Supraventricular tachycardia (SVT) is a series of fast atrial heartbeats that can cause the heart to contract at rates of 250 times per minute or faster. The term “supraventricular” means that the process is originating above the ventricles. These fast heartbeats can be uncomfortable and frightening. Supraventricular tachycardia is also called paroxysmal supraventricular tachycardia (PSVT) or paroxysmal atrial tachycardia (PAT).
Electrical heart conducting system
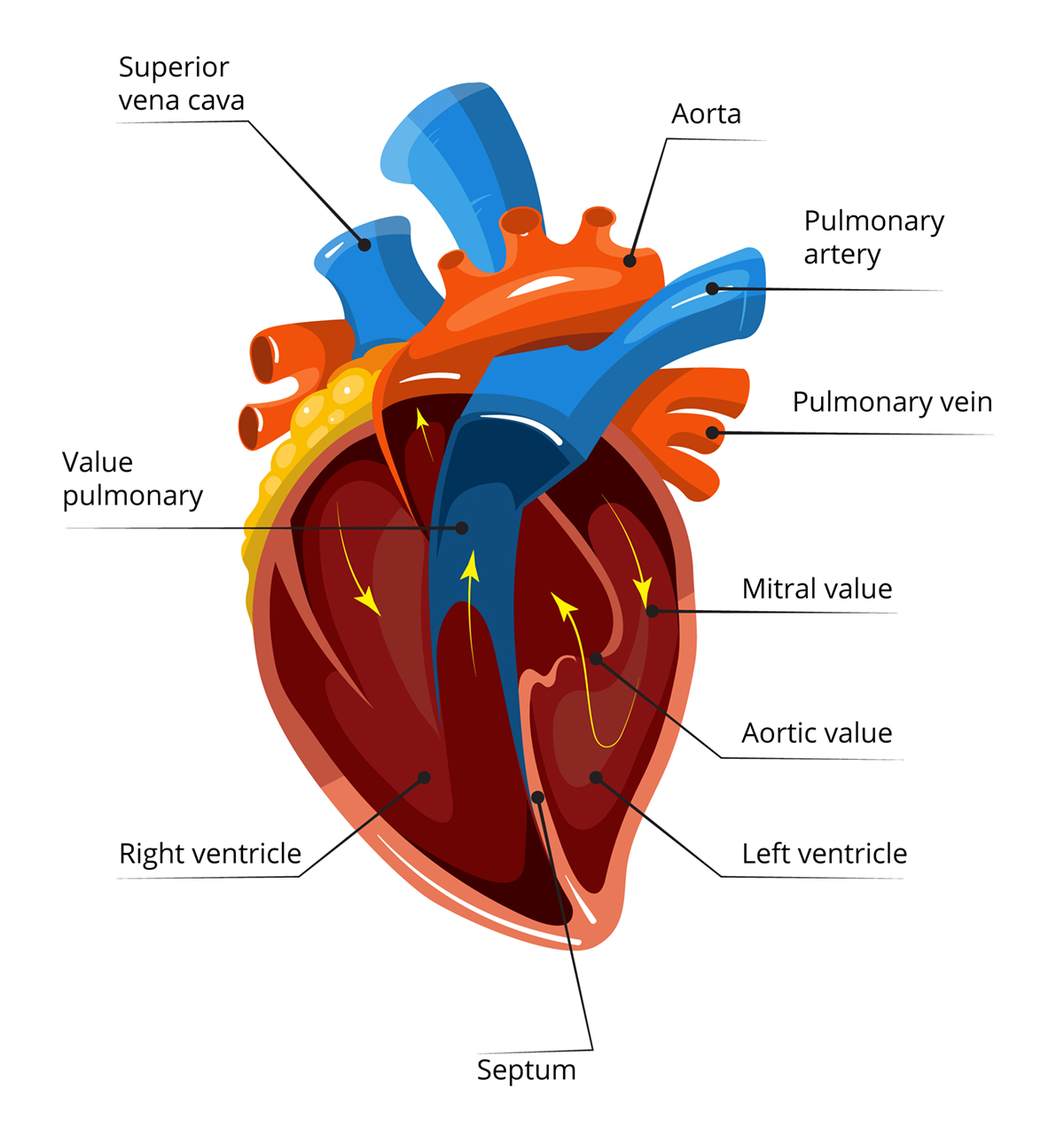
The heart consists of 4 chambers: 2 upper chambers called atria and 2 lower chambers called ventricles. The rhythm of the heart is normally controlled by a natural pacemaker called the sino-atrial node in the right upper chamber.
