision may be an excellent treatment method, but should be used only for significant problems and not just an "atypical" pap test.
Cone Biopsy
A cone biopsy removes a cone-shaped or cylinder-shaped piece of the cervix. It is usually done in an operating room and can be done with a laser or with conventional surgical instruments (cold-cone). A cone biopsy may be done for diagnosis or for treatment, although a diagnostic cone may treat the problem at the same time.
Although laser vaporization and cryotherapy are effective treatments for dysplasia, they are not suitable for invasive cancer. We must, therefore, be absolutely certain that there is not invasive cancer before treating with the laser or with cryo. If we cannot positively rule out invasive cancer on the basis of colposcopy, then an excisional biopsy is mandatory. (This means that the transformation zone of the cervix is removed and examined rather than destroyed.)
A cone biopsy may also be selected as treatment of dysplasia or carcinoma-in-situ. This treatment has a high success rate, but a "cold-cone" has a higher complication rate than a laser cone, cryo, or loop. In a small percentage of cases, a cone biopsy may interfere with childbearing. Many cases requiring cold cone biopsy in the past can be treated, with the laser or with the loop, with a lower chance of complications. Even though I see many women with difficult cases of cervical dysplasia in my practice, it has been many years since I have needed to do a cold cone biopsy!
Hysterectomy
If a woman with dysplasia or carcinoma-in-situ does not want to bear children in the future, then a hysterectomy may be chosen. It has the lowest recurrence rate of any treatment, but it is a major surgical procedure. If she has other problems that may be helped by hysterectomy, then this operation may be the best treatment, one that will take care of all of the problems at the same time. Even after a hysterectomy the dysplasia can come back on the vagina, so it is essential to get regular pap smears even if a hysterectomy is done.
Why treat cervical dysplasia?
Dysplasia is not cancer, but it can turn into cancer if it is not treated. By proper treatment of dysplasia and by proper follow-up, we can significantly reduce the chances that cancer might develop.
Once dysplasia is treated can I forget about it?
No! No matter how dysplasia is treated there is a possibility that it can recur. Usually a recurrence will not be a serious problem if it is detected early, but it can eventually develop into cancer if it is not treated. It is therefore essential to have regular checkups following treatment.
Very few experiences can be as frightening as receiving a call that your pap smear came back abnormal. Although cervical cancer is the first thing that may comes to mind, most of the time an abnormal pap smear indicates a minor problem with the cervix that may or may not need treatment.
What is the Pap smear?
During a pap smear some cells are scraped or brushed off the cervix, and prepared on a slide that can be examined under a microscope. The purpose of the Pap test is to detect changes that may lead to cervical cancer long before cancer develops. Pre-cancer of the cervix is easily treated, and almost always prevents cancer from developing.
Classification of Pap smearsThere have been many classifications of pap tests, leading to a great deal of confusion. It is much simpler to think of the pap smear as showing one of several things:
[list=] Normal, or a variation of normal, such as "irritation"
Probably normal, but there are mild changes that you should keep an eye on or evaluate further (ASCUS)
Pre-cancerous changes
Invasive cancer [/list]
No matter which classification system is being used, all pap smear reports can be thought of as belonging to one of the above groups.
Years ago, pap smears were graded on a scale from 1 to 5, with 1 being normal and 5 being cancer. There was little agreement between labs of what the numbers meant. Although this classification system is obsolete, some labs unfortunately still use this reporting system.
In order to understand how pap smears are classified, you first need to know a little more about the cervix.
What is the Normal Structure of the Cervix?
The cervix is the opening of the uterus. The outside of the cervix and the vagina are covered by a layer of flat cells called squamous cells. When a Pap smear is taken, some of these cells are scraped off to be examined under a microscope. The canal of the cervix is lined by tall column-like cells columnar cells.
Somewhere on the cervix the two cell types, squamous cells and columnar cells, meet at a place called the squamo-columnar junction. This junction may be on the outside of the cervix where it is easy to see or within the cervical canal where it may be difficult to see. The squamo-columnar junction is also called the transformation zone because the tall columnar cells are constantly being transformed into flat squamous cells. It is in this transformation zone that abnormal growth or dysplasia develops.
What is cervical dysplasia?
