What makes this procedure so important? The procedure enables the physician to see details about every possible process on the large intestine wall.
This includes patients with following issues:
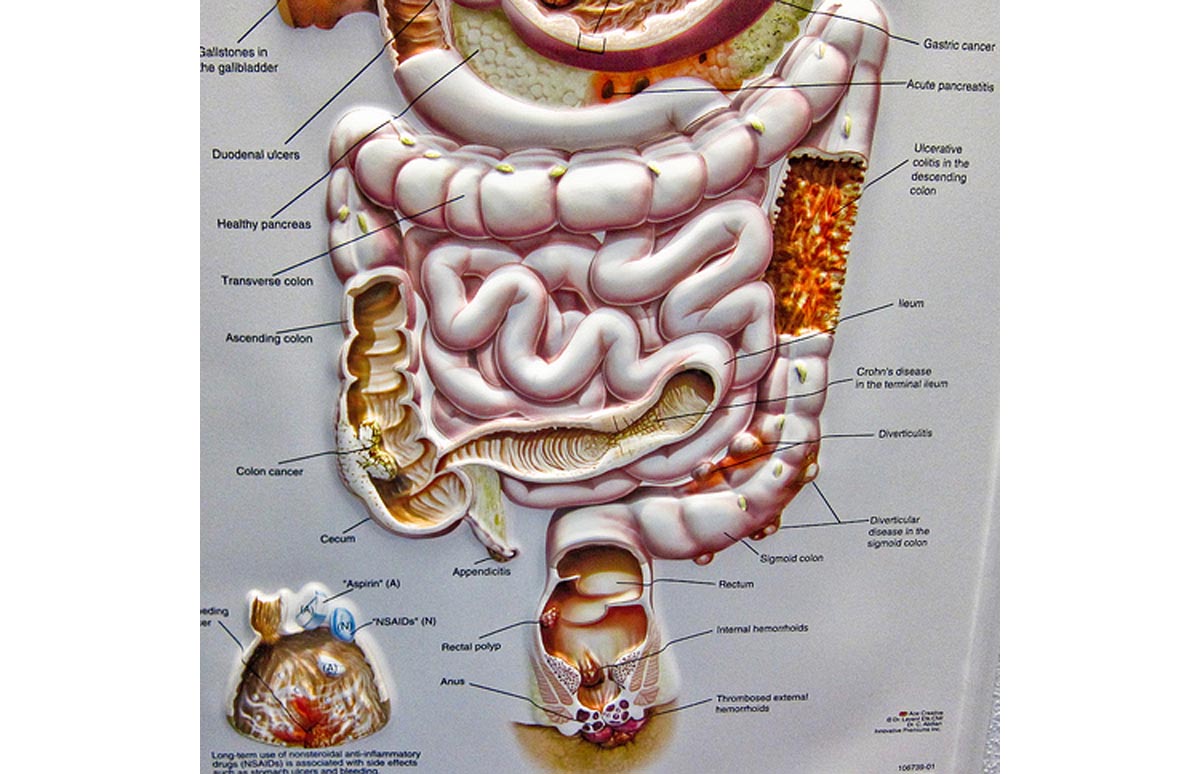
- inflamed tissue,
- abnormal growths, and
- ulcers
- early signs of cancer in the colon and rectum.
In the last couple of years colonoscopy exam is also used to diagnose patients with unexplained changes in bowel habits and to evaluate symptoms like abdominal pain, rectal bleeding, and unexplained weight loss.
Indications for the colonoscopy
There are many types of problems that can occur in the colon which could be the indication for the colonoscopy.
Although, viewing the inside of the colon directly by colonoscopy is usually the best exam, there are many other things such as the medical history, physical exam, laboratory tests and x-rays which could provide information useful for making a diagnosis.
Potential candidates for colonoscopy are patients with:
- Colon cancer: a serious but highly curable malignancy. Colorectal cancer is the second leading cause of cancer deaths in the United States. Colon cancer develops from growths within the wall of the intestine such as polyps or tumors. These growths often take 5-10 years to develop and may not cause many symptoms.
- Polyps: fleshy tumors which usually are the forerunners of colon cancer.
- Colitis (ulcerative or Crohn's): chronic, recurrent inflammation of the colon
- Diverticulosis and diverticulitis: pockets along the intestinal wall that develop over time and can become infected.
- Bleeding lesions: bleeding may occur in different parts of the colon.
- Abdominal symptoms, such as pain or discomfort, particularly if associated with weight loss or anemia
- Abnormal barium x-ray exam
- Chronic diarrhea, constipation, or a change in bowel habits
- Anemia
Info about colon or large intestine
The colon, or large bowel, is the last portion of the digestive tract or gastrointestinal tract. The colon begins in the right-lower abdomen and looks like a big question mark as it moves up and around the abdomen, ending in the rectum. It is 5 to 6 feet long. The colon has a number of functions including withdrawing water from the liquid stool that enters it so that a formed stool is produced.
Equipment used in colonoscopy
The primary tool in colonoscopy is called colonoscope. This is an incredibly flexible piece of equipment that can be directed and moved around the many bends in the colon.
Two types of colonoscopes:
- The original purely fiber-optic instrument has a flexible bundle of glass fibers that collects the lighted image at one end and transfers the image to the eye piece.
- The newer video endoscopes have a tiny, optically sensitive computer chip at the end. Electronic signals are transmitted up the scope to a computer which displays the image on a large video screen.
It is important to understand that there are open channels in all these scopes, which means that they are not only used to visualize the intestine but allow other instruments to be passed through in order to perform biopsies, remove polyps or inject solutions.