It beats about 60 times per minute at rest and and normally its pace increases when exercising. It is important to know that electrical impulses travel from the natural pacemaker through the atria, pass through a node called the atrio-ventricular node between the atria and ventricles, before running down the specialized fibers that activate the ventricles. There are several things that could cause damage to this impulse conducting system and lead to tachycardia. The term tachycardia refers to a rapid heartbeat of over 100 beats per minute. Supraventricular tachycardia is a rapid rhythm of the heart that begins in the upper chambers.
Symptoms of supraventricular tachycardia
The symptoms can come on suddenly and may go away by themselves. They can last a few minutes or as long as 1-2 days. The following symptoms are typical with a rapid pulse of 140-250 beats per minute:
- Palpitations

- Lightheadedness
- Dizziness
- Loss of consciousness
- Chest pain
- Shortness of breath
- Fatigue
- Diaphoresis
- Nausea
Some patients have no symptoms what so ever.
Although the symptoms may raise concern and may feel really scary, in general, supraventricular tachycardia is not a serious or life-threatening condition.
However, if any of these symptoms develops, immediate medical attention should be sought.
Incidence of the condition
Supraventricular tachycardia incidence is approximately 1-3 cases per 1000 persons. In some population-based studies, the prevalence of this condition was 2.25 cases per 1000 persons, with an incidence of 35 cases per 100,000 person-years. It is more common in patients who are of middle age or older, while adolescents are more likely to have SVT mediated by an accessory pathway. PSVT is not only observed in healthy individuals, it is also common in patients with previous:
- myocardial infarction,
- valve prolapse,
- rheumatic heart disease,
- pericarditis,
- pneumonia,
- chronic lung disease, and
- current alcohol intoxication
Causes of supraventricular tachycardia
Supraventricular tachycardia can be initiated in the:
- SA node;
- in the atria
- in the atrial conduction pathways; or
- in the AV node
Wolff-Parkinson-White Syndrome is a common cause of supraventricular tachycardia. In people with this syndrome there is an abnormal electrical connection between the atria and ventricles. This extra tissue forms a short circuit between these chambers. It provides an extra pathway for electrical impulses and so they are conducted through the tissue that normally blocks electrical impulses between the atria and ventricles.
There are several risk factors that can increase the chance of getting these rapid heart beats and the most common are:
- excessive smoking,
- caffeine, and
- alcohol use
- digitalis toxicity
Types of tachycardia originating from the atria
Sinus tachycardia
Sinus tachycardia is a condition characterized by an accelerated sinus rate that is a physiologic response to stress. Heart rate is faster than 100 beats per minute and generally involves a regular rhythm. The most common causes are:
- hypoxia
- hypovolemia
- fever
- anxiety
- pain
- hyperthyroidism
- exercise usually
Certain drugs such as stimulants (eg. nicotine, caffeine), medications (eg. atropine, salbutamol) and recreational drugs (eg. cocaine, amphetamines, ectsasy) can also induce sinus tachycardia.
Sinus nodal reentrant tachycardia
This condition is caused by a reentry circuit, either in or near the sinus node. The heart rate is usually 100-150 beats per minute, and ECG tracings usually demonstrate normal sinus P-wave morphology.
Atrial tachycardia
Atrial tachycardia is an arrhythmia originating in the atrial myocardium which means that it doesn’t affect the heart conducting system. The heart rate is regular and is usually 120-250 beats per minute. Because the arrhythmia does not involve the AV node, nodal blocking medications are usually unsuccessful in terminating this arrhythmia.
Multifocal atrial tachycardia
This is a condition that arises within the atrial tissue and is characterized by 3 or more P-wave morphologies. This type of arrhythmia is fairly uncommon and is typically observed in elderly patients. The heart rate is greater than 100 beats per minute, and ECG findings typically include an irregular rhythm.