The term "plasia" means growth. Cervical dysplasia means disordered growth. It is easier to understand cervical dysplasia if we first examine the normal cervix. When we look at the lining of the normal cervix under a microscope we see layers of cells. The normal distribution is that the bottom layer is made of round young cells. As the cells mature they rise to the surface and flatten out, so that on the surface the cells are flat
In cervical dysplasia there is a lack of this organized growth process. In mild dysplasia (CIN I) only a few cells are abnormal, while in moderate dysplasia (CIN II) the abnormal cells involve about one-half of the thickness of the surface lining of the cervix
In severe dysplasia or carcinoma-in-situ (CIN III) the entire thickness of cells is disordered, but the abnormal cells have not yet spread below the surface. Carcinoma-in-situ means "cancer in place". If this condition is not treated, it often will grow into an invasive cervical cancer
In dysplasia and carcinoma-in-situ, all of the abnormalities are confined to the surface lining (or "skin") of the cervix. In invasive cancer, the cells are not only disordered throughout the entire thickness of the lining, but they invade the tissue underlying the surface. Invasive cancer is treated entirely differently than dysplasia
Newer classification systems
It is important to realize that the different grades of cervical dysplasia are not a stepwise progression but rather represent a description ranging from a slight irregularity in the cells to a full thickness abnormality. The most important concept is that dysplasia is limited to the "skin" of the cervix, and has not invaded into the underlying tissue. Even "carcinoma-in-situ" is not invasive cancer. In the past, there was a tendency to treat "carcinoma-in-situ" as a much more serious problem than severe dysplasia, when in fact they are essentially the same.
Because of this confusion a new classification system for cervical dysplasia was developed. Remember that "plasia" means "growth." "Neoplasia" means "new growth." The surface layer of cells ("skin") is called "epithelium." Putting this together, a new growth within the epithelium is called "intraepithelial neoplasia." If we are describing the cervix, then the term used is "cervical intraepithelial neoplasia," or "CIN."
The grades of CIN are similar to the older system, with the difference being that severe dysplasia and carcinoma-in-situ both being placed in the category of CIN III. Mild dysplasia is called CIN I and moderate dysplasia is called CIN II.
Again, you should remember that cervical dysplasia should be considered to be pre-cancerous, but not cancer. Statistically, mild dysplasia is more likely to go away without any treatment than severe dysplasia. Severe dysplasia, if left untreated, is more likely to become invasive cancer. To emphasize this, an even newer classification system was developed which simply calls dysplasia low grade (less likely to progress to cancer) or high grade (more likely to progress to cancer) if not treated. Remember, it is extremely uncommon for dysplasia to progress to cancer if it is properly treated and the women has regular follow up exams!
The Atypical Pap (ASCUS)
This is the category that drives women crazy! This means some cells that are slightly funny looking, but not abnormal enough to call dysplasia. (ASCUS stands for "atypical cells of undetermined significance.) This category could also be called "probably normal, but I want to keep a close eye on things." There is a tremendous variation between labs on how many pap smears come back with this reading, which corresponds to the old "Class 2" classification. Some labs will be very liberal in calling normal variations "atypical," which causes women to worry needlessly. Other labs have stricter criteria for this classification.
Infection or vaginitis frequently causes this type of pap smear, so often the pap smear is repeated after the infection is treated. It is common to get this type of pap smear after treatment of the cervix for dysplasia. Since many studies show that 20% to 30% of women with this type of pap smear have dysplasia, it is a good idea to do colposcopy for pap smears that persist in showing these changes.
Often these changes will persist off and on for years, but it is important to understand that this is not a significant problem if dysplasia has been ruled out by colposcopy.
How is Dysplasia Detected?
Usually the abnormal cells are first discovered on a routine Pap test. The Pap test is a screening test that examines cells scraped off the surface of the cervix. When abnormal cells are seen on a Pap test, we must look at the cervix more closely to determine the exact nature of the abnormality. To do this we examine the cervix with a special microscope called a colposcope. This examination is called colposcopy.
How is cervical dysplasia treated?
There are many ways to treat cervical dysplasia (CIN). Factors influencing the choice of treatment for cervical dysplasia include the extent and severity of the dysplasia, the age of the woman, and whether or not she has any other gynecological problems. Often the experience of the physician or other clinician, and the availability of equipment are also major factors. The following are the most common methods of treating cervical dysplasia:
Cryotherapy
Cryotherapy, or freezing, is done by placing a probe against the cervix which cools the cervix to sub-zero temperatures. The cells damaged by freezing are shed over the next month in a heavy watery discharge. The main advantages of freezing are that it is simple to do and uses inexpensive equipment.
One problem with freezing is that the depth cannot be precisely controlled, so abnormal cells may be left behind. This is less of a problem with small areas of mild to moderate dysplasia, and more of a problem with severe dysplasia and carcinoma-in-situ.
