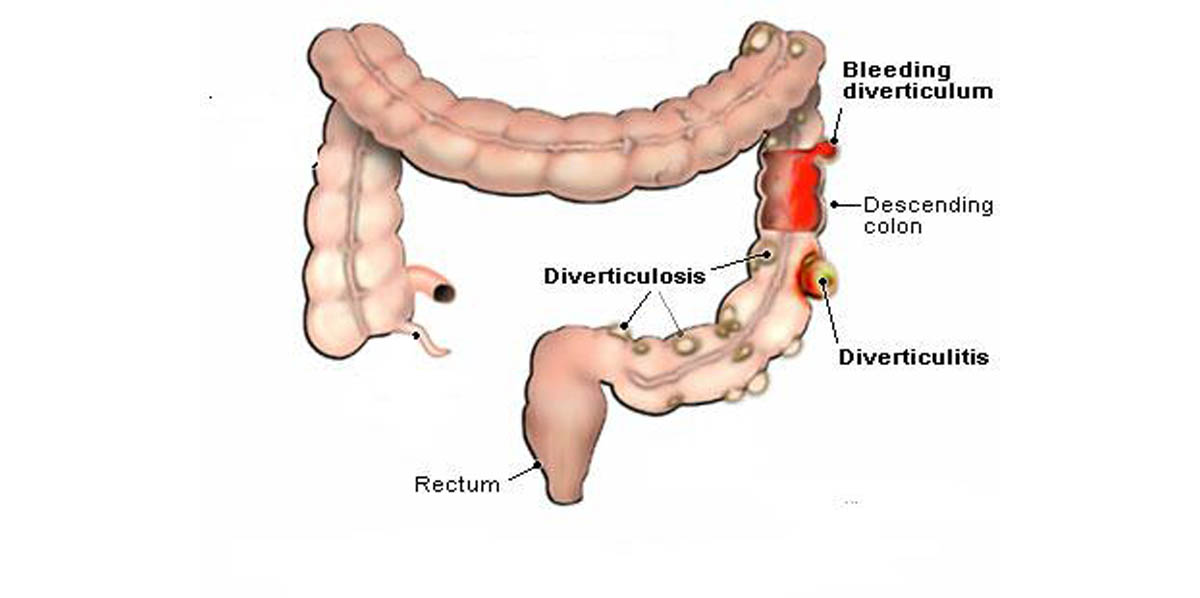
The basic condition is diverticulosis which involves the formation of small pouches called diverticula on the outside of the colon, because diverticulitis actually develops from it.. Diverticulitis occurs when one of these diverticula becomes inflamed. Mild cases of diverticulitis can be treated with rest, changes in your diet and antibiotics, but serious cases may require surgery to remove the diseased portion of the colon.
Incidence
Problem with diverticulitis is that, although it usually affects the middle-aged and the elderly, it can strike younger patients as well. The prevalence of diverticulitis has increased from an estimated 10% in the 1920s to between 35 and 50% by the late 1960s.
At this moment 65% of those 85 years of age and older can be expected to have some form of diverticular disease of the colon. Less than 5% of those aged 40 years and younger may also be affected by diverticular disease. Among the patients with diverticulosis, 10-25% patients will go on to develop diverticulitis during their lifetime. Genetics are believed to play an important role. that the proof of that lies in the fact that Asian people tend to have a predominance of the right-sided diverticula, while Western people tend to have the left-sided form of the disease. While some older studies concluded that diverticulitis was more common in women, the more recent work has noted a similar incidence in men and women.
Possible causes of diverticulitis
Aging causes changes in collagen structure that may lead to the weakening of the colonic wall. The development of colonic diverticula is considered to be a result of raised intraluminal colon pressures. This means that these diverticula develop when naturally weak places that exist in colon give way under pressure. Pouches are most common in sigmoid and descending colon - the lower portions of your large intestine just above your rectum.
Experts think that this is because the sigmoid colon has the smallest diameter of any portion of the colon, and therefore it is the portion which would be expected to have the highest intraluminal pressure. It also very often occurs as a result of straining during bowel movements. Another problem is that these small pouches are growing with time, which allows the small parts of the stool to become lodged in them leading to an infection. Colonic motility disorders, corticosteroids, and ingestion of non-steroidal anti-inflammatory drugs may also be predisposing factors.
Possible complications
There are several possible complications that could occur when person has already developed diverticulitis. If it is left untreated, diverticulitis can lead to serious complications requiring extensive surgery. A small tears or perforations can develop in an infected pouch, which in turn can cause the infection to spread to the whole of your abdomen. This is a very serious infection called peritonitis. If the infection is limited to an area around the wall of your colon where the diverticula are inflamed, you may develop a localized collection of pus known as an abscess.
Sometimes the inflamed diverticula can cause the narrowing of the bowel, leading to an obstruction. Also, the affected part of the colon could adhere to the bladder or other organs in the pelvic area, causing a fistula, or abnormal communication between the colon and an adjacent organ. The most common is a colo-vesicular fistula (colon to urinary bladder). This is observed almost exclusively in men and in women following hysterectomy, probably because of the interposition of the uterus between the sigmoid colon and the urinary bladder. Colo-vaginal and colo-cutaneous fistulae are much less common. Another potential complication of diverticulitis is severe internal and colonic bleeding. Although there's no evidence that diverticular disease increases the risk of colon or rectal cancer, it can make cancer more difficult to diagnose.
