A varicocele is an enlargement of the veins within the scrotum, the bag of skin that holds the testicles. It isn't a rare condition because latest researches show that up to 1 in 5 men have a varicocele.
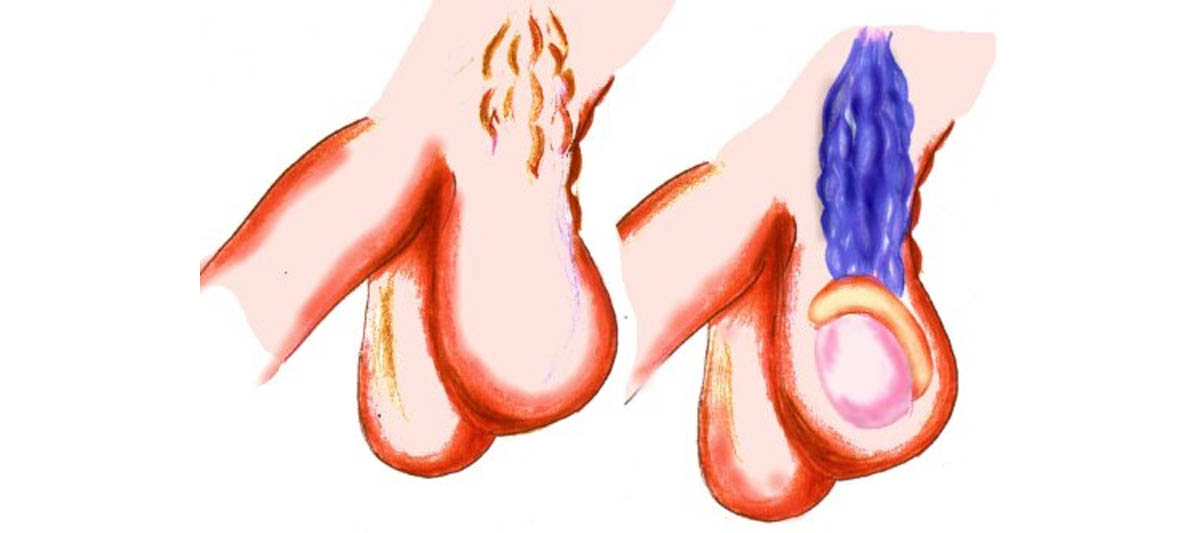
Normal male anatomy
The term varicocele specifically refers to the dilatation and tortuosity of the pampiniform plexus, the network of veins that drain the testicles. This plexus travels along the posterior part of the testicle with the epididymis and vas deferens, and then into the spermatic cord. The right testicle vein drains into the inferior vena cava, while the left testicle vein drains into the left renal vein, which then drains into the inferior vena cava.
This is important because, with this position, there is a greater chance for the left testicle to develop a varicocele because of the right angle between the veins. The small vessels of the pampiniform plexus normally range from 0.5 to 1.5 mm in diameter. Dilatation of these vessels beyond 2 mm is called a varicocele.
Possible causes of a varicocele
The idiopathic varicocele
Simply put, the cause of this type of varicocele is unknown — that is what "idiopathic" means. It occurs when the valves within the veins along the spermatic cord don't work properly. The result is a backflow of blood into the pampiniform plexus and increased pressure, ultimately leading to damage to the testicular tissue. As mentioned above, almost 98 percent of idiopathic varicoceles occur on the left side, apparently because the left testicular vein runs vertically up to the renal vein, but 70 percent of patients with varicoceles have them bilaterally.
The secondary varicocele
In medical terminology, the word "secondary" simply means that the condition was caused by another underlying problem. A secondary varicocele forms due to a compression of the venous drainage of the testicle. A pelvic or abdominal malignancy is a definite concern when a varicocele is newly diagnosed in a patient older than 40 years of age. A non-malignant cause of a secondary varicocele is known as "nut-cracker SMA" (superior mesenteric artery). This represents a condition in which the superior mesenteric artery compresses the left renal vein, causing increased pressure there to be transmitted retrograde into the left pampiniform plexus and leading to a varicocele.
Who is most at risk of developing a varicocele?