Another problem with cryotherapy is that the cervix often heals with the squamo-columnar junction, inside the canal of the cervix, making it difficult to see and causing problems with future evaluation. In spite of these problems, most authorities agree that freezing is an acceptable treatment for small areas of mild or moderate dysplasia. Cryotherapy has a high failure rate for treating large areas of dysplasia and dysplasia that extends into the cervical canal, so other methods are preferable when they are available. Although cryotherapy is acceptable, I stopping using it many years ago because of the excellent results obtained with the laser.
Laser Treatment
The carbon dioxide laser uses a tiny beam of light to vaporize the abnormal cells. This can usually be done in the office with no or very little discomfort. The laser is directed through the colposcope so that the area and depth of treatment can be controlled precisely.
Healing after laser treatment is much faster than after freezing because dead tissue is not left behind. Studies using the latest techniques of laser treatment are showing lower failure rates with the laser than with freezing. Another important advantage is that the cervix usually heals with the squamo-columnar junction visible, so that future evaluation is easily carried out.
The major disadvantage of the laser over the cryo is that it requires sophisticated equipment, and most gynecologists do not have a laser in their office. It is much more expensive to do laser if it has to be done in the hospital. The laser is often replacing cryotherapy in centers where it is available. I believe that the laser is the treatment of choice for most cases of cervical dysplasia (CIN).
Loop Excision
Also known as "LLETZ" or "LEEP", loop excision uses a fine wire loop with electrical energy flowing through it to remove the abnormal area of the cervix. The tissue removed is sent to the laboratory for examination. This procedure, therefore, can often treat and diagnose the problem at the same time. Loop excision is commonly done under local anesthesia and usually causes little discomfort. This can often be used as a substitute for cone biopsy.
Loop excision is sometimes done during the initial colposcopy exam. The advantage of this is that the problem is treated at the time of diagnosis, so it is not necessary to wait for lab results before treatment. At other times, a tiny sample may be taken at the time of the initial evaluation. This might show that no treatment is necessary or allow a choice of other treatment methods (such as laser).
Since many women may prefer time to consider treatment options before choosing a treatment method, I prefer to evaluate the cervix by colposcopy during the first visit, and discuss treatment options at that time, rather than to treat the cervix before a woman has had time to think about her treatment choices.
There is a concern among experts that loop excision is being done for very minor abnormalities that do not require treatment. It is not unusual to see a woman who has had several loop excision procedures done when there was essentially nothing wrong with the cervix. When indicated, loop excision may be an excellent treatment method, but should be used only for significant problems and not just an "atypical" pap test.
Cone Biopsy
A cone biopsy removes a cone-shaped or cylinder-shaped piece of the cervix. It is usually done in an operating room and can be done with a laser or with conventional surgical instruments (cold-cone). A cone biopsy may be done for diagnosis or for treatment, although a diagnostic cone may treat the problem at the same time.
Although laser vaporization and cryotherapy are effective treatments for dysplasia, they are not suitable for invasive cancer. We must, therefore, be absolutely certain that there is not invasive cancer before treating with the laser or with cryo. If we cannot positively rule out invasive cancer on the basis of colposcopy, then an excisional biopsy is mandatory. (This means that the transformation zone of the cervix is removed and examined rather than destroyed.)
A cone biopsy may also be selected as treatment of dysplasia or carcinoma-in-situ. This treatment has a high success rate, but a "cold-cone" has a higher complication rate than a laser cone, cryo, or loop. In a small percentage of cases, a cone biopsy may interfere with childbearing. Many cases requiring cold cone biopsy in the past can be treated, with the laser or with the loop, with a lower chance of complications. Even though I see many women with difficult cases of cervical dysplasia in my practice, it has been many years since I have needed to do a cold cone biopsy!
Hysterectomy
If a woman with dysplasia or carcinoma-in-situ does not want to bear children in the future, then a hysterectomy may be chosen. It has the lowest recurrence rate of any treatment, but it is a major surgical procedure. If she has other problems that may be helped by hysterectomy, then this operation may be the best treatment, one that will take care of all of the problems at the same time. Even after a hysterectomy the dysplasia can come back on the vagina, so it is essential to get regular pap smears even if a hysterectomy is done.
Why treat cervical dysplasia?
Dysplasia is not cancer, but it can turn into cancer if it is not treated. By proper treatment of dysplasia and by proper follow-up, we can significantly reduce the chances that cancer might develop.
Once dysplasia is treated can I forget about it?
No! No matter how dysplasia is treated there is a possibility that it can recur. Usually a recurrence will not be a serious problem if it is detected early, but it can eventually develop into cancer if it is not treated. It is therefore essential to have regular checkups following treatment.
Loading...





_f_280x120.jpg)