Signs and symptoms
Asymptomatic diverticulosis is a common condition, but only a few patients with diverticula develop symptomatic diverticulitis. It is very often very difficult to diagnose diverticulitis because it can mimic the symptoms characteristic to some other gastrointestinal diseases. For example, diverticulitis can feel like appendicitis, except the fact that the patients generally have pain in the lower left side of abdomen, instead of the lower right side. There is no rule about this pain. It may begin suddenly and be very severe but it can also begin with mild pain that becomes worse over several days and fluctuates in intensity.
The most common symptoms are:
- Abdominal tenderness
- Fever, nausea
- Constipation or diarrhea
The less common symptoms are:
- Vomiting
- Bloating
- Bleeding from your rectum
- Frequent urination
- Difficulty or pain while urinating
- Tenderness in your abdomen when wearing a belt or bending over
Risk factors for developing diverticulitis
Since the exact cause of diverticulitis is still poorly understood, no one really knows a lot about the possible risk factors for developing diverticulitis. The bottom line is that all the risk factors contributing to the development of this condition do so by increasing the pressure on the wall of colon. The most common are:
Aging
As a person ages, the outer muscular wall of the colon thickens, causing the inside space to narrow. The narrowing increases the pressure in the colon and makes it more likely for pouches to form. The fact is also that the outer wall thickening also makes it more difficult for your colon to move the waste through to your rectum. The results are known – the waste stays in your colon longer, becoming harder and dryer and exerting additional pressure on weak areas when the muscles of your colon try to move it along. This is also represents a risk factor for infection.
Too little fiber
Diverticulitis is rare in countries where people eat a high-fiber diet that helps keep stools soft while it is common in industrialized nations where an average diet is high in carbohydrates and low in fiber. This means that it has a lot to do with the things we eat. Too little fiber contributes to small, hard stools that are difficult to pass, which increases pressure in your colon.
Diagnosis of diverticulitis
If we talk about differential diagnosis, then we should know that it includes colon cancer, inflammatory bowel disease, ischemic colitis, and irritable bowel syndrome, as well as a number of urological and gynecological processes.
Lab studies
Routine laboratory data are important to confirm the presence of infection and to exclude other possible etiologies of abdominal pain. A CBC count identifies leukocytosis. Urinalysis and urine cultures can be used to identify urinary tract infection.
Imaging Studies
X-ray
On a plain radiograph, an abdominal series may show any obstructions, ileus, or free air, indicating visceral perforation.
Contrast enema
This method is only useful in mild-to-moderate cases of diverticulitis when the diagnosis is in doubt. A water-soluble contrast should be used.
Ultrasonography
This is a safe, helpful, noninvasive method to evaluate acute diverticulitis. A common ultrasonographic finding is the visualization of an abnormal mural thickening of more than 4 mm involving a segment of 5 cm or longer at the point of maximal tenderness.
CT scan
Computerized tomography of the abdomen is considered the optimal method of investigation in patients suspected of acute diverticulitis. The CT scan is very sensitive (98%) in diagnosing diverticulitis. It may also identify patients with more complicated diverticulitis, such as those with an associated abscess.
Colonoscopy is contraindicated in the acute phase of diverticulitis due to the risk of perforation.
Treatment of diverticulitis
In general, the treatment can vary depending on the severity of the symptoms. If the symptoms are mild, home treatment should be enough. But, if the symptoms are long-lasting and tend to progress, hospitalization and even surgery may be included in the treatment.
Home care
It includes remaining quiet for a few days. Patients should also temporarily avoid all the whole grain products, fruits and vegetables so that their colon can rest and heal. Once your symptoms have improved, often in two to four days, patients can gradually start increasing the amount of high-fiber foods in their diet. Some antibiotics may be prescribed to help kill the bacteria causing the infection.
If a patient has moderate or severe pain, doctor may recommend an over-the-counter pain reliever such as acetaminophen (Tylenol, others).
Hospitalization
About half the people with diverticulitis require hospitalization and many of them need intravenous antibiotics.
Surgery
There are two common types of operations which are done in order to relieve all the symptoms caused by diverticulitis.
Read More: Diverticulitis diet
Primary bowel resection
This is the standard surgery for people with diverticulitis. Surgeon removes the diseased part of your intestine and then reconnects the healthy segments of your colon. Depending on the amount of inflammation, there is an open surgery-classical approach or laparoscopic surgery. Laparoscopic surgery may not be an option if the patient is very overweight or has an extensive inflammation.
Bowel resection with colostomy
A big problem may occur when a patient has so much inflammation in the colon that it's not possible to rejoin it ot the rectum. During a colostomy, surgeon makes an opening in your abdominal wall. The unaffected part of your colon is then connected to this opening, and waste passes through the opening into a bag.