Varicoceles are a fairly common medical problem in men, and age is the only known risk factor for developing this condition. Varicoceles appear in about 15 percent of men between 15 and 25 years of age, mostly in puberty. During puberty the testicles grow rapidly and need more blood delivered to them. So, if the valves in the veins in the scrotum aren't functioning well, the veins can't transport this extra blood from the testicles. This then leads to the creation of a varicocele.
Signs and symptoms of a varicocele: What should you look out for?
Varicoceles usually develop slowly and may not have any symptoms. However, if there are symptoms, they tend to occur during hot weather, after heavy exercise, or when a man has been standing or sitting for a long time.
Signs of a varicocele include:
* a strange and dull ache in the testicle
* a feeling of heaviness or dragging in the scrotum
* dilated veins in the scrotum that can be felt under fingers
* discomfort in the testicle or on that particular side of the scrotum
Diagnosis of varicocele
* Physical examination
In most cases, the doctor will conduct a physical exam which may reveal a twisted, non-tender mass above the patient’s testicle. Some people have described the mass as feeling like a bag of worms. If it's large enough, the doctor will be able to feel it while the patient is standing up. In other cases the doctor may ask a patient to take a deep breath and hold it while he bears down. This is called the Valsalva maneuver. This helps your doctor detect abnormal enlargement of the veins.
* Scrotal ultrasound
If the physical exam is inconclusive, the doctor may order a scrotal ultrasound. This test, which uses high-frequency sound waves to create precise images of structures inside the body, may be used to ensure there isn't another reason for patient’s symptoms.
Complications of a varicocele if left untreated
An untreated varicocele may cause:
* Atrophy of the testis
The bulk of the testicle is made up of sperm-producing tubules. When damaged, the testicle shrinks and softens.
* Infertility
It's not clear how varicoceles affect male fertility, but some experts believe that the testicular veins cool the blood in the testicular artery, helping to maintain the proper temperature for optimal sperm production.
Treatment options for a varicocele
Open surgery: This is the most common form of treatment, usually done on an outpatient basis. General or local anesthetic is used.
There are several possible approaches to the vein:
* through the groin (transinguinal)
* abdomen (retroperitoneal)
* below the groin (infrainguinal/infrapubic)
Laparoscopic surgery: With this approach, the surgeon makes a small incision in the abdomen and passes a tiny instrument through the incision to see and to repair the varicocele.
Recovery after surgical repair usually proceeds rapidly and in most cases, the patient can return to normal activities that aren't strenuous after two days. There will be some pain but it’s usually mild. The doctor should advise a patient to take over-the-counter (OTC) painkillers, such as acetaminophen (Tylenol, others) or ibuprofen (Motrin, Advil, others) to relieve the discomfort. Also, avoiding sexual intercourse for a week or so may be advised.
Varicocele embolization
This non-surgical solution has been successful at eliminating varicoceles for thousands of men, and can have you back to your active lifestyle in only a few days. Many men choose this non-surgical alternative because it does not involve general anesthesia, incisions in the scrotum, or sutures.
A radiologist inserts a tube into a vein in the patient’s groin or neck through which instruments can be passed. Viewing enlarged veins on a monitor, the doctor releases balloons to create a blockage in the testicular veins, which interrupts the blood flow and repairs the varicocele. This procedure uses sedation and may take several hours. Because it presents somewhat greater risks than open surgery and offers little advantage, this procedure isn't widely used.
Advantages of this procedure:
* Outpatient procedure
* Recovery time usually less than 24 hours
* No anesthesia
* No incision/no stitches
* Fewer complications than surgery
Cost of this procedure
Although it isn't cheep, the cost is generally comparable to varicocele surgery. However, the cost varies by geographic area and local insurance company policies.
Read More: Male Varicocele And Infertility: Myths And Reality
Possible complications
Some of the most common complications are:
* bruising at the catheter site
* nausea
* low-grade backache
* Infection
* hydrocele
* loss of a testicle
* recurring of the varicocele
Embolization and semen analysis
Studies have shown that varicocele repair can improve semen analysis significantly, but there is no guarantee. It has been proven that pregnancy rates in infertile couples improve after varicocele repair by about 30-50%.