Preparations for the colonoscopy
The colon must be free of solid matter for the test to be performed properly. To prepare for the procedure you will have to follow a liquid diet for 1 to 3 days beforehand. The liquid diet should be clear and not contain food colorings, and may include
- fat-free bouillon or broth
- strained fruit juice
- water
- plain coffee
- plain tea
- diet soda
- gelatin
The day before the colonoscopy is performed, the patient is given laxative preparations such as sodium picosulfate, sodium phosphate solution, or a solution of polyethylene glycol and electrolytes, and large quantities of fluid. Administration of sedative drugs at colonoscopy has drawbacks, including an increased rate of complications, higher cost, and longer recovery periods for patients.
Because this procedure definitely disrupts the absorption in the large bowel, be sure to inform your doctor of any medical conditions you have or medications you take on a regular basis such as:
- aspirin
- arthritis medications
- blood thinners
- diabetes medication
- vitamins that contain iron
You should stay at home the evening before the test because the preparation given to you make you use the bathroom frequently. You should stop drinking clear liquids 6 to 8 hours before the colonoscopy.
The procedure
Although it can be done by other health professionals, the procedure is most often performed by a doctor who specializes in problems of the digestive system called gastroenterologist. Just before the procedure, the patient may receive a pain medication and a sedative through an intravenous (IV) line in an arm or a hand. These medications reduce pain and will make you feel relaxed and drowsy during the test. Patient then lies on his side with knees drawn up toward the abdomen and the doctor gently inserts a gloved finger into the anus to check for tenderness or blockage. Then a thin, well-lubricated colonoscope is gently inserted and advanced while the intestinal lining of the colon is examined through the scope. Although it is almost painless, it could be very unpleasant because patient may feel the urge to have a bowel movement while the scope is in the colon.
The doctor may also insert tiny instruments such as loops through the colonoscope to collect tissue samples or remove growths. Colonoscopy also has an important therapeutic role because it is not only used to observe but to treat. The doctor can remove most of the abnormal growths in the colon, like polyps, which are growths in the lining of the bowel. Polyps are removed using tiny tools passed through the scope. Most polyps are not cancerous, but they could turn into cancer. Just looking at a polyp is not enough to tell if it is cancerous. The polyps are sent to a lab for testing. By identifying and removing polyps, a colonoscopy is likely to prevent most cancers from forming.
The colonoscope is then slowly withdrawn and the air is allowed to escape. After the scope is removed, your anal area will be cleaned with tissues. If you are having cramps, passing gas may help relieve them.
The test usually takes less then one hour, approximately 30 to 45 minutes, but it may take longer, depending upon what is found and what is done during the test.
After the procedure
A recovery area is available to monitor vital signs until the patient is fully awake. It is normal to experience mild cramping or abdominal pressure following the exam. If the effects of the sedatives are prolonged, the physician may suggest an appointment at a later date. Patient must know that, if a biopsy has been performed or a polyp removed, the results will not be available for three to seven days and be prepared for the waiting. Rarely, patients experience severe abdominal pain, fever, bloody bowel movements, dizziness, or weakness afterward.
Possible Complications of Colonoscopy
Patients should know that although colonoscopy is a safe procedure, complications can sometimes occur and they should be prepared for it. The most common complications include:
- Bloating and distension - They typically occur for about an hour after the exam until the air is expelled
- Perforation - A puncture of the colon walls, which could require surgical repair.
- Bleeding - During the polyp removal or biopsy heavy bleeding may result and sometimes the patient may require blood transfusion or reinsertion of the colonoscope to control the bleeding.
- Due to the mild sedation, the patient should not drive or operate machinery following the exam
- Infections - Instances of transmission of infection from one patient to another or to endoscopic personnel have been documented but are extremely rare.
- Abdominal distension - Colonic distension during colonoscopy can cause notable discomfort and may also impair mucosal blood flow.
- Small bowel obstruction - Small bowel obstruction is another rare complication of colonoscopy, although it is perhaps more common in patients who have a history of abdominal surgery and postoperative adhesions.
Results of colonoscopy
If the doctor has taken a tissue sample, these samples are usually sent to a pathology lab, where they are examined under a microscope for evidence of certain diseases.
Other samples of colon tissue may be sent to a microbiology lab to determine whether certain kinds of infection are present. Your doctor may be able to discuss some of the findings with you immediately after the procedure. Other results are usually available in 2 to 4 days.
Colonoscopy
Normal:
The lining of the colon appears smooth and pink, with numerous folds. No abnormal growths, pouches, bleeding, or inflammation are present.
Abnormal:
Some of the more common abnormal findings of colonoscopy include hemorrhoids (the most common cause of blood in the stool), polyps, tumors, one or more sores (ulcers), pouches in the wall of the colon (diverticulosis), or inflammation. A red, swollen lining of the colon (colitis) may be caused by infection or inflammatory bowel disease.
See Also: Should You Ask For Anesthesia When You Have A Colonoscopy?
Virtual colonoscopy- alternative
Virtual colonoscopy uses x rays and computers to produce two and three-dimensional images of the colon from the lowest part, the rectum, all the way to the lower end of the small intestine, and display them on a screen. It is considered to be an alternative to conventional colonoscopy.
It is much more comfortable than conventional colonoscopy because it does not use a colonoscope. As a result, no sedation is needed, and you can return to your usual activities or go home after the procedure.
- en.wikipedia.org/wiki/Colonoscopy
- www.digestive.niddk.nih.gov
- www.gicare.com
- Photo courtesy of ex_magician on Flickr: www.flickr.com/photos/ex_magician/5708374253/guts.jpg