Atrial flutter
Atrial flutter is a tachycardia which arises above the AV node with an atrial rate of 250-350 beats per minute. It is proven that atrial flutter is caused by a macro-reentrant right atrial circuit. It is commonly observed in patients with ischemic heart disease, myocardial infarction, cardiomyopathy, myocarditis, pulmonary embolus, toxic ingestion, or chest trauma.
Atrial fibrillation
It is a very common type of arrhythmia arising from chaotic atrial depolarization. The atrial rate is usually 300-600 beats per minute, while the ventricular rate may be 170 beats per minute or more. It is associated with rheumatic heart disease, hypertension, ischemic heart disease, pericarditis, thyrotoxicosis, alcohol intoxication, mitral valve prolapse, and digitalis toxicity.
Diagnosis of supraventricular tachycardia
EKG and holter monitoring
The electrocardiogram is one of the best diagnostic tools for diagnosis of supraventricular tachycardia. It provides a picture of the heart rhythm and is recorded by placing adhesive or gel pads on the chest and limbs. If the patient is experiencing SVT during the ECG, a clear diagnosis can be made. Besides usual ECG test, a holter monitor may also be used to record the heart rhythm continuously for 24 hours. This type of monitor is particularly helpful in documenting asymptomatic or very frequent rhythm abnormalities.
Lab-tests
- Heart enzymes - A cardiac enzyme evaluation should be ordered for patients with chest pain, patients with risk factors for myocardial infarction, and patients who are otherwise unstable and present with heart failure, hypotension, or pulmonary edema. Young patients with no structural heart defects have a very low risk of myocardial infarction.
- Electrolyte levels - These levels should be checked because electrolyte abnormalities can contribute to PSVT.
- CBC - A complete blood cell count helps assess whether anemia is contributing to the tachycardia or ischemia.
- Thyroid tests - The results from thyroid studies are rarely diagnostic of hyperthyroidism.
- Digoxin levels - Digoxin level test should be done in patients on Digoxin because supraventricular tachycardia is one of the many heart rhythm problems that can be caused by supra-therapeutic levels of this drug.
Electrophysiology (EP) study
Doctor may also recommend an electrophysiology (EP) study - the test in which flexible wires are inserted into a vein, usually in the groin, and threaded into the heart. Electrodes at the end of the wires send information about the heart's electrical activity.
READ Supraventricular tachycardia: Long term side effects
Treatment of supraventricular tachycardia
Some supraventricular tachycardias do not cause symptoms and may not need any treatment. However, when symptoms occur, treatment is usually recommended. Treatment of supraventricular tachycardia is aimed at correcting the cause of the arrhythmia or controlling the rapid heart rates.
Medications
Medications are generally helpful in maintaining a normal heart rhythm. Medications may be used to treat many patients with supraventricular tachycardia and the most commonly used classes of medications are:
ß-blockers
These are medications commonly used to treat high blood pressure and other heart problems such as angina. In cases of Supraventricular Tachycardia, they are used specifically to decrease conduction through the AV node during the tachycardia which should stop that unpleasant heartbeat.
Calcium channel blockers
These are also used to treat high blood pressure and heart problems. Like ß-blockers, they may be used to decrease conduction through the AV node. Some of the most commonly used calcium channel blockers include verapamil or diltiazem.
Anti-arrhythmic medications
These agents are used to treat various heart rhythm problems and directly affect the atrial or ventricular heart tissue.
Radiofrequency ablation
During this procedure, special plastic tubes called catheters are inserted into a vein in the groin area and are guided to the heart using a fluoroscope. What is the purpose of these tubes? The catheters are used to record electrical signals from inside the heart. Special radio waves are delivered at the tip of this catheter to the precise location of the supraventricular tachycardia, creating a small coagulation of the tissue approximately 2 mm in diameter. The procedure has a 90% to 95% chance of successfully treating this condition, so that it does not recur or require medication.
- www.circ.ahajournals.org
- www.emedicine.com
- www.nlm.nih.gov
- Photo courtesy of rosmary by Flickr : www.flickr.com/photos/rvoegtli/5343361247/