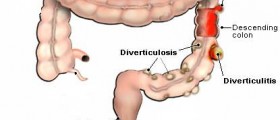
Diverticula are something like getting a hernia inside your body. The lining of the colon weakens so that it plops down to make a little pocket. If you just have the pockets, but they aren't inflamed, you have a condition called diverticulosis. If something has made them inflamed, then you have diverticulitis.
There are things called "true" diverticula, which are deep pockets involving all of the layers of the lining of the colon, and "false" diverticula, which involve just the top two layers of the colon. Either way, you have a serious problem. Diverticuli can also occur in the small intestine, which feeds into the colon.
People of European descent tend to get more false diverticula and to have their pain on the left side of the abdomen while people of Asian descent tend to have more true diverticula and to have their pain on the right side of the colon.
Chances are that your doctor was taught some things about diverticulosis and diverticulitis that turned out not to be true. Here are some of the facts about these conditions that aren't yet general knowledge, even in the medical profession.
- Diverticulosis (just the pockets) doesn't always progress to diverticulitis (inflamed pockets). It doesn't even usually progress to diverticulitis. Only about 1 percent of patients who have diverticulosis will get diverticulitis that is confirmed with a colonoscopy or a CT scan.
- Constipation doesn't cause diverticulosis. In fact, people who have hard stools and who have fewer bowel movements have lower rates of diverticulosis. Once you get diverticulitis, however, it really is a good idea to avoid constipation.
- Whether or not you eat nuts, seeds, and high-fiber plant foods doesn't have a lot to do with whether or not you develop diverticulitis.
- All of this doesn't mean, however, that it's impossible to predict whether or not you will get diverticulitis. People who have low vitamin D levels are more likely to get diverticulitis. People who already have diverticulitis are more likely to develop complications when their vitamin D levels are low.
The simple message here is that if you have diverticulitis, you need to be taking vitamin D. This is doubly true if you have dark skin, spend most of your time indoors (as many Americans do during the summer), are overweight (the fat underneath the skin can soak up vitamin D your skin makes before it can get to the rest of the body), or you live someplace more than half way from the equator to the poles. If you notice that your symptoms are worse in the winter (if you live in a cooler climate) or in the summer (if you live in an area where people avoid summer heat by sitting indoors near an air conditioner), then you probably need to take vitamin D, even if your doctor hasn't ordered a vitamin D test.
How much vitamin D is enough? Just 1,000 IU per day probably will make a difference. This dosage of vitamin D is very inexpensive. You really shouldn't take too much vitamin D. Taking 50,000 IU per day, for example, can lead to bone deformations (too much calcium rather than too little) and a propensity for sunburn.
Once you get diverticulitis, you aren't doomed to get it again. If you do nothing at all, there's about a 50 percent chance you'll have another round of symptoms. If you just take a Lactobacillus supplement 10 days a month (It's not necessary to take the supplement every day), then there's just a 13 percent chance of a relapse. If you take a drug called Mesalamine, there's also just a 13 percent chance of having symptoms again. You may not have to take the medication every day. If you take both Lactobacillus and Mesalamine, however, there is almost no chance you'll have to deal diverticulitis again. It may take you several months to start feeling good again, but a combination of vitamin D, Lactobacillus, and the prescription drug Mesalamine is usually your best guarantee of staying diverticulitis-free.
- David A. Johnson, MD. Debunking Myths About Diverticular Disease. Medscape Gastroenterology. 7 April 2014.
- Photo courtesy of SteadyHealth